Can a Tooth Infection Cause Meningitis?
You wake up with a throbbing toothache. It is annoying, but you push through your day. You tell yourself it is probably nothing serious.
But somewhere in the back of your mind, a worrying question appears. Can a tooth infection cause meningitis?
It sounds scary. Almost dramatic. But it is a fair question, especially when you hear stories about dental problems leading to serious illnesses.
Let me give you the short answer first: Yes, it is possible, but it is very rare.
Now, let me explain exactly what happens, why it is unlikely for most people, and what you should watch for. This guide will give you clear, honest, and practical information without trying to scare you. You will learn how your mouth connects to your brain, when a tooth infection becomes dangerous, and how to protect yourself.
Understanding the Basics: What Is a Tooth Infection?
Before we talk about meningitis, we need to understand what a tooth infection really is. Most people use the term loosely, but there are different types.
A tooth infection usually starts deep inside your tooth. It begins when bacteria reach the pulp. The pulp is the soft center of your tooth where nerves and blood vessels live.
How a tooth infection begins
Imagine you have a cavity you ignored for months. Or a cracked tooth from chewing something hard. Maybe you had a failed filling. These openings let bacteria travel inside your tooth.
Once bacteria enter the pulp, your body fights back. Inflammation starts. Pus forms. Pressure builds inside your tooth. This pressure has nowhere to go because the tooth is hard enamel on the outside.
That pressure causes the intense, throbbing pain people remember for life.
Types of tooth infections
Not all tooth infections are the same. Here is a simple breakdown:
| Type of Infection | Location | Common Symptoms |
|---|---|---|
| Dental abscess (periapical) | Tip of the tooth’s root | Sharp pain, sensitivity to hot/cold, pain when biting |
| Periodontal abscess | Gums next to a tooth root | Swollen gums, bad taste, loose tooth |
| Gingival abscess | Only in the gum tissue | Localized red swelling, mild pain |
The type that most concerns us for meningitis is the dental abscess at the root tip. This type can spread beyond the tooth into nearby spaces.
What happens when a tooth infection spreads
A healthy immune system usually walls off a tooth infection. Your body creates a pocket of pus called an abscess. This keeps bacteria contained.
But sometimes, the infection breaks through this wall.
When that happens, bacteria travel into surrounding tissues. They might go into your jawbone. They might move into your cheek or neck. And in very rare cases, they travel toward your brain.
This is where our main question becomes relevant.
What Is Meningitis? A Quick, Clear Explanation
Meningitis sounds terrifying, and rightfully so. But understanding what it is helps you stay calm and informed.
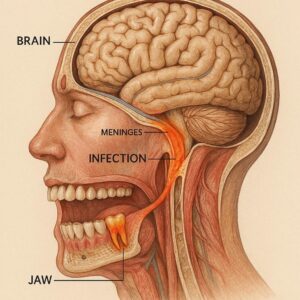
Meningitis is inflammation of the membranes that cover your brain and spinal cord. These membranes are called the meninges.
The two main types of meningitis
There are two broad categories. They are very different from each other.
Viral meningitis is more common. It is usually less severe. Many people recover on their own without specific treatment. It is rarely linked to tooth infections.
Bacterial meningitis is the dangerous one. It is a medical emergency. It moves fast and can cause brain damage, hearing loss, or death within hours. Bacterial meningitis is the type that could potentially come from a tooth infection.
How bacterial meningitis develops
Bacteria reach your meninges in a few ways. The most common route is through your bloodstream. Bacteria enter your blood from another infected site, travel up to your brain, and infect the meninges.
Another route is direct spread. Bacteria move from a nearby infected structure, like your sinuses, ears, or teeth, directly into the skull.
This second route is the one that connects tooth infections to meningitis.
Common symptoms of meningitis
Knowing these symptoms could save a life. They often appear suddenly.
-
Severe headache that feels different from any headache you have had
-
Stiff neck that makes it hard to touch your chin to your chest
-
High fever that comes on quickly
-
Sensitivity to light (photophobia)
-
Nausea and vomiting
-
Confusion or difficulty concentrating
-
Seizures in later stages
If you or someone you know has a tooth infection and develops these symptoms, seek emergency medical care immediately.
Important note: Do not wait to see if symptoms improve. Bacterial meningitis progresses very fast. Hours matter.
The Direct Connection: Can a Tooth Infection Cause Meningitis?
Now we reach the heart of the question. Let me give you the honest medical answer.
Yes, a tooth infection can cause meningitis, but it requires a specific set of circumstances. It does not happen often. Most tooth infections remain local problems.
However, when a tooth infection spreads, it follows predictable paths. One of those paths leads toward the brain.
The anatomical highway between your mouth and brain
Your face has several spaces filled with soft tissue and fat. Doctors call these fascial spaces. They are like hidden tunnels between structures.
A severe tooth infection, usually from an upper tooth, can spread into a space called the cavernous sinus. The cavernous sinus is a large vein at the base of your brain. It collects blood from your face and eyes.
If bacteria reach the cavernous sinus, they can cause a condition called cavernous sinus thrombosis. This is a blood clot with infection inside that vein. From there, it is a short step to meningitis.
Which teeth are most dangerous?
Not all teeth pose the same risk. Upper teeth, especially the molars and premolars, have roots that sit very close to your maxillary sinus. The maxillary sinus is an air-filled space behind your cheekbones.
An infected upper tooth can break through the thin bone separating your tooth root from your sinus. Once bacteria enter your sinus, they are one step closer to your brain.
Lower teeth infections rarely cause meningitis directly. They tend to spread downward into your neck. This creates another dangerous condition called Ludwig’s angina, which can block your airway. While not meningitis, it is equally life-threatening.
Realistic risk assessment
Let me put this in perspective. Dentists see thousands of tooth abscesses every year. Most treat them with antibiotics and root canals or extractions. Complications like meningitis are exceptionally rare.
According to dental literature, the number of tooth infections leading to brain abscess or meningitis is extremely low. You are more likely to get meningitis from a sinus infection or ear infection than from a tooth.
But rare does not mean impossible. Medical case reports document instances where dental infections spread to the brain. These cases usually involve:
-
People with weakened immune systems (diabetes, HIV, chemotherapy patients)
-
People who ignored a tooth infection for weeks or months
-
People who never received antibiotics or dental treatment
-
People with intravenous drug use (which introduces bacteria directly into blood)
The Step-by-Step Path: How a Tooth Infection Reaches the Brain
Let me walk you through exactly how this happens. Understanding the journey helps you recognize when things are going wrong.
Stage one: The established abscess
You have a tooth infection. Maybe you feel pain, maybe you do not. Some chronic abscesses cause little pain but still harbor bacteria. The abscess grows slowly.
Stage two: The breach
Your immune system fails to contain the infection. This can happen for many reasons. You might be stressed, sick, or diabetic. You might take steroids that suppress immunity. Or the bacteria might be particularly aggressive.
The abscess wall breaks down. Bacteria flood into surrounding tissues.
Stage three: Local spread
From your tooth root, bacteria move into your jawbone. This causes a bone infection called osteomyelitis. Or they move into your cheek, causing facial swelling you can see.
Stage four: Reaching the bloodstream
Once bacteria enter your bloodstream, a condition called bacteremia begins. Your blood carries these bacteria throughout your body. Most get filtered by your liver and spleen. But some survive.
Stage five: Crossing the blood-brain barrier
Your brain has a special defense called the blood-brain barrier. It keeps most bacteria out. But certain bacteria, like the ones found in mouth infections, can cross this barrier.
The most common oral bacteria linked to brain infections include:
-
Streptococcus species (especially Streptococcus anginosus group)
-
Fusobacterium
-
Actinomyces
These bacteria have tools that help them stick to blood vessels and slip through protective barriers.
Stage six: Meningitis develops
Once bacteria reach your meninges, your immune system responds aggressively. Inflammation floods the area. Swelling puts pressure on your brain. Pus forms around your spinal cord. This is meningitis.
The timeline from a simple tooth infection to meningitis varies. It can take weeks or months of neglect. But in rare aggressive cases, it can happen in days.
Warning Signs: When to Worry About Your Tooth Infection
Most tooth infections stay exactly where they belong. But sometimes they give you signals that something more serious is happening.
Do not ignore these signs.
Signs your tooth infection is spreading locally
Before worrying about meningitis, look for signs that your infection is leaving the tooth.
-
Swelling on your face that you can see from across the room
-
Swelling that moves under your jaw or down your neck
-
Difficulty opening your mouth more than a finger’s width
-
Trouble swallowing or speaking clearly
-
A fever that does not go away after a day or two
-
Feeling generally unwell, like you have the flu
These signs mean you need urgent dental care. Not tomorrow. Not next week. Today.
Signs pointing toward possible meningitis
If your tooth infection comes with any of these symptoms, go to an emergency room immediately. Do not go to your dentist first.
-
Severe headache that feels different from normal headaches
-
Stiff neck that makes looking down painful
-
Confusion or acting unlike yourself
-
Extreme sensitivity to bright lights
-
Nausea and vomiting without an obvious stomach cause
-
A rash that does not fade when you press a glass against it (this is a late sign but very serious)
Remember: You do not need all these symptoms. Even two or three together are enough to seek emergency care.
A note about dental pain without swelling
Many people worry that any tooth pain could cause meningitis. That is not true. A tooth that hurts but has no swelling, no fever, and no facial changes is almost certainly a local problem.
Pain alone is not a sign of dangerous spread. Pain is your tooth crying for help, but it does not mean your brain is in danger.
Risk Factors: Who Should Be Most Careful?
Some people face higher risks of dental infections spreading. If you fall into these categories, take tooth infections more seriously than the average person.
Medical conditions that increase risk
| Condition | Why It Increases Risk |
|---|---|
| Diabetes (especially uncontrolled) | High blood sugar weakens immune response |
| HIV or AIDS | Low white blood cell counts make fighting infection harder |
| Cancer chemotherapy | Suppressed bone marrow reduces infection-fighting cells |
| Long-term steroid use | Steroids mask inflammation and weaken immunity |
| Alcohol use disorder | Poor nutrition and liver damage impair immune function |
| Organ transplant recipients | Anti-rejection drugs suppress the immune system |
Anatomical factors
Some people are born with slight differences in how their facial spaces connect. These variations are rare, but they exist. You cannot know if you have them without imaging.
Behavioral factors
-
Avoiding dental care for years
-
Ignoring obvious cavities or broken teeth
-
Not finishing prescribed antibiotics
-
Using intravenous drugs (contaminated needles introduce bacteria directly into blood)
If any of these apply to you, do not let a tooth infection go untreated. See a dentist at the first sign of trouble.
Prevention: How to Stop This From Happening
The good news is that preventing a tooth infection from causing meningitis is simple. You do not need expensive treatments or complicated routines.
Basic dental hygiene that actually works
You have heard this before, but let me remind you why it matters.
Brush twice a day with fluoride toothpaste. Floss once a day. See your dentist every six to twelve months for cleanings and exams.
These simple habits prevent cavities. No cavities means no tooth infections. No tooth infections means zero risk of dental meningitis.
Treat small problems while they are small
A small cavity costs a filling. A large cavity that reaches the pulp costs a root canal or extraction. An ignored tooth that causes a facial infection costs hospitalization.
Treat problems early. It saves money, pain, and rare but serious complications.
What to do if you have a tooth infection
If your dentist tells you that you have an abscess, follow these steps:
-
Take the full course of antibiotics exactly as prescribed. Do not stop early even if you feel better.
-
Schedule the definitive treatment (root canal or extraction) as recommended. Antibiotics alone will not cure a tooth infection. They only control it temporarily.
-
Watch for the spreading signs I listed earlier. If you see them, call your dentist or go to an emergency room.
-
Take pain relievers as directed. Managing pain helps you rest and heal.
When antibiotics are not enough
Many people believe antibiotics cure tooth infections. They do not. Antibiotics reduce the bacterial load and stop the spread, but they cannot reach inside a dead tooth. The source of the infection remains.
You must remove the source. That means either a root canal (cleaning the inside of the tooth) or an extraction (removing the tooth completely). Delaying this step leaves you at risk of recurrence.
Treatment: What Happens If a Tooth Infection Spreads?
Let us talk about what doctors and dentists do if a tooth infection reaches the point where meningitis is a real concern.
Treating the spreading dental infection
Before meningitis develops, doctors focus on controlling the source and stopping the spread.
-
Intravenous antibiotics given through a vein in your hospital room
-
Surgical drainage of the facial abscess
-
Removal of the infected tooth (often done in the hospital if swelling is severe)
-
Monitoring your breathing if swelling threatens your airway
Most people recover fully at this stage. They never develop meningitis because doctors intervene in time.
Treating dental meningitis
If the infection reaches your meninges, treatment becomes much more aggressive.
-
High-dose intravenous antibiotics for two to four weeks
-
Possible admission to an intensive care unit
-
Corticosteroids to reduce brain swelling
-
Seizure medications if needed
-
Repeated lumbar punctures (spinal taps) to check if antibiotics are working
The mortality rate for bacterial meningitis is around 10 to 15 percent even with modern treatment. Survivors may face long-term problems like hearing loss, memory difficulties, or seizures.
This is why prevention and early treatment matter so much.
The role of lumbar puncture
A lumbar puncture, or spinal tap, is the test that confirms meningitis. Doctors insert a thin needle between two lower vertebrae to collect cerebrospinal fluid. They send this fluid to a lab to look for bacteria and white blood cells.
The test sounds scarier than it is. It takes about 15 minutes. Most people feel only pressure and mild discomfort.
Common Myths About Tooth Infections and Meningitis
Let me clear up some misinformation. The internet has many scary stories about teeth and brains. Some are true, but many are exaggerated.
Myth 1: Any tooth infection can cause meningitis at any time
Truth: Most tooth infections never spread beyond the tooth. Your body is very good at walling off infections. Meningitis from a tooth requires a perfect storm of neglect, aggressive bacteria, and a weakened immune system.
Myth 2: You will always have severe pain before meningitis develops
Truth: Some people have chronic, painless abscesses. These “silent” infections can exist for months or years without significant pain. They still pose a small risk of spreading.
Myth 3: Root canals cause meningitis
Truth: This is false. Root canals treat infections. They remove bacteria from inside your tooth. A properly done root canal eliminates the source of infection and reduces your risk of spread, not increases it.
Myth 4: If you have a tooth infection and a headache, you have meningitis
Truth: Tooth infections themselves cause headaches. The pain radiates from your jaw to your temple or ear. This is normal. A meningitis headache is different. It is severe, spreads to your whole head, and comes with neck stiffness and light sensitivity.
Myth 5: Antibiotics alone can prevent meningitis from a tooth infection
Truth: Antibiotics help, but they are not a guarantee. Some bacteria resist common antibiotics. And antibiotics cannot reach bacteria deep inside a dead tooth. You need definitive dental treatment.
What to Do Right Now: A Practical Action Plan
You came here with a question. Let me give you a clear action plan based on your current situation.
If you have no tooth pain or infection
Keep doing what you are doing. Maintain good oral hygiene. See your dentist regularly. You have nothing to worry about.
If you have a mild toothache that comes and goes
Schedule a dental appointment within the next week. The tooth likely has a cavity or a crack. Treating it now prevents an abscess later.
If you have constant, throbbing tooth pain
Call your dentist today. Ask for an emergency appointment. You may have a dying nerve or an early abscess. Treatment now is straightforward. Waiting makes it more complicated.
If you have facial swelling from a tooth
Go to a dentist or an emergency room today. Facial swelling means the infection has left the tooth. You need antibiotics and likely a root canal or extraction soon.
If you have facial swelling plus fever, difficulty swallowing, or trouble breathing
Go to an emergency room immediately. Do not pass go. Do not call your dentist first. This is a medical emergency.
If you have any meningitis symptoms (severe headache, stiff neck, confusion) with or without a known tooth infection
Go to an emergency room immediately. Tell them about your dental history. Let the doctors figure out the cause. Do not assume it is just a migraine or a sinus headache.
Real Cases: What Medical Literature Tells Us
Medical journals publish case reports of dental infections spreading to the brain. These reports are rare, which is good news. But they offer valuable lessons.
A typical case example
A 45-year-old man with diabetes ignored a painful tooth for three months. He developed swelling under his eye. He still did not seek care. Two weeks later, he arrived at an emergency room with a severe headache, fever, and confusion.
Doctors diagnosed meningitis from a dental abscess. He spent three weeks in the hospital on intravenous antibiotics. He lost hearing in one ear permanently. His tooth was extracted.
The lesson: Early treatment would have prevented all of this.
A less common case
A 28-year-old woman with no medical problems developed a tooth infection after a failed filling. She took antibiotics but did not return for a root canal. The infection returned two months later and spread to her brain within five days.
She survived with no permanent damage because she went to the emergency room quickly when symptoms appeared.
The lesson: Even healthy people can have complications. And fast action saves lives.
What these cases teach us
No one expects their tooth infection to turn into meningitis. But the people in these cases did not expect it either. The key difference between good and bad outcomes was time.
Those who sought care early did well. Those who delayed suffered permanent consequences.
Frequently Asked Questions (FAQ)
Q: How common is meningitis from a tooth infection?
A: Extremely rare. Dentists see thousands of tooth abscesses for every one that leads to meningitis. You are far more likely to get meningitis from a sinus or ear infection.
Q: Can a wisdom tooth infection cause meningitis?
A: Yes, if the wisdom tooth is in your upper jaw. Upper wisdom teeth sit close to your sinuses. An infected upper wisdom tooth follows the same potential path as any other upper tooth.
Q: How long does it take for a tooth infection to cause meningitis?
A: There is no set timeline. Some cases develop over weeks or months of neglect. Rare aggressive cases can develop in days. Do not try to calculate your risk based on time. Focus on symptoms instead.
Q: Can a root canal cause meningitis?
A: No. A properly performed root canal removes infection. It does not create it. In fact, a root canal is the treatment that prevents meningitis from a tooth infection.
Q: What if I have no dental insurance?
A: Many communities offer low-cost dental clinics, dental schools, or sliding-scale fees. An emergency room cannot refuse you care for a serious infection, but they will treat the infection, not the tooth. Look for community health centers in your area.
Q: Can I wait to see if my tooth infection gets better on its own?
A: No. Tooth infections do not heal without treatment. The pain may go away temporarily if the nerve dies, but the infection remains. Waiting only makes treatment harder and complications more likely.
Q: My tooth stopped hurting. Am I safe?
A: Not necessarily. When a tooth nerve dies, the pain stops, but the infection continues. A painless abscess is still an abscess. See a dentist.
Q: Can antibiotics cure a tooth infection without a root canal?
A: No. Antibiotics temporarily control the infection but cannot cure it. The dead tissue inside your tooth remains a breeding ground for bacteria. You still need a root canal or extraction.
Additional Resources
For more reliable information about dental infections and their complications, visit the American Association of Endodontists at www.aae.org. This organization represents root canal specialists and provides patient-friendly information about tooth infections, abscesses, and when to seek emergency care.
You can also check the Centers for Disease Control and Prevention (CDC) page on meningitis for symptom checklists and prevention tips.
Final Summary: What You Need to Remember
A tooth infection can cause meningitis, but this complication is very rare. It usually happens when someone ignores a dental abscess for weeks or months, has a weakened immune system, or both. The infection spreads from an upper tooth into the sinuses and then to the brain’s protective membranes. Most people never need to worry about this, but everyone should know the warning signs: severe headache, stiff neck, confusion, and light sensitivity. Treat tooth infections early, and you eliminate the risk entirely.
Conclusion
Here is what you need to take away from this guide.
First, yes, a tooth infection can cause meningitis, but it is exceptionally rare. Your odds of winning a small lottery prize are better than your odds of getting meningitis from a tooth.
Second, most tooth infections stay local. They cause pain and swelling, but they do not travel to your brain. Your body does a remarkable job containing them.
Third, prevention is simple. Brush, floss, see your dentist, and treat cavities when they are small. These habits cost little time and money but provide enormous protection.
Fourth, know the warning signs. Severe headache plus stiff neck plus confusion equals an emergency room visit. Do not wait. Do not assume it is nothing.
Finally, do not live in fear. The connection between teeth and meningitis is real but remote. Millions of people have tooth abscesses every year. Almost none develop meningitis. Be aware, but do not be terrified.
Take care of your teeth. Listen to your body. Seek help when something feels wrong. You will be fine.