Molar Teeth Implant: The Complete, Honest Guide to Replacing Your Back Teeth
If you have lost a back tooth, you might wonder if it is worth replacing. After all, no one sees it when you laugh. But a missing molar is not just about looks. It changes how you chew, how you speak, and even how the rest of your teeth hold their position.
This guide walks you through everything you need to know about a molar teeth implant. We will keep things simple, clear, and realistic. No confusing medical terms. No false promises. Just the honest information you deserve.
Important note: This article is for educational purposes. It does not replace professional medical advice. Always consult a licensed dentist or oral surgeon for your specific case.
Why Replacing a Missing Molar Matters More Than You Think
Many people ignore a lost molar. Because it hides in the back, they assume it does nothing important. That is a mistake.
Molars handle most of the heavy chewing. Grinding food, breaking down tough textures, and protecting your front teeth from excess pressure—these are molar jobs. When one goes missing, the remaining teeth must work harder.
Over time, this leads to:
- Uneven wear on your other molars
- Jaw muscle pain from awkward chewing habits
- Difficulty eating certain foods like nuts or steak
The Domino Effect on Your Smile
Here is what happens inside your mouth after a molar extraction. The empty space acts like a open door. The tooth opposite the gap has no pressure against it. So it starts drifting downward or upward. The teeth next to the gap begin leaning in.
What seems like a single missing tooth becomes a chain reaction. People often do not notice the changes until years later. By then, fixing the alignment requires braces or more extractions.
Bone Loss: The Hidden Consequence
Your jawbone needs stimulation. Every time you chew, the tooth root sends signals to your body to maintain bone density. Remove the root, and the bone starts melting away.
This is not visible right away. But after six months to a year, the bone shrinks. That can make placing an implant later more difficult or expensive. You might need a bone graft first.
What Exactly Is a Molar Teeth Implant?
A dental implant replaces both the root and the crown of a missing tooth. For a molar, this means a strong, wide implant that can handle heavy forces.
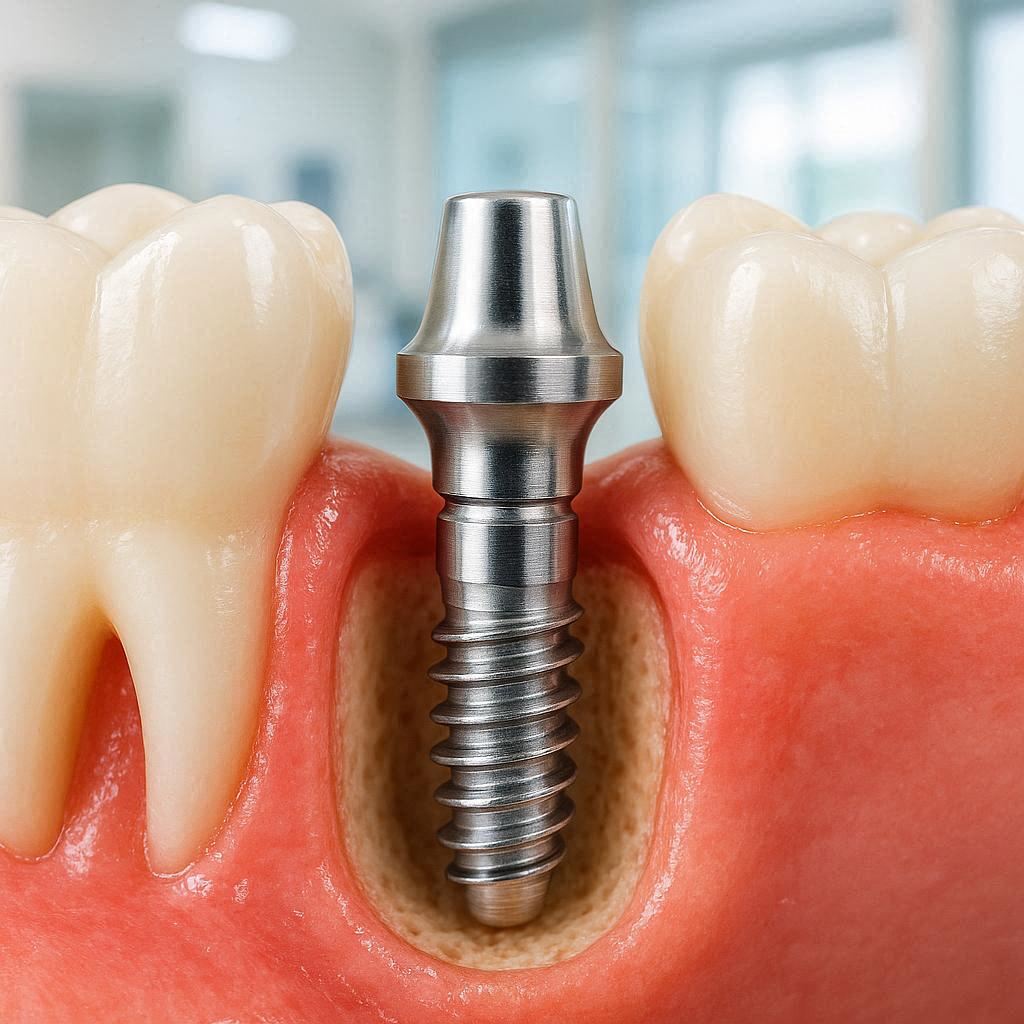
Think of it as three parts working together:
| Component | What it is | Purpose |
|---|---|---|
| The Implant (post) | A screw made of titanium or zirconia | Acts as the artificial root. Fuses with your jawbone. |
| The Abutment | A small connector piece | Joins the implant to the crown. |
| The Crown | The visible false tooth | Made of ceramic or porcelain. Looks and chews like a real molar. |
Unlike bridges, an implant does not touch or damage nearby teeth. Unlike dentures, it does not move or click. It sits securely in your bone, just like a natural root.
Are Molar Implants Different From Front Tooth Implants?
Yes. Molars handle much more bite force. Up to 200 pounds of pressure per square inch in some cases. So molar implants are wider and often shorter than front tooth implants.
Surgeons also place them differently. They must account for the maxillary sinus in the upper jaw and the inferior alveolar nerve in the lower jaw. These structures limit available bone height.
A front tooth implant prioritizes aesthetics. A molar implant prioritizes strength and durability.
Step-by-Step: What Happens During a Molar Implant Procedure
Let us walk through the entire process. Most people find the idea scarier than the reality.
Step 1: The Initial Consultation
Your dentist takes X-rays or a CT scan. They measure your bone density and width. They check for infections or nearby nerves. This is also when you discuss your medical history.
Note: Smokers, diabetics, and people with gum disease may need extra steps before getting an implant. Be honest with your doctor.
Step 2: Preparatory Work (If Needed)
Sometimes the bone is too thin. In that case, you need a bone graft. This adds synthetic or natural bone material to the site. Healing takes four to nine months. It sounds worse than it is. Most people compare the discomfort to a simple extraction.
If the sinus (in the upper jaw) sits too low, you may need a sinus lift. Again, this adds healing time but makes the implant possible.
Step 3: Implant Placement Surgery
The surgeon numbs the area completely. You are awake but feel nothing. They make a small cut in the gum. They drill a precise hole into the bone. Then they screw the implant post into place. Finally, they close the gum over it or attach a healing cap.
The whole surgery for one molar takes 30 to 60 minutes.
Patients often say: “I expected loud drilling and pain. But I just felt vibration. The worst part was the numbing injection.”
Step 4: Osseointegration (The Waiting Period)
This is the most important phase. Your bone grows around the implant surface. This fusion takes three to six months. During this time, you eat soft foods. You avoid chewing directly on that side.
Do not rush this. Implants fail most often when people skip this healing window.
Step 5: Placing the Abutment and Crown
Once the implant is solid, the surgeon uncovers it. They attach the abutment. Then they take impressions to create your custom molar crown. Two weeks later, you return. They screw or cement the crown onto the abutment.
You walk out with a new molar that looks, feels, and works like a natural tooth.
Pain, Recovery, and What You Actually Feel
Let us be real. You want to know how much this hurts.
During the surgery: Zero pain
Local anesthesia blocks everything. Some clinics offer sedation if you feel anxious. But for a single molar, most people stay awake and watch TV or listen to music.
After the numbness wears off: Moderate discomfort
Think of it like having a tooth pulled. The first 24 to 48 hours bring some swelling and soreness. Over-the-counter ibuprofen usually handles it. Most patients describe it as a 3 or 4 on a 10-point pain scale.
Days 3 to 7: Mild tenderness
You might feel pressure when chewing on that side. The gum tissue heals quickly. But the bone continues healing for months. That deep ache is normal. It means the fusion is working.
The full recovery timeline:
| Time after surgery | What to expect |
|---|---|
| 1–2 days | Swelling, minor bleeding, soft food diet |
| 3–7 days | Swelling goes down. Return to light work or normal routine |
| 1–2 weeks | Sutures dissolve or get removed. Resume most normal eating |
| 3–6 months | Osseointegration. Avoid hard foods on implant side |
| After crown placement | Full function. Eat anything you want |
Molar Implant vs. Other Options: An Honest Comparison
You have choices. Let us compare them directly.
Option 1: Do nothing
Cost: $0
Pros: No upfront expense.
Cons: Bone loss, shifting teeth, chewing problems, future expensive repairs.
Option 2: Removable partial denture
Cost: $300–$1,000
Pros: Cheap. No surgery.
Cons: Moves while eating. Covers palate. Can break. Needs replacement every 3–5 years. Does not stop bone loss.
Option 3: Dental bridge
Cost: $2,000–$5,000 (three-unit bridge)
Pros: Faster than implant (2–3 weeks). No bone grafting needed usually.
Cons: Shaves down two healthy teeth. Harder to clean. Average lifespan 10–15 years. Does not prevent bone loss under the missing tooth.
Option 4: Molar implant
Cost: $3,000–$6,000 (single tooth)
Pros: Preserves bone. Lasts 20+ years, often lifetime. No damage to other teeth. Feels natural. Easy cleaning (brush and floss normally).
Cons: Higher upfront cost. Longer treatment time (4–9 months). Requires surgery.
Which one is right for you?
“I tell my patients: A bridge is a bandage. An implant is a cure. If you can afford the time and money, the implant is always better for a molar.” — Dr. Elena Vasquez, prosthodontist.
Success Rates: Do Molar Implants Really Work?
Yes. But let us be honest about the numbers.
For a healthy person with good bone density and no gum disease, a single molar implant has a success rate between 95% and 98% after 10 years. After 20 years, success rates remain above 90%.
What lowers success rates?
- Smoking (cuts success to 85–90%)
- Uncontrolled diabetes
- Severe gum disease
- Poor oral hygiene
- Teeth grinding (bruxism)
- Insufficient bone (even after grafting)
What does “failure” look like?
Early failure (first 3–4 months): The implant never fuses to the bone. It stays loose. The surgeon removes it. You try again after healing.
Late failure (years later): Gum infection around the implant eats the supporting bone. The implant becomes mobile. This is preventable with good home care and regular checkups.
Most failures happen in people who skip their six-month cleanings.
Molar Implant Cost Breakdown (Real Numbers)
Prices vary wildly by location. But here is a realistic range in the United States (2025–2026 averages).
| Service | Low estimate | High estimate |
|---|---|---|
| Consultation and CT scan | $150 | $500 |
| Extraction of broken tooth | $200 | $600 |
| Bone graft (if needed) | $300 | $1,500 |
| Sinus lift (upper molars only) | $1,500 | $3,000 |
| Implant post placement | $1,500 | $3,000 |
| Abutment | $300 | $600 |
| Molar crown | $1,000 | $2,500 |
| Total (simple case, no graft) | $3,200 | $6,600 |
| Total (with bone graft) | $3,800 | $8,000+ |
Does insurance cover any of this? Some plans cover the crown portion. Very few cover the implant itself. But many cover the extraction and the bone graft. Always ask for a pre-treatment estimate.
Payment options
- Dental schools (50–70% cheaper, but longer appointments)
- CareCredit and other medical credit cards
- In-house financing (some clinics offer 0% for 12 months)
- FSA or HSA accounts
Who Is a Good Candidate for a Molar Implant?
Ideal candidates:
- Have one or more missing molars
- Have enough bone height and width
- Do not smoke heavily (or are willing to quit for 2 months)
- Have healthy gums
- Are committed to good oral hygiene
- Are at least 18 years old (jaw growth complete)
What if you do not qualify yet?
That does not mean never. It means not right now. You can:
- Quit smoking for 8 weeks before and after surgery
- Treat gum disease first (deep cleaning, antibiotics)
- Build bone with a graft and wait 6 months
- Control your diabetes with your doctor
Many patients go from “not a candidate” to “perfect candidate” in under a year.
Upper Molar Implants vs. Lower Molar Implants
The jaw matters more than you think.
Lower molars (first and second molars)
Easier to place. The lower jawbone is dense and thick. Nerves run below the roots, but modern imaging avoids them. Healing is predictable.
Challenge: If the nerve is too close, you cannot place a standard implant. Your surgeon might use a shorter implant or an angled placement.
Upper molars (first and second molars)
More complex. The maxillary sinus sits above these roots. Many people have sinus cavities that drop too low. That means a sinus lift before the implant.
The bone in the upper jaw is also softer. Osseointegration takes the full six months. But the success rate is still excellent when done correctly.
Third molars (wisdom teeth)
Dentists almost never replace wisdom teeth. They have no functional value. If you lose a wisdom tooth, you do not need an implant. Save your money.
How to Make Your Molar Implant Last a Lifetime
An implant does not decay. But it can fail from gum disease. The soft tissue around an implant is more delicate than around a natural tooth.
Follow these rules:
Daily care
- Brush twice a day with a soft brush
- Floss daily (use superfloss or implant-specific floss)
- Use a water flosser on low pressure to clean around the abutment
- Avoid abrasive toothpaste (no baking soda or charcoal)
Professional maintenance
- See your dentist every 6 months
- Request an implant check during your cleaning
- X-rays every 12–24 months to check bone levels
Lifestyle choices
- Do not chew ice, hard candy, or bones
- Wear a night guard if you grind your teeth
- Quit smoking (the #1 cause of late implant failure)
Note: A well-maintained molar implant has outlived patients in many studies. The record is over 40 years and counting.
Common Fears and Myths About Molar Implants
Let us clear up the misinformation.
Myth 1: “Implants are experimental.”
False. Modern implants have over 50 years of research. They are the standard of care for single tooth replacement.
Myth 2: “My body will reject the titanium.”
Titanium is biocompatible. Rejection is not a thing. Failure happens from infection or poor healing, not an allergic reaction. True titanium allergy affects less than 0.6% of people.
Myth 3: “It is better to wait until more teeth fall out.”
Worse. Every year you wait, bone loss gets worse. More missing teeth cost more to fix.
Myth 4: “The surgery is dangerous.”
For a healthy person, implant surgery is safer than wisdom tooth extraction. Serious complications occur in less than 1% of cases.
Myth 5: “I am too old.”
Age does not matter. People in their 80s and 90s get implants successfully. Overall health matters more.
The Psychological Benefit You Did Not Expect
Patients often report something surprising. After their molar implant, they feel more confident eating in public. No more worrying about food getting stuck in a gap. No more avoiding restaurants with crunchy or chewy dishes.
One patient told us: “I did not realize how much I was hiding my chewing. At dinner parties, I would cut my food into tiny pieces. Now I just eat normally. It feels like getting a small piece of my life back.”
It sounds dramatic. But the freedom to bite into an apple or enjoy a steak without thinking about your teeth is real.
How to Find a Good Implant Dentist for Your Molar
Not all dentists place implants. Look for:
- Oral surgeon (best for complex bone cases)
- Periodontist (gum and bone specialist)
- Prosthodontist (advanced restorative training)
- General dentist with implant fellowship (can be excellent for simple cases)
Ask these three questions before booking:
- “How many molar implants do you place per year?” (Look for 50+)
- “What happens if my implant fails?” (They should offer a warranty or free replacement)
- “Do you use 3D CT guided surgery?” (Yes is better. More precise, safer.)
Check Google reviews and RealSelf for patient photos. Avoid clinics with prices that seem too good to be true ($1,500 for the whole implant). Those usually exclude the crown or use cheap materials.
Alternatives You Might Not Have Considered
The mini implant
Smaller diameter. Less invasive. Cheaper ($1,500–$2,500). But not designed for molars. Mini implants flex under heavy chewing. Use them only for small teeth or temporary dentures. Do not put one on a molar.
The cantilever bridge
Attaches a false tooth to only one neighboring tooth. Cuts down only one healthy tooth instead of two. But it puts torque on that single tooth. High failure rate for molars. Most dentists avoid this.
Resin-bonded bridge (Maryland bridge)
Wings of metal or ceramic glue to the back of adjacent teeth. No drilling. Cheap ($1,000–$2,000). But the bond fails often for molars because of chewing forces. Good for front teeth. Bad for back teeth.
Orthodontic space closure
If you are missing a second molar, an orthodontist can sometimes move your wisdom tooth forward to close the gap. This takes 12–24 months. Not always possible. But when it works, you avoid an implant completely.
A Realistic Day-by-Day Recovery Timeline
Here is what your first week looks like, hour by hour.
Day of surgery (Day 0)
- Surgery at 9 AM. Home by 11 AM.
- Bite on gauze for 1 hour.
- Ice pack on cheek (20 min on, 20 min off).
- Eat cold soft food (yogurt, smoothie, pudding).
- Sleep with head elevated.
Day 1
- Swelling peaks. Looks like a mild chipmunk cheek.
- Pain 2–3/10 with ibuprofen.
- Rinse gently with warm salt water (no spitting).
- Avoid hot drinks and straws.
Day 2
- Swelling starts going down.
- Bruising may appear (yellow or purple on the cheek, normal).
- Eat scrambled eggs, mashed potatoes, soup.
- Brush other teeth carefully. Avoid the implant site.
Days 3–5
- Almost no pain. Minor tenderness to touch.
- Return to desk work or normal activities.
- Start gentle salt water rinses after meals.
- Sleep normally.
Days 6–7
- Gum looks pink and closed.
- Most people stop all pain medication.
- Try soft solids like pasta or soft bread.
- Avoid chewing on implant side completely.
Week 2
- Stitches dissolve or get removed.
- You forget you had surgery most of the day.
- Still avoid hard, sticky, or crunchy foods.
Month 1
- Normal life. Normal eating on the other side.
- The implant site feels like a hard lump under gum. That is the implant post.
- You start chewing very soft foods on that side (banana, cooked carrot).
Month 3
- Osseointegration half done.
- You can chew most things except nuts, ice, hard candy.
- No pain or awareness of the implant.
Month 6
- Implant is fully fused.
- You get your crown.
- Full function returns.
Nutritional Guide During Healing
Your mouth heals best when you eat well. But you also must protect the implant site.
| Phase | Recommended foods | Foods to avoid |
|---|---|---|
| Days 1–3 | Smoothies, yogurt, pudding, applesauce, protein shakes, broth | Coffee, alcohol, hot soup, nuts, chips, rice (gets in wound) |
| Days 4–7 | Scrambled eggs, oatmeal, mashed potatoes, cottage cheese, hummus | Crusty bread, steak, raw vegetables, popcorn |
| Weeks 2–4 | Soft fish, pasta, bananas, avocados, tofu, ground meat | Chewy candy, bagels, pizza crust, ribs |
| Months 2–6 | Everything soft. Introduce crunchy foods slowly (cookies, soft granola) | Nuts, ice, hard candy, chicken wings with bones |
| After crown | Eat anything. But always avoid ice chewing | Hard objects (pens, fingernails) |
Note: Bone healing requires protein, vitamin C, and calcium. Drink a protein shake daily during the first two weeks. It helps.
What No One Tells You About Living With a Molar Implant
Little quirks you should know:
- The crown clicks sometimes. When you first get it, you might hear a tiny click when biting down hard. That is the crown settling. It goes away in a week.
- Food traps differently. The space between your implant crown and the natural tooth next to it may trap food more than usual. Use floss or a tiny interdental brush.
- Cold sensitivity. For a few weeks after crown placement, the implant might feel cold. This fades as your nerves adapt.
- Professional cleanings require special tools. Your hygienist uses plastic or carbon-tipped scalers instead of metal ones. Metal scratches the crown surface.
- It is not completely numb. Some people expect an implant to feel like a fake tooth. But you feel pressure, texture, and temperature through your gum and bone. It feels remarkably natural.
Molar Implant Costs Around the World (For Medical Tourists)
Some readers consider traveling for cheaper care. Here are average prices for a single molar implant with crown.
| Country | Average cost (USD) | Reputation |
|---|---|---|
| United States | $4,500 | Excellent, gold standard |
| Canada | $4,000 | Excellent |
| United Kingdom | $4,200 | Very good |
| Mexico (border cities) | $1,800 | Good in major clinics, variable |
| Costa Rica | $1,500 | Very good in accredited clinics |
| Colombia | $1,600 | Good, growing reputation |
| Turkey | $700 | Mixed. Top clinics excellent. Cheap ones risky. |
| Thailand | $1,200 | Excellent in Bangkok hospitals |
| India | $900 | Good quality, but travel is far |
| Poland | $1,100 | Very good in major cities |
| Hungary | $1,000 | Excellent for dental tourism |
Warning on medical tourism: If your implant fails after you return home, your local dentist will charge full price to fix it. No warranty transfers across borders. Factor in the cost of a second surgery before you decide.
Frequently Asked Questions (FAQ)
1. Can I get a molar implant years after extraction?
Yes. But you may need a bone graft first. The bone shrinks over time. An evaluation with a CT scan tells you what is needed.
2. How long does the whole molar implant process take?
Four to nine months from extraction to final crown. Most of that is healing time. The actual surgeries take one to two hours total.
3. Will my insurance cover a molar implant?
Rarely. Some PPO plans cover 50% of the crown. Almost never cover the implant post. Call your insurer and ask for the “implant benefit rider.”
4. Can I have two molar implants at the same time?
Yes. Placing adjacent molars in one surgery is common. Recovery is slightly more uncomfortable but not double the pain.
5. What happens if the implant fails after five years?
Your dentist removes it. You heal for three months. Then you place a new implant. The bone is often still there. Success rate for the second attempt is over 90%.
6. Do molar implants feel different from real teeth?
Most people say no. You feel pressure and texture through the bone. The crown material mimics natural tooth enamel. Only the absence of a nerve makes it different (no hot/cold pain).
7. Can I get an MRI with a molar implant?
Yes. Titanium is not magnetic. It does not heat up or move in an MRI. Even the crown (zirconia or porcelain) is safe. Always tell the technician, but it is not a danger.
8. What is the youngest age for a molar implant?
Girls: 16. Boys: 18. The jaw must finish growing. Otherwise the implant ends up in the wrong position as the face matures.
9. Do I need time off work?
Plan for two days off if you have a desk job. One full week if you have a physical job (lifting, bending, heavy talking). Most people take Friday off and return Monday.
10. Can I drink coffee after the surgery?
Not on day one. Wait 48 hours. Hot drinks increase bleeding risk. When you resume coffee, drink it lukewarm and rinse with water afterward.
11. Will my implant crown stain like a real tooth?
Porcelain and zirconia crowns do not stain. Coffee, tea, and wine wash off with normal brushing. The cement line can stain over years, but a professional cleaning fixes it.
12. What if I grind my teeth at night?
You need a night guard. Grinding transfers excessive force to the implant. The implant is strong, but the crown can crack or the screw can loosen. A custom night guard costs $300–$600 and protects your investment.
Additional Resource
For a list of board-certified implant dentists in your area, including patient reviews and cost estimators, visit the American Academy of Implant Dentistry’s patient referral service:
👉 https://www.aaid.com/patient/ (official, non-commercial resource)
Conclusion
Replacing a missing molar with a dental implant is not the cheapest or fastest solution. But it is the most durable, most natural, and healthiest choice for your mouth. You protect your jawbone, save your remaining teeth from shifting, and regain full chewing power for decades. If you can commit to the healing time and the upfront cost, a molar teeth implant is one of the best investments you can make in your long-term oral health.
Disclaimer: This article is for general informational purposes only and does not constitute medical or dental advice. Individual results vary. Always seek the advice of a qualified dentist or oral surgeon with any questions you may have regarding a medical condition or dental treatment. Never disregard professional medical advice because of something you have read in this article.


