dental implants how long do they last
- On
- InDENTAL
The question comes up in nearly every consultation room across the country. You sit in the chair, flip through the glossy brochure showing perfect smiles, and ask the only thing that really matters when making a significant investment in your health: dental implants how long do they last?
It is a fair question. And the answer is not a simple number on a warranty card.
Unlike a car tire that wears down predictably after 50,000 miles or a roof that needs replacing every 20 years, a dental implant is a living, breathing partnership between advanced engineering and human biology. The short answer is that the implant fixture—the titanium post buried in your jawbone—can last a lifetime. The visible crown—the porcelain tooth attached to the top—typically requires replacement after 15 to 20 years due to normal wear and tear.
However, that simple answer hides a world of nuance. This guide will not give you vague platitudes. We will dissect the data, examine the failure rates, explore the daily habits that determine longevity, and provide a realistic, unvarnished look at what you can expect over the next thirty, forty, or fifty years.
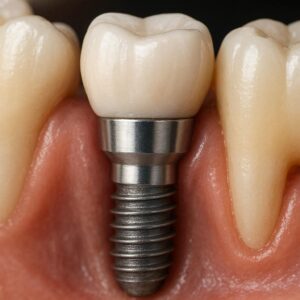
Table of Contents
ToggleThe Anatomy of Longevity: Understanding the Three Components
Before we can accurately answer dental implants how long do they last, we must break down the device itself. People often think of an implant as one solid object. It is not. It is a symphony of three distinct parts, and each part ages at a completely different rate. Misunderstanding this is the primary reason for confusion regarding lifespan.
1. The Implant Fixture (The Root)
This is the foundation. It is a screw-shaped post, usually made of commercially pure titanium or a titanium alloy. It is surgically placed directly into the jawbone. Titanium possesses a unique property called osseointegration. Bone cells do not see it as a foreign invader; they see it as a scaffolding to grow onto and bond with.
How long does this part last? In a healthy patient with good oral hygiene, the titanium post is designed to outlive you. It does not decay. It does not rust. Once the bone fuses to it completely—a process that takes three to six months—the connection is stronger than the original natural tooth root. The data from long-term studies tracking patients for over 30 years shows survival rates for the fixture consistently above 95%. In many cases, it is effectively permanent.
Important Note: While titanium is biologically inert, it is not magically immune to neglect. The fixture can still fail if the surrounding bone gets infected or if excessive force breaks the bond. We will address those specific failure modes later.
2. The Abutment (The Connector)
The abutment is the middleman. It is a small connector piece that screws into the titanium implant body and protrudes slightly above the gum line. Its job is to hold the visible crown in place. Abutments are made from titanium, zirconia, or gold.
How long does this part last? Under normal conditions, the abutment itself should last the life of the implant. The weak point is not the metal; it is the tiny screw that holds it all together. Abutment screws are designed to be the “mechanical fuse” in the system. If you bite down too hard on an unexpected olive pit, the screw might loosen or break to protect the more valuable implant fixture buried in the bone. Replacing a loose abutment screw is a 15-minute, non-invasive procedure. Replacing a broken implant fixture is oral surgery.
3. The Prosthesis (The Crown, Bridge, or Denture)
This is the part you see in the mirror. It is usually made of porcelain fused to metal (PFM), solid zirconia, or layered porcelain. It is the only part of the implant system that is not buried in sterile bone. It lives in the hostile environment of your mouth: acid from coffee, abrasive action from toothpaste, and crushing forces from chewing.
How long does this part last? This is the component with the shortest shelf life. The average lifespan of an implant crown is 10 to 20 years.
| Component | Expected Lifespan | Primary Threat | Replacement Difficulty |
|---|---|---|---|
| Implant Fixture | 25+ Years to Lifetime | Peri-implantitis (Gum Disease) | High (Surgical) |
| Abutment | 20+ Years | Screw Loosening/Fracture | Low (Non-Surgical) |
| Crown/Bridge | 10-15 Years | Chipping, Wear, Esthetics | Low to Moderate |
When you ask dental implants how long do they last, you are actually asking about the durability of the crown. You will likely need to change the “tires” (crown) long before you need to replace the “engine block” (fixture).
The Benchmark Data: What Does the Science Actually Say?
Marketing materials often promise a “Lifetime Guarantee.” Let’s put that in context with actual longitudinal studies. Dentists rely on a metric called the Survival Rate. This measures whether the implant is still physically in the mouth, even if it looks a bit worn or the gum is slightly inflamed.
-
At 5 Years: The survival rate for dental implants in the general population is 97% to 98% . This is higher than the survival rate of natural teeth in patients with a history of decay or bridge work.
-
At 10 Years: The survival rate remains remarkably high at 95% .
-
At 20+ Years: Data gets slightly thinner here due to the difficulty of tracking patients over decades, but the available Swedish studies (the birthplace of modern implantology) show survival rates between 90% and 93% .
But here is a crucial distinction: Survival vs. Success.
An implant can “survive” for 30 years even if it has 6mm of bone loss around it and the gums bleed constantly. That is not a “successful” implant in a clinical sense. A successful implant has zero bone loss, no bleeding, and a pristine crown. Achieving that level of perfection for decades requires more than just a skilled surgeon; it requires an engaged patient.
The Dichotomy of Failure: Why Don’t They Last Forever?
If you want a realistic answer to dental implants how long do they last, you must study failure. Looking at why implants fail is more instructive than looking at why they succeed. Failure falls into two distinct time frames: Early Failure (within the first year) and Late Failure (after 5+ years).
Early Failure (The First 12 Months)
This is almost always related to biology and surgical technique. The goal of surgery is to achieve osseointegration (bone fusion). If this fails, the implant will be loose and painful within weeks or months.
Common Culprits:
-
Smoking: Nicotine is a potent vasoconstrictor. It chokes off the tiny blood vessels trying to deliver healing cells to the implant site. Smokers have an early failure rate 2.5 to 3 times higher than non-smokers.
-
Uncontrolled Diabetes: High blood sugar (HbA1c over 7.0) impairs the immune system and slows down bone healing significantly.
-
Bone Quality: If the jawbone is too soft or too thin, the surgeon cannot achieve “primary stability”—that initial tight grip needed to hold the implant still while the bone grows. In these cases, a bone graft is necessary first.
-
Overheating the Bone: During drilling, if the surgeon does not use copious water irrigation, the friction heat can literally cook and kill the bone cells surrounding the implant site. This is a purely technical factor.
Quotable Insight: “An implant is a medical device. It is not a miracle. If the biological terrain is compromised by smoking or disease, the device will fail regardless of how expensive it was.” — Dr. P. Branemark (paraphrased principle of osseointegration)
Late Failure (Year 5 and Beyond)
This is where the answer to dental implants how long do they last gets personal. Late failure is almost entirely preventable and almost entirely the patient’s responsibility. The primary villain here is Peri-implantitis.
Peri-implantitis is the destructive, inflammatory process that affects the gums and bone surrounding an implant. Think of it as gum disease on steroids. Because an implant lacks the tiny ligament fibers that attach a natural tooth to gum tissue, bacteria have a “highway” straight down to the bone. Once infection sets in, bone loss can be rapid and painless. You often do not know it is happening until the implant becomes loose or the gum starts to recede, exposing gray metal threads.
Three Factors That Guarantee a Shorter Lifespan:
-
Poor Home Care: Skipping flossing around the implant crown. Bacteria love the margin where the crown meets the gum.
-
Lack of Professional Maintenance: Implants require a specific type of cleaning with non-metal scalers and plastic tips. A standard “scrape and polish” from a hygienist using steel instruments will scratch the titanium abutment, creating microscopic grooves for bacteria to hide in.
-
Occlusal Overload: Bruxism (teeth grinding). This is the silent killer of long-term implant success. The human bite can generate over 200 pounds of force. A natural tooth has a ligament that acts as a shock absorber. An implant is rigidly fused to the bone. It feels zero shock absorption. If you grind your teeth at night, that force transfers directly to the bone-implant interface, causing microscopic fractures in the bone (micro-cracks) that lead to loosening.
The Lifetime Comparison: Implants vs. The Alternatives
To truly appreciate the value proposition when asking dental implants how long do they last, we need to compare them against the other options you might have chosen instead. The upfront cost of an implant is undeniably higher. But the long-term cost of ownership tells a different story.
| Feature | Dental Implant | 3-Unit Dental Bridge | Removable Partial Denture |
|---|---|---|---|
| Expected Lifespan | 25+ Years (Fixture) | 7 – 10 Years | 5 – 7 Years |
| Impact on Adjacent Teeth | None (Independent) | Requires drilling down 2 healthy teeth | Clasps weaken anchor teeth |
| Bone Preservation | Prevents bone loss (Resorption) | Bone shrinks under the missing tooth space | Accelerates bone loss under the appliance |
| 5-Year Complication Rate | <5% (Peri-implantitis) | 15% (Decay under crowns) | 30% (Sore spots, breakage) |
| 10-Year Replacement Cost | Crown replacement only | Full bridge replacement (New decay) | New denture + possible tooth loss |
The Bridge Trap:
A patient missing one tooth often gets a 3-unit bridge. After 8 years, decay sneaks under the edge of one of the supporting crowns. Because the bridge is one solid piece, you cannot just fix the decay. The entire bridge must be cut off and thrown away. You are now missing three teeth instead of one. The implant, by contrast, leaves the neighboring teeth alone.
The Daily Grind: How Habits Impact Your Implant’s Lifespan
You have control over roughly 80% of what determines dental implants how long do they last. The surgeon and the lab technician control the other 20%. Here is a realistic look at the daily decisions that add or subtract years from your investment.
The Good Habits (The Longevity Protocol)
1. The Water Flosser is Non-Negotiable
String floss is great, but it often misses the “cuff” of tissue around the implant abutment. A water flosser (oral irrigator) with a soft rubber tip delivers a pulsating stream of water or antimicrobial rinse directly into the sulcus (the collar of gum around the implant). This flushes out food debris and disrupts the biofilm that causes peri-implantitis.
2. The Right Tools: Titanium Scalers Only
If your hygienist reaches for a metal instrument, stop them. Politely remind them you have an implant. Stainless steel will gouge the titanium abutment. Those scratches are a bacterial magnet. Implants require plastic, graphite, or gold-tipped scalers. If your dental office doesn’t stock these, find one that does.
3. The Night Guard (Your Insurance Policy)
Even if you don’t think you grind your teeth, the vast majority of adults do some degree of nocturnal clenching. For an implant patient, a custom-fitted night guard is not an optional accessory; it is the equivalent of a surge protector for your computer. It dissipates the crushing force of grinding across all teeth, preventing the implant from taking a lethal overload.
The Bad Habits (The Implant Killers)
1. Using Teeth as Tools
You know this one. Opening a bag of chips. Holding a fishing line. Biting a price tag off a new shirt. With natural teeth, the ligament provides feedback—you can “feel” when you are biting too hard. With an implant, you feel nothing until you hear a crack. That crack might be the crown, or worse, the bone.
2. Chewing Ice
Ice is hard, but more importantly, it is cold. Repeated thermal shock (hot coffee followed by ice water) causes the porcelain crown and the cement layer to expand and contract at different rates. Over time, this leads to micro-fractures in the porcelain. It looks like a hairline crack that eventually leads to a catastrophic “popcorn” fracture of the crown surface.
3. Neglecting the Annual “Implant Check”
A standard dental check-up looks for cavities. Implants do not get cavities. Therefore, the check-up for an implant is different. The dentist must take a Periapical X-ray annually to measure the bone level around the threads of the implant. They are looking for a “saucerization” effect—a smooth dip in the bone level. Catching 1mm of bone loss early allows for non-surgical intervention (deep cleaning, antibiotics). Catching 5mm of bone loss late means surgery or implant removal.
Material Science: Does the Type of Implant Matter?
When you search for dental implants how long do they last, you might stumble upon debates about “Brand A” versus “Brand B.” While surgeon skill trumps brand name every time, the materials used in your crown do have a significant impact on the lifespan of the visible tooth.
-
Titanium vs. Zirconia Fixtures: Traditional implants are titanium. There are now “metal-free” zirconia implants (white in color). Zirconia is extremely hard and hypoallergenic. However, titanium has a 40-year track record of osseointegration. Zirconia has a shorter long-term data set (approx 10-15 years). For longevity data, titanium remains the gold standard.
-
Crown Material Comparison:
-
Porcelain Fused to Metal (PFM): Durable but ugly in the long run. The gum may recede slightly, revealing a dark gray line at the gum margin. Lifespan: 10-15 years.
-
Layered Zirconia: Beautiful, natural-looking translucency. However, the layers of porcelain can chip off the solid zirconia core if you grind heavily. Lifespan: 10-15 years.
-
Monolithic (Solid) Zirconia: This is the tank of dental crowns. It is a solid block of zirconia with no porcelain layers to chip. It is incredibly strong but slightly less “life-like” in color depth. For back molars and heavy grinders, this is the material that answers the question dental implants how long do they last with the highest number. Lifespan: 20+ years.
-
Special Considerations: Age, Location, and Health
The longevity of an implant is not uniform across all mouths or all patients. Context is everything.
Age and Implant Longevity
Some people wonder, “Am I too old for an implant to last?” The answer is surprisingly counter-intuitive. Implants placed in a healthy 70-year-old have a higher success rate than implants placed in a healthy 30-year-old. Why?
-
Lower Expectations of Force: A 70-year-old is far less likely to be eating corn nuts, chewing on ice, or playing contact sports than a 30-year-old. The implant experiences less physical trauma.
-
Stable Occlusion: Older adults’ teeth have worn into a stable, comfortable bite pattern. Younger adults have more dynamic, changing bites.
Location in the Mouth
-
Front Teeth (Anterior): These implants last forever in terms of the fixture, but the crown has a high replacement rate. Why? Esthetics. Gums recede naturally over decades. If the implant crown was placed when you were 35, by age 65, it may look “long in the tooth” compared to the receded gum line. You will likely replace the crown for cosmetic reasons long before it breaks.
-
Back Molars (Posterior): These are the workhorses. They experience the highest biting forces. Fixture survival is excellent, but crown fracture and screw loosening are common. You might need a new abutment screw every 7-10 years on a back molar implant.
Medical Conditions
-
Osteoporosis Medications (Bisphosphonates): This is a critical, non-negotiable conversation with your surgeon. Medications like Fosamax, Actonel, or Boniva (and especially IV forms like Zometa or Prolia) alter bone metabolism. While they make bones denser, they can sometimes impair the jawbone’s ability to heal around a surgical site, leading to a rare but serious condition called Medication-Related Osteonecrosis of the Jaw (MRONJ) . Implants can still be placed successfully, but the risk profile changes dramatically. The implant might not last long if the surrounding bone dies.
-
Radiation Therapy: If you have had radiation to the head and neck for cancer treatment, the blood supply to the jawbone is permanently compromised. Implants can still work with Hyperbaric Oxygen therapy, but the long-term survival rate drops from 95% to roughly 75-85%.
The Maintenance Schedule: A Realistic Roadmap to 30+ Years
Since you want a definitive guide on dental implants how long do they last, here is a practical, year-by-year maintenance blueprint. This is not the “ideal world” schedule; this is what actually works for patients who keep their implants for life.
| Timeframe | Action Items | Why This Matters for Lifespan |
|---|---|---|
| Daily | Water floss around abutment. Use electric toothbrush with soft head. | Disrupts biofilm before it calcifies into tartar. |
| Weekly | Check for “wiggle.” Place finger on crown and try to move it. Any movement = emergency call to dentist. | A loose implant that goes untreated for 1 week will need surgery. One treated in 24 hours may just need a screw tightened. |
| Every 3-4 Months | Professional hygiene visit with implant-safe instruments. | Standard 6-month recall is too long for many implant patients. Peri-implantitis bacteria double every 4-6 hours. |
| Annually | Periapical X-ray (PA) of each implant. Bite force analysis. | Early detection of bone loss is the only way to stop late failure. |
| Every 5 Years | Remove and replace the abutment screw (if screw-retained). | Prevents screw fatigue fracture inside the implant body. |
| Every 15 Years | Evaluate crown for wear. Replace if margins are open. | Prevents decay on adjacent natural teeth and reduces risk of porcelain fracture. |
The Economic Reality: Total Cost of Ownership
Let’s talk about money, because the question dental implants how long do they last is fundamentally a financial one. You are calculating Return on Investment (ROI).
Scenario A: The 3-Unit Bridge
-
Year 1: $3,500 cost.
-
Year 10: Bridge fails due to decay on anchor tooth. Tooth needs root canal and new crown. Total new bridge cost: $4,200.
-
Year 20: Second anchor tooth fails. Implants now needed for 3 missing teeth.
-
Total 20-Year Cost: $15,000+
Scenario B: The Single Implant and Crown
-
Year 1: $4,500 cost (Implant surgery + abutment + crown).
-
Year 5: Screw tightening ($150).
-
Year 15: New Crown ($1,500).
-
Total 20-Year Cost: $6,150
The implant scenario saves you roughly $9,000 over 20 years and preserves the health of your neighboring teeth. The longer the implant lasts, the wider that financial gap becomes. If the implant fixture lasts 40 years, the cost per year of use becomes pennies on the dollar compared to the endless cycle of bridge replacement.
Common Myths About Implant Longevity (Debunked)
Myth 1: “Once it’s in, it’s in for good. I don’t need to see the dentist.”
Reality: This is the fastest way to lose an implant. Implants require more meticulous care than natural teeth, not less. Ignoring an implant is like never changing the oil in a luxury car. It will run great until the engine seizes catastrophically.
Myth 2: “Dental implants last forever.”
Reality: The titanium root can last forever. The crown on top will not. Expect to budget for crown replacement between years 10 and 20.
Myth 3: “Implants can’t get cavities, so they can’t fail.”
Reality: They do not get cavities (dental caries). They get Peri-implantitis (gum and bone infection). It is the same result—tooth loss—but a different disease process. In fact, peri-implantitis can destroy bone faster than gum disease destroys bone around a natural tooth.
Myth 4: “If it fails, I can just get another one.”
Reality: You can try. But when an implant fails, it leaves behind a crater in the jawbone. Bone grafting is required to fill the hole. The second implant has a slightly lower success rate than the first. It is always better to save the first one.
Warning Signs You Should Never Ignore
Since you are now an informed patient seeking the truth about dental implants how long do they last, you need to know the early warning radar. Implant failure is rarely a sudden explosion. It is usually a slow leak.
-
The “Funny Taste”: A metallic or salty taste around the implant site suggests a micro-leak of blood or fluid from inflammation under the gum.
-
Thread Exposure: Look in the mirror. If you see gray metal threads where there used to be pink gum, call now. This is recession. It is irreversible without surgery.
-
Floss That Shreds or Smells: If the floss shreds every time you go around that tooth, the margin of the crown is open or rough, trapping bacteria and food.
-
Pain When Chewing (Not Hot/Cold): An implant has no nerve, so it shouldn’t hurt. Pain on biting down indicates pressure on the bone interface. It means the bone is inflamed or the screw is loose.
The Future of Longevity: What’s on the Horizon?
The implants being placed today in 2026 have a different longevity outlook than those placed in 1996. Technological advancements are pushing the boundaries of what “long-lasting” means.
-
Surface Technology: Modern implants have hydrophilic surfaces (water-loving). This means the blood clot adheres better and bone cells migrate faster. Osseointegration that used to take 6 months now takes 3-6 weeks. This reduces early failure risk significantly.
-
Guided Biofilm Therapy: New air-polishing devices using erythritol powder can clean the implant surface without scratching it, removing biofilm 10x more effectively than hand scaling.
-
Genetic Testing: We are on the cusp of using simple saliva tests to identify patients genetically predisposed to aggressive peri-implantitis (high Interleukin-1 levels). These patients can then be put on a 3-month recall schedule from day one to prevent late failure.
Summary of the Article
A dental implant fixture is a permanent replacement for a tooth root with a success rate exceeding 95% over decades, provided it remains free from peri-implantitis. The visible crown, however, is subject to normal wear and typically requires replacement after 15 to 20 years due to chipping or esthetic changes. Ultimately, the lifespan hinges entirely on the patient’s commitment to daily water flossing, annual professional maintenance with specific implant-safe tools, and protecting the investment with a night guard against grinding forces.
Frequently Asked Questions (FAQ)
Q: What is the most common reason an implant fails after 10 years?
A: The most common reason for late failure is Peri-implantitis, which is a bacterial infection of the gums and bone surrounding the implant. It is usually caused by poor oral hygiene and lack of professional cleanings.
Q: Can I whiten my implant crown?
A: No. Porcelain and zirconia do not respond to whitening gels. The color is permanent. If your natural teeth shift color or yellow over the years, the implant crown may stand out as brighter. This is why many people replace the crown after 15-20 years for esthetic matching.
Q: Does the implant warranty mean it will last that long?
A: No. A warranty (typically 5-10 years) covers manufacturer defects in the titanium fixture itself, which are incredibly rare. It does not cover bone loss, gum infection, or crown fracture. The warranty is not a promise of clinical success.
Q: Is it true that an MRI will pull out my implant?
A: No. Dental implants are made of non-magnetic titanium or zirconia. They are completely safe in MRI machines. They may cause a slight “artifact” or blurring on the image directly next to the implant, but they will not heat up or move.
Q: How much does replacing just the crown cost compared to a whole new implant?
A: Replacing just the crown costs between $1,000 and $2,000. Replacing the entire implant (if the fixture fails and needs removal, bone graft, and new surgery) can cost between $4,000 and $6,000. Maintaining the fixture is significantly cheaper.
Additional Resources
For further independent reading on the science of osseointegration and long-term implant outcomes, visit the Foundation for Oral Rehabilitation (FOR): https://www.for.org. This non-profit provides evidence-based information for patients and professionals regarding implant dentistry.
dentalecostsmile
Newsletter Updates
Enter your email address below and subscribe to our newsletter