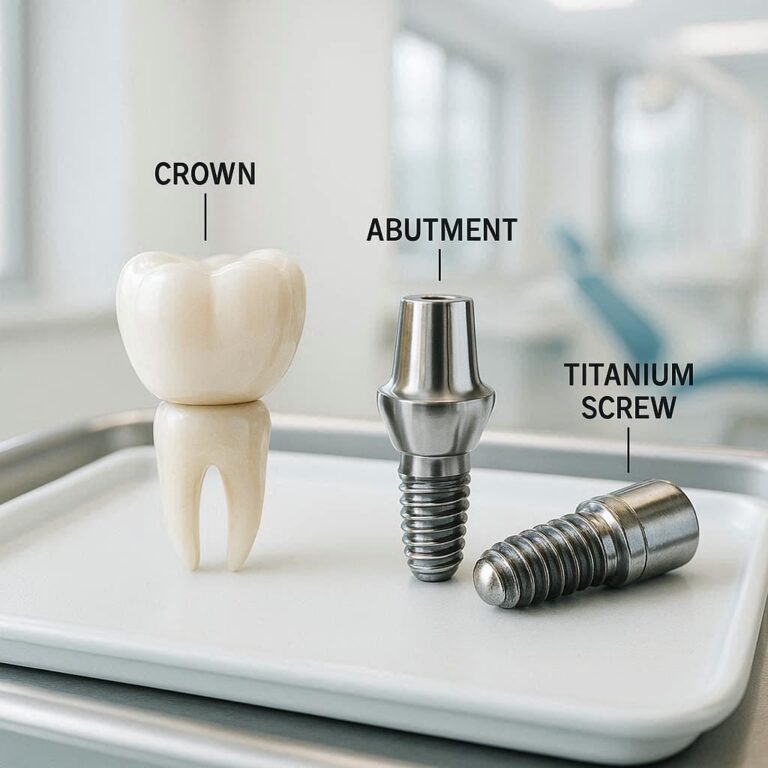
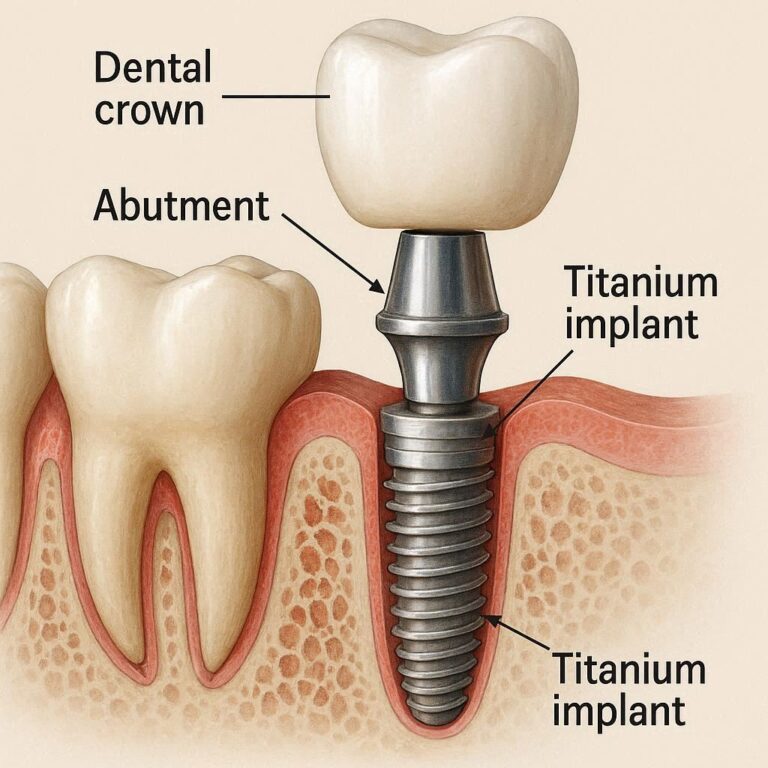
why no dairy after tooth extraction
The oral surgeon’s instructions felt clear until you got home, stared into the fridge, and saw the yogurt. Wait. Why no dairy after tooth extraction? You just had a molar yanked out, you are starving, and the only thing that sounds remotely soothing is a cold, creamy milkshake or a smooth bowl of cottage cheese. Yet, the discharge papers explicitly state: No dairy for 48 to 72 hours.
It seems counterintuitive. Dairy is soft. It requires no chewing. It is the poster child for “comfort food.” So why does every dentist and oral surgeon treat a glass of milk like it is contraband in the days following oral surgery?
This is not a myth passed down through dental folklore. There is a hard, physiological, and somewhat unpleasant reason behind this restriction. And while you might be craving that yogurt parfait, consuming it too soon could set your recovery back by days, increase your pain levels, and even land you back in the dreaded dental chair for an emergency visit.
In this comprehensive guide, we will dissect the science behind the “no dairy” rule. We will explore the specific interactions between milk proteins, oral bacteria, and the delicate blood clot that is currently acting as the sole guardian of your exposed jawbone. More importantly, we will provide you with a 14-day roadmap of delicious, dairy-free alternatives that will keep you full, happy, and healing on schedule.
Whether you had a simple extraction, a complex wisdom tooth removal, or a bone graft, understanding this one dietary rule is the linchpin of a pain-free recovery. Let’s get into the gritty, honest details of why that cheese stick needs to stay in the wrapper for just a little while longer.
The Sacred Blood Clot: Why Your Mouth Is a Construction Zone
Before we can understand why no dairy after tooth extraction, we have to understand what is actually happening inside that empty socket in your jaw. Most people think of the extraction site as just a “hole.” In reality, it is a highly active, incredibly fragile biological construction site.
The Formation of the Protective Barrier
When the dentist removes a tooth, they are not just pulling out enamel. They are severing the periodontal ligament and leaving behind exposed bone and nerve endings. Nature’s first response to this trauma is bleeding. This isn’t a bad thing; it is the delivery system for the body’s master builders.
Blood fills the socket and begins the coagulation cascade. Within minutes to hours, this blood transforms from a liquid into a semi-solid gelatinous mass known as the blood clot.
Important Note: Think of the blood clot as the scaffolding covering an open pit. Without that scaffolding, raw bone is exposed to air, food debris, and billions of bacteria. This exposure is the direct cause of “dry socket” (alveolar osteitis), a condition universally described by patients as more painful than the extraction itself.
What Dairy Does to the Clot (The Inflammation Connection)
Here is where the dairy issue enters the picture. Dairy products, particularly fermented ones like yogurt, kefir, and aged cheese, are rich in specific proteins and histamines. Additionally, milk contains casein, a protein that has been shown in some studies to interact with the inflammatory response in certain individuals.
While the link between milk and mucus production is a common anecdotal complaint, the real issue in an extraction socket is localized inflammation and bacterial load.
-
Inflammatory Response: Dairy can be slightly pro-inflammatory for a subset of the population. In the delicate first 48 hours, you want zero additional inflammation. Swelling is already fighting for space. Adding a food that might trigger a histamine or inflammatory reaction in the gum tissue can increase pressure on the clot.
-
pH Disruption: Milk is slightly acidic (pH 6.5 to 6.7). While not as corrosive as soda, introducing an acidic environment to a raw wound can delay the epithelialization (scabbing over) of the gum tissue.
-
Residue and Texture: Milk, when mixed with saliva, leaves a film. This biofilm can coat the back of the throat and, critically, the surgical site. This sticky film traps bacteria against the forming clot.
Why Dairy Increases the Risk of Dry Socket
The most compelling reason for the ban is the risk of infection leading to clot disintegration. The oral cavity is home to hundreds of bacterial species. Some are friendly; some are not. When you introduce lactose (milk sugar) into a wound that is trying to seal itself, you are essentially throwing a pizza party for Streptococcus mutans and other bad actors.
As bacteria feast on lactose, they produce acid and enzymes. These enzymes, particularly fibrinolytics, can literally dissolve the fibrin mesh that holds your blood clot together. If the clot dissolves before the gum tissue grows over the bone (which takes about 4-7 days), you are left with a dry socket.
Direct Quote from an Oral Surgeon: “When patients come in with dry socket and I ask what they ate, ‘milkshake’ or ‘yogurt smoothie’ is the answer about 30% of the time. It’s the combination of suction from the straw and the bacterial feeding frenzy from the lactose.” — Dr. A. Nguyen, DDS, Oral & Maxillofacial Surgery.
The Unique Danger of Fermented Dairy (Yogurt & Kefir)
Wait a minute, you might think. Yogurt has probiotics. Probiotics are good bacteria! Shouldn’t that help? In a healthy gut, yes. In an open surgical wound on your jawbone? Absolutely not.
Fermented dairy products contain live active cultures. Introducing a foreign strain of live bacteria—even a “good” one like Lactobacillus—into a sterile (or semi-sterile) wound bed is a recipe for an immune reaction. Your body’s white blood cells are already overwhelmed trying to clean up debris from the extraction. If they now have to fight a colony of yogurt cultures settling into the socket, the area becomes a battleground of inflammation, pus, and pain.
This is why the prohibition on yogurt and kefir is often stricter than for plain milk. Yogurt is a living product. Do not put living things in a fresh wound.
The Hidden Culprit: Nausea and Anesthesia Interactions
While the clot risk is the primary medical concern, there is a secondary, more immediate and visceral reason to avoid dairy: The vomit factor.
The Anesthesia and Antibiotic Cocktail
After a tooth extraction, your system is flooded with foreign chemicals. You likely received:
-
Local Anesthetic (Lidocaine/Articaine with Epinephrine): This constricts blood vessels and can make some people feel jittery or nauseous.
-
Nitrous Oxide (Laughing Gas): A known cause of dizziness and stomach upset.
-
IV Sedation or General Anesthesia: The after-effects of propofol or midazolam include significant nausea for 12 to 24 hours.
-
Post-Operative Antibiotics (Clindamycin or Amoxicillin): One of the most common side effects of oral antibiotics is gastrointestinal distress and nausea.
-
Opioid Painkillers (Codeine, Hydrocodone): These are notorious for causing severe stomach upset and vomiting.
Now, introduce dairy into this mix.
The Curdling Effect
Dairy is heavy. It requires specific enzymes (lactase and rennet) to break down. When your stomach is already queasy from anesthesia and pain meds, a heavy dairy product can sit like a rock. But worse than that is the potential for vomiting.
If you vomit within the first 72 hours of extraction, the pressure and acid content of the vomit will almost certainly dislodge the blood clot.
Critical Warning: Dry socket from vomiting is extremely common. The force of retching creates negative and positive pressure swings in the mouth. This physically suctions the clot out of the socket. If you feel nauseous, it is better to eat nothing or just ice chips than to force down a creamy, dairy-heavy “meal replacement” shake that might come back up.
Lactose Intolerance in a Stressed Body
You might not be lactose intolerant normally. But after surgery, your body is in a state of stress. Cortisol levels are high, and digestion slows down. Many people experience temporary secondary lactose intolerance during illness or recovery. The last thing you need is bloating, gas, and cramping that makes it impossible to lie still and rest.
Day-by-Day Recovery Timeline and Dairy Reintroduction
Let’s create a realistic roadmap. This isn’t about being paranoid; it’s about being strategic so you heal faster and can eat pizza again sooner.
| Day Post-Op | Condition of Socket | Dairy Status | Why? |
|---|---|---|---|
| Day 1-3 | Acute Inflammation Phase. Raw wound, active bleeding/clot stabilization. High swelling. | ABSOLUTELY NO DAIRY. | Highest risk of bacterial fermentation, inflammation, and nausea/vomiting interaction with drugs. |
| Day 4-5 | Proliferation Phase. Clot is stable. White/yellow granulation tissue may be visible (this is good—not pus!). | Strictly Limited. Soft cheese maybe? Still NO. | The clot is still vulnerable to fibrinolytic bacteria from yogurt/milk. The gum hasn’t sealed the bone. |
| Day 6-7 | Early Sealing. Gum tissue begins to creep over the socket edges. Swelling mostly gone. | Test with Caution. | A small amount of cold, plain milk (not yogurt or cheese) can be sipped (no straw!). Watch for any tingling or pain in the socket within 1 hour. |
| Day 8-10 | Tissue Closure. The hole is still there, but it is now covered by a thin layer of pink gum tissue. | Yogurt & Soft Cheese Allowed. | The barrier to the bone is now biological (gum tissue) not just a clot. Fermented dairy is safer now. |
| Day 14+ | Remodeling. The socket is filling in with bone from the bottom up. | Resume Normal Diet. | Continue to flush the socket with a syringe if provided, but dairy is no longer a risk factor. |
Dairy-Free Alternatives: What to Eat for the First Week
So, if you can’t have that soothing yogurt or cottage cheese, what on earth are you supposed to eat? You need calories to heal, but you also need food that is anti-inflammatory and soft. Here is a detailed, high-protein, dairy-free menu for the first critical 5 days.
The “Safe” Food List (Anti-Inflammatory & Soft)
| Food Category | Recommended Options | Preparation Tip |
|---|---|---|
| Proteins | Eggs (scrambled soft), Silken Tofu, Bone Broth, Salmon (poached/flaked cold), Hummus (smooth). | Ensure eggs are not too hot. Heat increases blood flow to the wound. Let food cool to room temp. |
| Fruits | Bananas (mashed), Applesauce, Avocado (mashed with lime), Mango puree. | Avoid berries with small seeds (strawberry/kiwi) for Day 1-4. Seeds can get lodged. |
| Vegetables | Mashed Potatoes (made with broth, not milk), Pumpkin Puree, Carrot puree. | Use chicken broth or olive oil to thin mashed potatoes instead of butter/milk. |
| Grains | Oatmeal (soupy, not thick), Cream of Wheat/Rice, Polenta. | Make it very thin. Thick, sticky oatmeal can adhere to the extraction site. |
| Liquids | Water, Coconut Water (no pulp), Aloe Vera Juice, Dairy-Free Protein Shakes (Pea Protein or Oat Milk base). | Room temperature or cold. NEVER USE A STRAW. |
A Sample 3-Day Dairy-Free Healing Menu
Day 1 (Ice and Liquids)
-
Breakfast: Cold coconut water.
-
Lunch: Smooth bone broth (room temp).
-
Dinner: Dairy-free pea protein shake mixed with water (sipped from a cup).
-
Snack: Applesauce pouch (squeezed gently into mouth, avoid suction).
Day 2 (Purees)
-
Breakfast: Cold banana mashed with a fork and a splash of oat milk.
-
Lunch: Avocado blended with salt and a squeeze of lime (Vitamin C for healing!).
-
Dinner: Silken tofu blended with soy sauce and a tiny bit of ginger (anti-inflammatory).
Day 3 (Soft Solids)
-
Breakfast: Scrambled eggs (cold or lukewarm).
-
Lunch: Hummus (very smooth, check for no whole chickpeas).
-
Dinner: Poached salmon, flaked very small and mixed with mashed avocado.
A Quick Comparison: Dairy vs. Dairy-Free Post-Op
| Feature | Dairy Option (e.g., Yogurt) | Dairy-Free Alternative (e.g., Mashed Avocado) |
|---|---|---|
| Risk to Clot | High (Lactose feeds bacteria; Casein inflames). | Low (Avocado fat is anti-inflammatory). |
| Nausea Risk | High (Heavy, curdles with meds). | Low (Light, easy to digest). |
| Nutritional Value | Good protein/calcium but comes with risk. | Healthy fats, Potassium, Vitamins C & E. |
| Temperature | Usually cold (good). | Can be room temp (good). |
| Cleanliness | Sticky residue requires active rinsing. | Easily rinsed away with saline. |
The Science of Healing: Why Anti-Inflammatory Foods Matter
Since we are removing dairy to lower inflammation, let’s double down on foods that actively reduce swelling and pain. The first 72 hours after an extraction are a battle against edema (swelling) and prostaglandins (pain chemicals).
Foods That Fight Swelling (Better Than Ice Cream)
-
Pineapple (Juice or Puree): Pineapple contains Bromelain, a powerful enzyme that has been clinically proven to reduce post-surgical swelling and bruising. It is a natural anti-inflammatory. Note: Strain the juice to remove any fibrous bits.
-
Turmeric (in Broth): Curcumin is a potent anti-inflammatory compound. Mixing a tiny pinch of turmeric into warm (not hot) bone broth can speed up tissue repair.
-
Omega-3s (Flaxseed Oil): If you can’t have salmon, add a teaspoon of flaxseed oil to your smoothie or mashed potatoes. Omega-3s reduce the production of inflammatory cytokines.
Important Note on “Healing Shakes”: The market is flooded with “healing smoothies.” Be very careful. A smoothie made with berries, spinach, and chia seeds is a nightmare for an extraction site. The seeds and tiny leaf fragments will wedge themselves into the open socket and cause a severe foreign body reaction. Stick to filtered, seedless liquids for the first 4 days.

Why No Dairy After Tooth Extraction: The Specific Case of Bone Grafts
This is a critical distinction that many general articles miss. If you had a bone graft placed in the socket (common with molar extractions or preparation for a future implant), the “no dairy” rule extends significantly longer and becomes much more crucial.
The Graft Material Interaction
A bone graft is usually a mixture of cadaver bone particles or bovine (cow) bone mineral mixed with your own blood. It looks like wet sand packed into the hole. The body needs about 4 to 6 months to turn this “sand” into your own living jawbone.
Introducing dairy proteins (especially bovine casein) near a bovine bone graft creates an immunological gray area. While the graft material is sterile and processed to remove all proteins, your body is hypersensitive in that area.
-
Cross-Reactivity: Your immune system is on high alert. If you flood the area with milk proteins from a cow, the localized immune cells might confuse the bovine graft particles for an invader and attack the graft. This leads to graft failure (the graft turns to mush and washes out).
-
Infection = Lost Graft: A bone graft is an avascular (low blood flow) scaffold. It cannot fight infection like living tissue can. If a bacterial colony from yogurt sets up shop in the graft, the only solution is to open the gum back up, scrape out the infected graft, and start over.
Rule of Thumb for Bone Grafts: *Avoid all dairy for a minimum of 7 days post-graft. Some oral surgeons recommend 14 days strictly dairy-free to ensure the gum tissue seals over the expensive graft material completely.*
How to Safely Reintroduce Dairy (The 7-Day Test)
You’ve made it 5 days. The hole is looking less like a crater and more like a dimple. You are desperate for cheese. Here is the safe, methodical way to bring dairy back without triggering a late-onset dry socket.
The Step-by-Step Reintroduction Protocol
-
Day 6 (The Sip Test): Pour 2 ounces of cold milk into a cup. Sip it slowly. Do not swish. Let it slide down the opposite side of your mouth. Wait 4 hours. Do you feel any new throbbing? Any sour taste in the extraction area? If yes, wait 2 more days. If no, proceed.
-
Day 7 (The Soft Cheese Test): Eat a small piece of mozzarella (fresh, soft, not stringy). Chew on the opposite side. The key here is to avoid the “sucking” motion used to pull melted cheese off a pizza. Just let it dissolve and swallow.
-
Day 8 (The Yogurt Test): This is the final boss. Eat 1/4 cup of plain, pasteurized yogurt (Greek or regular). Fermented dairy is the biggest risk for bacterial overload. After eating, perform a gentle salt water rinse (do not swish vigorously—just tilt head side to side). If the socket feels fine the next morning, you are in the clear.
Signs You Reintroduced Dairy Too Soon
-
Sour or “Cheesy” Smell from the Socket: This is not normal healing breath. This is lactose fermenting in the wound. Rinse with salt water immediately and stop dairy for 3 more days.
-
Delayed Swelling: If your cheek puffs up again on Day 7 after being flat on Day 5, look at what you ate 12 hours prior.
-
Dull Ache Returning: Pain should decrease daily. A sudden return of a deep, boring ache indicates clot irritation or infection.
Debunking Myths: “But My Friend Ate Ice Cream and Was Fine!”
You will always find the anecdotal outlier. The friend who ate a double cheeseburger 2 hours post-op and “never had a problem.” Or the uncle who swears by drinking buttermilk for gum health.
The Survivorship Bias in Oral Surgery
This is called survivorship bias. The people who got dry socket are at home in agony, not bragging about their fast food choices. Dry socket occurs in about 2-5% of all routine extractions. However, that number spikes to 20-30% for lower wisdom teeth.
By avoiding dairy, you are simply stacking the odds in your favor. You are removing one variable from a complex healing equation. Is it guaranteed that yogurt will cause dry socket? No. But is it a risk factor that is incredibly easy to eliminate? Yes.
Myth: “But the Cold Dairy Helps Swelling!”
Correction: Cold helps swelling. Dairy does not.
You can achieve the same, if not better, anti-inflammatory effect with:
-
Frozen Peas (conforms to face shape better than a gel pack).
-
Ice Water (sipped, not strawed).
-
Dairy-Free Sorbet (Check ingredients! Many sorbets have milk solids. Look for Coconut Milk Ice Cream or Fruit Sorbet made with water).

The Role of Oral Hygiene While Avoiding Dairy
During the dairy-free phase, you might be tempted to skip brushing because your mouth hurts. That is a critical error. The absence of dairy doesn’t mean bacteria aren’t thriving on other food sources.
How to Clean Without Dislodging the Clot
Days 1-3: The Passive Rinse
Do not spit. Do not swish.
-
Fill a cup with warm salt water (1/2 tsp salt per 8oz water).
-
Put the cup to your lips.
-
Tilt your head side-to-side gently.
-
Open your mouth over the sink and let the water fall out. Do not purse your lips and spit.
Days 4-7: The Soft Brush
-
Brush your teeth normally, but avoid the extraction site.
-
Use a baby toothbrush with extra soft bristles for the teeth adjacent to the socket.
-
Continue salt water rinses.
Days 7+: The Syringe (If Provided)
-
Some surgeons give you a curved plastic syringe. Use this only after Day 5-7 (or when instructed).
-
Fill with warm salt water.
-
Place the tip near the socket opening, not in it.
-
Gently flush to remove food debris. This is the most satisfying (and sometimes gross) part of healing.
Long-Term Nutrition: Rebuilding Bone After Extraction
Once you have passed the 2-week mark and dairy is back on the menu, your focus should shift from “avoiding pain” to “building bone.” The jawbone needs specific nutrients to fill in that socket completely.
Key Nutrients for Socket Regeneration
| Nutrient | Why It Matters | Dairy Sources | Dairy-Free Sources |
|---|---|---|---|
| Calcium | Primary building block of new bone matrix. | Milk, Cheese, Yogurt. | Fortified Oat Milk, Collard Greens, Almonds (ground/butter). |
| Vitamin D | Required to absorb calcium. Without D, you just pee out the calcium. | Fortified Milk. | Sunlight, Salmon, Egg Yolks. |
| Vitamin K2 | Directs calcium into the bone and away from soft tissue/arteries. | Gouda, Brie, Butter. | Natto (fermented soybeans), Chicken Liver. |
| Magnesium | Activates Vitamin D. | Yogurt. | Pumpkin Seeds (butter), Spinach (cooked soft). |
Insight: *Interestingly, hard aged cheeses (like Gouda and Cheddar) are some of the best sources of Vitamin K2 MK-7, which is essential for jawbone density. This is why dairy is beneficial after the soft tissue has healed. The key is timing.*
Psychological Impact: Dealing with Food Cravings During Recovery
Let’s be honest. A lot of the frustration around why no dairy after tooth extraction is emotional, not nutritional. You are in pain, you are bored, you are stuck on the couch, and all you want is comfort food. And for most of us, comfort food is cheese, ice cream, or creamy pasta.
The Cortisol-Craving Connection
Pain increases cortisol. Cortisol increases cravings for high-fat, high-sugar foods (like ice cream) because the brain is seeking a dopamine hit to counter the stress. Recognizing this is half the battle.
How to Hack Your Brain with Dairy-Free Comfort Food
-
Craving Ice Cream? Freeze a very ripe banana. Blend it with a splash of oat milk and a spoonful of cocoa powder. This makes “Nice Cream.” It is cold, creamy, sweet, and zero dairy. It’s also loaded with potassium which helps reduce muscle soreness from clenching your jaw.
-
Craving Mac and Cheese? Make a “Cheeze” sauce from boiled potatoes and carrots blended with nutritional yeast and a bit of mustard. Pour over overcooked, soft pasta. It hits the umami, salty, creamy notes without a drop of milk.
-
Craving a Milkshake? Blend Oat Milk, a banana, and a tablespoon of sunflower seed butter (no gritty seeds!). Sunflower butter is an excellent source of Vitamin E, which reduces scar tissue formation.
Why No Dairy After Tooth Extraction: The Medication Deep Dive
Earlier we mentioned nausea, but the interaction goes deeper than just an upset stomach. The medications prescribed post-extraction have specific relationships with dairy calcium that can sabotage your recovery in less obvious ways.
1. Antibiotics (Tetracyclines & Fluoroquinolones)
If your dentist prescribed Doxycycline or Ciprofloxacin (common for severe infections or penicillin allergies), consuming dairy within 2-3 hours of the pill is a known disaster.
The Mechanism: Calcium (from milk) binds to the antibiotic molecule in the gut. This forms an insoluble complex—essentially a rock that your body cannot absorb. You end up passing the antibiotic in your stool without ever getting it into your bloodstream. This means the bacteria in your socket are having a field day while you think you are protected.
Rule: Wait at least 3 hours after dairy before taking these antibiotics, or 2 hours before.
2. Painkillers (NSAIDs and Opioids)
-
Ibuprofen (Advil/Motrin): Milk can coat the stomach lining, which is actually good for preventing ibuprofen-induced ulcers. However, full-fat milk slows gastric emptying. This means your pain relief takes longer to kick in. When your jaw is throbbing, you want relief in 20 minutes, not 60 minutes. Stick to a few crackers or a banana with ibuprofen instead of a glass of milk.
-
Opioids (Hydrocodone/Tylenol #3): As mentioned, these cause gastroparesis (stomach paralysis). Dairy proteins require strong stomach acid to break down. If your stomach is semi-paralyzed from codeine, the milk just sits there, fermenting and causing sulfur burps. This can trigger vomiting, which is catastrophic for the clot.
3. Chlorhexidine Rinse (Prescription Mouthwash)
This is the gold standard rinse for preventing infection after extraction. Do not use dairy for 30 minutes after rinsing. Chlorhexidine is a cation (positively charged). Certain compounds in dairy (anions) can neutralize it, rendering the mouthwash ineffective. You want that blue stuff clinging to the gum tissue, not reacting with milk residue.
The Visual Guide: What a Healing Socket Looks Like
Knowing what is normal can prevent you from panicking and reaching for a “soothing” yogurt thinking you already have an infection. Here is what you should see during the dairy-free phase.
| Timeline | Visual Appearance | “Is this normal?” |
|---|---|---|
| Day 1-2 | Dark red/black hole. Blood clot visible. Slight white film on top of clot. | YES. The white film is fibrin, a protein mesh. Do not scrape it off. This is not dairy residue. |
| Day 3-4 | Clot appears smaller. Gum tissue edges are white/grey and puffy. | YES. This is sloughing of dead skin cells (epithelium). It looks gross but is healing. |
| Day 5-7 | Clot is gone (replaced by granulation tissue). Hole is a creamy yellow/white color. Bad breath? Yes. | YES. Granulation tissue looks exactly like wet macaroni and cheese. This is where people freak out and think it’s pus. Pus has a foul odor and is accompanied by swelling and fever. Granulation tissue is firm and odorless (or smells like iron/blood). |
| Day 10 | Hole is much smaller. Pink gum closing over the top. | YES. You are winning. |
If you see green or yellow liquid oozing from the socket, or a red, inflamed ring around the hole with a white center, then you have an infection. But the standard white/yellow “mac and cheese” look is a good sign of healing collagen.
Frequently Asked Questions (FAQ)
Q: Can I drink almond milk or oat milk after tooth extraction?
A: Yes, absolutely. Plant-based milks do not contain lactose or casein. They are the ideal alternative during the first 3-5 days. Ensure they are unsweetened to limit sugar for bacteria, and drink from a cup, not a straw.
Q: What happens if I accidentally ate some yogurt on Day 2?
A: Do not panic. One spoonful is unlikely to cause immediate dry socket unless you were already prone to it. Stop eating it immediately. Rinse gently with salt water (head tilt only). Monitor for increased pain over the next 12 hours. Most likely, you will be fine, but do not eat any more.
Q: Why no dairy after tooth extraction specifically for wisdom teeth?
A: Wisdom tooth sockets are deeper and located at the very back of the mouth. This area has less blood flow than the front of the jaw. Consequently, healing is slower, and the risk of food impaction (and subsequent bacterial fermentation of dairy) is much higher. The “no dairy” rule is most strictly enforced for lower wisdom teeth.
Q: Can I have butter?
A: Technically, butter is 80% fat and only trace amounts of milk protein (casein) and lactose. However, it is greasy. Greasy food is hard to clean out of a socket. It is best to avoid butter on toast for the first 3 days simply because the crumbs and grease combination creates a difficult-to-flush paste.
Q: Is Greek yogurt worse than regular yogurt?
A: Yes, in the context of a fresh wound. Greek yogurt is strained to remove liquid whey. This concentrates the protein and live bacterial cultures. It is a denser source of the very things that irritate the clot. Stick to no yogurt at all for the first week.
Q: When can I have a milkshake?
A: Two factors here: Dairy and Straw. You need to wait until the clot is secure (Day 5-7) AND you must use a spoon, not a straw. The suction from a straw is the #1 cause of dry socket, even above dairy. If you must have a milkshake on Day 6, eat it with a spoon very carefully.
Conclusion
The restriction on dairy after a tooth extraction serves two critical purposes: safeguarding the fragile blood clot from bacterial fermentation and inflammation, and preventing nausea that could physically dislodge the clot. By understanding the science behind casein and lactose in an open wound, patients can make informed choices that drastically reduce their risk of dry socket. Committing to a dairy-free diet for the first 5 to 7 days is not an arbitrary rule; it is the most effective, evidence-based strategy to ensure a smooth, pain-free, and expedited recovery.
Additional Resource
For a visual guide on proper post-operative care and how to mix salt water rinses, please visit the official patient education portal of the American Association of Oral and Maxillofacial Surgeons (AAOMS).
Link: https://myoms.org/procedures/dental-extractions/