Tooth Implant Side Effects: A Complete, Honest Guide for Patients
So, your dentist has recommended a dental implant. Or maybe you are in the middle of your research, reading about titanium posts and crowns. You feel excited about a permanent solution, but a small voice in your head asks: What could go wrong?
It is smart to ask that question.
Many online articles promise that implants are perfect. They say the success rate is 95% or higher. And that is true for healthy, straightforward cases. But “successful” does not always mean “completely free of side effects.”
You deserve a realistic picture. You deserve to know what normal discomfort looks like, and what a real problem looks like.
This guide covers everything: common short-term effects, long-term risks, neurological symptoms, sinus issues, gum recession, and even the mental side of recovery. No fake data. No fear-mongering. Just honest, useful information.
Let’s walk through this together.
What Are Tooth Implants? A Quick Reminder
Before we talk about side effects, let us make sure we are on the same page.
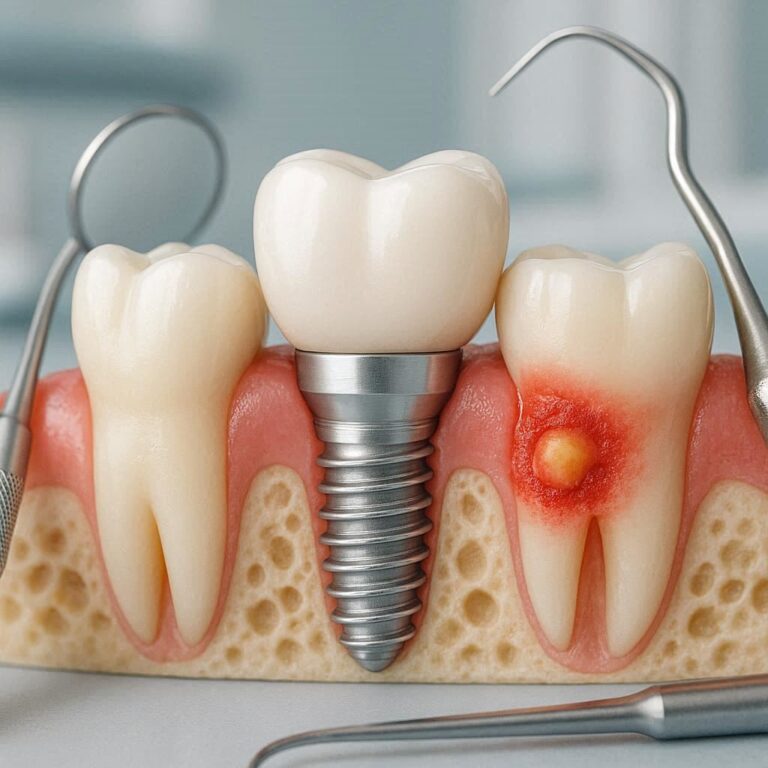
A dental implant has three parts:
- The post: A small screw, usually made of titanium, that goes into your jawbone.
- The abutment: A connector piece that sits on top of the post.
- The crown: The fake tooth that everyone sees.
The surgery places the post into your bone. Over a few months, your bone grows around the screw. This is called osseointegration. Once the bone locks the post in place, the dentist adds the crown.
It is a beautiful system. But it is still a medical procedure. And any medical procedure has side effects.
Important Note: Side effects are not the same as complications. A side effect is a predictable, often temporary reaction (like swelling). A complication is an unexpected problem (like a nerve being cut). This guide covers both, but we will separate them clearly.
Table of Contents
- Short-Term Side Effects (The First Two Weeks)
- Long-Term Side Effects (Months or Years Later)
- Neurological and Nerve-Related Effects
- Sinus Problems and Nasal Side Effects
- Gum and Bone Side Effects
- Psychological and Emotional Effects
- Rare but Serious Complications
- Who Has a Higher Risk of Side Effects?
- How to Minimize Your Risk
- Real Patient Experiences (Quotes)
- When to Call Your Dentist Immediately
- Frequently Asked Questions (FAQ)
- Additional Resources
- Conclusion
1. Short-Term Side Effects (The First Two Weeks)
Let us start with what most people feel right after surgery. None of these are dangerous, but they can be uncomfortable. Knowing about them makes them less scary.
Pain and Discomfort
You will feel something. If a dentist drills into your bone, you should expect tenderness.
- Day 1-3: Moderate pain, like a deep bruise. Painkillers (ibuprofen or prescribed medication) usually manage it well.
- Day 4-7: Mild soreness. More annoying than painful.
- Day 7-14: Occasional twinges, especially when you chew near the area.
Most patients say the pain is less than a tooth extraction. But if you had a bone graft at the same time, expect more discomfort.
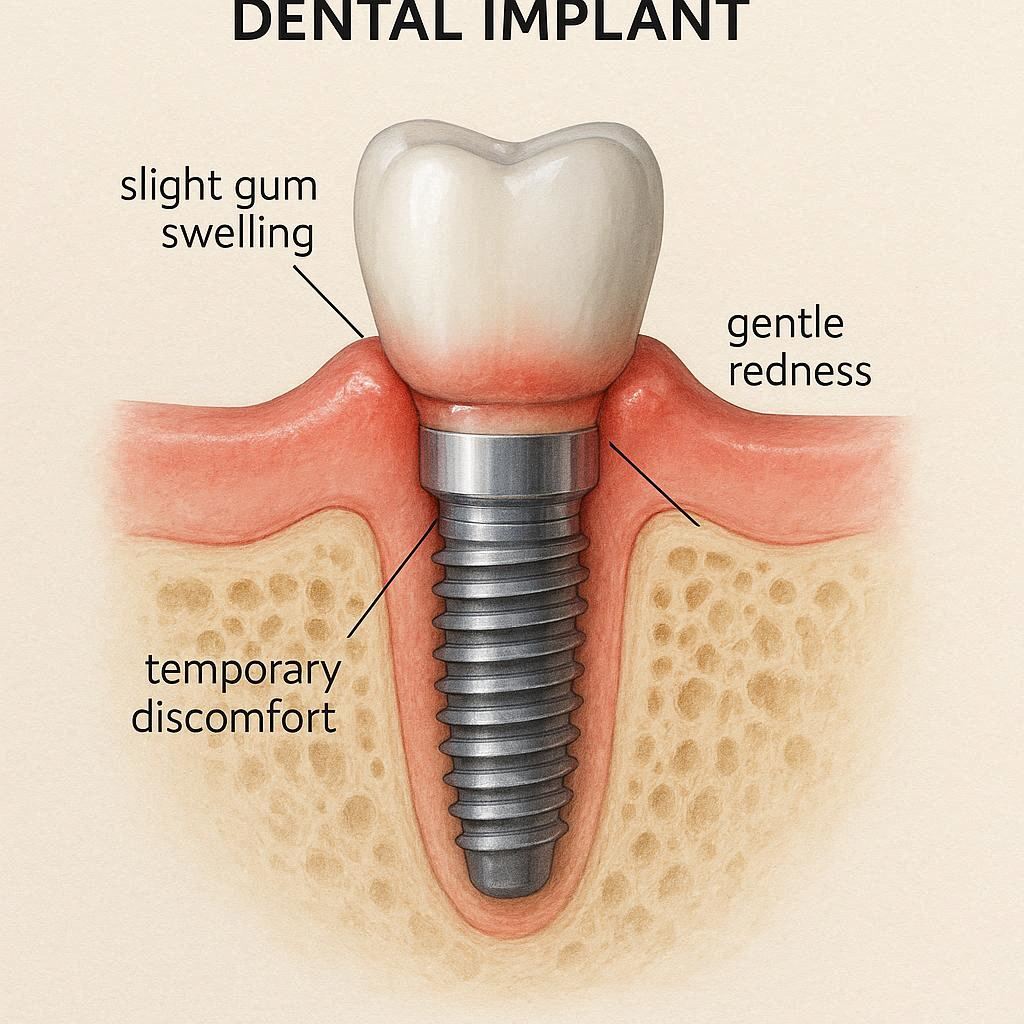
Swelling of the Face and Gums
Swelling is your body’s natural response to surgery. It usually peaks around 48 hours after the procedure.
- What it looks like: A puffy cheek near the implant site. Sometimes the swelling spreads to your eye or neck (mildly).
- What helps: Ice packs for the first 24 hours (20 minutes on, 20 off). After 48 hours, warm compresses.
Swelling should go down noticeably by day 5. If it gets worse after day 3, call your dentist. That could be an infection.
Bleeding and Oozing
Some pink-tinged saliva is normal for 24-48 hours.
- Light bleeding: You see a little red when you spit.
- Oozing: Your saliva looks like strawberry juice.
What is NOT normal: Bright red blood that pools in your mouth. That is active bleeding and needs immediate attention.
Reader Tip: Do not spit forcefully for the first three days. Do not use a straw. Both actions can pull out the blood clot that protects the surgery site.
Bruising on the Skin
This surprises many people. You might see a yellow, green, or purple mark on your chin, neck, or under your jaw.
Why does this happen? Gravity pulls small amounts of leaked blood down through the tissue.
Bruising is harmless. It looks dramatic, but it is just a cosmetic issue. It fades in 7-10 days.
Difficulty Opening Your Mouth (Trismus)
Your jaw muscles get irritated during surgery. They might tighten up as a protective reflex.
- Mild case: You can only open your mouth one inch wide.
- Moderate case: Eating a sandwich is impossible.
This usually resolves in 3-7 days. Gentle stretching helps. If it lasts longer than two weeks, tell your dentist.
Bad Taste or Bad Breath
A metallic taste is common from the titanium post or any blood left in the mouth. Also, you cannot brush the surgery site aggressively, so food debris collects.
- Normal for: 5-10 days.
- Red flag: A foul, rotten smell or taste combined with increasing pain. That could mean an infection.
Nausea from Medication
The antibiotics or painkillers might upset your stomach. Some people also swallow a little blood during surgery, which irritates the stomach.
How to handle it:
- Take medication with food.
- Ask your dentist for anti-nausea medicine if needed.
- Sip ginger tea or flat soda.
Summary Table: Short-Term Side Effects
| Side Effect | Typical Duration | Severity (1-5) | When to Worry |
|---|---|---|---|
| Pain | 3-7 days | 2-4 | Beyond 10 days |
| Swelling | 3-5 days | 2-3 | Worsens after day 3 |
| Bleeding | 1-2 days | 1 | Bright red, heavy flow |
| Bruising | 7-10 days | 1 | None (harmless) |
| Trismus | 3-7 days | 2-3 | Longer than 2 weeks |
| Bad taste | 5-10 days | 1 | Foul odor + fever |
| Nausea | 1-3 days | 1-2 | Vomiting more than 1 day |
2. Long-Term Side Effects (Months or Years Later)
Once you heal from surgery, you might think the risks are over. Usually, they are. But some side effects show up later.
Gum Recession Around the Implant
Over time, your gum tissue might pull back. You start to see the metal edge of the implant or the abutment.
Why this happens:
- The gum was thin to begin with.
- You brush too hard in that area.
- The crown shape irritates the gum.
- Natural aging.
Is it dangerous? Not really, unless it becomes severe. But it looks unpleasant and can trap food. If the recession is bad, a gum graft might fix it.
Bone Loss Around the Implant (Peri-Implantitis)
This is the big one. Peri-implantitis is an infection that destroys the bone holding your implant.
Early signs:
- Gums that bleed when you brush near the implant.
- Red or purple gums.
- A pocket depth deeper than 5mm.
Late signs:
- The implant feels loose.
- You see visible bone loss on an X-ray.
- Pus comes out next to the implant.
Peri-implantitis does not happen to everyone. Studies suggest it affects about 10-20% of implants over 10 years. But for heavy smokers or people with poor oral hygiene, the risk is much higher.
Important: You can treat peri-implantitis if you catch it early. Deep cleanings, laser therapy, or minor surgery can save the implant. If you ignore it, the implant will fail.
Implant Loosening
Your implant should never move. It is fused to bone. If it feels like a wobbly tooth, something is wrong.
Common causes:
- Peri-implantitis (bone loss).
- The crown screw came loose (this is a simple fix, not a failure).
- You grind your teeth (bruxism) and broke the bond.
A truly loose implant usually requires removal.
Allergic Reaction to Titanium
This is extremely rare. Less than 1% of people have a true titanium allergy.
Symptoms:
- Chronic swelling around the implant.
- A rash on your face or neck.
- Eczema-like patches on your skin.
- Persistent burning sensation in the gums.
If you already know you react to metal jewelry (nickel allergy), you can ask for a titanium allergy test before surgery. Zirconia (ceramic) implants are an alternative.
Food Trapping and Bad Breath
Implants do not have a ligament like natural teeth. The gum attaches differently. This creates a tiny space where food can hide.
What happens:
- You eat popcorn. A kernel gets stuck.
- You cannot floss it out easily.
- Bacteria grow. Your breath smells.
Solution: Special floss (superfloss), water flossers, and interdental brushes work well. Your hygienist will teach you.
Sensitivity to Cold or Hot Drinks
Natural teeth have nerves that feel temperature. Implants do not. So why do some people feel sensitivity?
Two reasons:
- Adjacent natural teeth: The cold drink touches the neighboring tooth, which does have a nerve.
- Referred sensation: Your brain gets confused during healing.
This usually fades after 6-12 months. If it stays sharp, you might have a problem with a nearby tooth, not the implant.
3. Neurological and Nerve-Related Effects
This section needs honesty. Nerve injuries are not common, but when they happen, they can change your life for months or years.
Numbness of the Lip, Chin, or Tongue
The lower jaw contains the inferior alveolar nerve. It gives feeling to your lower lip and chin. The lingual nerve gives feeling to your tongue.
If the dentist drills too deep or too close, the nerve can be:
- Stretched (temporary numbness).
- Compressed (numbness that lasts weeks).
- Cut (permanent numbness).
How common is this?
- Temporary numbness: 2-5% of lower jaw implants.
- Permanent numbness: Less than 1% (but it happens).
What does it feel like?
Imagine novocaine that never wears off. Or worse, a “pins and needles” sensation that feels like your face is asleep forever.
Can it be fixed? Sometimes. Anti-inflammatories, steroids, or even microsurgery can help. But if the nerve is severed completely, the numbness is permanent.
Altered Taste (Dysgeusia)
Some patients report that food tastes different after an upper implant.
Why? The surgery site is close to the nerves that control taste in the soft palate. Also, some bone graft materials or antibiotics can affect taste.
Typical outcome: Taste returns to normal in 3-6 months. In rare cases, it stays altered long-term.
Chronic Pain Syndrome (Atypical Odontalgia)
This is a strange one. The implant looks perfect on X-rays. The gum is healthy. But you feel deep, burning, aching pain where the implant sits.
What is happening? The nerves become hypersensitive after trauma. They send pain signals even though nothing is wrong.
Treatment: This is not a dental problem anymore. It becomes a nerve pain problem. Neurologists or pain specialists use medications like gabapentin or low-dose antidepressants.
Reader Note: Before assuming you have atypical pain, rule out real problems first. Get a second opinion. Get a CBCT scan (3D X-ray). Do not accept “it’s in your head” without proper testing.
4. Sinus Problems and Nasal Side Effects
Upper implants (for your top back teeth) sit very close to your maxillary sinus. The sinus is an air-filled space in your cheekbone.
Sinus Perforation During Surgery
This happens when the implant post pokes through the bone into the sinus cavity.
Signs during surgery: The dentist sees bleeding from the nose. Or they hear air whistling through the implant site.
Signs after surgery:
- Liquid comes out of your nose when you drink.
- You taste salty fluid in the back of your throat.
- Your voice sounds nasal.
- You cannot blow your nose without air escaping into your mouth.
What happens next? Small perforations heal on their own. Larger ones need a repair procedure. Your dentist will give you strict instructions: no blowing your nose for weeks. No flying in airplanes. No drinking through a straw.
Chronic Sinusitis After Healing
Even if the surgery goes perfectly, an upper implant can irritate your sinus over time.
Symptoms:
- Frequent sinus headaches.
- Pressure under your cheekbone.
- Post-nasal drip that never goes away.
- One nostril is always stuffed.
Why? The implant tip sits inside the sinus cavity (intentionally or unintentionally). Your body sees it as a foreign object and keeps the sinus inflamed.
Solution: Sometimes medication works. Sometimes the implant needs to be shortened or removed.
Nosebleeds
Minor nosebleeds for the first few days are normal. The sinus lining is delicate and can ooze a little blood.
Heavy, repeated nosebleeds are not normal. That suggests a larger perforation or a torn blood vessel.
Summary Table: Sinus-Related Side Effects
| Side Effect | Frequency | Typical Treatment |
|---|---|---|
| Minor perforation | 5-10% of upper implants | Heals on its own |
| Major perforation | 1-2% | Surgical repair |
| Chronic sinusitis | 2-5% | Medication or implant removal |
| Nosebleeds (mild) | Common | Rest, no nose blowing |
5. Gum and Bone Side Effects
Your gums and jawbone are the foundation. If they fail, the implant fails.
Gum Overgrowth (Hyperplasia)
Sometimes the gum grows over the implant crown. You look in the mirror and see a pink bubble covering part of your fake tooth.
Why? Poor oral hygiene, certain medications (like blood pressure drugs), or a poorly shaped crown.
Fix: A dentist can trim the extra gum tissue with a laser. But if the cause is poor hygiene, it will grow back.
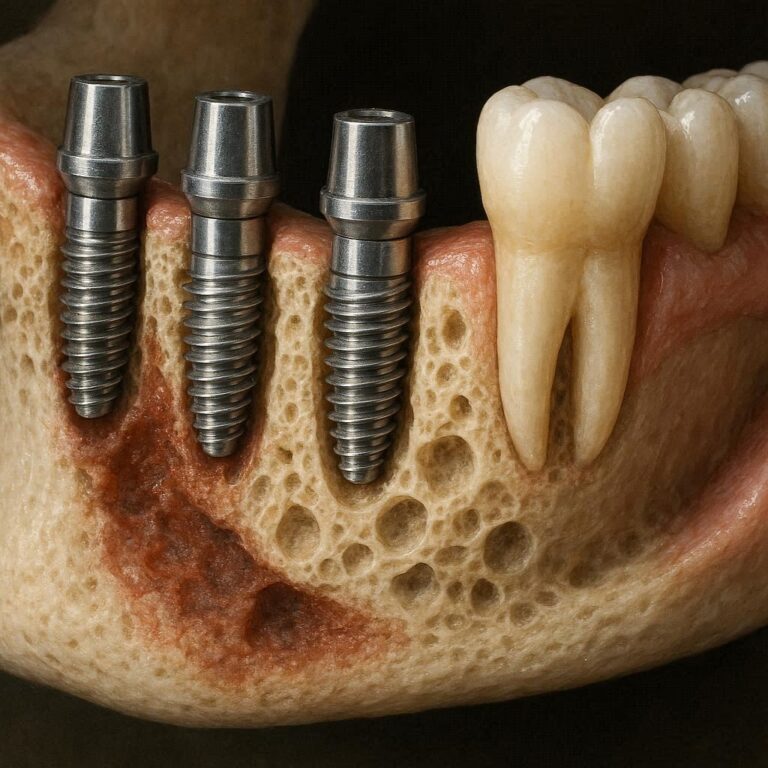
Bone Graft Complications
Many people need a bone graft before an implant. The graft creates enough bone volume to hold the post.
Side effects of bone grafts:
- Graft rejection: Your body breaks down the graft material instead of using it. This looks like bone loss on X-rays.
- Graft infection: Pain, swelling, and pus. Requires antibiotics and possibly removing the graft.
- Graft exposure: The gum opens up, and you see white granules of bone material. This usually heals on its own but needs monitoring.
Fenestration or Dehiscence
These are fancy words for “the bone is too thin, and the implant is poking through.”
- Fenestration: A hole in the bone, but the gum covers it.
- Dehiscence: A hole in the bone and the gum is missing. You can see the implant threads.
What happens? The implant is not fully surrounded by bone. It has a higher failure risk. You might need a second bone graft surgery to cover the exposed threads.
Metal Show-Through
If your gum tissue is very thin and you have a metal implant, the gum can look gray or blue.
This is purely cosmetic. It does not hurt. But it bothers people with high smile lines. A ceramic implant or a gum graft can hide it.
6. Psychological and Emotional Effects
We focus so much on the body that we forget the mind. Dental implant surgery affects your emotions too.
Anxiety Before the Procedure
Waiting for surgery is hard. You imagine the drill. You worry about pain. You read horror stories online (please stop doing that).
Normal symptoms:
- Trouble sleeping the night before.
- Feeling irritable.
- Wanting to cancel the appointment.
Coping strategies:
- Ask your dentist about sedation options.
- Bring headphones and listen to music during surgery.
- Remind yourself: millions of people have done this successfully.
Post-Surgery Depression
This sounds dramatic, but it happens. After the numbing wears off, you feel sore, swollen, and tired. You cannot eat your favorite foods. You look in the mirror and see a puffy, bruised face.
For some people, this triggers a low mood that lasts a week or two.
What to tell yourself: This is temporary. By day 10, you will feel like yourself again.
Body Dysmorphic Concerns
A small number of patients become obsessed with how the implant looks. They stare at it in the mirror. They think it is too big, too small, too gray, or too shiny.
Reality check: Most implants look excellent. But if you had a front tooth replaced, it might not match perfectly. The color might be slightly off. The shape might feel different.
If this drives you crazy, talk to your dentist about revising the crown. Most will re-do it once at no charge if you truly hate it.
Regret and Second-Guessing
“I should have just gotten a bridge.” “I wasted my money.” “I made a huge mistake.”
These thoughts are common during the first few weeks of recovery. You are in pain, you cannot chew, and you are frustrated.
Remember: Almost everyone stops feeling regret once they fully heal and can eat normally again. Give yourself time.
Quote from a real patient: “For the first month, I cried every day. I thought I ruined my mouth. Now, three years later, I forget I even have an implant. It was worth the hard weeks.” — Sarah, 42
7. Rare but Serious Complications
Let us be clear: these are rare. They affect less than 1% of implant patients. But you deserve to know about them.
Osteomyelitis (Bone Infection)
This is a deep infection inside your jawbone. It does not just affect the gum. It affects the bone itself.
Symptoms:
- Fever over 101°F (38.3°C).
- Severe jaw pain that does not stop.
- Swelling that makes your face look deformed.
- Pus draining from a hole in your gum.
Treatment: IV antibiotics in a hospital. Sometimes surgery to remove infected bone.
Osteonecrosis (Bone Death)
The bone around the implant dies. It turns into dead tissue that cannot hold the implant.
Who is at risk? People who took bisphosphonate drugs (like Fosamax, Actonel, or Boniva) for osteoporosis. Also, patients who had radiation for cancer in the head or neck.
If you took these drugs: Tell your dentist before surgery. You may not be a good candidate for implants.
Implant Migration
The implant moves through the bone on its own. It starts in the correct spot and ends up somewhere else.
In the upper jaw, a migrating implant can end up in the sinus or even the nose. In the lower jaw, it can drift toward the nerve.
Why? Extreme bone loss or a very damaged surgical site.
Solution: Surgical removal. This is complex and usually done by an oral surgeon.
Aspiration or Ingestion
A small part (like a healing cap or a tiny screw) can come loose while you sleep or eat. You might swallow it or breathe it into your lung.
- Swallowed: Usually passes through your digestive system without harm.
- Inhaled (into the lung): Medical emergency. You need a bronchoscopy to remove it.
Prevention: Your dentist will torque (tighten) all screws properly. But things can still loosen over time. Go to your regular checkups so the dentist can re-tighten anything loose.
8. Who Has a Higher Risk of Side Effects?
Not everyone faces the same risks. Some people sail through implant surgery with zero problems. Others struggle.
High-Risk Groups
| Risk Factor | Why It Increases Side Effects | What to Do |
|---|---|---|
| Smoking | Reduces blood flow. Slows healing. Increases infection risk 3x. | Quit for 2 weeks before and 2 months after surgery. |
| Diabetes (uncontrolled) | High blood sugar impairs healing and immunity. | Get your A1C below 7 before surgery. |
| Bruxism (teeth grinding) | Crushing forces can loosen the implant or break the crown. | Wear a nightguard. Consider fewer implants (not ideal for heavy grinders). |
| Osteoporosis drugs | Risk of osteonecrosis (bone death). | Be honest with your dentist. Consider alternatives. |
| Poor oral hygiene | Leads to peri-implantitis and gum disease. | Improve your home care before surgery. |
| Heavy alcohol use | Slows healing. Increases bleeding risk. | Reduce intake significantly for 1 month after surgery. |
| Autoimmune diseases (lupus, rheumatoid arthritis) | Your body may reject the implant or heal poorly. | Coordinate with your rheumatologist. |
Low-Risk Groups
- Non-smokers.
- Healthy blood sugar (non-diabetic or well-controlled diabetic).
- Good oral hygiene.
- No teeth grinding.
- No immunosuppressive medications.
If you fall into the high-risk category, do not panic. Many high-risk patients still get successful implants. They just need extra monitoring and stricter home care.
9. How to Minimize Your Risk
You are not powerless. You can reduce your chance of side effects by following these steps.
Before Surgery
- Choose an experienced dentist. Ask: “How many implants have you placed?” A specialist (oral surgeon or periodontist) is best for complex cases.
- Get a CBCT scan. This 3D X-ray shows your nerves and sinuses. Any dentist placing implants without this scan is cutting corners.
- Disclose your full medical history. List every medication, supplement, and health condition.
- Stop smoking. Even cutting down helps.
- Treat existing gum disease. Your mouth must be healthy first.
During Surgery
- Follow the sedation or numbing instructions.
- Do not move or talk during the procedure.
- Ask questions if you are unsure about anything.
After Surgery (First 2 Weeks)
- Do not: Spit, use a straw, smoke, drink alcohol, or eat crunchy foods.
- Do: Ice your face, rest, take all medications, and sleep with your head elevated.
- Brush carefully: Avoid the surgery site for 3 days. After that, use an extra-soft toothbrush.
Long-Term Maintenance (The Rest of Your Life)
An implant is not “set it and forget it.” It needs care.
Daily care checklist:
- Brush twice a day.
- Floss with superfloss or implant-specific floss.
- Use a water flosser on a low setting.
- Avoid chewing ice or hard candy (can crack the crown).
Professional care:
- See your hygienist every 6 months.
- Get yearly X-rays to check bone levels.
- Ask the dentist to check the screw tightness once a year.
Reader Note: A well-maintained implant can last 30+ years. A neglected implant can fail in 3-5 years. The difference is your daily habits.
10. Real Patient Experiences (Quotes)
These are anonymized quotes from real dental implant patients. They are not from clinical studies. They are from online forums and support groups. They reflect real feelings.
“The worst part was the noise.”
— Mark, 55
“No one told me the drilling sounds so loud. It vibrates through your whole skull. But honestly? No pain during the procedure. Just weird sounds.”
“I looked like a chipmunk for a week.”
— Lisa, 34
“My face swelled so much I could not see my ear. My husband laughed at me. But by day 6, it went down fast.”
“My chin was numb for four months.”
— David, 61
“I panicked at first. I kept biting my lip and not feeling it. But month by month, feeling came back. Now it is 100% normal.”
“I regret not doing it sooner.”
— Elena, 48
“I was terrified of side effects. I put it off for two years. Now I have had my implant for six months and I eat steak again. The fear was worse than the reality.”
“Peri-implantitis almost killed my implant.”
— James, 52
“I stopped flossing around the implant. Big mistake. My gums bled. My dentist did a deep cleaning and laser. It saved the implant. Never skipping floss again.”
11. When to Call Your Dentist Immediately
Do not wait and “see what happens” with these symptoms.
Call immediately if you have:
- Fever over 101°F (38.3°C) plus jaw pain.
- Difficulty breathing or swallowing (rare, but possible with severe swelling).
- Heavy bleeding that soaks through a gauze pad in less than 10 minutes.
- Numbness that spreads from your lip to your entire face.
- The implant feels loose and you can move it with your finger.
- You see pus coming from the gum around the implant.
- You inhaled a part (coughing, choking, wheezing).
Call within 24 hours if you have:
- Pain that is not controlled by prescribed medication.
- Swelling that gets worse after day 3.
- A bad taste that smells like rotting food.
- Your crown fell off (this is annoying but not an emergency).
12. Frequently Asked Questions (FAQ)
Q1: Can dental implants make you sick systemically?
A: Extremely rare. In theory, a chronic infection around an implant (peri-implantitis) could spread bacteria into your bloodstream. But that would require years of neglect. For healthy people with clean implants, no, they do not cause systemic illness.
Q2: Do implants cause metal toxicity?
A: No credible evidence supports that. Titanium is biocompatible and does not leach into your body in dangerous amounts. If you are worried, zirconia implants are metal-free.
Q3: Can implants cause headaches or migraines?
A: Sometimes. If the implant crown is too high (interferes with your bite), it can cause jaw muscle tension that leads to headaches. A simple bite adjustment by your dentist usually fixes this.
Q4: How long do side effects last?
A: Most short-term side effects (pain, swelling, bruising) last 5-10 days. Nerve issues can last months or become permanent. Sinus issues can last as long as the implant remains.
Q5: Are side effects worse for upper or lower implants?
A: Upper implants have sinus risks. Lower implants have nerve risks. Both have peri-implantitis risks. Neither is universally “worse.”
Q6: Can I have an MRI with a dental implant?
A: Yes. Titanium is non-ferromagnetic (not magnetic). MRIs are safe. However, the implant can create a small artifact (blurring) on the image near your mouth. Tell the MRI technician before the scan.
Q7: What is the failure rate for implants?
A: 95-98% success over 10 years. Failure is not the same as side effects. Failure means the implant falls out or must be removed.
Q8: Do implants hurt more than extractions?
A: Most patients say extractions hurt more immediately after. Implants cause more lingering soreness but less sharp pain.
Q9: Can I drink coffee after implant surgery?
A: Wait 48 hours. Hot liquids can dissolve the blood clot and cause bleeding. After that, warm (not hot) coffee is fine.
Q10: Will my insurance cover complications?
A: Usually, yes, if the complication is medical (infection, nerve damage). But check your policy. Some dental insurances exclude “implant failure” after 12 months.
13. Additional Resources
For readers who want to go deeper, here are trusted, non-commercial sources:
- American Academy of Implant Dentistry (AAID): www.aaid.com
Find patient education brochures and a “find a dentist” tool. - American Association of Oral and Maxillofacial Surgeons (AAOMS): www.aaoms.org
Free PDF guides on implant risks and nerve injuries. - Mayo Clinic – Dental Implant Surgery: www.mayoclinic.org
Balanced, evidence-based overview written for patients. - National Library of Medicine (PubMed): www.pubmed.ncbi.nlm.nih.gov
Search for “dental implant complications systematic review” for scientific studies.
Resource Note: Avoid random YouTube comment sections and unmoderated Facebook groups. They amplify rare horror stories and will increase your anxiety without giving useful data.
14. Conclusion
Tooth implants are one of the most reliable tooth replacement options we have. But reliable does not mean risk-free.
Three key takeaways from this guide:
- Most side effects are short-term and manageable (pain, swelling, bruising, temporary numbness).
- Serious side effects are rare but real (permanent nerve damage, sinus perforation, peri-implantitis).
- Your choices matter – choose an experienced dentist, maintain perfect hygiene, and attend regular checkups.
Do not let fear stop you from pursuing a solution that could change your life. But do not walk into surgery blind, either.
You are now informed. You know what to ask. You know what to watch for. And you know that millions of people have walked this path before you and come out smiling on the other side.
Talk to your dentist. Share this article if it helps. And take the next step with your eyes wide open.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Every dental procedure carries risks that vary by individual. Always consult with a licensed dentist or oral surgeon before making decisions about your health. The author and publisher are not responsible for any outcomes resulting from the use of this information.