Dental Code for Miscellaneous: D9999 and Unlisted Procedures
If you have ever looked at a dental bill or a treatment plan and seen a code labeled “miscellaneous,” you probably felt a little confused. You are not alone. In the world of dental billing, the “miscellaneous” code—officially known as D9999—is one of the most misunderstood and misused codes in the entire Current Dental Terminology (CDT) code set.
When a dental office uses a miscellaneous code, it often raises questions. Will insurance cover it? Is it a trick to charge more? Or is it simply the only way to bill for a service that doesn’t have a standard code?
This guide is designed to clear up the confusion. We will walk you through everything you need to know about the dental code for miscellaneous services. Whether you are a patient trying to understand your bill, a dental assistant learning the ropes, or an office manager looking to improve your billing accuracy, this article will serve as your go-to resource.
We will cover what the D9999 code is, why it exists, when it is appropriate to use it, and how to ensure you get paid for legitimate services without triggering audits or denials.
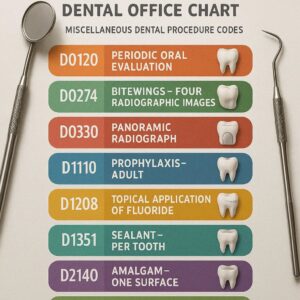
What Exactly is the Dental Code for Miscellaneous (D9999)?
To put it simply, the D9999 code is a placeholder. It is officially titled “Unspecified adjunctive procedure, by report.” In everyday language, it is the code used when a dentist performs a procedure that does not have a specific, predefined code in the CDT manual.
The American Dental Association (ADA) publishes the CDT codes annually. These codes are designed to cover the vast majority of dental procedures, from a routine exam (D0120) to a complex root canal (D3330). However, dentistry is constantly evolving. New technologies emerge, and sometimes a dentist needs to perform a unique service that isn’t listed in the book.
When that happens, the office cannot simply make up a code. They must use D9999 or another “unlisted” code to bill for the service.
The “By Report” Requirement
The most critical part of understanding D9999 is the phrase “by report.” This is not just a formality. It is a requirement.
When a dentist submits a claim with a D9999 code, they cannot just send in the code number and expect payment. They must attach a detailed narrative report to the claim. This report must explain:
-
What the procedure was.
-
Why it was necessary.
-
How much time was spent.
-
What materials or technology were used.
-
Why no other standard code applies.
Think of it like submitting a custom order. You don’t just say “I want a widget.” You have to draw a blueprint.
The Difference Between D9999 and Other Unlisted Codes
It is important to note that D9999 is not the only “miscellaneous” code in the dental world. There are several other unlisted codes that fall under specific categories.
| Code | Category | Description |
|---|---|---|
| D9999 | Adjunctive General Services | Unspecified adjunctive procedure, by report. Used for services not otherwise categorized. |
| D3999 | Endodontics (Root Canals) | Unspecified endodontic procedure, by report. Used for unique root canal treatments. |
| D4999 | Periodontics (Gums) | Unspecified periodontal procedure, by report. Used for unique gum treatments. |
| D5999 | Prosthodontics (Crowns/Bridges) | Unspecified fixed prosthodontic procedure, by report. Used for unique bridge or crown services. |
| D6999 | Oral Surgery | Unspecified oral surgery procedure, by report. Used for unique surgical extractions or implants. |
Important Note: Most insurance companies prefer that you use a category-specific unlisted code (like D3999 for root canals) rather than the general D9999 if the procedure falls within that category. Using the general miscellaneous code when a more specific unlisted code exists can lead to automatic denials.
Why Would a Dentist Use a Miscellaneous Code?
If you are looking at a treatment plan and see a miscellaneous code, it is natural to wonder why the dentist doesn’t just use a “normal” code. In an ideal world, every procedure would have a perfect code. In reality, there are several legitimate reasons why a dentist must resort to D9999.
1. New or Emerging Technology
Dentistry is a field of rapid innovation. Five years ago, a specific laser treatment for gum disease might not have existed. Today, it might be the standard of care for certain patients, yet the CDT codes may not have caught up yet. Until a new code is created, the dentist must use D9999 to bill for these advanced treatments.
2. Complex or Unusual Cases
Sometimes, a patient’s anatomy is unique. A standard extraction code (D7140) assumes a routine tooth removal. But what if the tooth is fused to the bone (ankylosed) and requires an hour of surgical time using specialized burs and techniques? The dentist might bill D9999 with a report to accurately reflect the complexity and time involved, rather than undervaluing the service with a standard code.
3. Adjunctive Services
Adjunctive services are extra procedures that support the main treatment but aren’t always listed. For example:
-
Custom sedation protocols: If a patient requires a specific combination of sedatives that is not covered by the standard sedation codes.
-
Specialized patient education: Extensive, one-on-one education for a patient with severe dental anxiety or special needs that goes beyond the standard “patient education” code.
-
Third-party coordination: Coordinating care with a physician, oncologist, or orthodontist in a complex medical case that requires significant time outside of the appointment.
4. Non-Clinical Time
Insurance codes are typically designed for chairside procedures. However, there are times when a dentist spends significant time on a patient not in the chair. This might include:
-
Reviewing complex medical histories with a patient’s primary care physician.
-
Creating a detailed treatment plan for full-mouth rehabilitation that takes hours to design.
-
Managing a post-operative emergency after hours.
If the dentist wishes to be compensated for this professional time, and no standard code applies, D9999 may be the only option.
How Insurance Companies Handle D9999
This is where things get tricky. If you are a patient, you need to know that D9999 is not a standard benefit. Most dental insurance plans are designed to pay for specific codes listed in a fee schedule.
When an insurance company receives a claim with a D9999 code, the process typically goes one of three ways:
Scenario 1: Automatic Denial
Many insurance companies have automated systems that kick out any claim with a D9999 code. The computer does not recognize it as a valid payable code, so it denies the claim immediately. The dental office then has to appeal the denial, often requiring them to fax the narrative report and wait for a human to review it.
Scenario 2: Delayed Review
If the claim is not automatically denied, it goes to a “pending” status. A human claims adjuster will review the narrative report. They will decide one of three things:
-
Approve: They agree the service was necessary and pays the “usual and customary” fee or the dentist’s submitted fee.
-
Downcode: They decide that the service actually matches a standard code. For example, they might say, “This was just a regular extraction,” and pay the standard D7140 rate instead of what the dentist charged.
-
Deny: They decide the service is not a covered benefit under the patient’s contract.
Scenario 3: Reduced Payment
Even if approved, insurance companies rarely pay the full amount billed for a miscellaneous code. They often look for the “least expensive alternative procedure” (LEAT) and pay based on that.
Key Takeaway for Patients: If your dentist recommends a procedure that will be billed under D9999, you should ask for a pre-determination (predetermination of benefits) before the work is done. This is a request sent to the insurance company to confirm if the service is covered and how much they will pay. It saves you from nasty surprises later.
Common Uses for D9999 in Modern Dentistry
To make this concept more concrete, let’s look at real-world scenarios where a dental professional might legitimately use the miscellaneous code.
1. Advanced Laser Therapy
While there are codes for laser soft tissue surgery (D7910), if a dentist uses a specific type of laser for bacterial reduction (LBR) or to treat peri-implantitis (inflammation around implants) in a way not specified by standard codes, D9999 is often used.
2. Dry Socket Treatment (Complex)
There is a code for dry socket treatment (D9930). However, if the dry socket is severe, requires multiple visits, or involves the use of specialized platelet-rich fibrin (PRF) therapy to heal, a dentist might bill D9999 to capture the complexity and advanced materials used.
3. Management of Medical Emergencies
If a patient has a medical emergency in the dental chair—such as a severe allergic reaction, syncope (fainting) that requires advanced intervention, or a diabetic crisis—the dentist may use D9999 to bill for the time and expertise required to stabilize the patient, separate from the dental procedure that was being performed.
4. Custom Oral Appliances
Standard night guards (D9940) and snoring devices (D9941) have codes. However, if a dentist creates a highly complex, multi-functional orthotic appliance for a patient with severe TMJ disorder that combines features of a night guard, a repositioning splint, and a sleep apnea device, there may be no single code to describe it. D9999 allows the dentist to bill for the custom fabrication.
5. Patient Education for High-Risk Cases
For a patient undergoing chemotherapy or radiation therapy to the head and neck, the pre-treatment dental education and preventive protocol are critical. If the dentist spends 90 minutes consulting with the oncologist and educating the patient on radiation caries prevention, this may be billed under D9999, as it goes far beyond a standard D1330 (oral hygiene instruction).
How to Write a Successful “By Report” Narrative
For dental professionals, the success of a D9999 claim hinges entirely on the quality of the narrative report. A vague, one-sentence description will almost certainly result in a denial.
A strong narrative report should read like a short, professional letter. Here is a checklist of what to include:
-
Patient Information: Name, ID number, and date of service.
-
Diagnosis: What is the medical or dental condition that necessitated this procedure?
-
Detailed Description: A step-by-step explanation of what was done. Avoid jargon that a layperson adjuster wouldn’t understand, but be precise.
-
Bad: “Laser treatment.”
-
Good: “Using the BIOLASE Epic X diode laser at 1.5 watts, performed circumferential laser decontamination of implant #19 to treat peri-implantitis. Procedure time: 45 minutes.”
-
-
Time: How long did the procedure take? Time is a critical factor in justifying reimbursement.
-
Materials Used: List specific brands or materials if they are costly (e.g., “PRF tubes,” “Alloderm graft,” “specific laser tip”).
-
Why No Standard Code?: Explicitly state why a standard CDT code does not apply. For example: “There is no specific CDT code for laser decontamination of dental implants using this specific protocol.”
-
Signature: The narrative must be signed by the dentist who performed the procedure.
Sample Narrative Excerpt
“Patient presented with acute pain and swelling around tooth #14. Upon examination, a standard extraction (D7140) was attempted but deemed impossible due to extensive root ankylosis (fusion to bone) and dilacerated roots. A surgical extraction was performed requiring flap reflection, troughing of buccal bone using a surgical handpiece, and sectioning of the root into three pieces. Total surgical time was 75 minutes. Due to the complexity and time exceeding the scope of standard extraction codes (D7210, surgical extraction), this claim is submitted under D9999. A standard code does not accurately represent the complexity, time, or skill required for this procedure.”
Risks and Pitfalls of Using D9999
While D9999 is a necessary tool, it is also a red flag for insurance auditors. Overuse or misuse of miscellaneous codes can lead to serious consequences for a dental practice.
1. Audits
Insurance companies routinely audit providers who use high volumes of unlisted codes. If a practice uses D9999 frequently without solid justification, it may trigger a full audit of all claims, which is time-consuming and stressful.
2. Contract Violations
If a dentist is in-network with an insurance company, they have a contract that stipulates they will bill accurately. Using D9999 to bypass fee schedules (e.g., billing D9999 for a routine extraction just to get paid more than the contract allows) is considered fraud. It can result in termination from the insurance network or even legal action.
3. Patient Dissatisfaction
Patients often do not understand why a “miscellaneous” charge appears on their bill. If insurance denies it, the patient is left holding the balance. This can lead to frustration, negative online reviews, and a breakdown in trust between the patient and the practice.
4. Delayed Cash Flow
Because D9999 claims require manual review, they take much longer to process than standard claims. A practice might wait 60 to 90 days for payment, which can disrupt cash flow.
A Patient’s Guide to Handling D9999 on Your Bill
If you are a patient and you see a miscellaneous code on your treatment plan or explanation of benefits (EOB), here is a step-by-step approach to handling it without panic.
Step 1: Ask Questions Before Treatment
Before the dentist starts any work, ask:
-
“Why does this procedure require a miscellaneous code?”
-
“Is there a standard code for this procedure?”
-
“Have you sent a pre-determination to my insurance?”
Step 2: Understand Your Financial Responsibility
If you are in an in-network practice, the dentist typically cannot charge you more than the contracted rate for standard codes. However, for D9999, there is often no contracted rate. You may be responsible for the full fee. Ask the office manager to estimate your out-of-pocket cost based on similar procedures.
Step 3: Review Your EOB Carefully
When the insurance company processes the claim, you will receive an EOB. Look for:
-
Allowed Amount: Did they assign a dollar value?
-
Remark Codes: Look for messages like “Procedure code not covered” or “Missing documentation.”
-
Patient Responsibility: Is the balance showing as yours, or is the provider writing it off?
Step 4: Appeal if Necessary
If your insurance denies the claim, you have the right to appeal. Work with your dental office to get the narrative report and any supporting x-rays or photos sent to the insurance company. Often, a denial is simply due to the automated system not seeing the attached report.
Alternatives to the Miscellaneous Code
Before reaching for D9999, a wise dental biller will exhaust all other options. Sometimes, there is a better way to bill that ensures faster payment and less hassle.
1. Code Gapping
Code gapping is using a standard code that is the closest match to the procedure, even if it isn’t perfect. For example, if a dentist does a complex soft tissue graft, they might use D4266 (guided tissue regeneration) instead of an unlisted code if it loosely fits. However, this must be done ethically. You cannot use a code for a service you did not perform.
2. Multiple Units
Sometimes, a standard code allows for multiple units. For example, D9910 (application of desensitizing medicament) can be billed with multiple units if it was applied to multiple quadrants. This avoids needing a miscellaneous code for the same service repeated.
3. Bundled Services
Many dental procedures are “bundled.” This means the global fee includes follow-up visits, adjustments, and some adjunctive care. Before billing D9999 for a post-op visit, check if it is already included in the original procedure’s global period (usually 90 days for major procedures like crowns and implants).
The Future of Miscellaneous Codes
The CDT code set is updated annually by the ADA. Every year, new codes are added, and old ones are revised. Often, these new codes emerge from what was previously being billed under D9999.
For example, in recent years, specific codes have been added for:
-
Silver diamine fluoride application (D1354).
-
Teledentistry consultations (D9995 and D9996).
-
Specific sleep apnea appliances.
This trend suggests that as technology and techniques become mainstream, the need for miscellaneous codes decreases. However, there will always be a need for a “catch-all” code for the truly unique cases that fall outside the norm.
Important Notes for Dental Offices
If you work in a dental office, managing D9999 requires a specific workflow to ensure compliance and profitability.
-
Document Immediately: Do not wait weeks to write the narrative. Document the complexity at the time of service while details are fresh.
-
Use Visuals: Attach photos, x-rays, and intraoral scans to your paper claims or portal submissions. A picture is worth a thousand words—and often worth a thousand dollars in claim approval.
-
Train Front Desk Staff: Your front desk must be able to explain D9999 to patients without causing alarm. A simple script works: “This is a specialized procedure that doesn’t have a standard code. We will send a detailed report to your insurance to explain why it was necessary.”
-
Follow Up: Do not let D9999 claims linger. Set a tickler system to follow up on unprocessed claims after 30 days.
Conclusion
The dental code for miscellaneous services, D9999, is a vital but often misunderstood part of dental practice management. It serves as a safety net, allowing dentists to provide innovative and complex care that falls outside the standard coding structure. However, it comes with significant responsibilities. For the dental team, success with D9999 relies on meticulous documentation, honest reporting, and clear communication with patients. For patients, understanding this code empowers you to ask the right questions, verify coverage beforehand, and navigate your dental benefits with confidence.
While it may seem like a mysterious or risky code, D9999 is simply a tool—one that, when used correctly, ensures that unique dental needs are met and fairly compensated.
Frequently Asked Questions (FAQ)
Q1: Is D9999 a valid dental code?
Yes, D9999 is a valid Current Dental Terminology (CDT) code published by the American Dental Association. It is intended for unspecified adjunctive procedures that must be reported with a detailed narrative.
Q2: Does insurance cover D9999?
It depends on your specific plan. Some plans explicitly exclude unlisted codes. Others will cover them if the dentist submits a compelling narrative report and the procedure is deemed medically necessary. Always request a pre-determination to check coverage.
Q3: Can a dentist charge me anything they want for D9999?
If the dentist is out-of-network, they can set their own fee. If they are in-network, they are typically bound by their contract to charge a “reasonable and customary” fee, but because there is no set fee schedule for D9999, it can vary. You should always agree on the fee in writing before treatment.
Q4: Why did my insurance deny my D9999 claim?
Common reasons include: lack of a narrative report, the service was deemed not medically necessary, the insurance plan excludes unspecified codes, or the adjuster decided the service matched a standard code that is already covered (or not covered) under your plan.
Q5: What is the difference between D9999 and D9995?
D9995 is a specific code for teledentistry—synchronous (real-time) consultations. D9999 is a general miscellaneous code. If the service is teledentistry, you must use D9995 or D9996, not D9999.
Q6: How long does it take to get paid for a D9999 claim?
Because these claims require manual review, they typically take 4 to 8 weeks longer than standard claims. In some cases, it can take up to 90 days for a final determination.
Additional Resource
For the most up-to-date information on dental coding and to verify the latest changes to CDT codes, we recommend visiting the official source:
American Dental Association (ADA) – CDT Code Resources
https://www.ada.org/en/publications/cdt