Dental Implants and Receding Gums: Causes, Solutions, and Prevention
If you are considering dental implants, or if you already have them, you might have noticed something concerning: your gums are shrinking or pulling away from the implant. You are not alone. Gum recession around implants is a common issue, but it is also one that many people do not expect.
Let us be clear from the start. Dental implants are one of the best solutions for missing teeth. They look natural, feel strong, and can last a lifetime. However, they are not magic. They require healthy gums to support them.
When receding gums happen around an implant, it is different from natural tooth recession. With a natural tooth, your gum might grow back a little, or you might need a simple gum graft. With an implant, the stakes are higher. The metal post does not have the same biological seal as a real tooth root.
This guide will walk you through everything you need to know. We will explore why this happens, what you can do about it, and how to prevent it from starting in the first place. No confusing medical terms. No fluff. Just practical, honest advice.
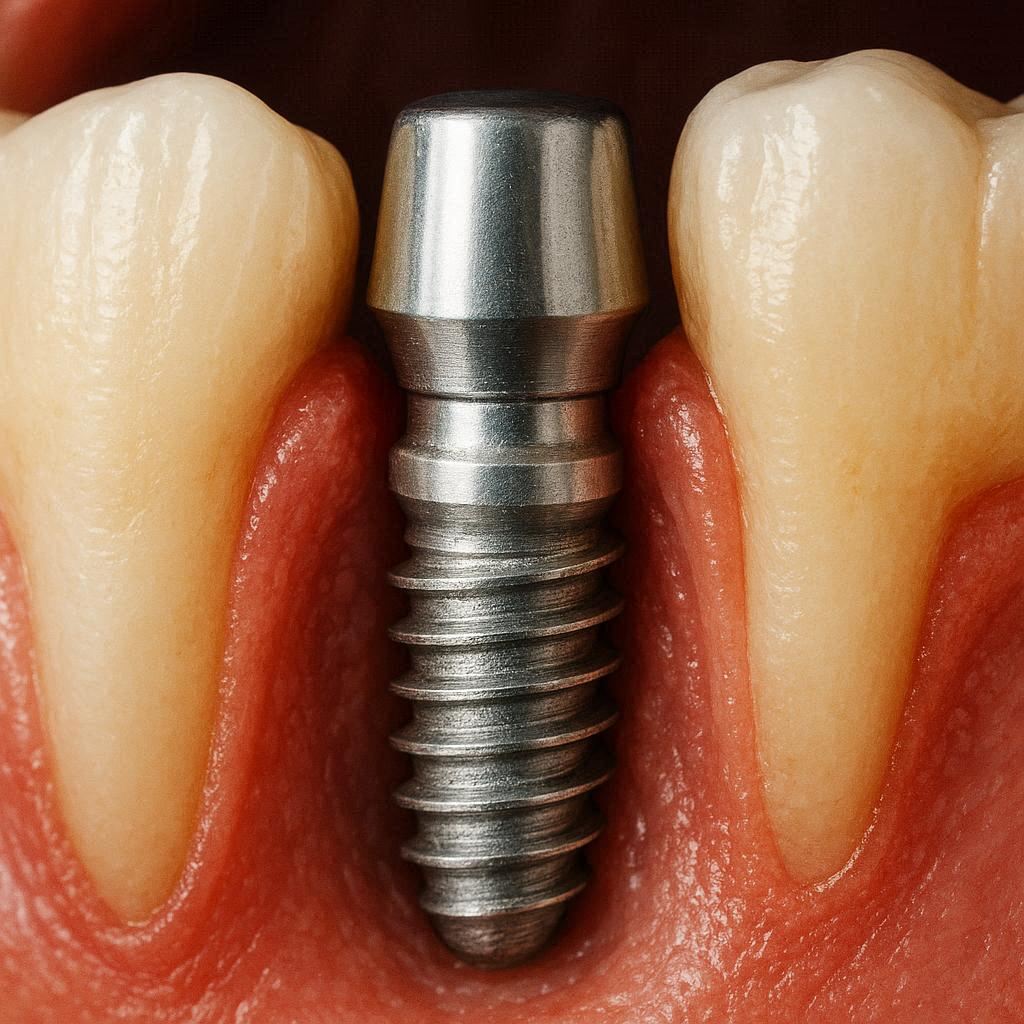
What Exactly Are Receding Gums Around Implants?
To understand the problem, you first need to understand the anatomy of an implant.
A dental implant has three main parts:
- The implant post: A titanium or zirconia screw placed into your jawbone.
- The abutment: A connector piece attached to the top of the post.
- The crown: The artificial tooth you see and use for chewing.
Around a healthy natural tooth, the gum attaches firmly to the tooth’s root. This creates a strong barrier against bacteria.
Around an implant, the gum attaches to the abutment or the implant itself. This attachment is weaker. It is called the “peri-implant seal.” When this seal breaks down due to gum recession, you expose the rough surface of the implant or the abutment.
What does it look like?
- You see more of the implant crown looking longer than before.
- A dark or metallic line becomes visible near the gumline.
- The gum looks thin, red, or swollen in a small area.
- You can feel a notch or rough edge when you run your tongue over the area.
Recession is not just a cosmetic issue. It is a warning sign. Ignoring it can lead to bigger problems like infection or even implant failure.
Why Does Gum Recession Happen Around Implants? (The Real Reasons)
Many people assume that if they pay for a high-quality implant, they will never have gum problems. That is not realistic. Recession happens for several reasons. Some are related to the procedure itself. Others are related to your daily habits.
1. Thin Gum Tissue (Genetic Predisposition)
Some people simply have thin gum tissue. This is called a “thin biotype.” If you have always had delicate, see-through gums, you are more likely to develop recession around an implant.
Think of your gum like a blanket. A thick blanket protects you better. A thin blanket wears out faster.
Dentists can measure your gum thickness before surgery. If you have a thin biotype, they may recommend a connective tissue graft at the same time as the implant placement. This adds bulk to the gum and prevents future recession.
2. Incorrect Implant Placement
This is a major factor. The position of the implant matters a lot.
An implant placed too far to the outside of the bone (toward your cheek or lip) will have thin bone and gum covering it. Over time, that thin bone resorbs (melts away), and the gum follows. Suddenly, the metal implant becomes visible.
An implant placed too shallow may not have enough gum covering the top. An implant placed too deep can trap bacteria, but that causes a different problem (infection), not primarily recession.
The ideal position: The implant should sit in a spot where the bone is thick and the gum can wrap around it like a turtleneck.
3. Peri-Implantitis (The Silent Disease)
This is the big one. Peri-implantitis is an inflammatory condition that affects the gum and bone around an implant. It is similar to periodontitis (gum disease) but happens around implants.
How it leads to recession:
Bacteria build up around the implant. Your immune system attacks these bacteria. In the process, the inflammation destroys the bone holding the implant. As the bone disappears, the gum has nothing to support it. The gum shrinks back, exposing the implant threads.
Peri-implantitis does not happen overnight. It starts as “peri-implant mucositis” – a reversible gum inflammation. If you ignore bleeding gums that brush easily, the disease progresses to bone loss.
Important note: Peri-implantitis is treatable if caught early. But advanced cases may require removing the implant entirely.
4. Aggressive Brushing Habits
You might think that scrubbing your implant hard will keep it clean. It does the opposite.
Natural teeth have a ligament that cushions aggressive brushing. Implants do not have this ligament. They are anchored directly into bone.
When you brush too hard with a stiff toothbrush, you traumatize the gum tissue around the implant. The gum reacts by pulling away. Over time, this creates a visible recession line.
Signs you brush too hard:
- Your toothbrush bristles look frayed after two weeks.
- You see notches or abrasion on your natural teeth.
- Your gums look pale or shiny.
5. Lack of Attached Gums
Your mouth has two types of gums:
- Attached gums: Firm, keratinized tissue tightly bound to the underlying bone.
- Mobile gums: Looser tissue that moves when you pull your cheek.
Implants need a healthy band of attached gums around them. If you only have mobile gums in that area, the implant moves slightly when you chew. This micro-movement irritates the gum, causing it to recede over time.
Some dentists check for this during your implant evaluation. If you lack attached gums, they can perform a simple graft to create it before placing the implant.
6. Smoking and Tobacco Use
Tobacco is terrible for gum health. It constricts blood vessels. Less blood flow means less oxygen and fewer nutrients reaching your gum tissue.
Smokers have thinner, paler gums. These gums are more prone to recession. Also, smoking weakens your immune response to bacteria. If you develop peri-implantitis as a smoker, you will lose bone and gum much faster than a non-smoker.
7. Teeth Grinding (Bruxism)
Do you grind or clench your teeth at night? You might not even know it.
Grinding puts excessive force on your implant. Unlike a natural tooth, an implant has no shock-absorbing ligament. All that force transfers directly to the gum and bone.
This constant micro-trauma can cause the gum to recede. In severe cases, it can even fracture the implant crown or loosen the abutment screw.
Signs of grinding:
- Waking up with a sore jaw or headache.
- Flattened, worn-down natural teeth.
- Your partner hears grinding noises at night.
How Serious Is Gum Recession Around Implants?
Let us be honest. The seriousness depends on how much recession has occurred.
Mild recession (1-2 mm):
You notice a small gap between the gum and the crown. There is no bone loss. The implant is still healthy. This is mostly a cosmetic concern. However, it can trap food and bacteria, so you need to keep it extra clean.
Moderate recession (3-4 mm):
You can see the rough surface of the implant or the abutment. There may be some bone loss visible on an X-ray. Bacteria can colonize the exposed rough surface easily. This increases your risk of peri-implantitis.
Severe recession (5+ mm or exposing threads):
This is an emergency. The implant is losing its support. You may see bleeding, pus, or feel mobility (the implant moves). Without treatment, the implant will fail.
The bottom line: Do not ignore even mild recession. It is easier to treat early.
Treatment Options for Receding Gums Around Implants
Good news: You have options. The best treatment depends on the cause and severity of the recession.
We will break this down into three categories: non-surgical, surgical, and extreme cases.
Non-Surgical Treatments (For Early Recession)
These work best when you catch the problem early, before significant bone loss occurs.
1. Professional Cleaning and Debridement
A dentist or hygienist uses special instruments (plastic or titanium, never metal scalers) to clean around the implant. They remove bacterial buildup from the exposed surface.
They may also use an ultrasonic scaler with a plastic tip. This is gentle but effective.
2. Laser Therapy
Dental lasers can remove inflamed gum tissue and kill bacteria without cutting your gums. Lasers also stimulate some healing in the surrounding tissue.
Laser treatment is painless for most people. It takes one or two short visits. It does not regrow gum, but it can stop recession from getting worse.
3. Chlorhexidine or Antimicrobial Rinses
Your dentist may prescribe a chlorhexidine mouthwash. You use it for two weeks. This reduces the bacterial load around the implant.
Important: Do not use chlorhexidine for more than two weeks without a break. It can stain your teeth and alter your taste perception.
4. Switching to a Soft Toothbrush and Correct Technique
This is simple but powerful. Switch to a soft or extra-soft toothbrush. Hold it like a pencil. Use small, circular motions at a 45-degree angle toward the gum. Do not scrub.
Many cases of mild recession stop progressing just by changing brushing habits.
Surgical Treatments (For Moderate to Severe Recession)
If non-surgical methods do not work, or if the recession is already significant, surgery may be necessary.
1. Apically Positioned Flap + Bone Graft
This sounds scary, but it is a common procedure.
The dentist gently lifts your gum away from the implant. They remove any inflamed tissue or granulation tissue. If there is bone loss, they place a bone graft material around the exposed implant threads. Then, they reposition the gum at a higher level and suture it in place.
Recovery: Mild swelling for 2-3 days. Soft food diet for one week. Full healing takes 4-6 weeks.
Success rate: High, if the implant is otherwise stable and you have good hygiene.
2. Connective Tissue Graft
This is for cases where you simply do not have enough gum thickness. The dentist takes a small piece of connective tissue from the roof of your mouth (palate). They suture it around the receded area on the implant.
This adds bulk to the gum. It covers the exposed metal. It also makes the area more resistant to future recession.
Drawback: You have two healing sites – your palate and the implant area. The palate can be sore for a week. Salt water rinses help.
3. Guided Bone Regeneration (GBR)
When the recession is caused by significant bone loss, you need to rebuild the bone first. GBR uses a membrane and bone graft material to encourage your body to grow new bone around the implant.
After the bone heals (4-6 months), the dentist can then address the gum recession.
4. Implantoplasty
This is a specialized procedure for implants with exposed rough surfaces. The dentist uses small burs and polishers to smooth the exposed part of the implant. A smooth surface is harder for bacteria to stick to.
After smoothing, the gum may reattach slightly. Or the dentist may perform a graft to cover the smooth surface.
Warning: Implantoplasty weakens the implant slightly. It is only suitable for implants that are not under heavy biting forces.
Extreme Cases: When the Implant Must Be Removed
Sometimes, you cannot save the implant. This is the case when:
- More than 50% of the bone around the implant is lost.
- The implant is mobile (moves when you push on it).
- You have persistent pus or abscesses despite treatment.
- The implant is fractured.
Removing an implant is usually straightforward. The dentist uses a special drill to unscrew it or a trephine drill to core it out. You will feel pressure but not pain.
After removal, the socket is cleaned out. A bone graft is placed. You wait 4-6 months for healing. Then, you can consider a new implant or another option like a dental bridge.
Honest truth: A removed implant is not a failure of you as a patient. Sometimes implants fail due to factors no one can control. The key is to learn from it and plan the next step carefully.
Prevention: The Best Medicine for Your Implants
Preventing gum recession is much easier than treating it. And most prevention is simply good daily care.
Daily Home Care Routine
Here is a realistic routine that takes 3-4 minutes per day.
Morning:
- Brush with a soft or extra-soft toothbrush for 2 minutes. Use a non-abrasive toothpaste (avoid baking soda or charcoal products).
- Use a water flosser on a low setting. Aim the water stream directly at the gumline around your implant. Do not blast it at full power.
- Rinse with plain water or a non-alcoholic mouthwash.
Evening:
- Floss with superfloss or implant-specific floss. This floss has a stiff end to thread between teeth and a spongy middle to clean the implant surface.
- How to floss: Make a “C” shape around the implant. Gently rub up and down 2-3 times. Do not snap the floss down into the gum.
- Use a small interdental brush (like a proxy brush). Gently insert it between the implant and the adjacent tooth. Twist it 2-3 times. This cleans the concave surface where floss misses.
- Brush for 2 minutes as usual.
- Optional: Use a water flosser again for 30 seconds.
What to avoid:
- Toothpicks (they can damage the gum seal).
- Metal scalers or sharp objects.
- Whitening strips or abrasive whitening toothpaste (they can roughen the crown surface).
Professional Maintenance Schedule
You cannot do this alone. Your dentist or hygienist needs to see you regularly.
| Risk Level | Recommended Recall Interval | What They Do |
|---|---|---|
| Low risk (healthy gums, non-smoker, good hygiene) | Every 12 months | Examine, clean with plastic instruments, take X-rays every 2-3 years. |
| Moderate risk (history of gum disease, thin gums, occasional smoker) | Every 6 months | Full exam, cleaning, check pocket depths, early detection of issues. |
| High risk (prior peri-implantitis, heavy smoker, uncontrolled diabetes) | Every 3-4 months | Deep cleaning around implants, laser therapy if needed, close monitoring of bone levels. |
Lifestyle Changes That Protect Your Gums
Quit Smoking
We know this is hard. But for your implant, it is essential. Smokers have a 3x higher risk of peri-implantitis and recession.
If you cannot quit completely, reduce your use. Every cigarette you skip helps restore blood flow to your gums.
Manage Teeth Grinding
If you grind your teeth, get a nightguard (occlusal splint). Do not buy a cheap over-the-counter boil-and-bite guard. Those are too soft and can worsen clenching. Get a hard or hard-soft hybrid guard from your dentist.
Wear it every night. Even if you think you only grind sometimes. The forces from one night of severe grinding can cause irreversible damage.
Control Medical Conditions
- Diabetes: High blood sugar weakens gum healing. Keep your HbA1c below 7% if possible. Let your dentist know your latest numbers.
- Osteoporosis: Some medications for osteoporosis (bisphosphonates like Fosamax) can affect bone healing. Tell your dentist all medications you take.
- Autoimmune diseases: Conditions like rheumatoid arthritis or lupus can affect gum health. Work with your rheumatologist to keep inflammation under control.
Realistic Expectations: What Can and Cannot Be Done
Let us set honest expectations.
What CAN be improved or fixed:
- Mild to moderate recession without bone loss: Usually reversible with better hygiene and sometimes a small gum graft.
- Exposed implant threads: Can be covered with a connective tissue graft in most cases.
- Peri-implantitis in early stages: Can be arrested with deep cleaning, lasers, and antibiotics.
- Cosmetic appearance of receded gums: Greatly improved with gum grafting or pink porcelain (a pink ceramic added to the crown).
What CANNOT be done:
- Regrow lost gum tissue naturally: Your gum will not grow back on its own. You need a graft.
- Reverse severe bone loss: Once the bone is gone, it requires surgery (bone graft) to rebuild. It will not come back with mouthwash or vitamins.
- Guarantee success: Every surgery has risks. Even with the best dentist and perfect home care, an implant can still develop recession years later.
- Make a failing implant stable again: If the implant is mobile or has lost more than half its bone support, it is time to remove it. Trying to save it often leads to more bone loss and a worse outcome for a future implant.
Comparative Table: Natural Tooth vs. Implant Gum Recession
Understanding the differences helps you know what to expect.
| Feature | Natural Tooth Recession | Implant Gum Recession |
|---|---|---|
| Attachment | Strong ligament (PDL) attaches gum to tooth. | Weak seal; gum attaches directly to abutment. |
| Sensitivity | Often cold/hot sensitivity due to exposed root. | No sensitivity (implant has no nerve). |
| Risk of infection | Moderate (root cavities possible). | High (peri-implantitis can destroy bone quickly). |
| Regrowth potential | None without surgery. | None without surgery. |
| Treatment complexity | Lower. Simple gum graft works well. | Higher. May need bone graft + gum graft. |
| Prognosis if untreated | Tooth may loosen but lasts years. | Implant failure within 1-3 years. |
| Cost of treatment | 600−2,000 for gum graft. | 1,500−5,000 depending on bone loss. |
Step-by-Step Guide: What to Do If You Notice Recession Today
Do not panic. Follow this plan.
Step 1: Observe and document (Day 1)
- Take a photo of your implant and gums with your phone.
- Note any bleeding, pain, or bad taste.
- Check if the implant feels loose when you wiggle it gently with a clean finger.
Step 2: Improve your hygiene immediately (Day 1)
- Switch to a soft toothbrush.
- Stop flossing aggressively. Use gentle, up-and-down motions.
- Rinse with warm salt water (1 teaspoon salt in 1 cup warm water) twice daily.
Step 3: Call your dentist (Day 1 or 2)
- Explain exactly what you see: “My gum is pulling away from my lower right implant. I see metal. No pain.”
- Ask for a “peri-implant evaluation.” Do not let them just look. Ask them to probe gently and take an X-ray (periapical or CBCT if needed).
Step 4: Attend the appointment (Within 1-2 weeks)
- Do not wait months. Recession progresses.
Step 5: Follow the treatment plan
- If they say “just watch it,” ask for a specific recall interval. “Watch it for 3 months” is fine. “Watch it indefinitely” is not.
Step 6: Modify long-term habits
- Get a nightguard if you grind.
- Quit smoking (ask your dentist for resources – many offer smoking cessation programs).
- Schedule your next cleaning before you leave the office.
Frequently Asked Questions (FAQ)
1. Can gum recession around an implant fix itself?
No. Unlike a small cut in your mouth, receded gum tissue will not grow back on its own. Once the gum has pulled away, it stays away unless you have a surgical procedure like a gum graft. The only exception is very mild recession caused by aggressive brushing. If you stop the trauma, the gum may stabilize but will not fully regrow.
2. How common is gum recession after dental implants?
It is more common than most dentists advertise. Studies suggest that up to 30-50% of implant patients experience some degree of gum recession within 5-10 years. Most cases are mild (1-2 mm) and cosmetic. Moderate to severe recession happens in about 5-10% of cases, usually due to thin gums, smoking, or peri-implantitis.
3. Will my dental insurance cover treatment for receding gums around implants?
It depends on your plan. Most dental insurance plans cover gum graft surgery for natural teeth. For implants, some plans consider it “cosmetic” if the implant is otherwise healthy. However, if the recession is caused by peri-implantitis (a disease), many plans will cover treatment. Always call your insurance company before scheduling surgery. Ask for the CDT codes (D4266 or D4267 for gum grafts) and verify coverage.
4. Can I get a gum graft if I already have an implant?
Yes, absolutely. A connective tissue graft can be performed around an existing implant. The success rate is slightly lower than around a natural tooth (about 80-90% vs. 95%+), but it is still a very effective procedure. The key is that the implant itself must be stable (not mobile) and free of active infection.
5. How do I know if my implant is failing due to recession?
Recession alone does not mean implant failure. Look for these red flags:
- The implant feels loose or moves when you push it.
- You see a dark line around the gum that bleeds easily.
- You have a persistent bad taste or pus when you press on the gum.
- An X-ray shows bone loss around more than half of the implant length.
If you have none of these signs, your implant is likely healthy despite the recession.
6. What is the best toothbrush for implants?
The best is an ultra-soft manual toothbrush or an electric toothbrush with a pressure sensor and a “sensitive” brush head.
- Manual: Look for “extra soft” or “ultra soft” on the package. Brands like GUM, Nimbus, or Dr. Collins are good.
- Electric: Oral-B iO or Sonicare with a sensitive mode. These have pressure sensors that light up red if you brush too hard. Do not use a “whitening” or “firm” brush head.
7. Can receding gums cause me to lose my implant?
Yes, if left untreated. Recession exposes the rough surface of the implant. Bacteria colonize this surface. This leads to peri-implantitis (bone loss). As bone loss progresses, the implant loses support. Eventually, the implant becomes loose and falls out or must be removed. This process takes months to years, so early detection saves implants.
8. Are some people more at risk for gum recession around implants?
Yes. You are at higher risk if you:
- Have thin, delicate gum tissue (thin biotype).
- Have a history of gum disease (periodontitis).
- Smoke or use tobacco.
- Have uncontrolled diabetes.
- Grind your teeth.
- Received your implant from a dentist who did not check your gum thickness before surgery.
9. How much does it cost to fix receding gums around an implant?
Costs vary widely by location and the severity of the case. Here are average ranges in the US (without insurance):
| Procedure | Cost Range |
|---|---|
| Professional cleaning (peri-implant debridement) | 150−350 |
| Laser therapy | 300−800 per session |
| Connective tissue graft (one implant) | 1,200−3,000 |
| Bone graft + gum graft (combined) | 2,500−6,000 |
| Implant removal | 500−1,500 |
| New implant after removal | 3,000−6,000 |
10. Can a water flosser make gum recession worse?
No, not if used correctly. A water flosser on a high pressure setting can traumatize the gum. Always use the lowest effective setting (start at level 2-3 out of 10). Direct the water at a 90-degree angle to the gum. Do not blast directly into the pocket. Used properly, a water flosser is excellent for implant hygiene because it cleans without physical friction.
Additional Resources
We believe in giving you trustworthy, actionable information. For a deeper dive into peri-implant diseases and prevention, we recommend the following resource:
Link: American Academy of Periodontology – Implants and Peri-Implantitis
This resource is maintained by board-certified periodontists (gum specialists). It includes patient-friendly videos, illustrations, and a “Find a Specialist” tool to locate a periodontist near you.
Conclusion: Three Key Takeaways
Gum recession around dental implants is common but manageable. Early detection and gentle home care can stop most cases from progressing. For advanced recession, modern surgical techniques like gum grafts and bone grafts offer excellent success rates, but the best approach is always prevention through regular professional checkups and daily hygiene.
Disclaimer: This article is for informational purposes only and does not constitute medical or dental advice. Always consult with a licensed dentist or periodontist for a proper diagnosis and treatment plan tailored to your specific situation. Individual results vary, and not all procedures are suitable for every patient.