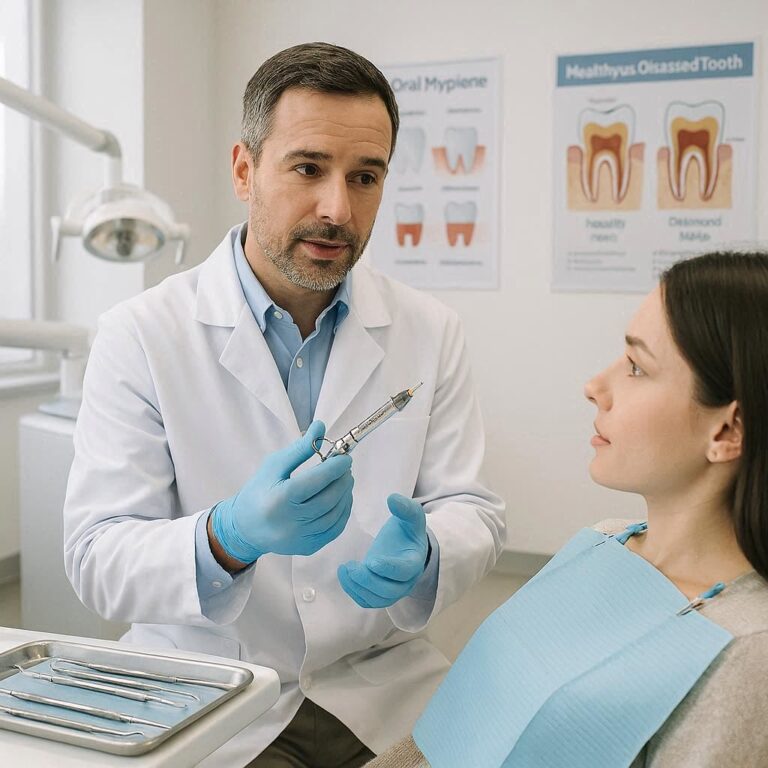
What Does Tooth Cavity Pain Feel Like?
The human mouth is a remarkably sensitive ecosystem. Within the hard, protective shell of enamel lies a living tissue filled with nerves and blood vessels. When that fortress wall gets breached by a cavity, your body sends a very specific set of signals. But if you have never had one before—or if it has been years since you last sat in a dental chair—you might find yourself prodding at a tooth with your tongue in the middle of the night, wondering: What does tooth cavity pain feel like?
It is rarely a one-size-fits-all sensation. The feeling evolves. It starts as a whisper and, if ignored, can escalate into a scream that dominates every waking thought. Some describe it as a subtle annoyance; others compare it to an ice pick driven deep into the jawbone. Understanding the nuances of this pain is not just about satisfying curiosity. It is about early detection. It is about saving your tooth structure, your time, and quite possibly, your wallet.
This comprehensive guide will walk you through every stage of cavity pain. We will explore the sharp zings, the dull aches, and the confusing moments when a cavity hurts less even though the problem is getting worse. By the end of this article, you will have a clear, realistic roadmap of what to expect. You will know when to reach for the sensitivity toothpaste and when to run to the phone to book an emergency appointment.
Let us dive deep into the nerve-wracking, but entirely manageable, world of dental decay sensations.
The Silent Saboteur: Why Cavities Are Masters of Disguise
Before we can accurately describe the pain, we must first understand the crime scene. Tooth enamel is the hardest substance in the human body. It is harder than bone. It is designed to withstand 70 pounds of bite force and a lifetime of hot coffee and ice water. However, enamel has one critical weakness: it has no nerves.
This is the most deceptive part of the cavity process. The decay begins on the surface, often in a microscopic pit or a sticky patch of plaque that you missed while brushing. As bacteria feast on sugar and excrete acid, they erode the mineral structure of the enamel.
The Pain Paradox
Because there are no nerves in the outer shell, you feel absolutely nothing during the early stages of a cavity. You could have a hole the size of a pinhead, or even larger, and remain blissfully unaware unless your dentist spots the shadow on an X-ray. This is why waiting for pain to signal a problem is a dangerous game.
The pain only begins when the decay tunnel crosses the boundary line known as the Dentinoenamel Junction (DEJ) . Once it hits the Dentine, the game changes. Dentine is a yellowish, porous material made up of thousands of microscopic tubules. These tubules act like tiny highways leading directly to the nerve chamber, or Pulp, at the center of the tooth.
-
Enamel: No feeling.
-
Dentine: The Warning Zone.
-
Pulp: The Agony Zone.
The pain you eventually feel is the result of fluid movement within these microscopic tubules irritating the nerve endings deep inside. The deeper the cavity, the shorter the highway, and the more intense the traffic jam of pain signals.
Stage 1: The Early Warning Signs (The Sensitivity Phase)
This is where most people first Google the phrase “what does tooth cavity pain feel like.” You are not in agony, but something is off. This stage is characterized by provoked pain. This means the tooth only hurts when a specific stimulus is introduced. Remove the stimulus, and the pain vanishes like a ghost within seconds.
The “Cold Water Shock”
This is the hallmark of early-to-moderate decay. You take a sip of iced water or a bite of ice cream, and a sharp, electric current seems to jolt through the specific tooth.
“It feels like a quick, bright flash of lightning inside my gum. It’s not a throb. It’s a zap. And then it’s gone.”
Why does cold cause more pain than heat in early stages?
Cold liquids cause the fluid inside those dentine tubules to contract and flow outward rapidly. This sudden shift of fluid yanks on the nerve fibers. Because the decay hasn’t reached the main nerve yet, the nerve is just “irritated” and hypersensitive. Once the tooth warms back up to body temperature, the fluid stops moving, and the pain stops.
How to Distinguish Cavity Sensitivity from Gum Recession Sensitivity:
This is a critical differential diagnosis that even confuses professionals sometimes.
| Feature | Cavity Sensitivity | Gum Recession Sensitivity |
|---|---|---|
| Location | Isolated to one specific tooth, usually in the grooves or between teeth. | Generalized across multiple teeth, usually along the gumline. |
| Visual Clue | You might see a dark spot, white chalky area, or a hole (though often hidden). | The tooth looks long, with a yellowish root surface exposed near the pink gum. |
| Pain Duration | Lingers for 5-10 seconds after the cold is gone (as the fluid re-settles). | Pain stops immediately the second the cold stimulus is removed. |
The Sweet Tooth Sting
This is a unique and often overlooked sign. Have you ever bitten into a piece of sticky caramel, a dried apricot, or even a soft piece of chocolate and felt a dull, aching burn localized to one spot?
That is the osmotic effect in action. The high concentration of sugar pulls fluid out of the dentine tubules. This dehydration of the tubules triggers a nerve response. If you feel a consistent twinge of pain every time you eat something sugary, and only on one tooth, you are likely dealing with a cavity that has already broken through the enamel shell.
“It’s not a sharp stab. It’s more like a deep, nagging ache that starts about five seconds after I swallow the sweet stuff. It makes me want to press my tongue against the tooth really hard to make it stop.”
What It Does Not Feel Like (Yet)
At this stage, the tooth does not hurt spontaneously. You can watch a movie, go for a run, or sleep soundly without any discomfort. The tooth is quiet unless you poke the bear with cold or sugar.
Important Note for Readers: If you are in this stage, you are in a golden window of opportunity. A filling at this point is usually small, requires minimal drilling, and is often painless. Do not wait for it to get worse.
Stage 2: The Escalation (The Lingering Ache)
This is the phase where denial becomes difficult. The cavity has now eaten through the majority of the dentine layer. The protective barrier between the outside world and the tooth’s nerve is razor-thin. The pain changes character from a sharp zing to a deep throb.
The “Hot Drink” Betrayal
Whereas early cavities love the cold, advanced cavities react dramatically to heat. You go to enjoy a warm cup of coffee on a chilly morning, and instead of comfort, you get a wave of oppressive, deep pressure.
This is a more dangerous sign than cold sensitivity. Heat causes the gas and fluid inside the confined tooth chamber to expand. When the nerve inside the pulp chamber is already inflamed (a condition called Pulpitis), this expansion has nowhere to go. It strangles the nerve against the hard walls of the tooth chamber.
The feeling is often described as:
-
A dull, pressurized thud.
-
Like the tooth is “too big” for the socket.
-
A sensation that the tooth is being slowly unscrewed from the jawbone.
The Lingering Effect
This is the single most important clinical sign distinguishing a mild cavity from a serious one. In Stage 1, the pain stopped when you swallowed the ice cream. In Stage 2, you swallow the coffee, and the pain hangs around for a while.
-
Stage 1 (Reversible Pulpitis): Pain lasts 1-10 seconds after stimulus removal.
-
Stage 2 (Irreversible Pulpitis): Pain lasts 30 seconds to several minutes after stimulus removal.
“I drank my tea, and the tooth hurt for a good two minutes afterward. I could feel my heartbeat in my jaw. It wasn’t sharp; it was just this heavy, sickening pressure.”
The Biting Pressure (The “Cracked” Sensation)
As the cavity undermines the enamel ceiling, the tooth becomes structurally weak. You might be chewing something soft, like bread or a banana, and feel a sudden, sharp give and a pain that makes you jump.
What does it feel like?
It feels like you just bit down on a tiny, invisible pebble or a piece of broken glass. You might even hear a faint “click” or “crunch” in your head (this is often the sound of the enamel roof flexing or cracking).
The Release Pain:
Curiously, sometimes the worst pain happens not when you bite down, but when you release the bite. When you bite, you push the cracked pieces together. When you let go, they snap apart, and that sudden separation of the dentine under the cavity sends a massive jolt to the nerve.
A Detailed Sensory Table: Mapping the Stages of Decay Pain
To help you visualize the progression of “what does tooth cavity pain feel like,” refer to this comparative guide. This table outlines the transition from healthy enamel to full-blown infection.
| Stage of Decay | Primary Sensation | Trigger | Pain Duration | What’s Happening Inside |
|---|---|---|---|---|
| Stage 0: Healthy | None. Smooth, cool surface. | N/A | N/A | Enamel intact. |
| Stage 1: Incipient (Watch) | Subtle Catch. Sometimes a rough spot noticed by tongue, but no pain. | Food packing into a groove. | N/A | Demineralization spot (White spot lesion). Reversible with fluoride. |
| Stage 2: Enamel Cavity | Fleeting Sharpness. Like a quick electric shock. | Cold drinks, cold air breath. | 1-2 seconds. Stops immediately. | Decay in enamel only. Dentine not yet exposed. |
| Stage 3: Dentine Cavity | Nagging Ache / Sweet Sensitivity. Dull, radiating burn. | Sugar, Acid (Soda), Cold. | 5-20 seconds. May linger slightly. | Decay into yellow dentine. Tubules exposed. Bacteria present. |
| Stage 4: Deep Cavity | Deep Throb / Pressure. “Tooth feels higher.” Pain on biting. | Hot liquids, Chewing pressure. | Minutes. Requires cold water to soothe. | Decay near pulp. Inflammation of nerve (Pulpitis). |
| Stage 5: Abscess / Necrosis | Relentless Throb / Swelling. Pain spreads to jaw/ear. Feels like a bruise on the bone. | Spontaneous (No trigger needed). Lying down makes it worse. | Constant. Wakes you from sleep. | Nerve is dead. Infection is in the jawbone. |
Stage 3: The Crisis (When the Pain Doesn’t Stop)
We have reached the point where the question “what does tooth cavity pain feel like” takes on a much more desperate tone. This is Spontaneous Pain. The tooth no longer needs coffee or ice cream to hurt. It hurts all on its own. It often hurts worse when you are trying to rest.
The Nighttime Horror
Why do cavities scream loudest at 3:00 AM? This is a cruel trick of biology and physics.
-
Positional Pressure: When you lie flat in bed, blood rushes to your head. This increases the blood pressure inside the already inflamed, confined pulp chamber. The nerve is being squeezed to death by its own blood supply.
-
Lack of Distraction: During the day, work, conversation, and ambient noise distract your brain. At night, the world is silent. There is no competition for your brain’s attention. The pain signal from the tooth becomes the only thing on the channel.
-
The Vicious Cycle: The pain makes you anxious. Anxiety raises your blood pressure further. Higher blood pressure makes the tooth throb harder.
“It feels like there is a tiny, angry heart inside my tooth, and it’s beating out of sync with my own. I can’t get comfortable. I can’t think. I just rock back and forth.”
The Ice Water Cure (A Dangerous Diagnostic Trick)
You may discover a strange, temporary relief measure. If you swish ice-cold water around the tooth, the throbbing stops for about 30 seconds.
Why does this work?
In a severely inflamed tooth with Irreversible Pulpitis, the nerve is swollen and strangled by lack of blood flow. Cold causes vasoconstriction (shrinkage of blood vessels). It temporarily reduces the volume of the pulp, relieving the pressure on the nerve endings.
The Warning: If you find yourself sleeping with a glass of ice water by the bed specifically to numb one tooth, you have crossed the threshold. This is not a fix. This is a symptom that the nerve is dying a slow, painful death. The only solution is a Root Canal Treatment or Extraction.
The Spreading Fire
At this stage, the pain loses its precision. Earlier, you could point to exactly which tooth hurt. Now, the pain feels like it’s coming from your entire lower jaw, or it’s radiating up toward your ear and temple.
This phenomenon is called Referred Pain. The nerve signals are so intense that they overwhelm the local circuitry and spill over into neighboring nerve branches. You might swear you have an ear infection or a sinus headache. It is not uncommon for patients to visit an ENT (Ear, Nose, Throat) doctor, only to be sent to the dentist.
Stage 4: The Deceptive Silence and The Abscess
This is perhaps the most misunderstood chapter in the cavity pain story. There is a moment when the relentless, agonizing throb suddenly… stops.
Many people celebrate this. “Great! The tooth healed itself!”
It did not heal. It died.
What Does Nerve Death Feel Like?
The cessation of pain is often followed by a strange, heavy numbness. The tooth might feel “wooden” or “dead” when you tap on it. You might think the worst is over. You are wrong. The worst is just moving from the inside of the tooth to the outside.
The Birth of an Abscess
The dead nerve tissue (now a rotting soup of protein) becomes a feast for bacteria. The bacteria multiply inside the sealed chamber of the tooth root. They have nowhere to go but out the tip of the root and into the jawbone.
The feeling changes entirely:
-
The “Pimple” on the Gums: You may notice a small, yellow or white bubble on the gum right below the tooth root. It might pop, releasing a foul, salty-tasting liquid. This is a Fistula—a drainage tract for pus.
-
The “Floating Tooth”: As pus and pressure build up in the bone socket, the tooth is literally lifted slightly out of its socket. Every time you close your mouth, this tooth hits first. It feels like the tooth is too long. It feels like you are chewing on a bruise.
-
The Facial Swelling: The pain is no longer a sharp nerve pain. It is a deep, boring, bone pain. It feels like someone is pressing a hot iron against the outside of your jaw. If you look in the mirror and one side of your face looks like you are storing a golf ball in your cheek, you are in a medical emergency.
“I didn’t feel the tooth at all. What I felt was my whole jaw throbbing. It felt like I’d been punched. My face was hot to the touch, and I felt like I had the flu.”
Critical Note: This is not a wait-and-see moment. An abscess is a pocket of infection. If left untreated, this infection can spread from the jaw into the soft tissue spaces of the neck (Ludwig’s Angina) or into the bloodstream (Sepsis). This can close off your airway or become life-threatening.
Comparative Analysis: Cavity Pain vs. Other Dental Pains
Because the mouth is a crowded neighborhood of tissues, it is easy to confuse cavity pain with other conditions. Here is how the sensation differs.
Cavity vs. Cracked Tooth Syndrome
| Aspect | Cavity (Deep) | Cracked Tooth |
|---|---|---|
| Trigger | Temperature (Hot/Cold), Sugar. | Pressure (Biting). |
| Sensation | Dull, lingering ache or throb. | Sharp, inconsistent stab. |
| Consistency | Fairly consistent once symptomatic. | Random. Sometimes it bites, sometimes it doesn’t. |
| X-Ray | Shows dark shadow. | Usually invisible on X-ray. |
Cavity vs. Sinus Pressure (Sinusitis)
| Aspect | Cavity in Upper Molar | Sinus Infection |
|---|---|---|
| Number of Teeth | One specific tooth feels “high” or throbs. | Multiple upper back teeth ache all at once. |
| Positional Change | Lying down makes both worse. | Leaning forward or bending over dramatically increases sinus pain. |
| Nasal Symptoms | Usually none (unless coincidental). | Stuffy nose, post-nasal drip, green/yellow mucus. |
Cavity vs. Gum Disease (Perio Abscess)
| Aspect | Tooth Cavity Abscess | Periodontal (Gum) Abscess |
|---|---|---|
| Pain Source | Deep in the bone socket at root tip. | More superficial, in the gum pocket. |
| Gum Recession | Not necessarily. | Usually present. |
| Tooth Vitality | Tooth is usually dead or dying. | Tooth is often alive (responds to cold). |
The Psychology of Tooth Pain: Why It Feels So Unbearable
To fully answer “what does tooth cavity pain feel like,” we must acknowledge the psychological component. Tooth pain is uniquely debilitating compared to a cut on your arm or a bruise on your leg.
-
Proximity to the Brain: The Trigeminal Nerve, which supplies the teeth, is the largest cranial nerve. It is hardwired directly into the brainstem. There is very little “filtering” of these signals. A toothache is like a fire alarm that goes off inside the command center.
-
The Primal Fear: Evolutionarily, the inability to eat due to mouth pain meant starvation. Deep in our lizard brain, we are hardwired to panic about anything that threatens our ability to chew.
-
The Helplessness: Unlike a sprained ankle you can elevate, you cannot “rest” a tooth. You have to talk, drink, and swallow saliva. The injured part is constantly in use and constantly being reintroduced to temperature changes.
-
The Anticipation Anxiety: Once you know the tooth hurts with cold, you start flinching before the glass touches your lips. This anxiety loop amplifies the perception of pain.
A Step-by-Step Guide: What to Do When You Feel That Feeling
If you are currently experiencing any of the sensations described above, here is a realistic, non-panicked action plan based on the stage of pain you are in.
If You Feel: Fleeting Cold Sensitivity (Stage 1)
-
Do Not Panic. This is not an emergency, but it is a deadline.
-
Visual Check: Use your phone flashlight and a mirror. Look for a dark spot or a hole in the grooves of the tooth.
-
Change Your Paste: Switch to a Stannous Fluoride toothpaste (like Sensodyne Repair & Protect or Crest Pro-Health). This helps plug the dentine tubules and can actually remineralize very early decay.
-
Book a Checkup: Schedule a dental visit within the next 2-4 weeks. Mention the sensitivity. They may just need a small filling.
If You Feel: Lingering Pain or Pain on Biting (Stage 2)
-
Avoid the Triggers. Chew on the other side. No ice water. No hard candy.
-
Pain Management: Over-the-counter Ibuprofen (Advil/Motrin) is the gold standard here. It reduces inflammation in the pulp. Acetaminophen (Tylenol) helps with pain perception but does little for the swelling inside the tooth. Never place aspirin directly on the gum—it causes a chemical burn.
-
Book an Appointment: This week. Do not wait until next month. The difference between a filling and a root canal is often just a few weeks of ignoring Stage 2 pain.
If You Feel: Throbbing at Night / Spontaneous Pain (Stage 3)
-
Sleep Elevated. Prop yourself up on several pillows. Do not lie flat.
-
Cold Water Sips: Use this only for brief relief to fall asleep. Do not rely on it for days.
-
Call the Dentist First Thing in the Morning. Be honest about the pain level. Say, “I have spontaneous pain that wakes me up at night.” Most offices will find a way to squeeze you in that day.
If You Feel: Swelling in Face or Gum Pimple (Stage 4 – Emergency)
-
Check for Red Flags:
-
Swelling under the eye.
-
Swelling under the jawline that feels hard.
-
Fever (temperature over 100.4°F / 38°C).
-
Difficulty swallowing or breathing.
-
-
If Yes to Red Flags: Go to the Emergency Room or Urgent Care. You need antibiotics immediately.
-
If No Red Flags (Just a small gum pimple): Call dentist immediately. Rinse with warm salt water (1 tsp salt in 8oz warm water) to encourage drainage of the pimple. Do not pop it with a needle.
The Long-Term Outlook: What Happens After the Pain?
Understanding the pain is half the battle. Knowing what comes next removes the fear of the unknown.
The Filling Appointment (Stage 1-2 Pain)
Procedure Sensation:
-
Numbing: You will feel a small pinch from the anesthetic needle. Modern techniques make this very tolerable.
-
The Work: You will feel vibration and water spray, but no sharp pain.
-
Aftermath: The tooth may feel slightly bruised or sensitive to cold for a few days. This is “Post-Op Sensitivity.” It fades quickly.
The Root Canal Appointment (Stage 3 Pain)
Procedure Sensation:
-
The Relief: Many patients find the root canal appointment is less painful than the toothache that brought them in. Why? Because you are finally numb, and the source of the pressure (the inflamed pulp) is being removed.
-
The Feeling: Pressure, pushing, and the sound of small files.
-
Aftermath: Soreness in the jaw muscle from holding your mouth open. The bone around the tooth might be tender for a few days. The deep, throbbing nerve pain is GONE.
The Extraction (Stage 4 Pain – No Saving Tooth)
Procedure Sensation:
-
Pressure: You will feel strong, firm pushing. This is the sensation of the ligament around the tooth being stretched. It is not pain if you are numb. Do not confuse “pressure” with “pain.”
-
Aftermath: The socket will heal over 1-2 weeks. You must follow “Dry Socket” prevention instructions carefully (No smoking, no straws, no spitting).
Prevention: Never Having to Ask the Question Again
The best answer to “what does tooth cavity pain feel like” is “I don’t know, and I plan to keep it that way.” Here is how.
The Modern Approach to Cavity Prevention
| Old Advice | Modern, Realistic Advice |
|---|---|
| “Brush twice a day.” | “Brush correctly twice a day. Angle the bristles 45 degrees into the gumline. Use a soft brush.” |
| “Floss daily.” | “Clean between your teeth daily. Use string floss, a Waterpik, or interdental brushes. Whatever you will actually do consistently.” |
| “Avoid sugar.” | “Manage frequency of sugar intake. It is better to eat a whole chocolate bar in 5 minutes than to sip a sugary soda for 2 hours. Acid attacks last 20-30 minutes after each sip. “ |
| “See a dentist.” | “See a dentist before you feel pain. Pain is the last symptom to appear.” |
The Role of Fluoride and Xylitol
-
Fluoride: This mineral incorporates into the enamel crystal structure, making it acid-resistant. Use a fluoride mouthwash at a separate time from brushing to maximize exposure.
-
Xylitol: This natural sweetener starves cavity-causing bacteria (Strep Mutans). Chewing xylitol gum after meals increases saliva flow and changes the mouth environment to be cavity-resistant.
Conclusion
What does tooth cavity pain feel like? It feels like a journey. It begins as a silent, invisible erosion, then whispers as a sharp zing to cold sweets. It escalates into a lingering, deep ache that can betray you in the quiet of night with a throbbing pulse. If ignored past this point, it either vanishes in a deceptive silence, only to return as a swollen, bone-deep pressure of infection. Recognizing the specific stage of this pain is the key to saving the tooth—and saving yourself from significant discomfort. Listening to these early signals from your enamel allows for simple fixes before the nerve is ever involved. Your mouth is always communicating; this guide ensures you understand the language of decay.
Frequently Asked Questions (FAQ)
Q1: Can a cavity stop hurting on its own?
Yes, but this is not good news. The pain stops when the nerve inside the tooth dies completely. The infection, however, does not stop. It continues to eat away at the jawbone silently, leading to an abscess later. Never assume a vanishing toothache means the problem is solved.
Q2: Why does my tooth only hurt when I eat sweets?
Sugar creates an osmotic gradient. It pulls fluid out of the microscopic tubes in your tooth (dentine tubules). This movement of fluid tugs on the nerve endings deep inside the tooth. If only one tooth hurts with sugar, it strongly suggests a cavity that has already broken through the hard enamel shell.
Q3: What is the difference between cavity pain and a cracked tooth?
Cavity pain is typically triggered by temperature (cold/hot) and sugar. Cracked tooth pain is triggered almost exclusively by biting pressure, and often hurts more when you release the bite than when you bite down.
Q4: Does a cavity always hurt when it’s small?
No. In fact, small cavities (limited to enamel) rarely hurt at all. This is the single biggest reason to visit the dentist for checkups even when your mouth feels fine. By the time you feel pain, the cavity is already moderate to large.
Q5: Why is my toothache so much worse at night?
This happens for two main reasons. First, lying down increases blood pressure to the head, which increases pressure inside an inflamed tooth. Second, there are fewer distractions, so your brain focuses entirely on the pain signal. Sleeping with your head elevated on extra pillows can help reduce the throb.
Q6: Can a cavity feel like an earache?
Absolutely. This is called referred pain. The nerves that supply the lower back teeth are very close to the nerves that supply the ear. A severe lower molar cavity can cause a deep, radiating pain that mimics an ear infection.
Additional Resource:
For more detailed information on the different types of dental pain and their causes, visit the American Dental Association (ADA) patient resource center:
MouthHealthy.org – Toothache Information