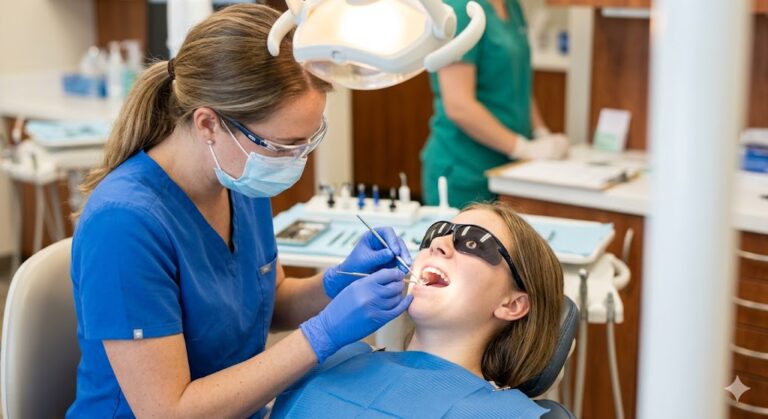
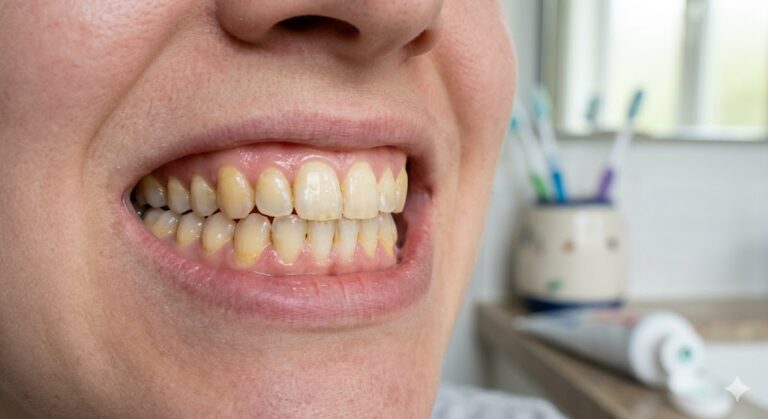
Why Did My Dental Implant Come Out?
- On
- InDENTAL
The moment you feel that unsettling shift in your mouth—or worse, the sudden absence of a tooth you paid thousands to replace—your mind races to one singular, frantic question: why did my dental implant come out? It is a scenario that feels like a nightmare, especially after enduring months of surgery and healing. You followed the instructions. You kept it clean. So, why did it fail?
Let’s pause and take a deep breath. In most cases, the thing that came out of your mouth is not the implant itself. Understanding the difference between the parts of your dental restoration is the first critical step in solving the problem and saving your smile. The implant is a titanium screw buried deep in your jawbone. What you see above the gum line is a crown. What connects them is a tiny screw called an abutment.
More often than not, the abutment screw has loosened or the crown cement has failed. But in rarer, more serious cases, the entire implant fixture has indeed lost its bond with the bone. This comprehensive guide will walk you through every possible scenario, from the simple, fixable annoyances to the complex medical reasons for true implant failure.
We will leave no stone unturned. We will explore the biology of bone healing, the mechanics of chewing forces, and the hidden habits that sabotage dental work. By the end of this article, you will know exactly what to do next and how to talk to your dentist with confidence.
Table of Contents
ToggleA Crucial Distinction: The Crown vs. The Fixture
Before we dive into the reasons for failure, we need to establish a clear vocabulary. Many patients say “my implant came out” when they are actually holding a porcelain tooth in their hand. Here is a simple breakdown of the anatomy of an implant restoration.
| Component | Description | Is It Supposed to Come Out? | What It Feels Like |
|---|---|---|---|
| Implant Fixture | The titanium screw in the jawbone. | NO. This requires surgical removal if it fails. | A gritty, metallic taste or a visible metal screw thread in the gum hole. |
| Abutment | The connector post attached to the fixture. | Rarely. It can loosen but usually stays in the gum. | A small metal nub sticking out of the gum. |
| Crown | The white, visible tooth part. | Sometimes. It can be screwed in (retrievable) or cemented (permanent). | You are holding a hollow white tooth in your hand. |
| Healing Cap | A temporary cover during healing. | Yes. It falls out often before the final crown is placed. | A small, flat metal disc. Not an emergency. |
Important Note: If you are holding a white tooth with a hollow underside or a small metal screw attached to it, your implant fixture is likely still in the bone. This is a mechanical failure of the restoration, not a biological failure of the implant. This is usually a quick, inexpensive fix.
Part 1: The Early Warning Signs Before It Comes Out
Implants rarely fail without warning. Recognizing these red flags can save you from a complete loss. If you have experienced any of these sensations in the weeks leading up to the event, they hold the key to understanding why did my dental implant come out?
-
Persistent Discomfort vs. Normal Healing Pain: After surgery, pain should decrease daily. If pain increases after two weeks, especially a deep, throbbing ache that wakes you up at night, the body is fighting something—either infection or movement.
-
The “Loose Tooth” Sensation: A successful implant feels exactly like a healthy natural tooth fused to your skull. There should be zero movement. If you can wiggle the implant or crown even a fraction of a millimeter with your tongue or finger, the integration has been compromised.
-
A Bad Taste That Won’t Go Away: This is a hallmark of Peri-implantitis. It is not just morning breath. It is a sour, metallic, or foul drainage coming from a specific spot around the implant. This is pus seeping out from a pocket of infection deep under the gum.
-
Receding Gums Exposing Metal: You should not see the rough, dark gray threads of the implant screw. If gum tissue shrinks back, it leaves the implant vulnerable to bacteria and plaque accumulation.
-
Difficulty Chewing: If you subconsciously avoid chewing on that side because it “feels weird” or “high,” you are sensing micromovement. This movement prevents bone from fusing to the titanium.
Part 2: Immediate Mechanical Reasons (When the Crown Comes Off)
Let’s address the most common and least alarming scenario. You bite into a sandwich, and suddenly you are spitting out a tooth. You look in the mirror and see a metal stump or a hole in your gum.
This is the “Abutment Screw Fracture or Loosening” scenario. It accounts for roughly 60% of emergency calls regarding “my implant came out.” Here is why this happens.
2.1 The Abutment Screw Loosened
The abutment screw is a tiny but mighty piece of hardware. It is the set screw that holds your visible tooth onto the implant fixture in the bone. Over time, the forces of chewing can act like a mini impact wrench, backing this screw out.
Common Culprits:
-
Inadequate Torque: The dentist did not tighten the screw to the manufacturer’s exact specifications using a torque wrench. Under-tightening leads to wobble; over-tightening leads to fracture.
-
Poor Fit: If the crown does not seat perfectly flat on the implant, a “microgap” exists. Every time you chew, the crown rocks back and forth, unscrewing the connection.
-
Bruxism (Grinding): You are applying 200-300 pounds of lateral force to a tiny screw. No screw can withstand that forever without maintenance.
What This Looks Like: You have a hollow crown in your hand. The metal abutment is still attached to the implant in your mouth (it looks like a silver peg sticking out of the gum).
The Fix: This is typically a 15-minute, non-painful appointment. The dentist removes the loose abutment, cleans the connection, inspects the threads, and re-torques a new screw. Do not use Super Glue. You will turn a simple fix into a $2,000 surgical extraction.
2.2 Crown Cement Failure
If your implant crown is cement-retained (meaning it is glued onto the abutment like a cap on a pen), that cement can degrade over time.
| Cement Type | Durability | Common Failure Mode |
|---|---|---|
| Temporary Cement | 6-12 months | Designed to fail for retrievability. |
| Permanent Cement | 5-15 years | Saliva dissolution or occlusal overload. |
| Resin Cement | 10+ years | Rarely fails; usually bond strength exceeds tooth strength. |
Reader’s Story: “I was flossing and my front implant tooth popped right off into the sink. I panicked. I thought I broke the metal part. Turned out it was just temporary cement from my dentist so he could adjust the bite later. He put it back on in 5 minutes with stronger glue.”
The Fix: The dentist will clean out the old cement from inside the crown and place it back on. Crucial Warning: If any cement gets trapped under the gum line during this process, it causes a massive inflammatory reaction and bone loss. This is why many top surgeons prefer screw-retained crowns—they leave no hidden cement.
Part 3: Early Implant Failure (The Fixture Comes Out)
This is the scenario that carries the most emotional and financial weight. You look in the mirror, and instead of a tooth or a metal peg, you see a dark hole, or worse, a spiral piece of metal lying on your tongue. The titanium screw has detached from the bone.
This is classified as Early Implant Failure, occurring within the first 3 to 6 months of placement, before the final crown is even attached.
3.1 Failure of Osseointegration
Osseointegration is the biological process where living bone cells grab onto the titanium oxide surface of the implant. It is a miracle of modern medicine. When this process fails, the implant remains a foreign object in a wallowed-out socket. Eventually, the body expels it, much like a splinter.
Why does osseointegration fail?
-
Bone Quality (Type IV Bone): Some people have very soft, fatty marrow in their back upper jaw. It is like trying to screw a wood screw into drywall without an anchor. It will spin and never tighten. Implants in soft bone require a longer healing period (4-6 months vs. 3 months) and a gentle surgical technique.
-
Overheating the Bone: During drilling, the dentist must use copious amounts of cool saline water. If the drill bit spins too fast or the water flow is blocked, the bone temperature exceeds 47°C (117°F). This literally cooks the bone cells to death. Necrosis of the bone means no cells are alive to grow onto the implant. The implant will be loose from day one.
-
Smoking: This is the number one patient-modifiable risk factor. Nicotine constricts blood vessels by up to 50%. Without blood flow, the bone cannot heal. Smokers have an implant failure rate 2 to 3 times higher than non-smokers.
-
Systemic Disease: Uncontrolled Diabetes (high HbA1c) alters collagen formation and impairs white blood cell function. Osteoporosis medications (bisphosphonates) prevent normal bone turnover.
3.2 Infection (Peri-implantitis in the Early Stage)
Sometimes the implant integrates beautifully, but bacteria get into the wound during the first few weeks.
-
Contaminated Implant Surface: The titanium surface is sterile out of the package. If it touches the patient’s cheek, a non-sterile glove, or saliva before placement, a biofilm forms instantly.
-
Micro-movement: If the patient chews on the implant too early (against medical advice), the tiny wiggles pump bacteria down the side of the implant, preventing the gum collar from sealing.
Important Medical Note: If the implant comes out on its own within the first 6 weeks, it is almost always due to lack of initial stability or infection. There is rarely anything the patient did wrong except perhaps not following the soft-food diet.
Part 4: Late Implant Failure (Why It Happens Years Later)
You have had that implant for 8 years. It felt like part of your skull. You forgot it wasn’t a real tooth. Then one morning, it feels “spongy” when you bite down. By the afternoon, you can see a gap around it. This is Late Implant Failure.
4.1 The Silent Epidemic: Peri-implantitis
This is the primary answer to why did my dental implant come out after years of success. It is the implant equivalent of gum disease (periodontitis), but it is often more aggressive and harder to treat.
The Progression of Peri-implantitis:
-
Mucositis: Bleeding gums around the implant. Reversible with good cleaning. No bone loss yet.
-
Peri-implantitis: Inflammation spreads to the bone. The body begins resorbing (eating away) the jawbone around the threads.
-
Crater Formation: A deep, infected pocket forms. You cannot reach the bottom with floss. Food and anaerobic bacteria fester in this moat.
-
Loss of Support: Once more than 50% of the implant length has lost bone contact, the implant becomes mobile.
-
Expulsion/Fracture: The implant either falls out due to lack of support or breaks under normal chewing forces.
The “Gum Pocket” Comparison Chart
| Characteristic | Healthy Implant | Mucositis | Peri-implantitis |
|---|---|---|---|
| Bleeding on Probing | No | Yes | Yes (Profuse) |
| Pocket Depth | 1-3 mm | 4-5 mm | 6+ mm |
| Pus/Suppuration | No | No | Yes |
| Bone Loss (X-ray) | None | None | Visible “saucer” shape around threads |
| Treatment | Routine Cleaning | Improved Hygiene | Surgical Intervention |
What Causes Peri-implantitis?
-
Cement Left Behind: Microscopic flecks of cement under the gum act as a permanent splinter. The body tries to dissolve the cement, but in doing so, it dissolves the surrounding bone.
-
Poor Oral Hygiene: Flossing an implant is non-negotiable. You must use a Waterpik or Superfloss with a stiff end to thread under the bridgework.
-
Genetic Predisposition: If you lost your natural teeth to gum disease, you carry the bacteria and the immune response that will attack an implant just as aggressively.
4.2 Mechanical Overload and Fracture
Even titanium has a fatigue limit. After millions of chewing cycles, metal can crack.
-
Cantilever Forces: If an implant supports a bridge that hangs out over open space (no back tooth support), the leverage on the screw is immense. This is like holding a heavy bucket with your arm straight out instead of close to your body. Eventually, either the screw snaps or the implant fixture itself fractures.
-
Bruxism Complications: Nighttime grinding generates forces 5x higher than chewing. Without a custom Night Guard, these forces transmit directly to the bone-implant interface. The bone resorbs to get away from the pressure (a process called Microfracture Accumulation).
-
Fractured Fixture: In rare cases, the actual titanium screw splits vertically. This is catastrophic. The implant must be surgically removed (often with a trephine drill). When this piece comes out, it looks like a broken screw.
Part 5: Medical and Biological Factors Beyond Your Control
Sometimes, you did everything right. You flossed daily, wore your night guard, and never smoked. Yet, the implant failed. Why did my dental implant come out despite perfect care?
The answer lies in the complex interplay between foreign materials and the human immune system.
5.1 Titanium Allergy or Hypersensitivity
For decades, the dental industry claimed titanium allergy did not exist. Recent research, specifically the Melisa Test and patch testing, confirms that a small subset of the population (estimated 0.6% to 4%) develops a Type IV hypersensitivity reaction to titanium oxide particles.
What Happens: The body recognizes the titanium as an allergen. It recruits T-cells and macrophages to wall off the implant. Instead of bone forming on the implant, a soft layer of scar tissue forms around it. This is called Fibrous Encapsulation. The implant is never rigidly fixed. It sits in a soft, fleshy socket.
Symptoms:
-
Itching or eczema flare-ups after implant placement.
-
Unexplained bone loss without signs of infection (no pus).
-
Implant mobility despite good hygiene.
-
Full-body fatigue or neurological symptoms (very rare, controversial).
The Solution: If you suspect a titanium allergy, you can request a Zirconia Implant. These are white, ceramic, metal-free implants. They are highly biocompatible and offer an alternative for patients with metal sensitivities.
5.2 Autoimmune Conditions
Conditions like Lichen Planus, Sjögren’s Syndrome, and Lupus alter the oral environment.
-
Dry Mouth (Xerostomia): Saliva is nature’s disinfectant. Without it, plaque hardens into calculus 10x faster. Fungal infections (Candida) thrive, breaking down the gum seal around implants.
-
Oral Lichen Planus: This causes chronic inflammation and sloughing of the oral tissues. The junction where the gum meets the implant is a weak point that is constantly under attack.
5.3 Bisphosphonate-Related Osteonecrosis of the Jaw (BRONJ)
This is a critical warning for any reader taking bone medications.
-
Medications: Fosamax, Actonel, Boniva, Reclast, Zometa, Prolia, Xgeva.
-
The Risk: These drugs prevent bone turnover. While good for preventing spine fractures, they stop the jaw from healing after minor trauma. A dental implant placement is major trauma to the jawbone. In patients on IV bisphosphonates (cancer patients), the risk of the bone dying and sloughing out (leaving exposed jawbone that never heals) is significant. In oral bisphosphonates, the risk is low but real after 3+ years of use.
-
Result: The bone around the implant dies. The implant falls out, but the socket does not heal. It becomes a persistent, open wound in the jawbone.
Important Medical Note: If you have ever taken a bisphosphonate drug, you must inform your oral surgeon. A simple blood test (CTX test) can gauge your risk for implant surgery.
Part 6: A Deep Dive into the Surgery Itself (Iatrogenic Causes)
We must address the elephant in the room: sometimes, the reason the implant came out originates in the dentist’s chair. This is not about blame; it is about understanding technical complications so you can be an informed patient.
6.1 Poor Implant Positioning (Malposition)
Placing an implant is a 3D puzzle. If the angle is off by even 10 degrees, the long-term prognosis plummets.
-
Too Close to Adjacent Tooth: The implant damages the blood supply to the natural tooth next door. It also creates a “black triangle” gap where food gets permanently stuck.
-
Too Far Buccally (Toward Cheek): The implant is outside the bony envelope. The gum is thin, and the bone resorbs rapidly. The threads become exposed.
-
Too Deep or Too Shallow: An implant placed too deep creates a massive gum pocket. An implant placed too high (not enough bone coverage) lacks support for the neck of the fixture.
Table: Effects of Implant Malposition
| Error | Immediate Consequence | Long-Term Outcome |
|---|---|---|
| Angle Error | Crown looks bulky or “fake” | Screw loosening, bone resorption |
| Depth Error | Difficult to clean | Peri-implantitis within 2 years |
| Spacing Error | Damage to adjacent tooth root | Loss of natural tooth + implant |
| Nerve Impingement | Numb lip, chin, or tongue (Paresthesia) | Potential permanent nerve damage |
6.2 Failure to Manage the Sinus Cavity
In the upper back jaw, the sinus is a hollow air space. The bone between the mouth and sinus is often thin. If an implant is placed and it just barely touches the sinus membrane, the membrane can become inflamed.
-
Sinus Perforation: Air leaks through the implant socket. You can whistle through your nose. Bacteria from the mouth enter the sinus, causing Chronic Sinusitis.
-
Implant Migration into Sinus: This sounds like a horror movie, but it happens. If the bone is too soft, the implant can be pushed up into the sinus cavity during placement or while chewing later. If you have an upper implant that suddenly feels “high” or you have post-nasal drip that smells like infection, get an X-ray immediately.
Part 7: The Patient Factor – Habits That Unseat Implants
You are 50% of the success equation. Let’s look at the daily habits that can answer why did my dental implant come out.
7.1 The Nighttime Grinder (Bruxism)
We touched on this earlier, but it deserves its own section because it is the most common cause of late mechanical failure.
-
Fact: During REM sleep, the jaw muscles can contract with 1,000 psi of force.
-
Effect: This lateral force bends the implant screw. Over time, the screw fatigues and snaps. Or, the bone cells (osteocytes) sense the vibration and trigger resorption.
-
The Solution: A custom-fitted Occlusal Guard (hard acrylic, not a soft boil-and-bite sports guard). A proper night guard provides a flat, slippery surface that protects the implant by allowing the jaw to slide rather than lock up.
7.2 The Aggressive Flosser
Yes, you can be too clean.
-
The Mistake: Using a metal pick or a water flosser on the highest “jet” setting directly at the gum line of an implant.
-
The Consequence: You blow the fragile gum attachment off the implant surface. This creates a recession defect. Once the gum is gone, it does not grow back. The exposed implant surface collects more bacteria, accelerating bone loss.
-
The Correct Method: Use a Waterpik on Setting 3 or 4 with the Pik Pocket Tip (soft rubber tip) placed gently at the gum line, not under it.
7.3 Chewing Ice and Non-Food Items
Implant crowns are made of Zirconia or Porcelain fused to metal. These materials are harder than natural enamel. While they won’t chip easily, the shock of biting an ice cube doesn’t break the tooth—it breaks the bond to the bone.
Every time you crunch ice, the vibration travels down the titanium screw. This is called Microtrauma. Over 5-10 years, this microtrauma can cause a 1-2mm ring of bone loss around the top of the implant. That’s all it takes for bacteria to get a foothold and start peri-implantitis.
Part 8: What To Do Right Now: The Emergency Protocol
You are reading this because something is wrong right now. Here is the step-by-step guide to managing the situation like a pro.
Scenario A: You are holding the whole white tooth in your hand. The metal screw is still in your mouth.
-
DO NOT PANIC. This is a crown cement failure or abutment screw loosening.
-
DO NOT EAT on that side.
-
Inspect the Crown. Is it hollow? Is there dried glue inside? Gently clean out any debris with a toothpick. Do not scrub the inside aggressively.
-
Storage. Place the crown in a small container or plastic bag.
-
Call Your Dentist. Say: “My implant crown came off. The abutment looks intact.” They will see you within 1-2 days. This is not a weekend emergency unless you have a wedding to attend on Monday.
Scenario B: You see or feel the metal screw in the gum hole. The “tooth” is missing or you found a metal piece.
-
This is a potential surgical emergency.
-
Rinse Gently. Use warm salt water (1 tsp salt to 8 oz water) ONLY if it doesn’t hurt too much. Swish very gently. Do not spit vigorously. Let the water dribble out.
-
Cover the Site. If you have a sterile gauze pad, bite down gently on it to control any minor bleeding.
-
Medication Check. If you have a history of heart valve issues or joint replacement, contact your physician about the need for Antibiotic Prophylaxis due to the open wound in the bone.
-
Call Your Oral Surgeon/Periodontist IMMEDIATELY. This is a “Monday morning first thing” or “Emergency Room if severe pain/swelling” situation.
Scenario C: The implant is wiggly but still attached.
-
Go on a Soft/Liquid Diet. Do not wiggle it with your tongue. You are testing to see if it falls out, but you are making the bone defect bigger.
-
Antibiotics? If you have a fever or facial swelling, yes. If it’s just loose with no pain, wait for the doctor.
-
Imaging Needed. You need a CBCT Scan (3D X-ray). A normal panoramic X-ray might not show the true extent of bone loss. The CBCT reveals if the implant is salvageable.
Part 9: Can It Be Saved? Treatment Options After Failure
The implant came out. Now what? Here is the realistic roadmap for your dental future.
9.1 Re-Torque and Splinting (For Loose but Present Fixtures)
If the implant is just slightly mobile due to a loose abutment screw, the dentist can remove the crown, tighten the screw to 35 Ncm of torque, and cement the hole closed. This often resolves the issue for years.
9.2 Bone Grafting and Site Preservation
If the implant falls out due to infection, the socket left behind is infected and wider than the original implant. You cannot simply screw a larger implant in immediately.
-
The Process: The surgeon will curette (scrape) all infected granulation tissue out of the hole. This looks like red, mushy, diseased flesh. They will then pack the hole with Bone Graft Material (cadaver bone, cow bone, or synthetic).
-
Healing Time: 4 to 6 months. You need to wait for the graft to turn into hard, living bone before attempting another implant.
9.3 Implant Removal and Replacement (The “Rescue” Implant)
In cases of a fractured implant or early failure, the old fixture must be removed. This is done with a special tool called a Trephine Bur. It cuts a small core of bone around the implant to release it, causing minimal trauma.
-
Immediate Replacement? Sometimes, if there is enough healthy bone at the base of the socket, the surgeon can place a Wider Diameter “Rescue” Implant immediately after removing the failed one. This is technically demanding but saves the patient months of waiting.
-
Success Rate of Second Attempt: The success rate for a second implant in the same site is 85-90% , slightly lower than the first attempt (98%). Scar tissue and altered blood flow play a role.
9.4 Abandoning the Site: The Bridge or Partial Denture
Sometimes, the bone loss is so severe that another implant is not financially or biologically feasible. The options shift back to traditional dentistry:
-
Fixed Bridge: Involves cutting down the two adjacent healthy teeth to support a false tooth in the middle.
-
Removable Partial Denture (Flipper): A plastic plate with a tooth on it. Least expensive but least comfortable.
-
No Replacement: Leaving the space empty will cause the opposing tooth to “super-erupt” (grow down/up into the space) and the adjacent teeth will tilt into the gap within 6-12 months. This creates a collapse of the bite that is expensive to fix later.
Part 10: Prevention: How to Ensure Your Next Implant Stays Put
Since you are now an expert in why implants fail, let’s focus on how to make the next one—or the one on the other side of your mouth—a success story for life.
10.1 The 3-Month Hygiene Protocol
Forget brushing and flossing. Implants require Interproximal Brushing.
-
Tool: ProxyBrush (Go-Betweens) or Soft-Picks.
-
Technique: Slide the brush under the gumline between the implant crown and the natural tooth. You should feel it slide along the smooth metal abutment.
-
Frequency: Every single night. This removes the biofilm that causes peri-implantitis.
10.2 The Importance of a Night Guard
If you have one implant, you have already shown a susceptibility to tooth loss. Protect your investment.
-
Custom vs. OTC: A $20 drugstore guard is made of Thermoplastic Vinyl. It is soft and squishy. Chewing on soft plastic increases muscle activity in bruxers—it makes grinding worse. You need a hard acrylic guard made from a dental impression. It costs $400-$600 but saves a $5,000 implant.
10.3 Annual X-rays and Probing
Your dentist should use a Plastic or Carbon Fiber Probe (not metal) to measure the gum pocket around your implant annually. Metal probes scratch the titanium abutment, creating grooves for bacteria.
-
Red Flag: A pocket depth increase from 3mm to 5mm in one year is a sign of active disease.
Part 11: Psychological Impact and Financial Realities
We cannot conclude this guide without addressing the very real human cost of a failed implant. When you ask why did my dental implant come out, there is often an unspoken second question: “How could this happen to me after all I went through?”
It is normal to feel:
-
Anger: At the dentist, at your body, at the cost.
-
Defeat: “I did everything right and it still failed.”
-
Anxiety: “Will I ever be able to chew steak again?”
Understanding the Warranty:
Most dentists offer a 5-year warranty on the crown (the tooth part) but no warranty on the implant fixture (the screw) because the body’s healing is beyond their control. If an implant fails within the first year, many surgeons will replace it for a reduced fee or at no cost for the surgical part, but the patient often still pays for the new abutment and crown.
Financial Note: If you paid with a CareCredit or other medical credit card, check your policy. Some cards offer “Lost or Stolen” protection that might cover a medical device failure, though this is rare. More likely, you will need to budget $1,500 to $3,000 for a replacement implant surgery (if bone graft is needed) plus $1,500 for a new crown.
Part 12: Frequently Asked Questions About Dental Implant Failure
Q: Can a loose implant tighten back up on its own?
A: No. This is a dangerous myth. A loose implant means the bone has separated from the titanium. Bone does not reattach to a dirty, moving surface. The only way to save it is surgical intervention. Wiggling it will enlarge the bone crater and guarantee failure.
Q: Is it possible to swallow a dental implant?
A: It is possible to swallow an abutment screw or a crown (though rare). It is almost impossible to swallow a full-size implant fixture without choking. If you swallow a crown, it will likely pass through your digestive tract within 24-48 hours. You should still see a doctor for an abdominal X-ray to ensure it is not stuck. It will be, to put it bluntly, “recovered” naturally. It is not reusable after this journey.
Q: What is the white stuff in the hole where the implant came out?
A: This is usually Granulation Tissue (healing tissue) mixed with Fibrin (a clotting protein). It is a normal part of the wound healing process. If it is hard and you can scrape it out easily with a fingernail, it might be Necrotic Bone or Food Debris. Do not dig in the socket. Let the dentist debride it.
Q: Why does the implant smell bad when it comes out?
A: The smell of a failing implant is unmistakable. It is the smell of Anaerobic Bacteria (bacteria that live without oxygen) and Volatile Sulfur Compounds. This is the exact same smell as severe gum disease or a tonsil stone. It indicates an active, long-standing infection in the bone pocket.
Q: How long do I have to wait to get a new implant after one fails?
A: This depends on the bone defect.
-
Clean removal, minimal bone loss: 3-4 months.
-
Infection present, bone graft placed: 6-8 months.
-
Sinus lift or major reconstruction required: 9-12 months.
Additional Resources
For further reading on the science of osseointegration and peri-implant diseases, visit the official resource page of the American Academy of Periodontology.
Link to: https://www.perio.org/for-patients/periodontal-treatments-and-procedures/dental-implant-procedures/
Conclusion
Understanding why a dental implant comes out separates the simple mechanical fix of a loose crown from the complex biological failure of bone integration. By recognizing the early warning signs of infection or movement and acting swiftly, you give yourself the best possible chance of saving the implant or ensuring a successful replacement. Remember, most issues are manageable, and with the right specialist care, a stable, lasting smile remains a realistic and achievable goal.
dentalecostsmile
Newsletter Updates
Enter your email address below and subscribe to our newsletter