Is Tooth Decay The Same As Infection?
You wake up with a throbbing tooth. A friend says, “It’s probably just decay.” Another says, “No, that sounds like an infection.” You start to wonder: are they talking about the same thing?
It is a common question, and the answer is not a simple yes or no. Tooth decay and infection are closely related, but they are not identical. Think of decay as the open door, and infection as the uninvited guest who walks through it.
Understanding this difference matters. It can help you know when to book a routine checkup and when you need urgent care. It can also save you from unnecessary worry—or from ignoring a problem that needs immediate attention.
Let us walk through this together. We will keep the language simple, the examples clear, and the advice practical.
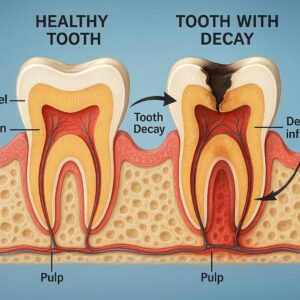
What Exactly Is Tooth Decay?
Tooth decay starts quietly. You probably will not feel it at first. Many people describe it as a slow process, almost invisible until it has done real damage.
In simple terms, tooth decay is the breakdown of your tooth enamel. Enamel is the hard, outer layer that protects your tooth. It is the toughest substance in your body, but it is not invincible.
Here is what happens behind the scenes.
The Science Made Simple
Your mouth is full of bacteria. Do not worry—that is normal. Most of these bacteria are harmless. Some are even helpful. But a few specific types, especially Streptococcus mutans, love sugar.
When you eat or drink something sugary, these bacteria feed on that sugar. As they eat, they produce acid. That acid attacks your enamel, leaching minerals out of it. Over time, this weakens the enamel and creates tiny holes.
Those tiny holes are the first stage of decay. Dentists call them “white spot lesions” because they look like chalky white patches on your tooth. At this stage, the damage is still reversible. Your saliva can help repair the enamel with minerals like calcium and phosphate.
But if the acid attacks continue, the enamel breaks down further. The white spots turn into brown or black holes. That is a cavity. Once a cavity forms, it cannot heal on its own. You need a dentist to clean it out and fill it.
Common Causes You Can Control
You have probably heard most of these before. But seeing them together helps explain why decay is so common.
-
Frequent snacking on sugary foods. Every time you eat sugar, your mouth produces acid for about 20 to 30 minutes. Grazing all day keeps that acid level high.
-
Poor oral hygiene. Skipping brushing or flossing leaves food particles for bacteria to feast on.
-
Dry mouth. Saliva is your mouth’s natural defense. It washes away food and neutralizes acid. Without enough saliva, decay spreads faster.
-
Acidic drinks. Soda, sports drinks, and even fruit juice can erode enamel directly, making it easier for decay to start.
-
Receding gums. When gums pull back, they expose the softer root surface of your tooth. That surface decays much faster than enamel.
How Dentists Classify Decay
Not all decay is the same. Dentists use stages to describe how deep the problem goes.
| Stage | What It Means | Do You Feel It? |
|---|---|---|
| Initial | Enamel is losing minerals but not yet broken. White spots appear. | No pain. |
| Enamel decay | A visible cavity forms in the enamel. | Usually no pain, or mild sensitivity to sweets. |
| Dentin decay | Decay reaches the softer layer under enamel. | Sensitivity to cold, hot, or sweet foods. |
| Pulp involvement | Decay touches the tooth’s nerve center. | Moderate to severe pain, especially at night. |
Once decay reaches the dentin or pulp, you are entering a new territory. That is where infection becomes a real possibility.
What Is a Tooth Infection?
An infection is different. While decay is a process of destruction, an infection is an invasion.
A tooth infection happens when bacteria get inside the innermost part of your tooth, called the pulp. The pulp contains nerves, blood vessels, and connective tissue. It is a living part of your tooth.
When bacteria reach that space, your immune system responds. You get inflammation, swelling, and eventually pus. That pus has nowhere to go. It builds up pressure inside your tooth, which is why infections hurt so much.
The Most Common Type: Dental Abscess
Doctors and dentists usually call a tooth infection a “dental abscess.” There are two main types.
Periapical abscess. This is the most common. It starts in the pulp of the tooth and spreads through the tip of the root into the surrounding bone.
Periodontal abscess. This one starts in the gums and bone around the tooth, not inside the tooth itself. It often happens with advanced gum disease.
For most people, when they ask “Is tooth decay the same as infection?” they are thinking of a periapical abscess. That is the one that follows untreated decay.
How an Infection Feels
An infection does not hide. It announces itself loudly.
-
Throbbing pain. The pain often comes in waves. It can spread to your jaw, ear, or neck.
-
Pain when chewing or touching the tooth. Even light pressure hurts.
-
Sensitivity to hot and cold. The sensation lingers long after the hot or cold is gone.
-
Swelling in your face or cheek. This is a sign the infection is spreading.
-
Fever. Your body is fighting back.
-
A bad taste in your mouth. The abscess may drain pus into your mouth.
-
Swollen lymph nodes under your jaw.
If you have these symptoms, do not wait. A tooth infection will not go away on its own. It needs treatment, often with antibiotics and a root canal or extraction.
Can an Infection Happen Without Decay?
Yes. While decay is the most common cause, it is not the only one.
A cracked tooth can let bacteria in, even if that tooth has no cavities. A deep filling that leaks over time can also lead to infection. Trauma to a tooth—like a fall or a sports injury—can damage the pulp even if the outside of the tooth looks fine.
But in the vast majority of cases, infection follows decay. Decay creates the pathway. Infection takes advantage of it.
The Direct Relationship Between Decay and Infection
Now we arrive at the heart of the question. Think of tooth decay and infection as two points on a timeline.
Decay comes first. It is the initial injury. Infection comes later, if decay is left untreated.
Here is a simple analogy.
Imagine your tooth is a house. The enamel is the front door. Decay is like someone slowly drilling a hole through that door. At first, the hole is small. You might not even notice it. But as the hole gets bigger, rain, insects, and rodents can get inside.
Infection is those unwanted guests. They only enter because the hole exists. Without the hole, they stay outside.
So while decay and infection are not the same thing, one leads directly to the other in most cases.
The Progression Step by Step
Let us track what happens inside a single tooth over time.
-
Healthy tooth. Enamel is intact. Pulp is protected.
-
Early decay. Minerals are lost from enamel. No bacteria inside yet.
-
Cavity forms. The hole reaches dentin. Bacteria start traveling down the hole.
-
Decay reaches pulp. Bacteria enter the nerve center. Inflammation begins.
-
Infection sets in. Pus forms. Pressure builds. Pain becomes severe.
-
Abscess forms. The infection spreads to the bone around the root tip.
At step four, decay and infection overlap. The decay created the pathway, and the infection is now active. But a dentist can still treat the tooth and save it with a root canal.
At step five or six, the infection is fully established. The tooth may still be saved, but the treatment is more complex.
Important Note for Readers
Do not assume that a painless cavity is safe. Many people ignore small holes or dark spots because they do not hurt. But decay can be deep and close to the pulp without causing any pain. By the time pain arrives, infection may already be present. Regular dental checkups catch decay before it reaches that point.
Key Differences at a Glance
To make things clearer, here is a side-by-side comparison.
| Feature | Tooth Decay | Tooth Infection |
|---|---|---|
| What it is | Destruction of tooth structure | Invasion of bacteria into the pulp |
| Causes | Sugar, acid, poor hygiene | Untreated decay, cracks, trauma |
| Pain level | None to mild sensitivity | Moderate to severe, throbbing |
| Visible signs | Holes, dark spots, white patches | Swelling, pimple on gum, pus |
| Can it heal on its own? | Early stage (white spots) only | No |
| Treatment | Filling, crown | Root canal, antibiotics, extraction |
| Emergency risk | Low | High |
You can have decay without infection. You cannot have a tooth infection without some way for bacteria to enter the tooth. That entry is almost always decay or a crack.
When Decay Becomes Dangerous
Not all decay leads to infection. Some people have small cavities for years without ever developing an abscess. Others get an infection within weeks of a cavity forming.
Why the difference? Several factors play a role.
Your Immune System
A strong immune system can keep bacteria in check. It can surround and contain a small number of invaders before they multiply enough to cause an abscess. But if your immune system is weakened—by stress, illness, or certain medications—even a small cavity can turn into a serious infection.
The Location of the Decay
Decay on the chewing surface of a molar moves slowly. The enamel there is thick. But decay between teeth, near the gum line, or on the root surface moves much faster. Those areas have thinner enamel or no enamel at all. Bacteria reach the pulp more quickly.
Your Oral Hygiene Habits
If you brush and floss regularly, you remove some of the bacteria that would otherwise travel down the cavity. You also stimulate saliva flow, which fights decay. Good hygiene does not stop an existing cavity from growing, but it can slow the progression significantly.
Access to Dental Care
This is an honest reality. People who see a dentist every six months rarely develop tooth infections. Their cavities are caught early and filled. People without regular dental care are the ones who show up in emergency rooms with facial swelling and severe pain.
If you cannot afford a dentist, look for community health centers or dental schools. They offer reduced-cost care. A small filling today prevents a costly root canal or extraction tomorrow.
Can You Have Both at the Same Time?
Yes. In fact, most tooth infections happen in teeth that also have active decay.
When a dentist treats an infected tooth, they almost always find decay underneath. The decay created the opening. The infection followed.
However, there is one exception worth mentioning. A tooth can have a root canal treatment that removes the infection, but the tooth itself may still have decay on the outside. The decay does not hurt because the nerve is gone, but it can still weaken the tooth and cause it to crack.
So yes, decay and infection can coexist. Treating the infection without addressing the decay is like closing your windows but leaving your front door wide open. The problem will return.
Treatment: What to Expect for Each Condition
Treatment depends entirely on how far the problem has progressed.
If You Only Have Decay (No Infection)
Your dentist will likely recommend one of these options.
Fillings. The dentist removes the decayed part of the tooth and fills the hole with composite resin, amalgam, or glass ionomer. The procedure is quick. You get numbing medicine, so you feel no pain.
Inlays or onlays. For larger cavities that do not need a full crown, these custom-made pieces fit into or onto the tooth. They are stronger than fillings and last longer.
Crowns. If decay is extensive and has weakened the tooth, a crown covers the entire visible part of the tooth. It protects the tooth from fracturing.
Fluoride or remineralization. For the earliest stage of decay (white spots only), you might not need a filling. Your dentist may apply fluoride varnish or prescribe a high-fluoride toothpaste to help the enamel repair itself.
If You Have an Infection
This is more serious. You need treatment that removes the bacteria from inside the tooth.
Antibiotics. These do not cure the infection inside the tooth. But they control the spread to surrounding tissues. Your dentist may prescribe them before a root canal if you have swelling or fever.
Root canal treatment. This is the standard treatment for an infected tooth. The dentist makes a small hole in the tooth, removes the infected pulp, cleans and disinfects the inside, and fills it with a rubber-like material. Then you get a crown to protect the tooth.
Extraction. If the tooth is too damaged to save, or if you cannot afford a root canal, the dentist removes the tooth entirely. This stops the infection immediately. You can later replace the missing tooth with an implant, bridge, or partial denture.
Incision and drainage. If you have a large abscess (a pocket of pus), the dentist may need to cut it open to let the pus drain. This relieves pressure and pain quickly, but you still need a root canal or extraction afterward.
A Word on Pain Management
Over-the-counter pain relievers like ibuprofen or acetaminophen can help with discomfort from both decay and infection. But they do not treat the cause. Never rely on painkillers to solve a dental problem. They only mask the symptoms while the underlying issue gets worse.
Common Myths and Misconceptions
Let us clear up a few things that confuse many people.
Myth: A black spot on your tooth always means infection.
Not true. A black or brown spot is decay, not infection. Infection causes swelling, pain, and sometimes a pimple on the gum. A dark spot by itself is a cavity that needs a filling, not emergency treatment.
Myth: If a tooth stops hurting, the infection went away.
False. This is dangerous thinking. An infection can kill the nerve inside your tooth. When the nerve dies, the pain stops. But the infection is still there, spreading into the bone. You may not feel it until the swelling becomes severe.
Myth: Baby teeth with decay do not matter because they fall out.
This is not correct. Baby teeth hold space for permanent teeth. Severe decay in a baby tooth can lead to an infection that damages the developing adult tooth underneath. It can also cause pain and difficulty eating.
Myth: You can cure a tooth infection with home remedies.
No. Salt water rinses, clove oil, and garlic can provide temporary comfort. They cannot reach the inside of your tooth where the bacteria live. Only a dentist can remove the source of the infection.
Myth: Root canals are painful.
This old belief comes from a time before modern anesthetics. Today, a root canal feels similar to getting a filling. The pain you feel beforehand—from the infection—is far worse than the procedure itself.
How to Prevent Decay From Becoming an Infection
Prevention is always easier and cheaper than treatment. You already know the basics, but let us focus on what actually stops decay from turning into infection.
Daily Habits That Make a Real Difference
Brush twice a day with fluoride toothpaste. Fluoride strengthens enamel and can reverse early decay. Use a soft-bristled brush and spend two full minutes brushing.
Floss once a day. Decay between teeth is the most common type to go unnoticed. Flossing removes the food and bacteria that your toothbrush cannot reach.
Limit sugar to mealtimes. Snacking on sugar throughout the day keeps your mouth acidic for hours. If you want something sweet, eat it with a meal. Your saliva has time to recover between meals.
Drink water. Water rinses away food particles and neutralizes acid. If you cannot brush after eating, swish with water.
Chew sugar-free gum with xylitol. Xylitol reduces the number of decay-causing bacteria in your mouth. Chewing also stimulates saliva, your natural protector.
Professional Prevention
Regular cleanings and exams. Your dentist can spot decay when it is still reversible or small enough for a simple filling. Do not wait for pain.
Sealants. These thin plastic coatings go on the chewing surfaces of back teeth. They block bacteria and food from settling into the deep grooves where decay often starts. Sealants are especially helpful for children and teenagers, but adults can get them too.
Fluoride treatments. In-office fluoride varnish provides a strong boost to your enamel. It is quick, painless, and affordable.
When to Act Immediately
Do not wait for your next scheduled appointment if you notice any of these signs.
-
A pimple-like bump on your gum near a tooth.
-
Swelling in your face or neck.
-
A tooth that hurts when you tap on it.
-
Pain that wakes you up at night.
-
A bad taste in your mouth that will not go away.
These are signs of infection, not just decay. Call your dentist the same day. If you cannot reach a dentist and you have facial swelling or trouble swallowing, go to an emergency room.
Frequently Asked Questions
Can a small cavity turn into an infection overnight?
No. The process takes weeks or months. But you cannot always feel the cavity getting deeper. A small cavity today can become an infection in a few months if you ignore it.
How do I know if my toothache is decay or infection?
Decay usually causes mild, brief sensitivity to sweets or cold. An infection causes constant, throbbing pain that gets worse when you lie down. It also causes swelling and sometimes fever.
Do I always need a root canal for an infection?
Most of the time, yes. The only alternatives are extraction or, in very rare cases, a procedure called pulpotomy (partial nerve removal) for specific situations. Antibiotics alone will not cure the infection.
Can a tooth infection spread to my body?
Yes. A tooth infection can spread to your jaw, neck, and even your bloodstream. This is called sepsis, and it is life-threatening. Do not ignore a dental abscess.
Is it safe to wait to treat a decayed tooth?
If the decay is shallow and not causing pain, waiting a few weeks for an appointment is usually fine. But if you have pain, sensitivity, or any signs of infection, do not wait. The longer you wait, the more treatment you will need.
Can I reverse decay without a filling?
Only in the earliest stage, when the decay is limited to the enamel and appears as a white spot. Once a hole (cavity) forms, you need a filling. No toothpaste or home remedy can fix a hole in your tooth.
Are some people more prone to decay and infection?
Yes. Genetics play a role in enamel strength and saliva composition. Some medications cause dry mouth, which increases risk. People with diabetes also have a higher risk of dental infections.
Additional Resources
For more reliable, science-based information on tooth decay and dental infections, visit the American Dental Association’s public education website:
MouthHealthy.org – Tooth Decay Topic Page
This site offers videos, printable guides, and advice for all ages. It is written in plain English and reviewed by dentists. No ads, no gimmicks—just honest information.
Conclusion
Tooth decay and infection are not the same thing, but they travel together. Decay is the slow breakdown of your enamel. Infection is what happens when that breakdown lets bacteria reach the nerve of your tooth. You can have decay without infection, but most infections start as untreated decay. Catch decay early, and you avoid the pain, expense, and danger of an infection. Brush, floss, see your dentist regularly, and never ignore a toothache that throbs or swells.