Can A Dental Implant Become Infected
You’ve invested time, money, and hope into your dental implant. It feels like a natural part of your mouth. But one morning, you notice a strange taste or a little swelling near the gum line. A quiet worry appears in your mind: can a dental implant become infected?
The short answer is yes. But here is the truth most websites won’t tell you upfront: the implant itself—the titanium screw—cannot get a cavity or decay. However, the living gum tissue and bone surrounding it absolutely can become infected. And if left untreated, that infection can lead to bone loss and even implant failure.
This guide is written for real people with real questions. You will learn exactly what causes implant infections, how to spot them early, what your dentist will do about them, and—most importantly—how to prevent them. No exaggerated claims. No fake shortcuts. Just honest, practical knowledge.
What Exactly Is a Dental Implant Infection? (And What It Is Not)
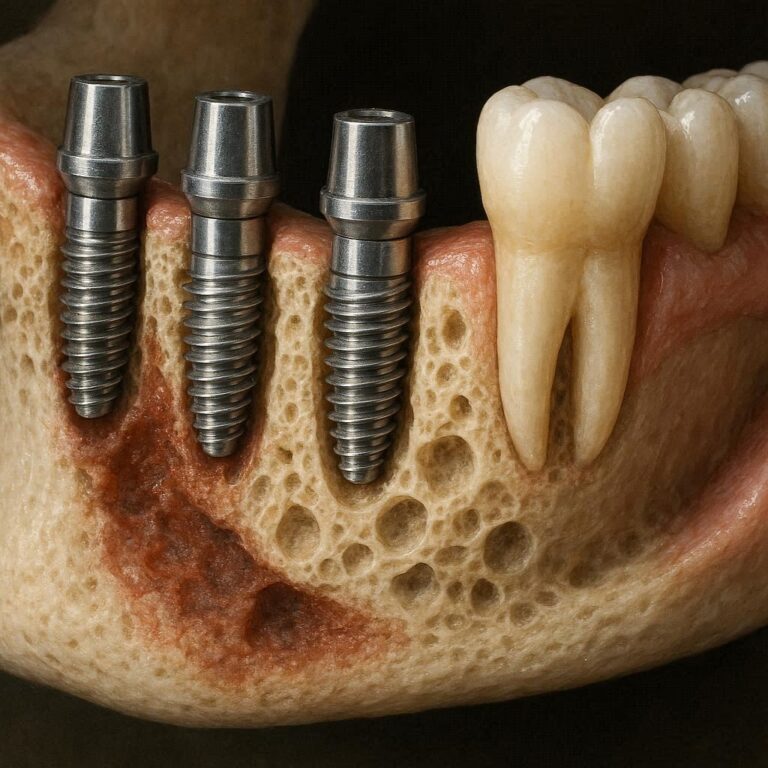
To understand infection, you first need to understand what a dental implant actually is. A complete implant usually has three parts:
- The implant post (titanium screw) placed into your jawbone.
- The abutment (connector piece) sitting on top of the post.
- The dental crown (the visible artificial tooth).
When people ask “can a dental implant become infected,” they usually mean the surrounding tissues. The correct medical term for implant infection is peri-implantitis.
Important Note: Peri-implantitis is not the same as a failed implant. An implant can fail due to poor bone healing, nerve damage, or allergic reactions without any infection present. Infection is one specific cause of failure, but it is not the only one.
Peri-Implant Mucositis vs. Peri-Implantitis
There are two levels of implant infection. Think of them as a warning light versus a full engine breakdown.
| Condition | What Happens | Reversible? |
|---|---|---|
| Peri-implant mucositis | Inflammation and infection limited to the gum tissue only. The gum bleeds when touched. No bone loss. | Yes, with professional cleaning and better home care. |
| Peri-implantitis | Infection has spread deeper into the bone supporting the implant. Bone begins to dissolve. | Partially. Bone loss cannot be reversed, but progression can be stopped. |
Key takeaway: The earlier you catch an implant infection, the better your chances of saving the implant with simple treatment.
How Does a Dental Implant Get Infected in the First Place?
Your mouth is full of bacteria—hundreds of species, both friendly and harmful. A healthy implant depends on a tight seal between the gum and the metal post. When that seal breaks down, bacteria march straight down to the bone.
Here are the real, common ways this happens.
1. Poor Oral Hygiene
This is the number one cause. Just like natural teeth, implants need daily cleaning. But implants don’t have the same ligament attachments as natural teeth. Bacteria can slide deeper, faster. If you skip brushing or flossing around the implant, plaque hardens into tartar, and the gums begin to swell and bleed.
2. Smoking or Tobacco Use
Tobacco is brutal on implants. It reduces blood flow to the gums, masks early signs of infection (smokers often bleed less, which sounds good but is actually bad), and slows healing. Smokers have significantly higher rates of peri-implantitis than non-smokers.
3. History of Periodontal Disease
If you lost your natural tooth because of gum disease, you are at higher risk for implant infection. The same bacteria that destroyed your natural tooth’s support system will happily attack your implant. This is why treating active gum disease before getting an implant is crucial.
4. Poor Implant Placement or Crown Fit
Not all implants are created equal. If the crown is too bulky, it traps food and plaque. If the implant is placed too close to another tooth, cleaning becomes impossible. If the abutment connection has microscopic gaps, bacteria colonize inside the implant itself. A skilled surgeon and restorative dentist make a massive difference.
5. Leftover Cement
Some implants are “cemented” rather than screwed. If excess cement gets pushed below the gum line, it acts like a sticky trap for bacteria. The gum stays inflamed, and infection follows. This is called cement-induced peri-implantitis.
6. Uncontrolled Medical Conditions
Diabetes (especially with high HbA1c levels), autoimmune diseases, and conditions requiring long-term steroid use all increase infection risk. These conditions impair your body’s ability to fight bacteria and heal tissue.
7. Bruxism (Teeth Grinding)
Grinding doesn’t directly cause infection, but it overloads the implant. Microscopic fractures in the bone or loosening of the abutment screws create spaces where bacteria can hide. Grinders often need night guards to protect their implants.
Early Warning Signs: How to Know if Your Implant Is Infected
Your body is excellent at sending signals. Learn to listen to them. Do not wait for pain—most implant infections start without pain.
The First Symptoms (Peri-Implant Mucositis)
- Bleeding when you brush or floss around the implant.
- Red, puffy, or shiny gum tissue next to the implant.
- Mild bad breath or a bad taste that doesn’t go away.
- No pain yet. The gum may feel slightly tender to pressure.
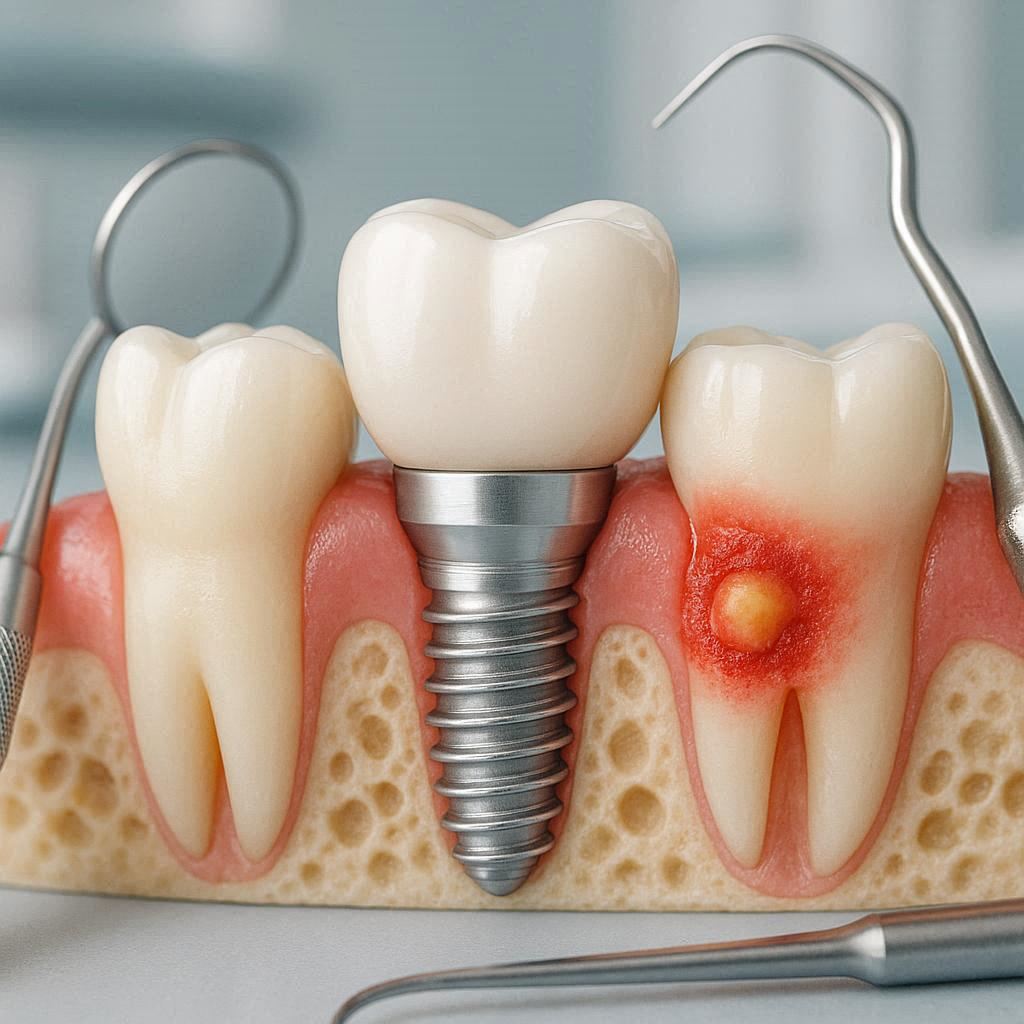
The Advanced Symptoms (Peri-Implantitis)
- Bleeding that worsens or happens spontaneously.
- Pus oozing from the gum line when you press near the implant.
- The gum pulls away, revealing the metal threads of the implant.
- The implant feels loose or clicks when you push it.
- Pain when chewing (this is late-stage).
- Visible metal where gum used to cover.
Important Note: An infected implant rarely causes fever or swollen lymph nodes unless the infection has spread to the jawbone space (a serious emergency). Most peri-implantitis stays localized—but that does not mean it is harmless.
A Quick Self-Check You Can Do at Home
- Look at your implant gum in a mirror. Is it pink or red?
- Gently touch the gum next to the implant with a clean finger. Does it bleed?
- Smell your floss after using it around the implant. Any odor?
- Does the implant feel different when you tap it with a spoon compared to a natural tooth?
If you answer “yes” to any of these, schedule a dental exam within the next week. Do not wait months.
What Happens If You Ignore an Infected Implant?
Ignoring peri-implantitis is like ignoring a small crack in a dam. At first, nothing dramatic happens. Then the damage becomes irreversible.
Stage 1: Bone Loss Begins
Once the infection reaches the bone, your body’s immune response starts breaking down bone tissue. The implant loses support. You cannot feel this happening. Only an X-ray can show it.
Stage 2: Bone Loss Accelerates
As more bone disappears, the implant becomes wobbly. Food packs around it. Cleaning becomes painful. The infection may spread to neighboring natural teeth, putting them at risk.
Stage 3: Implant Failure
The implant loses so much bone that it cannot stay firmly in place. At this point, the implant must be removed. After removal, you may need bone grafting before a new implant can even be considered.
Realistic outcome: Many infected implants can be saved if treated early (first 6–12 months of bone loss). Once 50% or more of the supporting bone is gone, the prognosis becomes guarded.
Professional Diagnosis: How Your Dentist Confirms an Implant Infection
You might suspect an infection. Your dentist will confirm it with three main tools. None of them hurt.
1. Probing Depths
Your dentist uses a tiny ruler (periodontal probe) to measure the pocket depth between your gum and the implant. Healthy pockets are 3mm or less. Infected pockets measure 5mm, 7mm, or even 10mm. Bleeding during probing is a major red flag.
2. X-Rays (Especially Periapical or CBCT)
Standard X-rays show bone levels around the implant. The dentist compares current X-rays to the ones taken right after placement. Any bone loss beyond the normal first-year remodeling (about 1–1.5mm is normal) suggests peri-implantitis. CBCT (3D X-ray) can show bone loss around the entire implant circumference.
3. Microbial Testing (Less Common but Useful)
In stubborn or recurrent infections, the dentist may swab the pocket and send it to a lab. This identifies which bacteria are dominant (e.g., P. gingivalis, T. forsythia). The results help choose the most effective antibiotic if needed.
What About Home Tests?
Avoid at-home “dental implant infection test kits” sold online. Most are unregulated and inaccurate. Your dentist’s clinical exam and X-rays are the gold standard.
Professional Treatment Options (From Simple to Complex)
Good news: many implant infections can be treated without removing the implant. Bad news: the treatment is more expensive and complex than treating a natural tooth infection. Here is what to expect.
Non-Surgical Treatment (For Peri-Implant Mucositis and Mild Peri-Implantitis)
This works when there is little to no bone loss yet.
Procedure name: Implant surface debridement
What happens:
- Your dentist numbs the area (usually not painful, but some patients prefer anesthesia for deep cleaning).
- Special plastic or titanium curettes scrape plaque and tartar from the implant surface. Metal scalers can scratch titanium; scratching creates more hiding places for bacteria.
- An ultrasonic scaler with a plastic tip flushes the pocket with water or antimicrobial solution.
- The dentist may place a local antibiotic gel (like minocycline microspheres) into the pocket.
What you feel: Pressure, scraping sounds, but minimal pain. Mild soreness for 1–2 days afterward.
Success rate: 70–90% for peri-implant mucositis if you improve your home care. Lower for established peri-implantitis.
Surgical Treatment (For Moderate to Advanced Peri-Implantitis)
If bone loss is significant, surgery becomes necessary.
Procedure name: Open flap debridement with or without bone grafting
What happens:
- The dentist (or periodontist) numbs you completely.
- A small incision is made in the gum. The gum is lifted back like a flap to expose the implant threads and lost bone.
- All infected tissue, granulation tissue, and surface bacteria are mechanically cleaned off the implant.
- The implant surface may be decontaminated using chlorhexidine, hydrogen peroxide, or a laser.
- If the bone defect has a certain shape, bone graft material (often synthetic or bovine-derived) is packed into the defect.
- The gum is sutured closed.
- You return in 10–14 days for suture removal.
What you feel: More discomfort than non-surgical treatment. Swelling and mild pain for 3–5 days. Soft food diet for 2 weeks.
Success rate: 60–85% depending on the bone defect shape and your compliance with aftercare.
What If the Implant Is Too Infected to Save?
Sometimes, despite everyone’s best efforts, the implant must come out.
Procedure name: Explantation (implant removal)
What happens:
- The dentist loosens the abutment screw and removes the crown.
- A special drill or reverse-torque instrument unscrews the implant.
- If the implant is well-integrated but infected, removal requires a trephine drill (like a cookie cutter around the implant).
- The socket is thoroughly debrided of infected tissue.
- Bone graft material is placed to rebuild the site for a future implant.
- You wait 4–12 months for healing.
Emotional reality: Explantation is disappointing, but it is not the end. Many patients successfully get a second implant after proper bone healing. Some choose a dental bridge or partial denture instead.
Are Antibiotics Enough Alone?
No. Antibiotics alone cannot cure peri-implantitis. The bacteria form a sticky biofilm on the implant surface that oral or even IV antibiotics cannot penetrate sufficiently. Antibiotics are always used alongside mechanical cleaning, not instead of it.
Home Care: Your Daily Defense Against Implant Infection
You are the first and most important line of defense. Your dentist cleans your implant once or twice a year. You clean it 365 days a year. Here is exactly how to do it right.
The Essential Tools (No Expensive Gadgets Required)
| Tool | Why It Works | How Often |
|---|---|---|
| Soft or extra-soft toothbrush | Gentle on gums, effective on plaque | Twice daily |
| Interdental brush (rubber-tipped or small bristle) | Cleans the concave areas around the implant post where floss misses | Once daily (evening) |
| Implant-specific floss or super floss | Has a stiff end to thread under the crown and a fluffy section to clean tightly | Once daily |
| Water flosser (optional but helpful) | Flushes debris from deep pockets if used at low pressure | As needed or once daily |
| Non-abrasive toothpaste | Avoid whitening toothpaste or baking soda; they scratch the crown and implant surface | Twice daily |
Step-by-Step Cleaning Routine (Takes 3 Minutes)
- Brush normally for 2 minutes, paying extra attention to the gum line around the implant crown. Use a “tilted” angle toward the gum.
- Use the interdental brush (choose a size that fits snugly but not forcibly). Insert it gently between the crown and the adjacent tooth. Move back and forth 3–5 times.
- Use implant floss (not regular waxed floss—it shreds). Thread the stiff end under the crown’s contact point. Wrap the fluffy part around the implant neck in a C-shape. Slide up and down below the gum line until the gum feels snug but not painful.
- Rinse with water or a non-alcohol mouthwash (alcohol dries tissue and may worsen inflammation).
What to Avoid
- Toothpicks or metal picks: They can scratch the implant surface or wedge into the gum too aggressively.
- Whitening strips: Chemicals can irritate the gum margin around an implant.
- Aggressive sawing motions with floss: This cuts the gum seal. Use gentle vertical motions.
Reader Note: If your hands have limited mobility (arthritis, etc.), ask your dentist about a “single-tufted brush” or a “water flosser with a perio tip.” Both are easier to use and very effective.
Professional Maintenance Schedule: How Often Should You See a Dentist?
Once your implant is restored, you enter a lifelong maintenance phase. Think of it like a car’s oil change—skip it, and the engine fails.
Recommended Schedule
| Time After Implant Placement | Recommended Visit |
|---|---|
| 2 weeks after crown placement | Check fit, bite, and gum health. |
| 3 months later | First maintenance cleaning. Probing depths recorded as baseline. X-ray taken. |
| Every 3–6 months | Regular implant maintenance (NOT the same as a standard cleaning). |
| Annually | Bitewing or periapical X-ray to check bone levels. |
Why Regular Implant Maintenance Is Different From a Regular Cleaning
A standard “prophylaxis” (regular cleaning) uses metal scalers that can scratch implants. An implant maintenance visit uses:
- Plastic or resin scalers.
- Rubber cup polishing with low-abrasive paste.
- Gentle flossing with implant-specific floss.
- Probing without aggressive force.
Do not let a hygienist use metal instruments on your implant. Politely ask, “Do you have plastic scalers for my implant?” A knowledgeable office will say yes.
Can You Get an Implant Infection Years After Placement?
Yes. And this surprises many people.
Peri-implantitis can appear 1 year, 5 years, or even 15 years after your implant was placed. It is not a “short-term complication.” It is a lifelong risk.
Reasons for late-onset infection:
- Changes in your health (new diabetes diagnosis, chemotherapy, etc.)
- New medications that cause dry mouth (less saliva means more bacteria)
- Poor home care creeping in over time
- A crown that becomes loose and traps food
- Gum recession exposing rough implant threads that collect plaque
Take-home point: The day your implant is placed is not the finish line—it is the starting line for a lifetime of maintenance.
Risk Factors You Can Control vs. Those You Can’t
To help you focus your energy, here is a realistic breakdown.
Risk Factors You Can Change (Modifiable)
| Risk Factor | What You Can Do |
|---|---|
| Poor oral hygiene | Follow the home care routine above. Set phone reminders. |
| Smoking | Quit or reduce. Even cutting down helps. Vaping is not a safe alternative for implant health. |
| Uncontrolled diabetes | Work with your doctor to lower HbA1c below 7–8% before implant placement. |
| Infrequent dental visits | Schedule your next maintenance visit before leaving the office. |
| Grinding | Get a custom night guard. Over-the-counter guards usually fit poorly around implants. |
Risk Factors You Cannot Change (Non-Modifiable)
- Genetics (some people have an aggressive inflammatory response to bacteria)
- Previous history of severe periodontitis
- Certain autoimmune conditions (Sjogren’s syndrome, lupus)
- Taking bisphosphonate medications (for osteoporosis or cancer)—these require special implant protocols
- Age (older adults heal more slowly, but successful implants are placed daily in people over 80)
Honest advice: If you have multiple non-modifiable risk factors, talk frankly with your implant dentist about a “maintenance-focused” approach—meaning more frequent checkups (every 3 months) and a lower threshold for early treatment.
Special Situations: Questions Real Patients Ask
“I have an implant and a bridge next to it. Is infection risk higher?”
Yes, but manageable. The bridge creates a “dead zone” where floss cannot pass. You will likely need a threader floss or a water flosser to clean underneath the bridge pontic. Also, the connection between the implant crown and the bridge is a trap for food. See your dentist every 4 months instead of 6.
“My implant crown is cemented. How do we know if cement is causing the infection?”
This is tricky. The dentist may need to remove the crown (cutting it off if cemented permanently) to check for residual cement. A cone beam CT scan can sometimes show excess cement as a radiopaque blob. If you have persistent bleeding and probing depths despite good cleaning, cement-induced peri-implantitis is on the list of suspects.
“I’m pregnant with an implant. Should I worry?”
Pregnancy hormones increase gum inflammation (pregnancy gingivitis). Your implant gum is not immune. Continue excellent home care and see your dentist for a thorough cleaning in the second trimester. Do not postpone necessary periodontal treatment—untreated gum inflammation is linked to preterm birth.
“I felt a crack in my implant crown. Can that cause infection?”
Yes. A cracked crown allows bacteria to leak down to the abutment connection. Over time, that bacterial leakage reaches the implant threads. Have any cracked or chipped crown replaced promptly—do not wait for pain.
Five Myths About Infected Implants (Debunked)
Let’s clear up the misinformation circulating online.
Myth 1: “Titanium implants cannot get infected because metal is not alive.”
Truth: The metal stays sterile. The living gum and bone around it get infected. You treat the tissue, not the metal.
Myth 2: “If my implant gets infected, it has to come out immediately.”
Truth: Most early-stage infections respond to deep cleaning and antibiotics. Removal is a last resort, not a first response.
Myth 3: “Hydrogen peroxide kills implant infection at home.”
Truth: Full-strength peroxide damages gum tissue and can discolor the crown. Diluted peroxide (1:10 with water) may help short-term, but it does not remove the bacterial biofilm. It is not a cure.
Myth 4: “Implants don’t need flossing.”
Truth: This is dangerous advice. Flossing is essential. Without floss, bacteria build up in the gingival crevice and trigger inflammation.
Myth 5: “Once an implant fails from infection, you can never get another one.”
Truth: After explantation and bone grafting, many patients receive a successful second implant. The success rate is lower (around 75–85% versus 95% for first implants), but it is very possible.
Cost Realities: Treating an Infected Implant
Let’s talk money honestly. Dental implant infection treatment is not cheap. But it is almost always cheaper than losing the implant and replacing it.
| Treatment | Approximate Cost (USD) | Notes |
|---|---|---|
| Implant maintenance cleaning | 100–250 | Covered by many insurances once or twice yearly |
| Non-surgical debridement (no anesthesia) | 200–400 | Often not covered separately; may be part of periodontal therapy |
| Non-surgical debridement with local antibiotics | 400–800 | Antibiotic gel adds cost |
| Open flap debridement (one implant) | 1,200–2,500 | Surgical fee + possible bone graft |
| Bone graft during surgery | 500–1,500 per site | Material cost + placement |
| Explantation (implant removal) | 300–800 | Relatively simple if implant is not fused tightly |
| New implant after bone graft | 3,000–6,000 total | Crown + abutment + implant |
Insurance note: Most dental insurances do NOT cover peri-implantitis treatment because implants are often considered a “major service” with limited annual maximums. Medical insurance rarely covers it unless the infection spreads to the jawbone (osteomyelitis). Be prepared to pay out of pocket.
Worth it? Yes. Losing an implant is more expensive (replacement + grafting) and emotionally draining. Treat early.
Prevention Is Cheaper Than Treatment: A Simple Checklist
Use this checklist monthly to stay ahead of trouble.
Once a month, ask yourself:
- Do I see any redness or swelling around my implant gum?
- Does my floss smell bad after using it around the implant?
- Does the implant area bleed when I brush gently?
- Have I noticed a new gap between my implant crown and the gum?
- Has my bite changed? (Does food hit the implant first?)
Twice a year (or as recommended):
- Schedule implant maintenance with your dentist.
- Bring your current toothbrush and floss to show your hygienist—they will spot mistakes.
- Request a copy of your X-ray so you can compare bone levels over time.
When traveling:
- Pack interdental brushes in your toiletry bag.
- Use bottled water with a water flosser if tap water is questionable.
- Do not skip flossing even for one night.
When to Seek Emergency Care
Most implant infections are not emergencies. But a few situations require immediate attention.
Go to an emergency dentist or hospital if:
- Your face is visibly swollen near the implant, and the swelling is spreading to your eye or neck.
- You have difficulty swallowing or breathing.
- You have a fever over 101°F (38.3°C) along with implant pain.
- The implant is so loose that it moves when you talk or swallow.
These signs suggest the infection has spread beyond the local bone into deeper facial spaces. This is rare with implants but possible in severely immunocompromised patients.
For all other symptoms: Call your dentist within 24–48 hours. You do not need the emergency room for bleeding gums or mild tenderness.
Living Well With a Dental Implant: Long-Term Outlook
Despite everything you have just read, stay hopeful. Dental implants remain one of the most successful medical devices ever invented. Their 10-year survival rate is around 95% for lower jaws and 90-95% for upper jaws. Most of the failures occur in the first year due to poor bone integration, not infection.
For the vast majority of people, infection can be prevented with good daily habits and regular professional care. If infection does occur, modern treatments save most implants. Only a small percentage need removal.
The formula for long-term success:
Good home care + Regular implant maintenance + Non-smoking + Controlled medical conditions + Early treatment if signs appear
Follow these five pillars, and your implant has every chance of lasting decades—even a lifetime.
Conclusion
A dental implant can become infected, but the infection is in the surrounding gum and bone (peri-implantitis), not the titanium post itself. Early signs like bleeding and redness should never be ignored. With excellent daily cleaning, regular professional maintenance, and prompt treatment at the first warning signs, most infected implants can be saved. Prevention remains the most effective and affordable strategy.
Frequently Asked Questions (FAQ)
1. Can a dental implant infection spread to my natural teeth?
Yes. The same bacteria that infect an implant can travel to adjacent natural teeth, causing gum disease and even bone loss around those teeth.
2. How quickly does peri-implantitis progress?
It varies. Some people lose 1–2mm of bone per year. Others hold stable for years. Smoking, poor cleaning, and diabetes speed progression.
3. Can I use mouthwash on my implant?
Yes, but choose non-alcohol mouthwash. Alcohol dries tissues and may worsen inflammation. Chlorhexidine (prescription) is excellent for short-term use (2 weeks) but stains teeth with long-term use.
4. Will my implant always feel different from natural teeth?
Yes. Natural teeth have a ligament that absorbs shock. Implants are rigid. That difference does not mean infection—it is normal.
5. Can a dentist tell if my implant is infected just by looking?
Often, but not always. Early infection may have no visible redness. Probing depths and X-rays are needed for a definitive diagnosis.
6. Is it safe to whiten my natural teeth with an implant?
Whitening gel will not harm the implant metal, but it can irritate the gum around the implant. Use custom trays that avoid the implant area.
7. Can I get an MRI with a dental implant?
Yes. Titanium is non-ferromagnetic. However, the implant crown (ceramic or metal) may create an artifact (blurring) on the MRI image. Always tell the MRI technician about your implant.
8. How do I clean under a fixed implant bridge?
Use super floss (stiff end threader plus fluffy section) or a water flosser with a perio tip. An interdental brush can fit under some bridges.
9. What is the most common bacteria found in infected implants?
Porphyromonas gingivalis, Treponema denticola, and Tannerella forsythia—the same bacteria found in severe natural gum disease.
10. Can COVID-19 affect implant healing or infection risk?
Early research suggests that severe COVID-19 may alter immune response and blood flow, potentially increasing peri-implantitis risk. If you had severe COVID, inform your dentist before implant placement or during maintenance.
Additional Resource
For a deeper, research-backed understanding of peri-implantitis, visit the American Academy of Periodontology’s patient page on implant maintenance:
👉 https://www.perio.org/for-patients/periodontal-treatments-and-procedures/dental-implants-and-peri-implantitis/
This resource provides clinical guidelines, illustrations, and a “find a periodontist” tool for complex cases.
Disclaimer
This article is for informational purposes only and does not constitute medical or dental advice. Every person’s oral health situation is unique. Do not use this information to diagnose or treat your own implant infection. Always consult a licensed dentist or periodontist for a proper examination, diagnosis, and treatment plan. The author and publisher are not liable for any outcomes resulting from the use of this information.