4 On 8 Dental Implants: A Complete, Honest Guide to Full-Arch Restoration
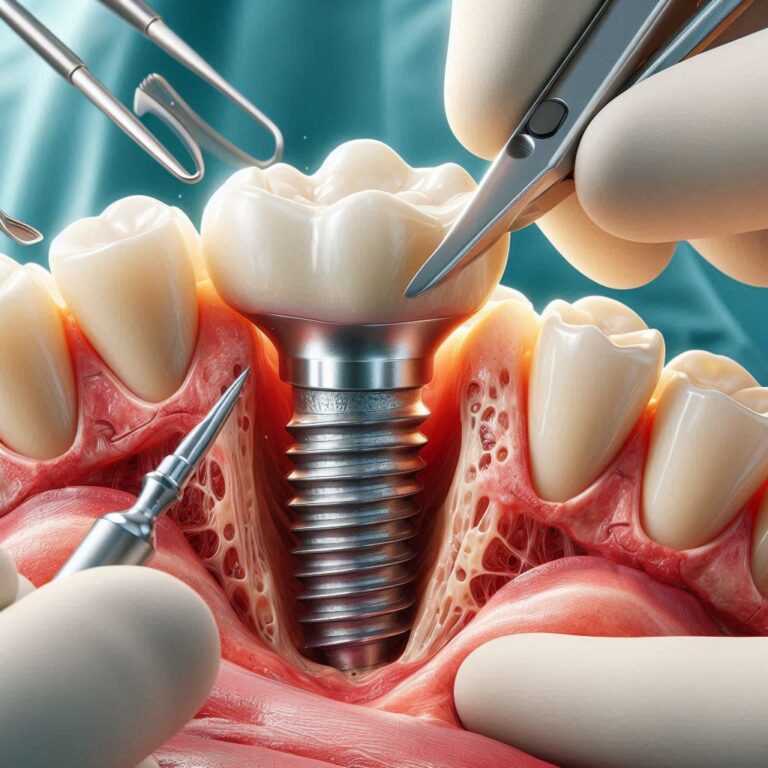
Losing most or all of your teeth changes your life. You might hide your smile, avoid certain foods, or feel embarrassed in conversations. Traditional dentures can help, but they come with their own problems: slipping, clicking sounds, sore spots, and limited chewing power.
That is why many people look for a more permanent solution. You have probably heard of “all-on-4” implants. But there is another powerful option: 4 on 8 dental implants.
This guide gives you a realistic, complete, and reader-friendly overview. We will explain what this technique is, how it differs from other methods, who it works best for, what the surgery feels like, and what you should expect for recovery and costs.
No fluff. No false promises. Just honest, useful information to help you make a smart decision.
What Are 4 on 8 Dental Implants? A Clear Definition
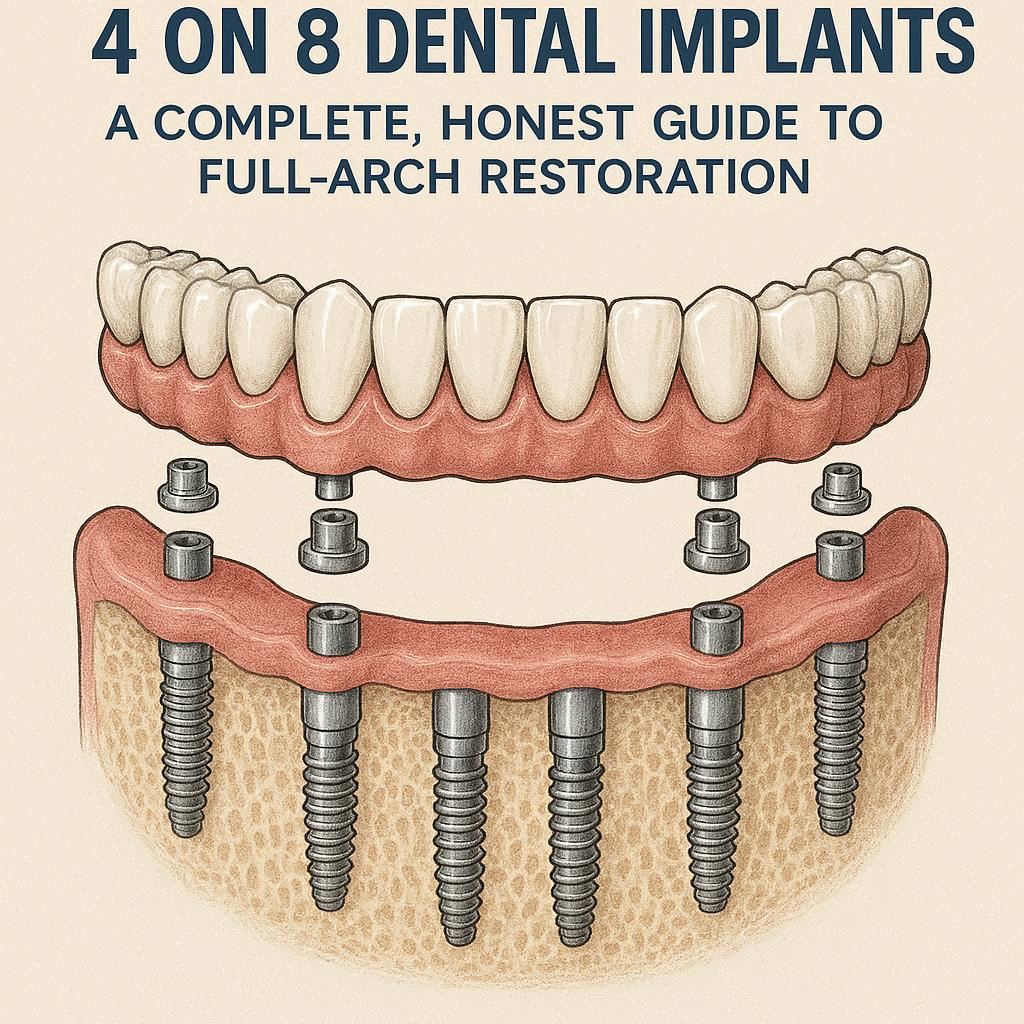
Let us start with the basics. The name “4 on 8” describes the structure of the implant system.
- The first number (4) refers to the number of dental implants placed in each jaw.
- The second number (8) refers to the number of teeth (or pontics) attached to those implants in a single arch.
In simple terms: your dentist places four titanium implant posts into your upper or lower jawbone. Then, they attach a fixed bridge that holds eight prosthetic teeth. This bridge replaces an entire arch of missing teeth.
Important note: Some people confuse “4 on 8” with “all-on-4.” They are related but not identical. All-on-4 uses four implants to support ten to fourteen teeth. The 4 on 8 technique uses four implants to support exactly eight teeth per arch.
The result is a non-removable, fixed restoration. You do not take it out at night. You clean it like natural teeth (with some adjustments). You chew with confidence.
Why Eight Teeth and Not More?
Dentists design the 4 on 8 prosthesis to replace the front eight teeth: from the left first premolar to the right first premolar. Why stop there?
- Bite balance: Eight teeth provide excellent chewing function without overloading the four implants.
- Anatomy: The area behind the premolars (molar region) has less bone volume in many patients. Avoiding that zone reduces the need for bone grafting.
- Simpler hygiene: Fewer teeth mean easier cleaning, especially for people with limited dexterity.
This approach prioritizes long-term stability over having a full set of 12 or 14 teeth. Many patients report they do not miss the back molars because the eight teeth handle most chewing tasks perfectly.
How 4 on 8 Differs from Other Implant Techniques
Choosing the right implant system can feel overwhelming. Let me make it easier with a straightforward comparison.
Comparison Table: 4 on 8 vs. All-on-4 vs. Traditional Implants
| Feature | 4 on 8 | All-on-4 | Traditional Single Implants |
|---|---|---|---|
| Implants per arch | 4 | 4 | 6 to 8+ |
| Teeth per arch | 8 | 10–14 | 1 per missing tooth |
| Removable? | No (fixed) | No (fixed) | No (fixed) |
| Bone grafting often needed? | Rarely | Sometimes | Often |
| Surgery sessions | 1 (main) | 1 (main) | Multiple |
| Average healing time | 4–6 months | 4–6 months | 3–8 months |
| Cost range (per arch) | 12,000–20,000 | 15,000–28,000 | 3,000–6,000 per implant |
| Best for | Moderate bone loss; full arch | Full arch; adequate bone | Single or few missing teeth |
Key Differences Explained
Number of teeth:
With all-on-4, you typically get a 12-tooth bridge (first molar to first molar). With 4 on 8, the bridge stops at the first premolar. This shorter bridge puts less stress on the implants.
Implant angulation:
All-on-4 uses tilted posterior implants to avoid sinus cavities and nerve canals. The 4 on 8 technique often uses straight (axial) implants because the bone in the premolar region is usually denser.
Surgical complexity:
4 on 8 is generally less complex. The dentist places implants in a straight line without needing advanced angulation. This simplicity reduces the risk of nerve or sinus complications.
Future flexibility:
If you lose one of the four implants in a 4 on 8 system, the entire bridge may need replacement. In all-on-4, the design sometimes allows for one implant to fail without losing the whole restoration. This is a real but uncommon risk.
Reader note: No single technique is “better” overall. The right choice depends on your bone quality, budget, health history, and personal preferences.
Who Is a Good Candidate for 4 on 8 Implants?
Not everyone qualifies. A good implant dentist will tell you “no” if the risks outweigh the benefits. Here is who typically makes a great candidate.
Ideal Candidate Profile
- You are missing all or most teeth in one jaw.
This technique works best for complete arch replacement, not for filling a few gaps. - You have moderate bone loss but not severe atrophy.
You need enough bone height and width to place four implants, each at least 10mm long and 3.5mm wide. The premolar area usually preserves bone better than the back molar region. - You do not clench or grind your teeth heavily.
Bruxism (teeth grinding) creates excessive forces that can break implant components or loosen the bridge over time. - You are a non-smoker or willing to quit.
Smoking dramatically increases implant failure rates. Most reputable dentists require a tobacco-free period of at least two weeks before surgery and throughout healing. - You have good general health.
Uncontrolled diabetes, active cancer treatments, severe osteoporosis, or autoimmune diseases can interfere with osseointegration (bone fusing to the implant). - You can maintain daily hygiene.
You must clean under the bridge and around each implant. This takes 2–3 minutes twice per day. If you have severe arthritis or other mobility issues, a removable denture might be safer.
When 4 on 8 Is NOT Recommended
- You only have 2–3 missing teeth in a row.
- Your bone loss is so severe that even standard implants are impossible without major grafting.
- You have active gum disease (periodontitis) that is untreated.
- You are pregnant (elective surgery is not advised).
- You take intravenous bisphosphonates (osteoporosis drugs) – this raises the risk of jawbone necrosis.
A Word About Age
Age alone is not a barrier. Many people in their 70s and 80s receive 4 on 8 implants successfully. What matters is healing capacity. A healthy 75-year-old with controlled blood pressure can heal as well as a 50-year-old smoker.
Step-by-Step: What Happens During the 4 on 8 Procedure
Let me walk you through the entire journey, from your first consultation to the day you eat an apple again. Understanding each step reduces fear and surprises.
Step 1: Initial Consultation and Imaging
Your dentist will:
- Review your medical and dental history.
- Examine your mouth, gums, and remaining teeth.
- Take a CBCT scan (3D X-ray). This shows bone quantity, quality, and the location of nerves and sinuses.
- Discuss your goals and budget.
At this visit, ask these questions:
- “How many 4 on 8 cases have you done in the last two years?”
- “Do you have before-and-after photos I can see?”
- “What happens if an implant fails?”
- “Is the final bridge metal-acrylic, zirconia, or hybrid?”
Step 2: Treatment Planning
Using special software, the dentist virtually places your implants. They determine:
- Exact implant positions.
- Implant length and diameter.
- Need for any extractions (if you still have failing teeth).
- Type of temporary prosthesis you will wear during healing.
You will receive an estimate and a timeline. Most clinics complete the entire process in 4–6 months from surgery to final teeth.
Step 3: Surgery Day (Tooth Extractions + Implant Placement)
This is the most intense but well-managed part. Here is what to expect.
Before surgery:
- You will take antibiotics (usually amoxicillin or clindamycin) one hour before.
- Sedation options: local anesthesia + laughing gas, oral sedatives, or IV sedation. Most patients choose IV sedation because they remember nothing.
During surgery (60–90 minutes per arch):
- The dentist numbs the area completely.
- If you have remaining teeth, they are extracted.
- The gum tissue is opened to expose the bone.
- Four small holes are drilled precisely where planned.
- Titanium implants are screwed into these holes.
- A healing cap or temporary bridge is attached.
You will feel pressure but no sharp pain. After surgery, you rest in a recovery area for 30–60 minutes.
Step 4: Healing and Osseointegration
Osseointegration is the magical process where your bone cells grow tightly around the titanium surface. This takes 4 to 6 months for the lower jaw and 5 to 7 months for the upper jaw (upper bone is softer and less dense).
During this period:
- You wear a temporary bridge or denture. It looks fine but is not for heavy chewing.
- You eat soft foods (mashed potatoes, smoothies, scrambled eggs, yogurt).
- You avoid crunchy, sticky, or hard foods.
- You visit the dentist every 4–6 weeks for checks.
Warning signs to report immediately:
Increasing pain, swelling after the first week, a loose implant, or bad taste from the surgery site.
Step 5: Uncovering and Final Impressions
Once the implants are fully integrated (your dentist confirms with an X-ray), you return for the next phase.
- The healing caps are removed.
- Impressions (digital or physical) are taken of your implants and gums.
- The dental lab fabricates your final 4 on 8 bridge. This takes 2–4 weeks.
- You choose the shape, size, and color of your new teeth.
Step 6: Fitting the Final Bridge
Your final appointment:
- The temporary restoration is removed.
- The permanent bridge is tried in. You check fit, bite, and appearance.
- The dentist screws the bridge onto the four implants (or cements it, though screw-retained is preferred).
- You receive cleaning instructions.
- You walk out with a complete, fixed smile.
Types of Materials Used for 4 on 8 Bridges
The implants themselves are almost always medical-grade titanium (or zirconia in some premium systems). But the bridge (the visible teeth) comes in different materials.
Comparison Table: Bridge Material Options
| Material | Durability | Aesthetics | Cost | Stain Resistance | Best for |
|---|---|---|---|---|---|
| Acrylic (temporary) | Low | Good | Low | Poor | Temporary use only |
| Acrylic with metal frame | Medium | Fair | Medium | Medium | Budget final bridges |
| Zirconia (monolithic) | Very high | Excellent | High | Excellent | Upper arch; high esthetics |
| PEEK (polymer) | Medium | Good | Medium | Good | Metal-free allergies |
| Hybrid (composite + fiber) | Medium | Very good | Medium | Medium | Lower arch; moderate forces |
Most Common Choice: Metal-Acrylic
Most 4 on 8 restorations use a titanium or gold alloy bar framework with pink acrylic gum-colored base and white acrylic teeth. This combination offers:
- Strength from the metal substructure.
- Repairability – if an acrylic tooth chips, the lab can repair it.
- Lower cost compared to full zirconia.
Downsides: Acrylic wears down over 5–10 years and can stain. You may need replacement of the acrylic portion after a decade.
Premium Option: Monolithic Zirconia
Zirconia bridges are milled from a single block of ceramic. They are:
- Extremely strong (can withstand 800–1,200 Newtons of force).
- Stain-proof and scratch-resistant.
- More biocompatible (rarely causes allergic reactions).
Downsides: Zirconia is expensive. It cannot be repaired easily – a fracture means replacing the whole bridge. It also transfers more force to the implants, which is only safe if your bone quality is excellent.
Reader note: Do not choose materials based on price alone. A cheap acrylic bridge that fractures every two years will cost more in the long run than a quality zirconia bridge that lasts 15+ years.
Recovery Timeline: What to Expect Week by Week
Recovery varies by person, but here is a realistic timeline.
Days 1–3 (The hardest part)
- Swelling peaks around day 2.
- Mild to moderate pain (controlled with ibuprofen + acetaminophen).
- Ice packs on the cheeks (20 minutes on, 20 off).
- Liquid diet only.
- No spitting, no straws, no rinsing vigorously.
Days 4–7 (Noticeable improvement)
- Swelling goes down.
- Pain becomes dull and manageable.
- You switch to soft foods: pudding, applesauce, mashed potatoes, protein shakes.
- Start gentle saltwater rinses (don’t swish, just move your head side to side).
Weeks 2–4 (Return to routine)
- Most people return to work after 3–7 days depending on their job.
- You can eat softer solid foods: pasta, scrambled eggs, well-cooked fish.
- Sutures dissolve or are removed.
- You begin gentle brushing of the temporary bridge with a soft toothbrush.
Months 2–4 (Quiet healing)
- You barely notice the implants.
- You can eat most foods except very hard or sticky items (nuts, caramels, beef jerky).
- Bone continues fusing to the implants.
Month 5–6 (Ready for final bridge)
- Digital impressions taken.
- Final bridge fabricated.
- Once placed, you can gradually reintroduce harder foods.
Month 6 and beyond (Full function)
- You eat apples, corn on the cob, steak – but with common sense. Biting into a whole apple is fine; chewing ice is not.
- You clean daily.
- Annual checkups with X-rays to monitor implant health.
Important warning: Some online testimonials claim you can eat “anything immediately.” That is unrealistic and dangerous. Rushing your healing can cause implant failure. Follow your dentist’s timeline strictly.
Costs of 4 on 8 Dental Implants (Realistic Estimates)
Let me be transparent: dental implants are a significant financial investment. But compared to the lifetime cost of denture adhesives, repairs, and replacements, many patients find implants cost-effective.
Breakdown of Costs per Arch
| Component | Low Estimate | High Estimate |
|---|---|---|
| Consultation and CBCT scan | $300 | $800 |
| Four titanium implants (surgical placement) | $4,000 | $8,000 |
| Temporary bridge (during healing) | $1,000 | $2,500 |
| Final bridge (metal-acrylic) | $4,000 | $6,000 |
| Final bridge (zirconia) | $6,000 | $10,000 |
| Anesthesia/sedation (IV sedation) | $500 | $1,200 |
| Total per arch (metal-acrylic) | $9,800 | $18,500 |
| Total per arch (zirconia) | $11,800 | $22,500 |
Two Jaws (Upper + Lower)
If you need both arches restored, expect to pay:
- Metal-acrylic both arches: 18,000–35,000
- Zirconia both arches: 22,000–45,000
Why the Wide Range?
Cost differences come from:
- Geographic location (downtown Los Angeles vs. rural Ohio).
- Dentist’s experience (a prosthodontist charges more than a general dentist).
- Lab quality (local US lab vs. overseas lab).
- Included warranties (some clinics include free replacement for 5–10 years).
Does Insurance Cover 4 on 8 Implants?
- Medical insurance: Rarely covers elective implants.
- Dental insurance: Some plans cover part of the extraction and temporary bridge costs. Few cover implants fully. Maximum annual benefits (1,000–2,000) cover only a fraction.
- Discount dental plans: These can save you 15–30% at participating providers.
Financing Options
Most clinics offer:
- CareCredit (medical credit card with 6–12 months no interest).
- In-house payment plans (0% interest over 12–24 months).
- Home equity loans (low interest, tax-deductible in some cases).
Reader note: Be skeptical of “$8,000 all-on-4 per arch” ads. Many exclude the final bridge, or they use low-quality materials and non-specialist dentists. Always ask for a complete itemized estimate before signing anything.
Pros and Cons of 4 on 8 Implants
Let me summarize the advantages and disadvantages honestly.
Advantages (Pros)
1. Fixed, non-removable teeth.
No adhesives. No soaking overnight. No clicking or slipping when you talk or laugh.
2. Preserves bone.
The implants stimulate your jawbone, preventing the “sinking face” look that happens with traditional dentures.
3. Better chewing power.
You regain about 70–85% of natural chewing force. Traditional dentures give you only 20–30%.
4. Shorter surgery than full-mouth individual implants.
Four implants per arch instead of eight or ten means less time in the chair and lower cost.
5. Easier cleaning than individual implant crowns.
You only have to clean around four supports, not twelve separate crowns.
6. No palatal coverage (for upper arch).
Traditional upper dentures cover the roof of your mouth, interfering with taste and sensation. 4 on 8 implants leave your palate uncovered.
Disadvantages (Cons)
1. High upfront cost.
Even the least expensive option costs more than a luxury vacation.
2. Not reversible.
Once you extract teeth and place implants, you cannot go back to natural teeth. This is a permanent change.
3. Requires surgery.
Any surgery carries risks: infection, bleeding, nerve injury (rare), or implant failure.
4. Maintenance is not zero.
You must buy special cleaning tools (water flosser, implant-specific brushes). You need professional cleanings every 6–12 months.
5. Potential for fractures.
The acrylic bridge can crack or chip, especially if you grind your teeth or eat very hard foods.
6. Harder to repair than a denture.
If a denture breaks, you can get a temporary repair in 24 hours. If a 4 on 8 bridge breaks, you may wait weeks for a lab-fabricated replacement.
A Real Patient’s Perspective
“I had my 4 on 8 lower arch done two years ago. The first week was rough – lots of swelling and soft foods. But now? I eat steak. I eat nuts. I forgot how to use denture glue. The only downside is the cost. I paid $16,000 for one arch. That hurt my savings. But looking back, I would do it again.”
— Margaret, 68, Florida
Daily Care and Maintenance of 4 on 8 Implants
You cannot treat 4 on 8 implants exactly like natural teeth. But the routine is manageable.
Cleaning Tools You Will Need
- Water flosser (Waterpik or similar) – non-negotiable.
- Super floss (thickened floss with stiff ends).
- Interdental brushes (small cone-shaped brushes).
- Soft toothbrush (electric preferred).
- Non-abrasive toothpaste (avoid whitening pastes with silica).
Daily Cleaning Protocol (5 minutes total)
Morning (2 minutes):
- Brush all surfaces of the bridge and any natural teeth with a soft brush.
- Use the water flosser on the highest comfortable setting. Aim the tip at the gum line around each implant.
- Rinse with an alcohol-free antibacterial mouthwash.
Evening (3 minutes):
- Water flosser first – this loosens debris.
- Use super floss or an interdental brush to clean under the bridge from the cheek side and tongue side.
- Brush thoroughly, paying attention to where the bridge meets the gum.
- Rinse with salt water (1 teaspoon salt in 8 oz warm water).
What to Avoid Forever
- Chewing ice, hard candy, or popcorn kernels.
- Using your teeth as tools (opening packages, biting tags off clothing).
- Smoking or tobacco products.
- Skipping annual checkups.
Professional Maintenance
Your dentist or hygienist will:
- Check implant stability by trying to move each implant with special instruments.
- Take X-rays every 12–24 months to check bone levels.
- Remove any hardened calculus (tartar) from under the bridge.
- Tighten the retaining screws if needed.
Reader note: Neglected implants can develop peri-implantitis – an infection around the implant that destroys bone. This is the #1 cause of late implant failure. Cleaning is not optional.
Risks and Complications: An Honest Discussion
No medical procedure is risk-free. Understanding the risks helps you make an informed decision and recognize early warning signs.
Common Complications (1–15% of cases)
| Complication | Likelihood | Prevention | Treatment |
|---|---|---|---|
| Post-op infection | 2–5% | Antibiotics, oral hygiene | Antibiotics, drainage |
| Implant fails to integrate (early failure) | 3–8% | Good bone quality, non-smoker | Remove implant, wait, try again |
| Swelling or bruising | 100% (mild) | Ice packs, head elevation | Resolves in 7–10 days |
| Temporary bridge loosening | 10–15% | Soft diet, avoid chewing on it | Temporary recementing |
| Nerve paresthesia (numbness) | <1% | CBCT planning, surgical guide | Usually resolves in 3–12 months |
| Sinus perforation (upper arch) | 2–4% | Avoid if sinuses are low | Self-heals; rare need for surgery |
Late Complications (after 1+ year)
- Peri-implantitis (bone loss around implant): Affects 10–20% of implant patients over 10 years. Caused by poor hygiene or smoking. Treatment: deep cleaning, sometimes surgery.
- Fractured bridge: Acrylic bridges break in 3–8% of cases over 5 years. Cause: grinding, accident, or manufacturing defect. Fix: repair or replace bridge.
- Screw loosening: Retaining screws can unscrew over time (2–5% per year). Fix: dentist retightens or replaces screw.
When to Call Your Dentist Urgently
- Severe pain not controlled by medication.
- Fever over 101°F (38.3°C).
- Pus or foul discharge from the implant site.
- One implant feels loose or clicks when you bite.
- The entire bridge moves (rare, but an emergency).
Realistic Success Rates
- 5-year success rate: 94–97% (meaning the implants are still functioning).
- 10-year success rate: 90–94%.
- 20-year success rate: 85–90% in non-smokers with good hygiene.
Smokers: Your success rate drops by 10–20% at every interval.
4 on 8 vs. Other Full-Arch Solutions: Which Should You Choose?
Let me help you compare side by side.
Comparison Table: Full-Arch Replacement Options
| Solution | Cost (per arch) | Chewing efficiency | Maintenance | Removable? | Best for |
|---|---|---|---|---|---|
| Traditional denture | 1,000–3,000 | 20–30% | Low (cleaning, adhesives) | Yes | Budget; no surgery |
| Implant-retained overdenture (2–4 implants, snaps into place) | 5,000–12,000 | 50–60% | Medium (remove to clean) | Yes (removable) | Good bone; wants removable option |
| 4 on 8 fixed bridge | 12,000–20,000 | 70–85% | Medium-high (special tools) | No | Average bone; wants fixed teeth |
| All-on-4 fixed bridge (10–14 teeth) | 15,000–28,000 | 75–85% | High (harder to clean back molars) | No | Good bone; wants full length |
| Individual implant crowns (8–12 implants) | 24,000–48,000 | 90–95% | High (floss each crown) | No | Unlimited budget; excellent bone |
Decision Guide: Ask Yourself
Choose 4 on 8 if:
- You want a fixed, non-removable solution.
- You have moderate bone volume (but not severe atrophy).
- You do not mind having 8 teeth instead of 12–14.
- You want to reduce surgical complexity and cost compared to individual implants.
Choose all-on-4 if:
- You want the longest possible bridge (includes molars).
- You have enough bone to support tilted posterior implants.
- You are willing to pay 15–25% more.
Choose implant overdentures if:
- You like the idea of removing your teeth for cleaning.
- You have a tighter budget but still want implant support.
- Your bone quality is too poor for a fixed bridge.
Choose traditional dentures if:
- You cannot undergo surgery (medical reasons).
- You have very limited funds.
- You accept the limitations of adhesives and slipping.
Reader note: Do not let anyone pressure you into a solution. A good dentist presents all options and respects your choice.
Preparing for Your 4 on 8 Journey: A Checklist
Preparation reduces stress and improves outcomes. Use this checklist.
3 Months Before Surgery
- Get a comprehensive medical exam. Your physician may adjust blood thinners or diabetes medication.
- Quit smoking completely. Ask your doctor about nicotine replacement if needed.
- Start eating a nutrient-dense diet (calcium, vitamin D, protein) to support bone healing.
- Schedule time off work (minimum 3 days, ideally 1 week).
2 Weeks Before Surgery
- Fill all prescriptions (antibiotics, pain medication, chlorhexidine mouthwash).
- Buy soft foods in advance: yogurt, pudding, applesauce, protein shakes, mashed potato mix.
- Buy cleaning tools: water flosser, super floss, soft toothbrush.
- Arrange transportation to and from surgery (if using sedation).
Day Before Surgery
- Eat a good dinner – you may not eat after midnight if using IV sedation.
- Prepare ice packs (bags of frozen peas work well).
- Wash your pillowcases and prepare extra towels (for drooling after surgery).
Day of Surgery
- Take pre-op antibiotics as directed.
- Wear comfortable, loose clothing with short sleeves (for IV access).
- Remove contact lenses, jewelry, and dentures.
- Bring a phone charger and a book – waiting time varies.
After Surgery (First Week)
- Sleep with your head elevated on two pillows.
- Apply ice packs for 20 minutes every hour while awake for the first 48 hours.
- Do not spit, rinse vigorously, or use straws for 7 days (prevents dry socket on extraction sites).
- Take pain medication before the anesthesia wears off (don’t “wait for pain”).
- Log your symptoms daily – this helps during follow-up calls.
Frequently Asked Questions (FAQ)
Q1: Is the 4 on 8 procedure painful?
During the surgery, you feel nothing if properly anesthetized. Afterward, most patients rate pain 4–6 out of 10 for the first 2–3 days. Over-the-counter ibuprofen and acetaminophen usually manage it well. Severe pain is rare and should be reported.
Q2: How long do 4 on 8 implants last?
The titanium implants themselves can last 30+ years or a lifetime if bone remains healthy. The acrylic bridge typically lasts 5–10 years before needing replacement. Zirconia bridges last 10–15+ years.
Q3: Can I get 4 on 8 on both upper and lower jaws at the same time?
Yes, many patients do both arches in one surgery. Be prepared for a longer procedure (2–3 hours) and more swelling. Some dentists prefer to stage them 3–6 months apart to make recovery easier.
Q4: Will people notice I have fake teeth?
Modern materials look very natural. Unless you smile widely and point out the bridge, most people will not know. The pink gum-colored base mimics natural tissue. Only a dentist will spot the difference.
Q5: What happens if one implant fails?
It depends. If the failed implant is not critical, the bridge may stay supported by the remaining three while you heal. If needed, the dentist can remove the failed implant, graft bone, and place a new implant later. In rare cases, the entire bridge needs remaking.
Q6: Can I eat steak and nuts with 4 on 8?
Yes, once fully healed (6+ months). Cut steak into small pieces. Chew evenly on both sides. Avoid biting directly into very hard nuts – crush them first. Use common sense.
Q7: How do I clean under the bridge?
A water flosser is the most effective tool. You aim the tip at the gum line from both the cheek and tongue sides. Super floss (with stiff ends) can be threaded underneath. Your dentist will show you the technique.
Q8: Is bone grafting always needed for 4 on 8?
No. The main advantage of 4 on 8 is that it places implants in the premolar region, which typically has better bone than the back molar area. Many patients avoid grafting entirely. Your CBCT scan will confirm.
Q9: Does insurance cover any part of 4 on 8?
Some dental insurance plans cover extractions, X-rays, and temporary prosthetics. A few premium plans cover implants at 50% up to a lifetime maximum. Medical insurance rarely covers elective implant surgery.
Q10: Can I get 4 on 8 if I have gum disease?
Not until the gum disease is treated and controlled. Active periodontitis increases implant failure risk. You will need scaling, root planing, and possibly gum surgery first. This process adds 3–6 months before implant placement.
Additional Resource
For peer-reviewed, unbiased information on dental implants, including clinical studies on success rates and materials, visit the American Academy of Implant Dentistry (AAID) patient education section:
🔗 www.aaid.com/patients
This resource offers:
- A “find an implant dentist” directory (board-certified members).
- Free downloadable guides on implant types.
- Real patient stories and videos.
Conclusion: Is 4 on 8 Right for You?
4 on 8 dental implants offer a fixed, natural-feeling, and durable solution for people missing most or all teeth in one arch. Compared to traditional dentures, they provide better chewing function, bone preservation, and confidence. Compared to all-on-4, they are often less complex and more affordable while still delivering excellent results. However, they require a significant financial investment, a commitment to daily hygiene, and the ability to undergo oral surgery. If you have moderate bone loss, realistic expectations, and a trusted implant dentist, 4 on 8 can be a life-changing, long-term answer to tooth loss.
Disclaimer:
This article is for informational purposes only and does not constitute medical or dental advice. Every patient is unique. Always consult a licensed dentist or oral surgeon for a personal examination and treatment plan. The author and publisher are not liable for any actions taken based on this content. Do not use this information to self-diagnose or delay seeking professional care.