What Causes Bone Loss Around Dental Implants?
If you have a dental implant—or you’re thinking about getting one—you’ve probably heard the term “bone loss.” And it might sound a little scary.
Here is the honest truth. Dental implants are one of the most successful restoration procedures in modern dentistry. They can last for decades. But like anything natural in your body, they need a healthy foundation. That foundation is your jawbone.
So, what causes bone loss around dental implants? The answer isn’t always simple. It can happen slowly, without any pain. It can also show up suddenly after an infection. The good news is that most causes are preventable or treatable.
In this guide, we’ll walk through every possible reason why bone loss happens around implants. We’ll use clear language, real-world examples, and practical advice. You will learn how to spot early warning signs, how your dentist diagnoses the problem, and what you can do right now to protect your implant.
Let’s start from the beginning.
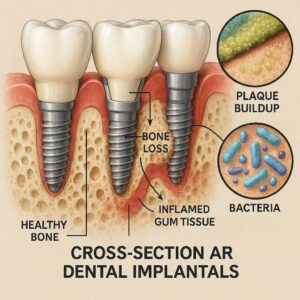
Understanding the Connection Between Implants and Your Jawbone
Before we dive into the causes, let’s look at how a healthy implant should work.
A dental implant is usually a small screw made of titanium. A surgeon places it directly into your jawbone. Over time, your bone grows tightly around that screw. This process is called osseointegration. Think of it like a tree growing roots into the soil. The stronger the roots, the stronger the tree.
Once the implant is stable, your dentist attaches a crown, bridge, or denture on top. Now you can chew, speak, and smile normally.
But here is the key. Your jawbone is alive. It constantly rebuilds itself. It needs stimulation from chewing and biting to stay dense and strong. A successful implant provides that stimulation. Unfortunately, when something goes wrong, your bone can start to melt away.
Important note: Some bone loss is normal immediately after implant surgery. A tiny amount of remodeling happens in the first year. But significant or ongoing bone loss is not normal. It is a sign of a problem.
Now, let’s explore the real causes.
The Number One Cause: Peri-Implantitis
If you remember only one term from this article, remember this: peri-implantitis.
Peri-implantitis is an inflammatory disease. It affects the soft tissue and bone around an implant. In simple words, it is like a severe version of gum disease, but around an implant instead of a natural tooth.
How Does Peri-Implantitis Start?
It almost always begins with bacteria. Your mouth naturally contains hundreds of types of bacteria. When you eat, a sticky film called plaque builds up on your teeth and implants. If you don’t remove plaque thoroughly, it hardens into tartar (calculus).
This bacteria-filled plaque and tartar irritate your gums. First, you might notice peri-implant mucositis. That is a reversible inflammation of the gums only. Your gums look red, swell, and bleed when you brush. At this stage, there is no bone loss yet.
But if the inflammation continues, it spreads deeper. The infection reaches the bone around your implant. Your body’s immune system tries to fight the bacteria. In doing so, it also starts breaking down bone tissue. This is peri-implantitis.
Signs of Peri-Implantitis to Watch For
-
Bleeding when you brush or floss around the implant
-
Red or purplish gums
-
Swelling or tenderness
-
Bad taste or bad breath that won’t go away
-
Pus coming from the gum around the implant
-
The implant feels loose or moves slightly
-
You can see more of the implant screw than before (gums have receded)
Why Peri-Implantitis Is So Dangerous for Bone Loss
Natural teeth have a special fiber attachment called the periodontal ligament. That ligament acts like a shock absorber and can send warning signals. Implants do not have this ligament. They are fused directly to bone. So when bacteria invade, the infection can destroy bone much faster. By the time you feel pain, significant bone loss may have already occurred.
Key fact: Studies show that peri-implantitis affects between 18% and 28% of patients with implants. That is nearly one in four people. But with good home care and regular dental visits, you can greatly reduce your risk.
Other Major Causes of Bone Loss Around Dental Implants
Peri-implantitis is the most common cause. But it is not the only cause. Bone loss can happen even without obvious infection. Let’s look at each cause in detail.
1. Overloading the Implant
Your implant has a specific strength limit. If you put too much pressure on it, the bone around it can break down. This is called mechanical overload.
Imagine carrying a heavy box. If the box is too heavy, the floor beneath you might crack. The same idea applies to your implant.
When does overloading happen?
-
You grind or clench your teeth at night (bruxism)
-
Your dentist places a crown that is too high, so you hit the implant first when biting
-
The implant is too small or too short for the forces in that area of your mouth
-
You use your implant to chew very hard items like ice, hard candies, or bones
Overloading causes microfractures in the bone. Your body tries to repair these fractures, but if the pressure continues, the bone resorbs (melts away) instead.
2. Poor Surgical Placement
Not all implants are created equal. And not all placements are perfect. When a surgeon places an implant, they must consider:
-
The amount and quality of bone available
-
The position of nearby nerves and sinuses
-
The space between the implant and neighboring teeth
-
The angle of the implant
If the implant is placed too close to another tooth root, the bone between them can die. If it is placed at the wrong angle, the chewing forces become uneven. That leads to overloading in one area. If there is not enough bone width, the implant may not have full coverage, and bone loss starts from day one.
This is why choosing an experienced implant dentist matters so much.
3. Smoking and Tobacco Use
Smoking is terrible for bone health. It is also terrible for implant success.
Nicotine and other chemicals in tobacco constrict your blood vessels. Less blood flow means less oxygen and fewer nutrients reaching your jawbone. Your body also has a harder time fighting infections.
A person who smokes has a significantly higher risk of peri-implantitis and bone loss. In fact, some studies show that smokers lose bone around implants at twice the rate of non-smokers.
If you smoke and you are considering an implant, quitting before surgery gives you a much better chance of long-term success. If you already have an implant, reducing or stopping smoking will slow down or stop further bone loss.
4. Uncontrolled Systemic Diseases
Your whole-body health affects your mouth. Some medical conditions make bone loss around implants more likely.
Diabetes is the most common example. When blood sugar is poorly controlled, your body heals slowly and fights infections poorly. High blood sugar also changes the quality of your bone. It becomes softer and more fragile.
Osteoporosis and other bone diseases directly weaken your jawbone. Some medications for osteoporosis, especially bisphosphonates like alendronate (Fosamax), can also cause a rare but serious condition called medication-related osteonecrosis of the jaw (MRONJ). This is when the bone dies and fails to heal after surgery.
Rheumatoid arthritis and other autoimmune diseases cause chronic inflammation. That inflammation can spread to your implant site and trigger bone loss.
Important note: Having one of these conditions does not mean you cannot get an implant. It means you need careful planning. Your dentist should work with your doctor to make sure your condition is well-managed before and after surgery.
5. Lack of Regular Maintenance
Here is a simple truth. Implants are not “set it and forget it.” They need regular care, just like natural teeth.
Many people believe that because an implant is artificial, it cannot get cavities. That is true. But it can still get bone loss. Without professional cleanings, bacteria build up around the implant. Your hygienist uses special instruments that will not scratch the implant surface. Scratches create hiding places for bacteria.
If you skip your dental checkups, small problems grow into big ones. A small amount of bleeding gums becomes peri-implantitis. A tiny bone loss becomes a loose implant.
6. Genetic Factors
Some people are simply more prone to bone loss. Genetics play a role in how your immune system responds to bacteria. Certain genetic markers make you produce more inflammatory chemicals. This means even a small amount of plaque can trigger a strong reaction that destroys bone.
If your parents or siblings have severe gum disease or have lost implants due to bone loss, you may have a higher genetic risk. A dentist can perform a genetic test to check for these markers. But even without a test, knowing your family history helps you be more vigilant.
7. Allergic Reaction to Implant Materials
This is rare. Very rare. But it does happen.
Most dental implants are made of titanium. The vast majority of people have no reaction to titanium. However, a small number of people have a sensitivity or allergy to titanium or the trace metals in the alloy (like aluminum or vanadium).
When an allergic reaction occurs, your body sees the implant as a foreign invader. It launches an inflammatory attack. That inflammation destroys the surrounding bone. Symptoms may include chronic swelling, a burning sensation, skin rashes, or fatigue.
If your implant fails without any clear cause (no infection, no overloading, good placement), your dentist might suspect an allergy. Testing is available through specialized labs.
8. Previous Radiation Therapy
If you have had radiation treatment for head or neck cancer, your jawbone changes. Radiation damages blood vessels and reduces the bone’s ability to heal and fight infection. This condition is called osteoradionecrosis.
Getting an implant in radiated bone is risky. The bone may never integrate with the implant properly. Or it may integrate initially but break down years later. Special protocols like hyperbaric oxygen therapy can improve success rates, but the risk of bone loss remains higher than average.
9. Poor Crown or Prosthesis Fit
The implant itself is only half of the story. The part you see and use—the crown, bridge, or denture—must fit perfectly.
If the crown is loose, it moves slightly when you chew. That movement rubs against the bone connection and causes micro-damage. If the crown has a gap where it meets the gum, bacteria collect in that space. If the crown is too bulky, it traps food and plaque.
A poorly fitting prosthesis creates a cycle. Bacteria cause inflammation. Inflammation causes bone loss. Bone loss changes the fit, making it even worse. By the time you notice, the problem is advanced.
10. Trauma or Injury
A direct blow to the face can damage an implant. Car accidents, sports injuries, falls, or even a punch can transfer enough force to break the bone-implant bond. The bone may crack or crush around the implant. Even if the implant itself does not break, the bone can die from the trauma.
This is less common than other causes, but it does happen. If you have an implant and you experience facial trauma, see your dentist immediately. Even if the implant feels fine, hidden bone damage could appear months later.
A Quick Reference Table: Causes vs. Solutions
| Cause | How It Destroys Bone | Most Effective Solution |
|---|---|---|
| Peri-implantitis | Bacterial infection triggers immune destruction | Professional deep cleaning, improved home care, antibiotics, possibly surgery |
| Overloading | Excessive pressure causes microfractures and bone resorption | Night guard for grinding, adjusting the crown, reducing hard foods |
| Poor placement | Inadequate bone support or uneven forces | Prevention: choose an experienced surgeon. Correction: bone graft or removal |
| Smoking | Reduced blood flow and healing | Quit smoking or reduce significantly |
| Uncontrolled diabetes | Poor healing and chronic inflammation | Manage blood sugar with medical help |
| Lack of maintenance | Undisturbed bacteria grow and spread | Regular professional cleanings every 3–6 months |
| Genetics | Overactive inflammatory response | More frequent cleanings, antimicrobial rinses |
| Titanium allergy | Immune reaction to metal | Replace with zirconia implant after testing |
| Radiation history | Damaged blood supply and bone vitality | Hyperbaric oxygen therapy before implant |
| Poor crown fit | Bacteria trap and micro-movement | Refit or replace the crown |
| Trauma | Physical bone fracture or crush | Immediate dental evaluation and possible bone graft |
How to Know If You Are Losing Bone Around Your Implant
Bone loss is often silent. You cannot see it with your naked eye. You may not feel it until it is advanced. That is why dental X-rays are essential.
Your dentist will take routine X-rays to measure the bone level around your implant. They compare new X-rays to old ones. Any decrease in bone height or thickness is measurable.
Other signs you might notice include:
-
The implant feels different when you bite
-
Food gets stuck around the implant more often
-
Your gum looks like it is “dropping” away from the implant
-
You see a dark triangle of space between the implant crown and the next tooth
-
The crown spins or moves (this is a late sign)
If you notice any of these, do not wait. Call your dentist. Early treatment is simpler, cheaper, and more effective.
Stages of Bone Loss Around Implants
Understanding the stages helps you see why early action matters.
Stage 0 – Healthy
No bleeding, no swelling, stable bone levels on X-ray. The implant is integrated and functions normally.
Stage 1 – Peri-implant mucositis
Gums bleed when probed. No bone loss yet. This is reversible with better cleaning and a professional cleaning.
Stage 2 – Early peri-implantitis
Up to 2 millimeters of bone loss. Bleeding, redness, possibly bad taste. Treatment: deep cleaning (debridement) and antimicrobial therapy.
Stage 3 – Moderate peri-implantitis
Between 2 and 5 millimeters of bone loss. The gum pocket deepens. Pus may appear. Treatment: surgical cleaning, bone graft may be possible.
Stage 4 – Advanced peri-implantitis
More than 5 millimeters of bone loss. The implant becomes mobile. Significant bone structure missing. Treatment: implant removal, extensive bone graft. A new implant may be possible after healing.
Important note: You can stop the progression at any stage except the last one. Once the implant is loose, saving it is very difficult. But even then, the bone can be rebuilt for a future implant.
Realistic Treatment Options for Bone Loss
Treatment depends entirely on the cause and stage. Here is what your dentist might recommend.
Non-Surgical Treatments
These work for early bone loss or peri-implant mucositis.
Professional mechanical debridement: Your hygienist uses special plastic or titanium instruments to clean the implant surface. This removes plaque and tartar without scratching.
Antimicrobial rinses: Chlorhexidine mouthwash kills bacteria around the implant. You usually use it for 2–4 weeks.
Systemic antibiotics: If the infection is aggressive, oral antibiotics like amoxicillin or metronidazole help.
Laser therapy: A dental laser can disinfect deep pockets around the implant. It also stimulates some healing in the surrounding tissue.
Home care coaching: Your dentist or hygienist shows you exactly how to clean around your implant. They may recommend special brushes, floss, or a water flosser.
Surgical Treatments
When bone loss is moderate to advanced, surgery is often necessary.
Open flap debridement: The dentist lifts your gum to expose the implant. They clean the entire surface and remove infected tissue. Then they place the gum back with stitches.
Bone grafting: If you have lost bone, the dentist can add synthetic or natural bone material. This material guides your own bone to grow back over several months. Sometimes a membrane covers the graft to protect it.
Implantoplasty: This is a special procedure for rough-surfaced implants. The dentist smooths the exposed part of the implant so bacteria cannot stick as easily.
Removal of the implant: If the bone loss is too severe or the implant is loose, removal is the only option. The dentist takes out the implant, cleans the socket, and adds bone graft material. After 4–12 months of healing, you may be able to try a new implant.
How to Prevent Bone Loss: A Daily and Long-Term Plan
Prevention is always better than treatment. Here is your practical action plan.
Your Daily Home Care Routine
-
Brush twice a day with a soft toothbrush. Pay special attention to the gumline around the implant.
-
Use an interdental brush (a small brush that fits between teeth). This is often more effective than floss for implants.
-
Floss daily using implant-specific floss or super floss with a stiff end.
-
Consider a water flosser (Waterpik). It flushes bacteria from deep pockets without damaging tissue.
-
Avoid abrasive toothpaste. Some whitening or “tartar control” pastes scratch implant surfaces. Look for low-abrasion formulas.
-
Use an antimicrobial mouthwash a few times per week, not every day (to avoid staining or resistance).
Your Professional Maintenance Schedule
-
See your dentist every 3 to 6 months for checkups and cleanings.
-
Get yearly X-rays to measure bone levels.
-
Ask your hygienist to use implant-safe instruments. Do not be shy about this.
-
If you have a history of gum disease, ask for a periodontal maintenance schedule instead of a regular cleaning.
Lifestyle Changes That Protect Your Bone
-
Stop smoking. If you cannot quit, reduce. Every cigarette you avoid helps.
-
Manage your blood sugar if you have diabetes. Keep your HbA1c below 7%.
-
Wear a night guard if you grind your teeth. Your dentist can make a custom one.
-
Eat a bone-healthy diet. Get enough calcium (dairy, leafy greens, almonds) and vitamin D (sunlight, fatty fish, supplements).
-
Avoid chewing ice, hard candy, or bones. Use your implant like a natural tooth, not like a tool.
When Should You See a Specialist?
Your general dentist can manage most implant maintenance and early problems. But certain situations require a specialist.
See a periodontist (gum and bone specialist) or a prosthodontist (implant restoration specialist) if:
-
You have already lost bone around your implant
-
Your implant is loose or feels different
-
You have a complex medical history (diabetes, osteoporosis, autoimmune disease)
-
A previous implant failed
-
Your general dentist recommends surgical treatment
Do not feel bad about seeking a second opinion. Implants are a significant investment in your health. You deserve expert care.
Frequently Asked Questions (FAQ)
1. Can bone loss around an implant be reversed?
It depends. Early bone loss (less than 2 mm) can often be stopped and even partially reversed with professional cleaning and improved home care. Moderate to severe bone loss cannot be fully reversed, but treatment can prevent it from getting worse. Bone grafting can replace lost bone, but the original bone levels may not return completely.
2. How fast does bone loss happen around implants?
It varies. Some people lose bone slowly over 5–10 years. Others, especially with aggressive peri-implantitis, can lose significant bone in just 6–12 months. This is why regular X-rays are critical.
3. Can a loose implant be tightened?
No. If an implant feels loose, the bone connection is already broken. Tightening the screw on top does not fix the bone loss. The implant usually needs removal and a bone graft.
4. Is bone loss painful?
Not usually. The early and moderate stages are often painless. You might notice bleeding or bad breath before any pain. Pain typically appears only when the infection is severe or the implant is very loose.
5. Can I get a new implant after bone loss?
Yes, in most cases. After removing a failed implant, your dentist will place a bone graft. After 4–12 months of healing, the bone is often strong enough for a new implant. Success rates for second implants are still high, especially if you address the original cause.
6. Do all implants eventually fail?
No. Most implants last 20 years or more. With excellent care, many last a lifetime. Failure rates are around 5–10% over 10 years. Most failures happen in the first year or after 10–15 years due to neglect.
7. How do I clean under an implant bridge?
You will need special tools. A water flosser, super floss with a stiff end, or floss threaders help. Your hygienist can show you the best technique for your specific bridge.
8. Can my dentist tell if I have bone loss without X-rays?
Not accurately. Your dentist can suspect bone loss if your gums bleed heavily, pockets are deep, or the implant moves. But only X-rays show the exact amount of bone loss.
9. Are zirconia implants better for preventing bone loss?
Zirconia implants are metal-free and do not cause allergic reactions. Some studies suggest less plaque buildup on zirconia surfaces. However, they are newer, and long-term data is still limited. Titanium remains the gold standard. Talk to your dentist about which material suits you.
10. Does my insurance cover bone loss treatment?
Dental insurance often covers a portion of peri-implantitis treatment, especially if it is coded as gum disease treatment. However, many plans have annual maximums. You may need to pay out of pocket for bone grafting or implant removal. Always check with your provider.
Additional Resource
For more detailed, science-backed information on dental implants and bone health, visit the American Academy of Periodontology’s patient education page:
👉 https://www.perio.org/for-patients/
This resource offers free brochures, videos, and a specialist locator to help you find a periodontist near you.
Conclusion
Bone loss around dental implants happens for many reasons, but the most common is peri-implantitis—a bacterial infection similar to severe gum disease. Other causes include overloading, smoking, poor placement, uncontrolled medical conditions, and lack of regular maintenance. The good news is that with proper daily cleaning, regular dental checkups, and healthy lifestyle choices, most bone loss is preventable. If you already have bone loss, early treatment can save your implant and your smile.


