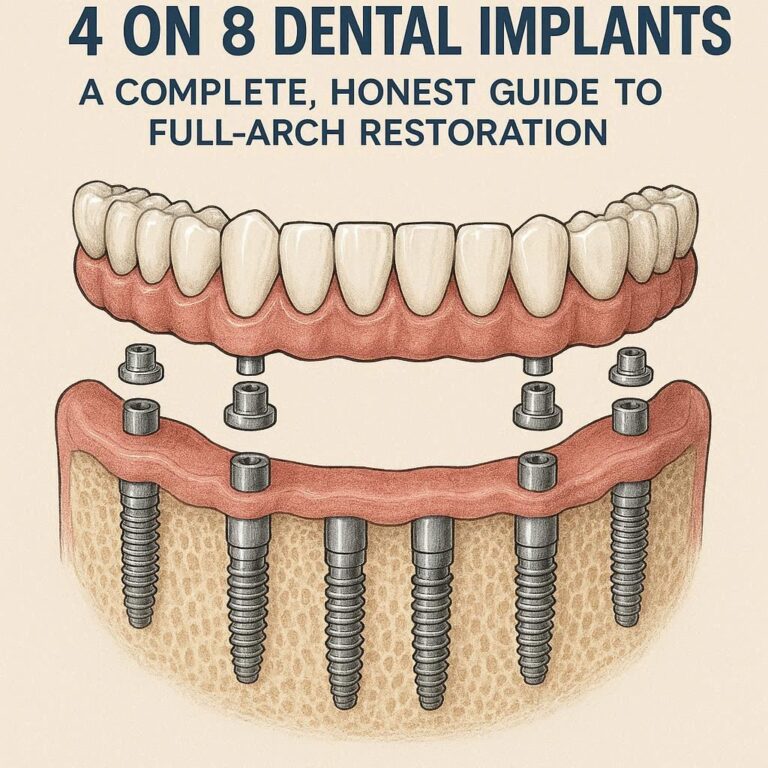
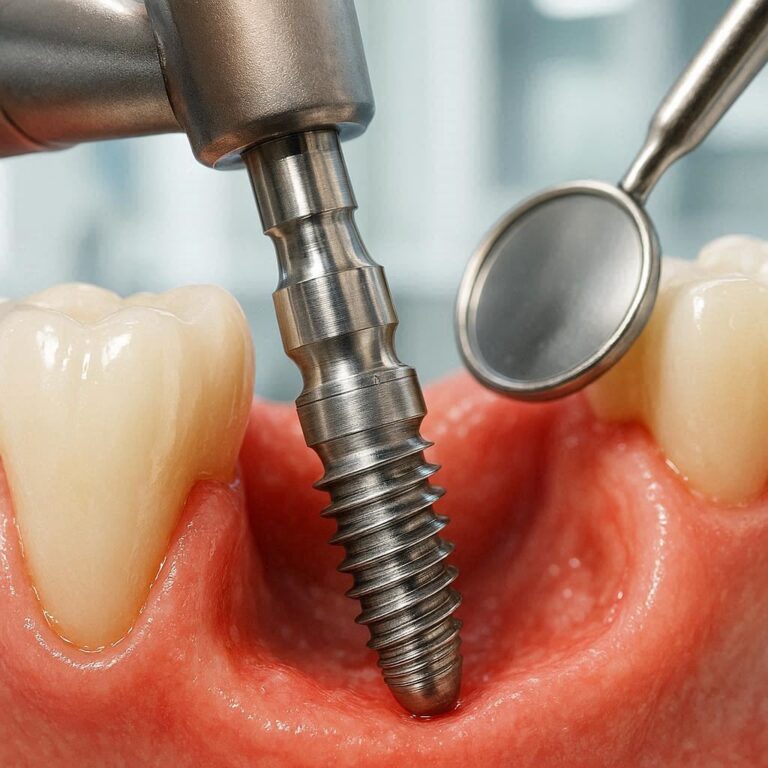
What Happens During the First Surgery for an Osseointegrated Implant?
If you are exploring options for limb replacement, you have likely heard the term “osseointegration.” It sounds complex. But the idea is actually quite simple and powerful.
Instead of a traditional socket that fits over your residual limb, an osseointegrated implant creates a direct connection between your bone and an external prosthetic. The first surgery is a major step in that journey.
You probably have questions. What does the procedure actually feel like? How long does it take? Is it painful?
Let us walk through everything. No confusing medical jargon. Just clear, honest, and helpful information.
Important note: This guide is for educational purposes. Always consult your surgical team for advice specific to your body and situation.
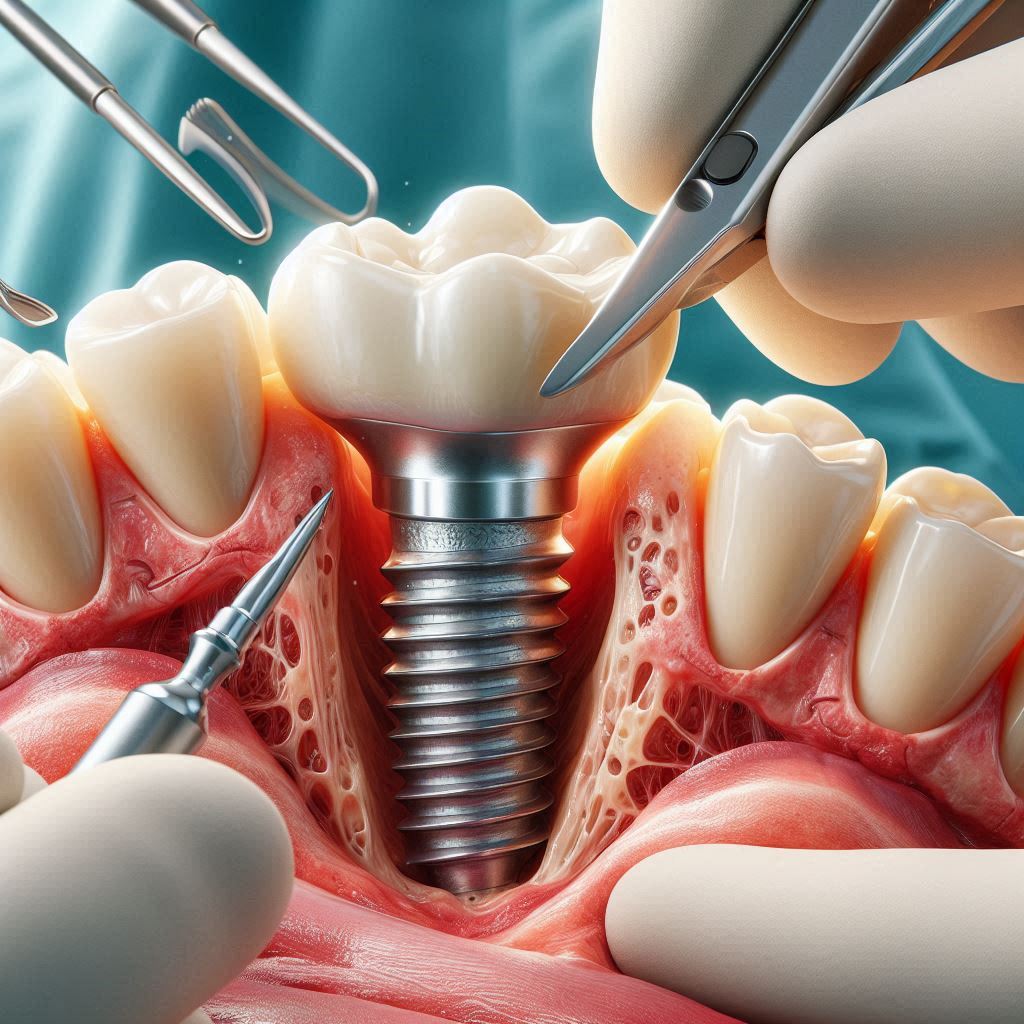
Understanding the Goal of the First Surgery
Before we dive into the operating room, let us talk about why this first surgery matters so much.
The first surgery for an osseointegrated implant has one main job: to place a metal fixture securely inside your bone. Think of it like laying a strong foundation for a house. Without a solid foundation, nothing else works.
- The fixture is usually made of titanium. This metal is special because bone cells naturally grow right onto its surface. That process is called osseointegration.
- The goal is to achieve a stable, long-lasting connection between the implant and your bone.
- The outcome will allow a connector (abutment) to later pass through your skin and attach to your external prosthetic leg or arm.
The first surgery does not give you a finished, wearable prosthetic. Instead, it prepares your body for the next phase. Patience is key here.
Who Is a Good Candidate for This First Surgery?
Not everyone is an ideal candidate right away. Surgical teams follow strict guidelines to keep you safe.
Good candidates typically have:
| Criterion | Why It Matters |
|---|---|
| Adequate bone quality | The bone must hold the implant firmly. |
| Good soft tissue coverage | Healthy skin and muscle over the bone reduce infection risk. |
| No active infections | Any bone or skin infection must be treated first. |
| Realistic expectations | You understand that healing takes months, not weeks. |
| Non-smoker (or willing to quit) | Smoking dramatically slows bone healing. |
If you do not meet all of these today, do not lose hope. Many people improve their candidacy with physical therapy, nutrition changes, or quitting smoking.
Reader note: Some centers now offer two-stage procedures for people with complex bone or skin issues. Ask your surgeon about their specific protocol.
Before the First Surgery: What You Need to Do
Preparation starts weeks before you ever see the operating room. Your surgical team will give you a checklist. Here is what is commonly included.
Pre-Surgical Testing
You will likely undergo several tests to ensure your body is ready.
- Bone density scan (DXA) – Checks how strong your bone is.
- CT scan or MRI – Provides 3D images of your bone shape.
- Blood work – Looks for signs of infection or nutritional deficiencies.
- ECG and chest X-ray – Ensures your heart and lungs tolerate anesthesia.
Lifestyle Adjustments
Small changes now make a big difference later.
- Stop smoking – At least four weeks before surgery. Some surgeons require eight weeks.
- Improve nutrition – Increase protein, vitamin D, and calcium intake.
- Optimize skin health – Treat any rashes, sores, or dry skin on your residual limb.
Planning Your Recovery
You will not be able to do everything alone after surgery. Set up support in advance.
- Arrange for someone to drive you home from the hospital.
- Prepare your living space for limited mobility.
- Stock up on easy-to-prepare meals and snacks.
The Day of the First Surgery: A Step-by-Step Walkthrough
Let us walk through the actual day. Knowing what happens next can ease a lot of anxiety.
Arrival and Check-In
You will arrive at the hospital several hours before your scheduled procedure. A nurse will:
- Confirm your identity and the surgical site.
- Start an IV line for fluids and medications.
- Ask you to change into a hospital gown.
- Review your consent forms one last time.
Meeting Your Surgical Team
Before surgery, you will meet or see several professionals.
- Surgeon – Explains the final plan and answers last-minute questions.
- Anesthesiologist – Discusses your anesthesia options.
- Operating room nurses – Describe what to expect when you wake up.
Anesthesia: What to Expect
Most first surgeries for osseointegrated implants use general anesthesia. That means you will be completely asleep and pain-free.
In some cases, a spinal or regional block is added. This provides pain relief that lasts several hours after you wake up.
Important: Tell your anesthesiologist about all medications, supplements, or allergies. Even over-the-counter drugs matter.
Positioning on the Operating Table
Once you are asleep, the team positions you carefully. For a leg implant, you will lie on your back. For an arm implant, you may lie on your side.
The surgeon will clean your skin with an antiseptic solution. Sterile drapes cover everything except the surgical site.
Step 1: The Skin Incision
The surgery begins with a carefully planned cut through your skin and soft tissues.
- The incision location is marked before surgery, often using a 3D-printed guide.
- The length of the cut depends on your anatomy, but it is typically 4 to 8 centimeters.
- The surgeon works to preserve as many nerves and blood vessels as possible.
Step 2: Exposing the Bone
After moving the muscle and other soft tissues aside, the surgeon reaches your bone. They use special retractors to keep the area open and visible.
At this point, the surgical field looks like a clean, exposed bone surface ready for work.
Step 3: Drilling and Preparing the Bone Site
This step is extremely precise. The surgeon uses a series of drills, each slightly larger than the last.
- The first drill creates a starter hole exactly where the implant will go.
- Each subsequent drill widens and shapes the hole.
- Constant irrigation (sterile saline solution) keeps the bone cool. Heat damages bone cells.
The final hole matches the exact shape of your titanium implant.
Step 4: Inserting the Titanium Fixture
Now comes the critical moment. The surgeon takes the sterile titanium implant and threads or taps it into the prepared hole.
- The implant fits tightly. This initial friction is called “primary stability.”
- A torque wrench measures exactly how tight the fit is.
- If stability is excellent, the first surgery may proceed to the next step. If not, the surgeon may stop here and close you up.
Step 5: Placement of the Abutment (Sometimes)
Different surgical centers use different protocols. There are two main approaches.
| Approach | What Happens During First Surgery |
|---|---|
| One-stage procedure | The surgeon attaches an abutment (a small metal post) to the implant. This post sticks out through your skin right away. |
| Two-stage procedure | The surgeon places only the implant inside the bone. Then they close the skin completely over it. A second surgery, months later, exposes the implant and adds the abutment. |
Both approaches work. The choice depends on your bone quality, infection risk, and your surgeon’s preference.
Step 6: Closing the Incision
If you had a one-stage procedure, the surgeon closes the skin around the abutment. Special sutures hold everything in place.
If you had a two-stage procedure, the surgeon closes the skin completely over the implant. No metal is visible after surgery.
The dressing goes on top. You may have a small drain to prevent fluid buildup.
Step 7: Recovery Room
You wake up in the post-anesthesia care unit (PACU). A nurse watches your vital signs and pain levels closely.
Most people stay in the PACU for one to two hours. Then you move to a regular hospital room.
Right After Surgery: What Feels Normal vs. Concerning
Understanding what to expect helps you tell the difference between normal healing and a potential problem.
Normal Experiences
- Moderate pain – Managed with oral or IV medications.
- Swelling – Peaks around day two or three after surgery.
- Bruising – Often spreads down your limb. This is normal.
- Fatigue – Anesthesia and surgery take energy from your body.
- Numbness – Some skin around the incision may feel numb for weeks or months.
When to Call Your Nurse or Surgeon Immediately
Do not hesitate to speak up. These signs need prompt attention.
- Fever over 101°F (38.3°C)
- Uncontrolled pain that medication does not touch
- Redness spreading quickly away from the incision
- Foul-smelling drainage from the wound
- Shortness of breath or chest pain
- Sudden coldness or color change in your residual limb
Reader note: Trust your instincts. You know your body better than anyone. If something feels wrong, ask for help.
Hospital Stay: What an Average Timeline Looks Like
Every patient recovers differently. But here is a realistic timeline for an uncomplicated first surgery.
Day of Surgery (Day 0)
- Wake up in recovery.
- Start pain medication.
- First small sips of water and ice chips.
- Leg implants: Bed rest with limb elevated.
Day 1 After Surgery
- Progress to a regular diet.
- Physical therapist visits to teach safe movements.
- Learn how to logroll or transfer without stressing the implant.
- Leg implants: No weight-bearing.
Day 2 After Surgery
- Pain typically peaks and then stabilizes.
- Wound checked and dressing changed.
- Begin gentle range-of-motion exercises.
- Plan for discharge if everything looks good.
Day 3 to 5
- Most patients go home or transfer to a rehabilitation facility.
- You receive written instructions for wound care, pain management, and activity restrictions.
- Follow-up appointment scheduled.
Pain Management After the First Surgery
Pain is a real concern. Let us be honest about it. The first week involves some significant discomfort, but it is manageable.
Your team will likely use a combination approach:
| Type | Examples | How It Helps |
|---|---|---|
| Oral opioids | Oxycodone, hydrocodone | Strong pain relief for the first days |
| Non-opioid pain relievers | Acetaminophen, ibuprofen | Reduces inflammation and opioid need |
| Nerve pain medications | Gabapentin, pregabalin | Targets nerve-related pain |
| Regional block | Continuous nerve catheter | Numbness that lasts 12 to 48 hours |
By week two, most people switch to only non-opioid medications. By week four, pain is usually mild and intermittent.
Healing Timeline: From Surgery to Next Steps
Healing after the first surgery for an osseointegrated implant happens in stages. Knowing this timeline helps you stay patient.
Weeks 1 to 2: Protection Phase
- No weight-bearing at all for leg implants.
- Sutures or staples removed around day 10 to 14.
- Keep the dressing clean and dry.
- Expect swelling to decrease noticeably.
Weeks 3 to 6: Early Healing Phase
- Swelling is mostly gone.
- Incision looks pink but closed.
- You may shower normally (check with your surgeon first).
- Gentle stretching continues.
- Leg implants: Still no weight-bearing.
Weeks 7 to 12: Bone Integration Phase
- Your bone begins to grow onto the titanium surface.
- X-rays show early signs of osseointegration.
- Start more active physical therapy.
- Leg implants: Introduction of very partial weight-bearing (10-20% of body weight).
Months 4 to 6: Maturation Phase
- Bone integration gets stronger each week.
- X-rays show dense bone around the implant.
- Increase weight-bearing gradually.
- Begin gait training for leg implants or grip training for arm implants.
Month 6 and Beyond: Ready for Full Use
- Most patients achieve full weight-bearing or full use.
- You are ready for the abutment (if you had a two-stage procedure).
- If you had a one-stage procedure, you might attach a prosthetic very soon.
Important: Some people heal faster. Others take longer. Do not compare your timeline to anyone else’s.
Potential Risks and Complications
Every surgery carries risks. Being informed helps you make good decisions and catch problems early.
Common but Manageable Risks
- Infection – The most talked-about risk. Antibiotics before and after surgery lower this risk dramatically.
- Wound breakdown – Skin may have trouble healing around the abutment. Special wound care usually solves this.
- Pain at the implant site – Usually temporary. Sometimes related to muscles or scar tissue.
Less Common but Serious Risks
- Implant loosening – The bone does not integrate properly. Revision surgery may be needed.
- Peri-prosthetic fracture – The bone breaks near the implant. This is rare with good bone quality.
- Nerve injury – May cause numbness or weakness. Most are temporary.
Your surgical team will discuss how they specifically prevent and manage each of these risks.
Lifestyle Changes During Recovery
Your daily life will look different for a while. That is okay. Think of this as an investment.
What You Cannot Do
- Drive a car for at least two weeks (longer if you take opioids).
- Lift anything heavy with the affected limb.
- Submerge the incision in water (no baths, pools, or hot tubs).
- Smoke or vape anything.
What You Can Do
- Work from home or do desk-based work after week one.
- Read, watch movies, listen to podcasts.
- Practice gentle breathing exercises.
- Eat nutritious meals to support healing.
Adapting Your Home
Small changes make daily life easier.
- Place a chair in the shower.
- Move phone chargers and remote controls within easy reach.
- Clear floor rugs that could cause tripping.
- Set up a temporary sleeping area on the ground floor if stairs are challenging.
Physical Therapy After the First Surgery
Physical therapy is not optional after osseointegration. It is essential.
Your therapist will guide you through three phases.
Phase 1: Protection and Mobility (Weeks 1 to 6)
- Learn safe transfers (bed to chair, chair to toilet).
- Maintain range of motion in nearby joints (hip or shoulder).
- Prevent muscle atrophy with isometric exercises.
- No stress on the implant itself.
Phase 2: Loading Introduction (Weeks 7 to 16)
- Begin partial weight-bearing for leg implants.
- Use a specialized loading device that measures force.
- Learn to interpret your body’s signals of “too much” versus “just right.”
Phase 3: Functional Training (Month 4 onward)
- Increase weight-bearing gradually.
- Practice walking with a walker, then crutches, then a cane.
- For arm implants: Practice gripping, pulling, and pushing tasks.
- Prepare for final prosthetic attachment.
Reader note: Do not skip therapy sessions even if you feel good. Consistent therapy is the single biggest predictor of a successful outcome.
One-Stage vs. Two-Stage Procedure: A Deeper Comparison
Since this decision impacts your experience, let us compare them in more detail.
| Feature | One-Stage Procedure | Two-Stage Procedure |
|---|---|---|
| Number of surgeries | One | Two (separated by 4-6 months) |
| Abutment placement | During first surgery | During second surgery |
| Metal through skin immediately? | Yes | No |
| Infection risk | Slightly higher | Slightly lower |
| Time to prosthetic use | Shorter (around 4-6 months) | Longer (around 8-12 months) |
| Wound care difficulty | Higher (must care around abutment) | Lower (skin fully closed initially) |
| Typical candidates | Good bone quality, low infection risk | Borderline bone quality, higher infection risk |
Both are valid approaches. The “best” choice depends entirely on your unique situation.
Emotional and Mental Preparation
This section is just as important as the medical details. Do not skip it.
The first surgery for an osseointegrated implant is a marathon, not a sprint. You will have good days and hard days.
Common Emotional Experiences
- Excitement – Finally, a path away from socket problems.
- Anxiety – What if something goes wrong?
- Impatience – Why is healing taking so long?
- Isolation – Friends and family may not fully understand.
- Hope – The possibility of better function and comfort.
Helpful Strategies
- Connect with someone who has done it. Online peer support groups are invaluable.
- Keep a daily log. Write down one small win each day.
- Celebrate non-scale victories. Being able to shower sitting down is a win. Sleeping through the night is a win.
- Ask for help when you need it. This is not weakness. It is wisdom.
Costs and Insurance Considerations
Let us be realistic. This surgery is expensive. Knowing the financial landscape helps you plan.
The total cost varies widely based on:
- Your country (US, Canada, Europe, Australia, etc.)
- Specific implant system used
- Hospital fees
- Surgeon’s experience
- Length of hospital stay
Typical Cost Ranges (Before Insurance)
| Location | Estimated Cost for First Surgery |
|---|---|
| United States | 40,000–100,000+ |
| Europe (private) | €25,000 – €60,000 |
| United Kingdom (private) | £30,000 – £70,000 |
| Australia | 50,000–90,000 AUD |
Insurance Coverage
- Some private insurance plans cover osseointegration.
- Medicare in the US covers it for certain leg amputations.
- Veterans’ health systems often cover it for service-related amputations.
- Many plans require prior authorization and proof of failed socket use.
Important: Call your insurance company before scheduling anything. Ask specifically about “osseointegration for limb prosthesis” and get written confirmation.
Checklist: Questions to Ask Your Surgical Team
Before you agree to the first surgery, ask these questions. Write down the answers.
- How many osseointegration surgeries have you personally performed?
- What is your infection rate for the first year?
- Do you use a one-stage or two-stage protocol? Why?
- Which implant system do you use, and why do you prefer it?
- What is your typical hospital stay length?
- How do you manage pain after surgery?
- What happens if the implant does not integrate?
- Can I speak with a previous patient of yours?
- What is your protocol for antibiotics?
- What is the total estimated cost I should expect?
Realistic Outcomes: What Success Looks Like
Let us paint a realistic picture of success. It is not the same for everyone.
Excellent Outcome
- Implant fully integrates with bone.
- No infections after two years.
- You wear your prosthetic 12+ hours daily.
- You walk or use your arm with less pain than with a socket.
- You perform daily activities more easily.
Good Outcome
- Implant integrates but takes longer (6-9 months).
- One minor skin infection, resolved with oral antibiotics.
- You wear your prosthetic 8 to 10 hours daily.
- Pain is moderately better than with a socket.
Acceptable Outcome
- Implant integrates but required a second surgery to manage skin issues.
- Two or three treatable infections in the first year.
- You wear your prosthetic 4 to 6 hours daily.
- Pain is slightly better or the same as before.
Even an acceptable outcome can be life-changing for someone who could not tolerate a socket at all.
When the First Surgery Is Not Successful
Honesty matters. Sometimes the first surgery does not go as planned.
Possible failure modes include:
- Deep infection requiring implant removal.
- Implant loosening due to poor bone integration.
- Persistent pain that does not improve with time.
If this happens, your team will discuss options:
- Remove the implant, treat the bone, and try again in 6 to 12 months.
- Convert to a different implant system.
- Return to socket prosthesis use.
Do not see this as a personal failure. Bone healing is complex, and sometimes bodies simply do not cooperate.
The Path Beyond the First Surgery
Assuming everything goes well, what comes next?
- Healing phase – You already read about this. Several months of protected healing.
- Abutment placement (if two-stage) – A much smaller surgery. Usually outpatient.
- Prosthetic attachment – You finally connect an external limb to your implant.
- Gait or function training – Learning to use your new connection effectively.
- Long-term maintenance – Lifelong skin care around the abutment and annual X-rays.
The first surgery opens the door. Everything after that builds on this foundation.
Conclusion
The first surgery for an osseointegrated implant places a titanium fixture directly into your bone. You will go through preparation, anesthesia, precise bone drilling, and implant insertion—followed by weeks of protected healing. While the process demands patience, it offers a path away from socket problems and toward a more direct, comfortable connection with your prosthetic.
Frequently Asked Questions (FAQ)
1. How painful is the first surgery for an osseointegrated implant?
You will be asleep during the procedure. Afterward, most patients rate pain as 5 to 7 out of 10 for the first few days, then steadily improving. Medications keep it manageable.
2. How long does the first surgery take?
Typically 90 minutes to 3 hours, depending on your bone quality and the specific technique used.
3. Will I have a visible metal pin sticking out after the first surgery?
Not always. In a two-stage procedure, the implant is completely buried under your skin. Only the second surgery exposes the metal.
4. Can I walk right after the first surgery for a leg implant?
No. Most surgeons require six to twelve weeks of no weight-bearing to protect bone healing.
5. What is the success rate of the first surgery?
In experienced centers, the five-year implant survival rate is over 90% for leg implants and over 85% for arm implants.
6. How do I shower after surgery?
Keep the dressing completely dry for the first 10 to 14 days. Use a waterproof sleeve or bag. Your team will give specific instructions.
7. Will I need a blood transfusion?
Rarely. Blood loss is typically minimal (50 to 150 mL) for this surgery.
8. Can I travel home out of state after the first surgery?
Most surgeons ask you to stay local for at least two weeks for follow-up and in case of complications.
9. How soon can I return to work?
Sedentary work: 2 to 4 weeks. Physical work: 3 to 6 months or longer.
10. Does the first surgery guarantee I will love my osseointegrated prosthesis?
No surgery guarantees satisfaction. But studies show most patients report significantly improved quality of life compared to sockets.
Additional Resource
The Osseointegration Group of Australia (OGA) Education Hub
A trusted, patient-friendly collection of videos, brochures, and peer stories.
Link: https://www.osseointegration.com.au/patient-education
Disclaimer: This article provides general educational information and does not constitute medical advice. Every surgical procedure carries risks. Outcomes vary based on individual health, anatomy, and surgical expertise. Always consult with a qualified, experienced osseointegration surgeon to discuss your specific case. Do not use this article to make medical decisions without professional guidance.