Signs of Dental Implant Rejection
So, you’ve invested in a dental implant. Maybe you are still in the healing phase, or perhaps you’ve had your new tooth for years. Either way, a small question might be lingering in the back of your mind: “How do I know if something is wrong?”
Let’s be honest. The word “rejection” sounds scary. It brings up images of your body fighting against a foreign object. But here is the good news first: true rejection of a dental implant is rare. Modern titanium implants are biocompatible, meaning your body usually accepts them like a trusted friend.
However, complications do happen. The difference between a simple infection and true failure often comes down to knowing what to look for.
This guide walks you through every possible sign of dental implant rejection in plain, simple English. No medical degree required. By the end, you will know exactly when to relax and when to pick up the phone to call your dentist.
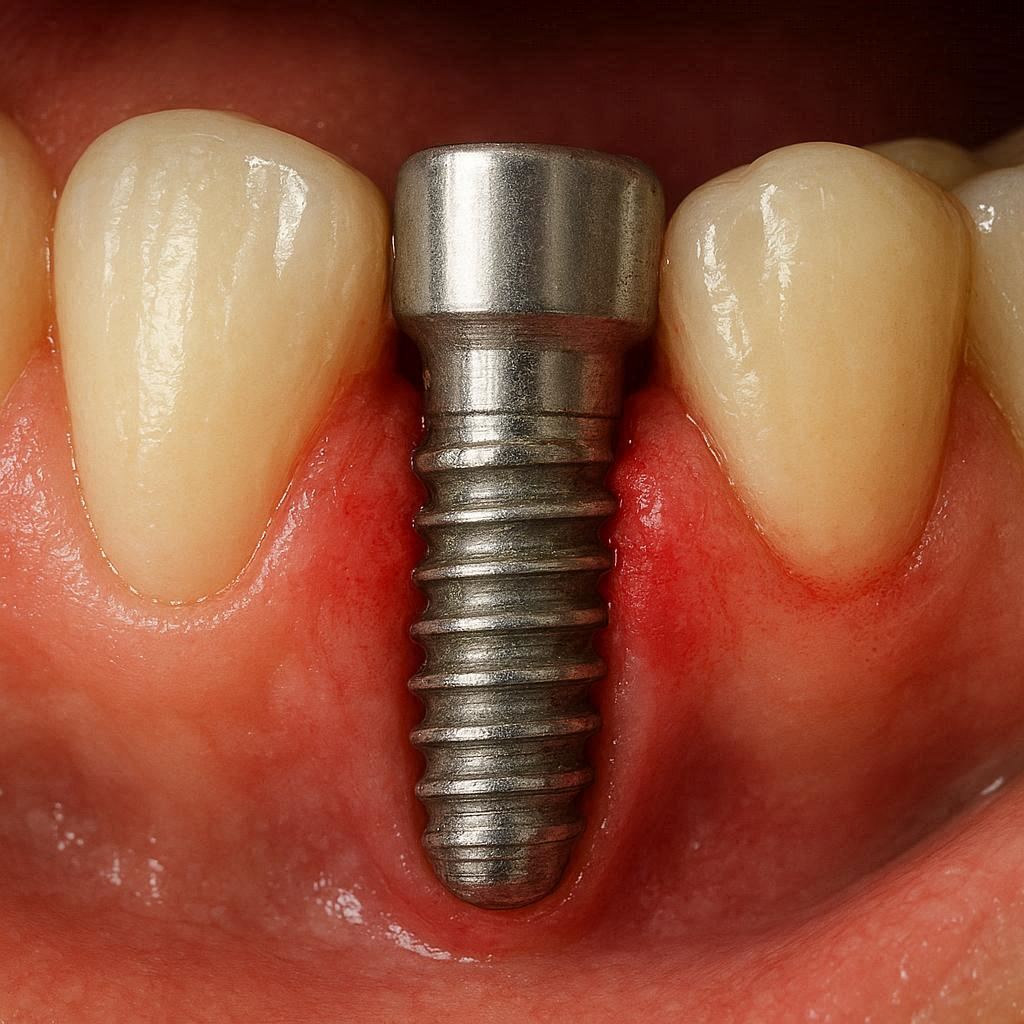
Understanding “Rejection” vs. “Failure”
Before we dive into the signs, we need to clear up a huge misunderstanding. In the medical world, “rejection” means your immune system actively attacks the implant. This is common in organ transplants. For dental implants, this almost never happens.
What most people call signs of dental implant rejection are actually signs of failed osseointegration or peri-implantitis.
- Osseointegration: The process where your jawbone grows tightly around the titanium screw. Think of it like a tree’s roots growing into the soil.
- Peri-implantitis: An infection around the implant that destroys the bone holding it in place.
Important Note: True allergic reactions to titanium exist, but they affect less than 0.6% of patients. If you are reading this, chances are high you are dealing with an infection or healing issue, not an allergy.
The Timeline: When Problems Usually Show Up
Dental implant problems do not all happen at once. They follow a timeline. Knowing when to worry helps you stay calm.
| Phase | Time After Surgery | Risk Level |
|---|---|---|
| Early Failure | 0 to 4 months | Moderate – The bone never grows onto the implant. |
| Late Failure | 4 months to 1 year | Low – Usually linked to biting forces. |
| Long-term Failure | 1+ years | Low to Moderate – Almost always infection (peri-implantitis). |
If you are in the first three months, your job is to watch for healing problems. If you are past the one-year mark, your job is to watch for gum health.
The 10 Most Common Signs of Dental Implant Rejection (And What They Actually Mean)
Let’s get to the heart of the article. Here are the physical signals your body sends when an implant is not happy.
1. A Spinning or Wobbly Tooth (The Biggest Red Flag)
This is the king of all warning signs. A healed, successful implant is fused to your bone. It should not move. Not even a little bit.
If you feel the crown (the fake tooth part) spinning in circles, or if you can wiggle it side to side, the implant has failed.
- What it feels like: Like a loose battery in a remote control. A slight click or rotation when you chew.
- What it means: The bone never attached (early failure), or the bone has broken down (late failure).
- What to do: Do not chew on that side. Call your dentist immediately. This requires removal in most cases.
2. Pain That Gets Worse, Not Better
Some discomfort after surgery is normal. You just had a screw drilled into your jawbone! But here is the rule: Pain should decrease every single day.
Normal healing: Day 3 is worse than Day 7. Day 14 is almost pain-free.
Sign of rejection: Day 14 is worse than Day 7. The pain wakes you up at night. It feels deep inside your jaw, like a toothache in a tooth that doesn’t exist.
This deep, throbbing pain usually means the implant is pressing on a nerve, or an infection is building pressure inside the bone.
3. A Low-Grade Fever That Won’t Quit
Your body runs a fever when it is fighting a war. After dental implant surgery, a slight rise in temperature for 24 hours is fine. But a fever that lasts three days or longer is your body saying, “I cannot handle this invader.”
- Watch for: 99.5°F to 101°F (37.5°C to 38.3°C) that persists.
- Why it matters: It suggests a systemic infection. The bacteria may be spreading beyond the implant site.
- Action step: Any fever 48 hours post-op requires a call to your surgeon.
4. Swelling That Spreads to Your Eye or Neck
Localized swelling on your cheek is normal. You look like a chipmunk for a few days. That is fine.
Not normal: The swelling starts small and then creeps upward toward your eye, or downward toward your chin and neck.
- Why this is dangerous: It suggests the infection is traveling through tissue planes. If it reaches your airway, it becomes an emergency.
- Visual sign: You cannot see the natural curve of your jawbone anymore. Your face looks like a smooth balloon.
5. The “Bad Taste” That Doesn’t Brush Away
Imagine a salty, metallic, or sour taste that lives in your mouth no matter how many times you brush. This is often a sign of an implant sinus communication (upper jaw) or a chronic leak.
In the upper jaw, implants sit very close to your sinus cavity. If the implant perforates the sinus or gets infected, fluid from the infection drips down into your mouth.
- The test: Rinse with salt water. If the bad taste comes back within 10 minutes, call your dentist.
- Associated sign: A runny nose on only one side when you lean forward.
6. A Pimple on Your Gum (The Fistula)
Look in the mirror. Do you see a small white or red pimple on the gum directly over your implant? This is not acne. This is a fistula – a tunnel your body creates to drain pus.
- What happens: You might press on the gum, and pus (yellowish thick liquid) comes out.
- Smell: It often smells bad, like rotten food.
- Meaning: The infection has found an escape route. The bone is actively being destroyed.
Reader Note: Do not pop it. Popping it only relieves pressure temporarily. The infection remains deep in the bone.
7. A Receding Gum Line That Shows Metal
Your gums should hug the implant crown like a turtleneck. If that turtleneck starts sliding down, exposing the shiny metal of the implant or the abutment, something is wrong.
- Slow recession (over years): This might just be aggressive brushing or thin gum tissue.
- Fast recession (over weeks or months): This is almost always caused by bone loss underneath.
You cannot lose gum tissue without losing bone first. If you see more metal this month than you did last month, ask for an X-ray.
8. Difficulty Screwing In the Abutment (For Your Dentist)
You will not feel this one yourself. But your dentist will. During a check-up, if your dentist tries to tighten the screw that connects the crown to the implant and it feels “mushy” or won’t tighten, the implant is failing.
- The analogy: Trying to screw a hook into drywall when the drywall has turned to dust.
- What you might notice: The crown feels like it is “squishing” when you bite down.
9. Unexplained Numbness or Tingling
Numbness right after surgery is common because of local anesthesia. But that wears off in 6-8 hours.
Permanent or long-term numbness in your lip, chin, or gum is a sign of nerve damage. This is not exactly “rejection,” but it is a serious complication that mimics the experience.
- What it feels like: You bite your lower lip but feel no pain. Your chin feels like it fell asleep three days ago and never woke up.
- Causes: The implant is too long and is touching the inferior alveolar nerve.
- Outcome: The implant might need to be removed to relieve pressure on the nerve.
10. The Clicking or Crunching Sound
When you chew, do you hear a quiet clicking sound? Or worse, a crunching sound like stepping on dry leaves?
- Clicking: Usually means the crown is loose on the abutment. Fixable.
- Crunching: This is a bad sign. It means the implant is grinding against dead bone or a loose fragment of bone. This is mechanical failure.
The Table of Truth: Normal vs. Worrisome Signs
To make things crystal clear, here is a side-by-side comparison.
| Your Symptom | Normal Healing (Relax) | Sign of Rejection (Call Dentist) |
|---|---|---|
| Pain | Dull ache that improves daily. Controlled by ibuprofen. | Sharp, shooting, or throbbing that gets worse. Keeps you awake. |
| Swelling | Peaks at day 2-3, then goes down. Soft and puffy. | Increases after day 4. Hard, hot, or spreading to the eye/neck. |
| Bleeding | Pink saliva for 24 hours. Light oozing when brushing. | Heavy, bright red bleeding. Bleeding that starts suddenly weeks later. |
| Mobility | None. Zero. The implant feels like a rock. | Any wiggle. Any rotation. Any clicking movement. |
| Gum Color | Pink or slightly red (first week only). | Bright red, purple, or white/grey. |
| Smell/Taste | Slight metallic taste from the titanium (rare). | Bad breath that doesn’t go away. Salty or sour taste of pus. |
Why Do Dental Implants Really Fail? (The Honest Causes)
Understanding the “why” helps you prevent the “what.” Let’s look at the real reasons implants fail, without the scary stories.
Smoking (The Number One Enemy)
If you smoke, your risk of failure doubles or triples. Nicotine constricts blood vessels. Your bone needs blood to heal. No blood = no bone growth.
Real talk: A smoker has a 15-20% failure rate. A non-smoker has a 95-98% success rate. The numbers do not lie.
Poor Oral Hygiene
An implant cannot get a cavity, but it can get infected. The gum attachment to an implant is weaker than the attachment to a natural tooth. Bacteria love this weak spot. If you do not floss around your implant, you are inviting peri-implantitis.
Grinding Your Teeth (Bruxism)
Your natural teeth have a ligament that acts like a shock absorber. Implants do not. They are rigid. If you grind your teeth at night, you are applying 500+ pounds of pressure directly to a rigid screw. Eventually, something breaks – either the crown, the screw, or the bone.
Medical Conditions
- Uncontrolled diabetes: High blood sugar slows healing and encourages infection.
- Osteoporosis medications (bisphosphonates): These can prevent bone from healing after implant placement.
- Autoimmune diseases: Conditions like lupus or rheumatoid arthritis make your body more likely to fight the implant.
Overheating the Bone During Surgery
This is on the surgeon, not you. If the drill gets too hot (over 47°C / 117°F), it kills the bone cells. The bone dies before the implant ever goes in. You cannot see this. You can only feel the result when the implant wobbles months later.
What Does “Rejection” Actually Feel Like? A Reader’s Description
“I knew something was wrong by week six. The pain wasn’t terrible, but it was always there. A 2 out of 10 that never became a 0. Then I noticed I could push my tongue against the crown and feel a tiny ‘tick’ of movement. My dentist confirmed the bone never grew. They removed the implant in ten minutes. The relief was instant.” — James, 54
“For me, it was the taste. A constant, salty, gross taste. I brushed five times a day. Nothing worked. Turns out, I had a sinus infection caused by the implant poking into my sinus. Removal fixed the taste in two days.” — Linda, 47
Step-by-Step: What to Do If You See These Signs
Do not panic. Follow this logical flow.
Step 1: The Home Check (24 Hours)
- Stop chewing on that side.
- Switch to warm salt water rinses (1 teaspoon salt in 1 cup warm water) three times a day.
- Take a photo of your gums with your phone. Compare it tomorrow.
Step 2: The Pain Test
- Take your normal painkiller (ibuprofen or acetaminophen).
- Does the pain go away completely? Probably fine.
- Does the pain stay the same or get worse? Call the dentist.
Step 3: The Mobility Test (Gentle!)
- Use a clean spoon handle. Tap the crown gently.
- Tap a natural tooth nearby. Listen to the sound.
- A healthy implant sounds high-pitched and solid (like tapping a rock).
- A failing implant sounds dull and muffled (like tapping a pencil on a cardboard box).
Step 4: Call Your Dentist
When you call, say these three things clearly:
- “My dental implant feels loose.”
- “I have pus or a bad taste.”
- “The pain is keeping me awake.”
Do not say: “I think it’s rejecting.” Let them diagnose.
Can a Rejecting Implant Be Saved?
Yes. Sometimes. It depends on how much bone is left.
| Problem | Is it savable? | The Fix |
|---|---|---|
| Loose crown (implant is tight) | Yes, easily. | Tighten the screw. |
| Infected gum (no bone loss) | Yes. | Deep cleaning + antibiotics. |
| Mild bone loss (peri-implantitis) | Maybe. | Surgery to clean the implant surface + bone graft. |
| Moderate bone loss (implant still stable) | 50/50. | Laser therapy + rigorous home care. |
| Implant is mobile (any movement) | No. | Remove the implant. Let bone heal. Try again in 6 months. |
| Fractured implant (broken screw) | No. | Removal required. |
The golden rule: Once the implant moves, it is game over. Movement means no bone attachment. You cannot glue bone back to titanium.
The Removal Process (It’s Not as Scary as You Think)
If your implant truly fails, you need it removed. Here is the honest truth about what happens.
- The procedure: Simpler than the placement. The dentist uses a special tool (like a reverse drill) to unscrew the implant.
- Anesthesia: Yes, you are numb. You feel pressure, not pain.
- Time: 10 to 20 minutes.
- Recovery: Easier than the original surgery. The hole fills with blood, then bone.
- What happens next: You wait 4 to 6 months for the bone to heal. Then, 80% of the time, you can try a new implant (often larger or placed at a different angle).
Quote from an oral surgeon: “I remove failing implants every week. Patients always say the same thing: ‘I should have done this months ago.’ The relief from chronic pain is immediate.”
Preventing Rejection: Your Daily Checklist
You have control over more than you think. Follow this checklist for a healthy implant.
Daily Habits (Non-Negotiable)
- Floss around the implant with special implant floss or a water flosser.
- Use a soft-bristle brush. Never metal scrapers.
- Rinse with alcohol-free mouthwash (alcohol dries out gum tissue).
Weekly Habits
- Use a rubber tip stimulator to massage the gum around the implant.
- Check for bleeding when you floss. Pink on the floss = inflammation.
Yearly Habits (Dentist Visit)
- Get a periapical X-ray (not just a bitewing). This shows the bone level around the screw.
- Have your dentist check the torque (tightness) of the abutment screw.
- Get a professional cleaning with plastic instruments only (metal scalers scratch implants).
Frequently Asked Questions (FAQ)
Q1: Can my body reject a dental implant after 10 years?
Yes, but it is almost never “rejection.” It is peri-implantitis – a slow, silent infection that eats away bone over years. That is why you need annual X-rays even a decade later.
Q2: How long after implant surgery is rejection most likely?
The highest risk window is the first 4 months. That is when osseointegration either happens or fails. After one year, the risk drops significantly unless you develop gum disease.
Q3: Will antibiotics fix a rejecting implant?
Antibiotics fix infections, not loose implants. If the implant is stable but the gum is red, antibiotics may help. If the implant wobbles, antibiotics do nothing. You need removal.
Q4: Can I feel a dental implant rejecting?
Yes. The most common first sign is a dull, persistent ache that feels like it is coming from deep inside the jawbone. Or a feeling that the tooth is “too tall” when you bite.
Q5: Is titanium allergy real?
Yes, but extremely rare (less than 1% of patients). Symptoms include chronic hives, eczema, or swelling far from the implant site. A blood test ( MELISA) can confirm it.
Q6: What happens if I ignore the signs?
Ignoring a loose or infected implant leads to bone destruction. You could lose so much jawbone that a second implant becomes impossible. You might need a complex bone graft or a denture.
Q7: Can I get a refund if my implant fails?
Most dental implants come with a manufacturer warranty (5 years to lifetime) for the hardware breaking. But the surgical fee is rarely refundable. Ask your dentist for their policy before surgery.
Q8: Does smoking cause immediate failure?
Not immediately, but it dramatically slows healing. A smoker might feel fine for 2 months, then suddenly the implant fails because the bone never fully matured. Quitting for 2 weeks before and 2 months after surgery is the gold standard.
Additional Resource: Where to Get Help
For readers who want to go deeper, the American Academy of Implant Dentistry (AAID) offers a free “Find a Specialist” tool. You can also read patient-reviewed guides on implant maintenance.
👉 Recommended Link: AAID Patient Resources – Dental Implant Information
Note: This resource provides dentist referrals and educational brochures. It is not a substitute for medical advice.
A Final Note of Encouragement
If you are reading this because you are worried about your own implant, take a deep breath. Dental implants have a success rate of over 95% over 10 years. That is better than hip replacements, knee replacements, and even root canals.
The signs we discussed are your body’s way of sending you a letter. Most of the time, the letter says, “Please floss better.” Less often, it says, “Please see your dentist.” Very rarely does it say, “This is an emergency.”
You are doing the right thing by educating yourself. Now, go look in the mirror. Brush gently. Floss carefully. And if something feels off, trust your gut. Your dentist would rather see you ten times for false alarms than miss one real problem.
Conclusion
- Know the red flags: Persistent pain, any movement of the implant, or a pimple on the gum are the clearest signs of trouble.
- Act early but don’t panic: Most “rejection” is actually treatable infection or loose screws, not total failure.
- Prevention is power: Daily flossing, quitting smoking, and yearly X-rays keep your implant solid for decades.
Disclaimer
This article is for informational purposes only and does not constitute medical advice. Always consult a licensed dentist or oral surgeon for personal health concerns. Do not delay seeking professional care based on content you read online.


