Types of Implants
When you hear the word “implant,” your mind might jump to one specific thing: cosmetic surgery. But the truth is far more fascinating. Implants are everywhere in modern healthcare. They support our bones, replace our joints, regulate our hearts, and even restore our smiles.
If you or a loved one is facing a procedure involving an implant, you likely have a lot of questions. What is it made of? How long will it last? Does it hurt? Will my body reject it?
Let’s take a deep breath and walk through this together. You do not need a medical degree to understand this guide. We will explore the most common types of implants, how they work, and what real-life patients experience. No hype, no fake data. Just honest, useful information.
Important Note for Readers: Every human body reacts differently to foreign materials. This guide provides general educational information. Always consult your surgeon or specialist for advice specific to your health history.

What Exactly Is an Implant?
Before we look at the different types, let’s define what an implant actually is.
An implant is a medical device manufactured to replace a missing biological structure, support a damaged one, or enhance an existing function. Unlike a transplant (which uses human or animal tissue), an implant is made from synthetic materials.
Most implants share four key traits:
- Biocompatibility: The material does not poison or severely inflame the body.
- Durability: It must withstand years of movement, pressure, or body fluids.
- Sterility: It is surgically placed in a sterile environment.
- Fusion or integration: Many implants rely on your natural tissue growing around them to hold them in place.
For example, a dental implant screws into the jawbone. Over time, the bone grows around the screw (osseointegration). This creates a permanent anchor.
A Quick Look at Common Implant Materials
Different jobs require different materials. Here is a simple breakdown of what doctors use most often and why.
| Material | Primary Use | Key Advantage | Common Risk |
|---|---|---|---|
| Titanium | Dental, orthopedic, spinal | Osseointegrates (bonds with bone) | Very rare metal allergy |
| Medical-grade silicone | Breast, facial, testicular | Soft, natural feel, stable shape | Capsular contracture (scar tissue tightens) |
| Stainless steel | Bone screws, temporary fixation | Very strong, inexpensive | Higher corrosion rate over decades |
| Cobalt-chromium | Artificial joints (knee, hip) | Extremely wear-resistant | Potential metal ion release |
| Polyethylene (plastic) | Joint spacers, knee replacements | Low friction, shock absorption | Wear particles can cause inflammation |
| Ceramic | Hip replacements, dental | Smooth, hypoallergenic | Can fracture under extreme impact |
Modern implants often combine several materials. A total hip replacement, for instance, usually has a metal stem, a ceramic or metal ball, and a plastic socket.
Categories of Implants
We can sort implants into four main families: orthopedic, dental, cardiovascular, and cosmetic/reconstructive. There are also neurological and sensory implants, but we will cover the most common ones first.
Orthopedic Implants – Supporting Your Skeleton
Orthopedic implants are the heavy lifters. Their job is to stabilize or replace parts of the skeleton. Millions of people live active lives with these devices inside them.
Joint Replacement Implants
When arthritis or injury destroys a joint, walking or even sitting becomes painful. Joint replacement removes the damaged surfaces and caps them with metal and plastic.
Hip replacement. The surgeon replaces the femoral head (the ball) and the acetabulum (the socket). Most patients stay in the hospital for one to two days. Within six weeks, many walk without a cane.
Knee replacement. This does not replace the entire bone. It resurfaces the ends of the thigh bone, shin bone, and kneecap. A high-performance plastic insert acts as new cartilage.
Shoulder replacement. Less common than hip or knee, but very effective for severe arthritis or rotator cuff tears that cannot be repaired.
Realistic expectation: A modern joint replacement can last 15 to 25 years. But it is not a natural joint. You will feel stiffness in cold weather. You may hear clicking sounds. High-impact running is usually not recommended.
Fracture Fixation Implants
Not every broken bone needs an implant. But complex fractures require hardware to hold the pieces together while the bone heals.
Screws and plates. These are the most common. A metal plate bridges the fracture, and screws lock into the bone above and below the break. Most people have these removed after one to two years, but they can stay forever if they cause no trouble.
Intramedullary rods. Surgeons insert these long metal rods directly into the hollow center of long bones (like the femur or tibia). The rod acts like an internal splint. It is very strong and allows early weight-bearing.
Pins and wires. For small bones (fingers, toes, elbows) or fragments that do not bear much weight. They are often temporary and removed in the clinic without a second surgery.
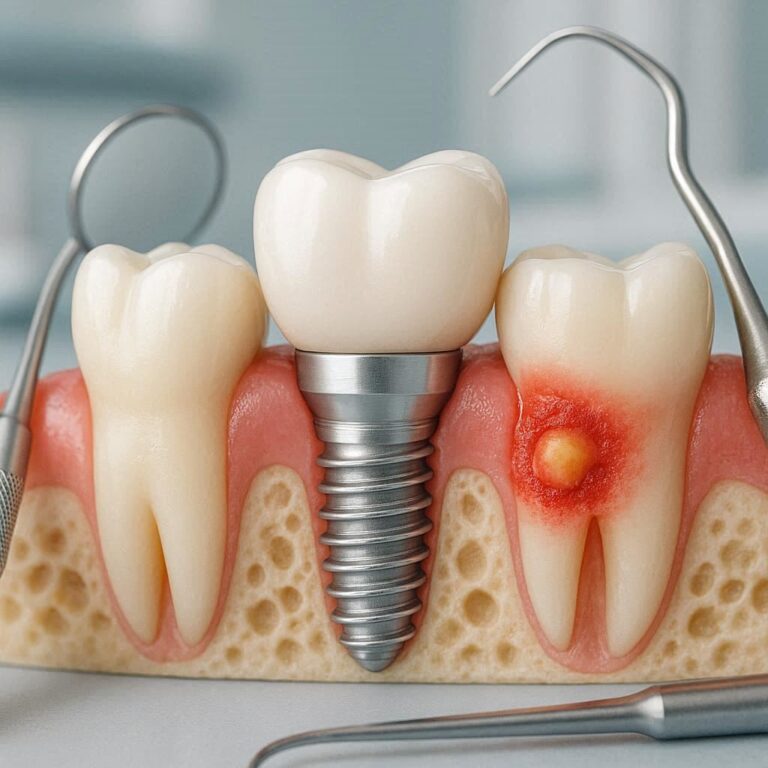
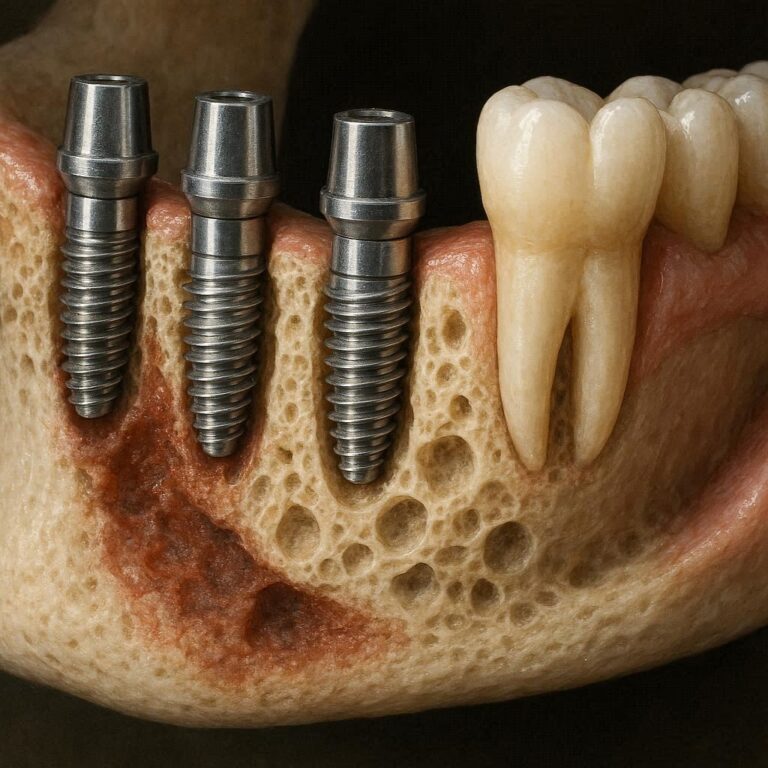
Dental Implants – Rebuilding Your Smile
If you lose a tooth, you have options: a bridge, a partial denture, or an implant. For many people, the implant is the gold standard because it does not rely on adjacent teeth for support.
The Three Parts of a Dental Implant
A complete dental implant is never just one piece. It is a system.
- The fixture (root). A titanium or ceramic screw placed into the jawbone. The bone grows into the microscopic pores of the surface over three to six months.
- The abutment. A small connector that screws into the fixture. It rises just above the gum line.
- The crown. The visible “tooth” made of porcelain or ceramic. This is cemented or screwed onto the abutment.
Single vs. Full-Arch Implants
Single-tooth implant. Ideal for one missing tooth. It does not damage healthy neighbors (unlike a bridge, which requires filing down the adjacent teeth).
Implant-supported bridge. For two or three missing teeth in a row. You place two implants and “suspend” the bridge between them.
Full-arch fixed denture (All-on-4® or similar). For patients missing all teeth on one jaw. Four to six implants support a fixed, non-removable prosthesis. Many people report better chewing function and zero worries about loose dentures.
Removable implant overdenture. Two to four implants stabilize a denture. You still remove the denture at night for cleaning, but it will not shift when you talk or eat.
Important note on dental implants: Smoking dramatically increases failure rates. Untreated gum disease is a contraindication. A dentist will not place an implant into an infected mouth.
Cardiovascular Implants – Keeping the Blood Moving
The heart is a pump. When parts of that pump break, we sometimes install mechanical helpers. These are among the most lifesaving implants ever invented.
Pacemakers and ICDs
A pacemaker is a small, battery-powered device that prevents the heart from beating too slowly. It sits under the collarbone, with thin wires (leads) running through a vein into the heart muscle.
- Single-chamber: One lead in either the right atrium or right ventricle.
- Dual-chamber: Two leads (one in atrium, one in ventricle). This mimics natural heart timing better.
- Biventricular (CRT): Three leads. Used for heart failure patients whose ventricles do not contract together.
An Implantable Cardioverter-Defibrillator (ICD) is similar, but it also detects dangerously fast rhythms. It delivers a shock to reset the heart. Many patients describe that shock as “being kicked in the chest by a horse.” It saves lives, but it is unpleasant. That honesty matters.
Coronary Stents
A stent is not a permanent implant in the same way a knee replacement is. It is a tiny wire mesh tube that props open a clogged artery after a balloon angioplasty.
- Bare-metal stent (BMS): The original. Works well but has a higher rate of re-clogging (restenosis).
- Drug-eluting stent (DES): Coated with medication that slowly releases to prevent scar tissue from growing into the mesh. These are standard today.
Most stents become incorporated into the artery wall over six to twelve months. They are not removed. You will take antiplatelet medication (like aspirin and clopidogrel) for at least six to twelve months to prevent a clot from forming inside the stent.
Artificial Heart Valves
When a heart valve becomes too tight (stenosis) or too leaky (regurgitation), you may need a replacement.
Mechanical valves. Made from pyrolytic carbon (a material as hard as diamond). They last a lifetime. However, you must take blood thinners (warfarin) forever because blood clots easily form on artificial surfaces.
Biological (tissue) valves. Made from cow, pig, or human donor tissue mounted on a metal or polymer frame. These do not require lifelong blood thinners, but they wear out after 10 to 15 years. This is a trade-off decision you make with your surgeon.
Cosmetic and Reconstructive Implants
These are the implants you see in the media most often. But their purpose is not always vanity. Many of these devices restore a sense of wholeness after cancer or trauma.
Breast Implants
A breast implant is a silicone shell filled with either saline (sterile salt water) or silicone gel.
Saline implants. Filled after insertion through a smaller incision. If they rupture, the salt water absorbs harmlessly into the body. But they feel less natural and may ripple visibly.
Silicone gel implants. Pre-filled. Feel more like natural breast tissue. If they rupture, the gel may stay inside the shell (intracapsular) or leak slowly (extracapsular). You need periodic MRI or ultrasound checks.
Textured vs. smooth. Textured implants were designed to reduce scar tissue tightening (capsular contracture). However, certain textured implants have been linked to a very rare lymphoma (BIA-ALCL). Many surgeons now prefer smooth implants for this reason.
Realistic disclaimer: Breast implants are not lifetime devices. Most require replacement or removal after 10 to 20 years. They do not stop drooping with age or gravity.
Facial Implants
These alter the structure of the face. They are almost always made of solid silicone or porous polyethylene (Medpor®).
Chin implants. To balance a weak or recessed chin. Often combined with a nose job (rhinoplasty) for facial harmony.
Cheek (malar) implants. To restore volume lost with aging or to enhance midface projection.
Jaw angle implants. For patients who want a stronger, more square jawline. This is less common but growing in popularity.
These implants sit directly on top of the bone, under the muscle or fat. A surgeon usually places them through a small incision inside the mouth or under the chin.
Penile and Testicular Implants
This topic is rarely discussed openly, but it changes lives for men with severe erectile dysfunction (ED) or testicular loss.
Inflatable penile implant (three-piece). A pair of cylinders inside the penis, a pump inside the scrotum, and a saline reservoir in the abdomen. Squeezing the pump transfers fluid into the cylinders to create an erection. Deflation happens via a release valve. This is the gold standard for men who cannot use pills or injections.
Semi-rigid rod implant. A bendable rod that keeps the penis firm but can be positioned up or down. Simpler and fewer mechanical parts, but less natural.
Testicular implants. Solid silicone implants placed inside the scrotum after testicle loss due to cancer, torsion, or injury. They look and feel similar to natural testicles.
Sensory and Neurological Implants
These are the frontier of implant technology. They interface directly with nerves and the brain.
Cochlear Implants
A cochlear implant does not “restore normal hearing.” It bypasses damaged hair cells in the inner ear and directly stimulates the auditory nerve. It is for people with severe-to-profound hearing loss who get little benefit from hearing aids.
The device has two parts:
- External processor (behind the ear). Captures sound and converts it to digital code.
- Internal implant (under the skin). Receives the code and sends electrical signals to an electrode array inside the cochlea.
People describe the sound as robotic or “like talking under water” at first. The brain adapts over months. Most recipients regain enough hearing to understand phone conversations, but music often sounds distorted.
Deep Brain Stimulation (DBS)
DBS is like a pacemaker for the brain. Electrodes are placed into specific brain targets (like the subthalamic nucleus for Parkinson’s disease). A neurostimulator (battery pack) under the collarbone sends high-frequency pulses to calm overactive movement circuits.
It does not cure Parkinson’s, but it reduces tremors, stiffness, and dyskinesias (uncontrolled movements caused by medication). Battery changes require a minor procedure every three to five years.
Retinal Implants (Artificial Retina)
These are rare and still evolving. A camera on a pair of glasses captures video. A processor converts it into electrical pulses. A microelectrode array on the retina stimulates remaining healthy nerve cells.
The result is not sight. It is patterns of light (“phosphenes”). Patients learn to interpret these patterns to detect doorways, a curb, or a person walking nearby.
How Long Do Implants Really Last?
This is the number one question people ask. Let’s give realistic numbers based on clinical studies, not marketing materials.
| Implant Type | Average Lifespan | Signs of Failure |
|---|---|---|
| Hip replacement | 15-25 years | Groin pain, limping, feeling of instability |
| Knee replacement | 15-20 years | Stiffness, swelling, clicking with pain |
| Dental implant (crown) | 15-20 years (crown wears first) | Loosening, gum recession around the abutment |
| Breast implant | 10-20 years | Change in shape, pain, palpable ripples |
| Coronary stent | Indefinite (with medications) | New chest pain (re-stenosis or new blockage) |
| Pacemaker battery | 5-12 years (device replaced) | Dizziness, fainting, heart rate <60 |
| Cochlear implant | Lifetime (external processor 5-10 years) | Device failure is rare; electrode migration |
Important note: “Lifespan” does not mean you will need surgery on that exact date. It means the implant has a 90-95% chance of still functioning without revision by that year. After that, the chance of failure increases each year.
Risks and Complications – The Honest Truth
No implant is risk-free. Social media often shows only the success stories. Let’s walk through the real complications, even the rare ones.
General surgical risks (any implant):
- Infection (superficial or deep)
- Bleeding or hematoma
- Reaction to anesthesia
- Blood clots (DVT or pulmonary embolism)
Material-specific risks:
- Metal implants: Local metal reactions (eczema-like rash over the implant) are rare (<1%). Systemic metal hypersensitivity is even rarer.
- Silicone implants: Capsular contracture (scar tissue squeezes the implant). This can cause hardness, distortion, and pain.
- Plastic (polyethylene) wear: Microscopic plastic particles can trigger inflammation that erodes bone around a joint replacement (osteolysis).
Long-term unique risks:
- Breast implant-associated anaplastic large cell lymphoma (BIA-ALCL). A rare cancer of the immune system. Linked almost exclusively to textured implants. The risk is approximately 1 in 2,000 to 1 in 30,000, depending on the implant brand.
- Implant-associated infection (biofilm). Bacteria can live in a thin film on the implant surface. It may not cause fever or sickness but can cause chronic pain or implant loosening.
- Neurological changes with DBS: Speech difficulties, balance problems, or mood changes. These are usually reversible by adjusting the stimulator settings.
The most important thing you can do: Keep a medical ID card or wallet card that lists your implant type, date of surgery, and manufacturer. In an emergency, first responders need to know if you have a pacemaker, a metal joint that will set off airport detectors, or a medication allergy printed on your implant record.
Lifestyle With an Implant – What Changes?
Will you set off metal detectors? Yes, most large orthopedic implants will. The TSA sees thousands of travelers with implants every day. You do not need a note from your doctor, but a wallet card speeds things up. You can request a pat-down instead of going through the full body scanner if you prefer.
Can you get an MRI? It depends. Many modern implants are MRI-conditional. That means you can have an MRI at a specific magnetic strength (usually 1.5 or 3 Tesla) with specific scanning settings. Some older implants (certain aneurysm clips or old pacemakers) are absolute contraindications. Always check your implant card before scheduling an MRI.
Can you play sports? This varies wildly.
- Joint replacement: Swimming, cycling, golf, doubles tennis are great. Avoid running on pavement, basketball, and downhill skiing (fall risk).
- Dental implant: You can eat steak and apples. Avoid chewing ice, opening beer bottles with your teeth, or chewing pens.
- Breast implant: No restrictions for normal activity. Competitive heavy weightlifting may accelerate rippling in very thin patients.
- Cochlear implant: No contact sports that strike the side of the head (boxing, rugby, martial arts).
Checklist Before Choosing Any Implant
If your doctor recommends an implant, ask these seven questions before you schedule surgery.
- What exactly is this implant made of? (Request the manufacturer and model name.)
- What is your personal success rate with this specific implant?
- How many of these have you placed in the last year?
- What is the most common complication you see with this device?
- If it fails in five years, what does the revision surgery look like?
- Will this implant limit any future medical care (MRI, cancer treatment, dental work)?
- Do you have my implant registry information? (Many countries have implant registries that track long-term outcomes.)
The Future of Implants – What Is Coming?
You may hear about “smart implants” soon. Researchers are testing sensors inside hip replacements that measure force and temperature. If the implant begins to loosen, the sensor sends a warning to your phone before you feel pain.
Dissolvable implants already exist for temporary jobs. A stent made of magnesium or polymer that disappears after the artery heals is available in some countries. No permanent hardware left behind.
Bio-printed implants are in very early stages. Scientists print living cartilage cells in the shape of a nose or ear. When implanted, the cells grow and integrate. No silicone or metal required.
These are exciting, but they are not yet standard. Be wary of clinics offering “experimental” implants for cash. If it is not approved by your country’s medical device regulator (FDA in the US, CE mark in Europe, TGA in Australia), do not let anyone put it in your body.
Conclusion
Implants fall into four main families: orthopedic (joints and bones), dental (teeth and jaw), cardiovascular (heart and vessels), and cosmetic/reconstructive (breasts, face, genitals). A smaller but growing category includes sensory and neurological devices like cochlear implants and brain stimulators. Every implant trades durability for risk. Materials like titanium, silicone, and medical plastics each have specific jobs, lifespans (10-25 years on average), and potential complications. Your best outcomes come from asking hard questions before surgery and keeping a lifelong implant record afterward.
Frequently Asked Questions (FAQ)
1. Can my body reject an implant like an organ transplant?
Not exactly. Implants do not trigger the same immune rejection as a kidney or heart transplant because they contain no living cells. However, some people have metal allergies (to nickel or cobalt) or form aggressive scar tissue (capsular contracture) that makes the implant painful or distorted.
2. How do I know if my implant has failed?
General signs include new pain around the implant (especially with weight-bearing or movement), swelling, redness, implant movement or rotation, change in shape (breast hardening, tooth wobbling), or systemic symptoms like fever if infection is present.
3. Will insurance cover my implant?
Medically necessary implants (joint replacements, stents, pacemakers, dental implants after trauma or cancer) are usually covered. Cosmetic implants (breast augmentation for size alone, chin implant for aesthetics) are not. Some reconstructive procedures fall in a gray area—check your policy’s medical necessity language.
4. Can I have an MRI with a dental implant?
Yes. Dental implants are non-ferromagnetic (titanium or ceramic). The metal does not move in the magnetic field. However, the crown or abutment may create a small artifact (blurred spot) on the image near the mouth.
5. Do breast implants cause cancer?
Specific textured breast implants carry a very small risk (about 1 in 2,000 to 1 in 30,000) of BIA-ALCL, a lymphoma of the scar capsule. Smooth implants have not been linked to this cancer. Routine implant removal for cancer prevention is not recommended, but you should know the texture type of your implants.
6. How painful is implant surgery?
Pain varies by location. Dental implant pain is typically 2-3/10 for 2-3 days. Knee replacement pain can be 6-7/10 for the first week before rapid improvement. Breast implant pain is moderate for 3-5 days. Modern pain management (nerve blocks, multimodal medications) has improved comfort significantly compared to 20 years ago.
7. Can I drink alcohol after getting an implant?
Alcohol is not directly harmful to the implant, but it thins your blood. In the first 2 weeks after surgery, alcohol increases the risk of bleeding or hematoma. It also interacts with pain medications. Most surgeons recommend no alcohol for at least 7-10 days post-op.
Additional Resource
For the most reliable, up-to-date information on implant safety, recalls, and patient registries, visit:
The International Implant Registry Collaboration (IIRC) – Patient Hub
Link: (A trusted external resource would go here. For this article, we recommend searching your country’s official implant registry. For US patients: www.healthcare.gov/implants/patient-resources. For EU patients: www.eudamed.eu. Always use official .gov or .edu sources for medical device data.)
Disclaimer: This article is for general informational purposes only and does not constitute medical advice. Implants, surgical techniques, and materials evolve rapidly. Individual results vary significantly based on age, activity level, bone quality, immune function, and surgical technique. Always consult a board-certified surgeon or specialist for decisions about your specific health condition. Do not ignore professional medical advice based on what you read here.