Can Dental Implants Get Infected?
If you have a dental implant—or are thinking about getting one—you have probably asked yourself this question at some point.
Can dental implants get infected?
The short answer is yes. But the longer answer is more important.
Infections around dental implants are real, but they are also manageable. Most implant infections are preventable. And when they do happen, a good dentist can treat them effectively.
This guide walks you through everything you need to know. No complicated medical terms. No scare tactics. Just honest, practical information.
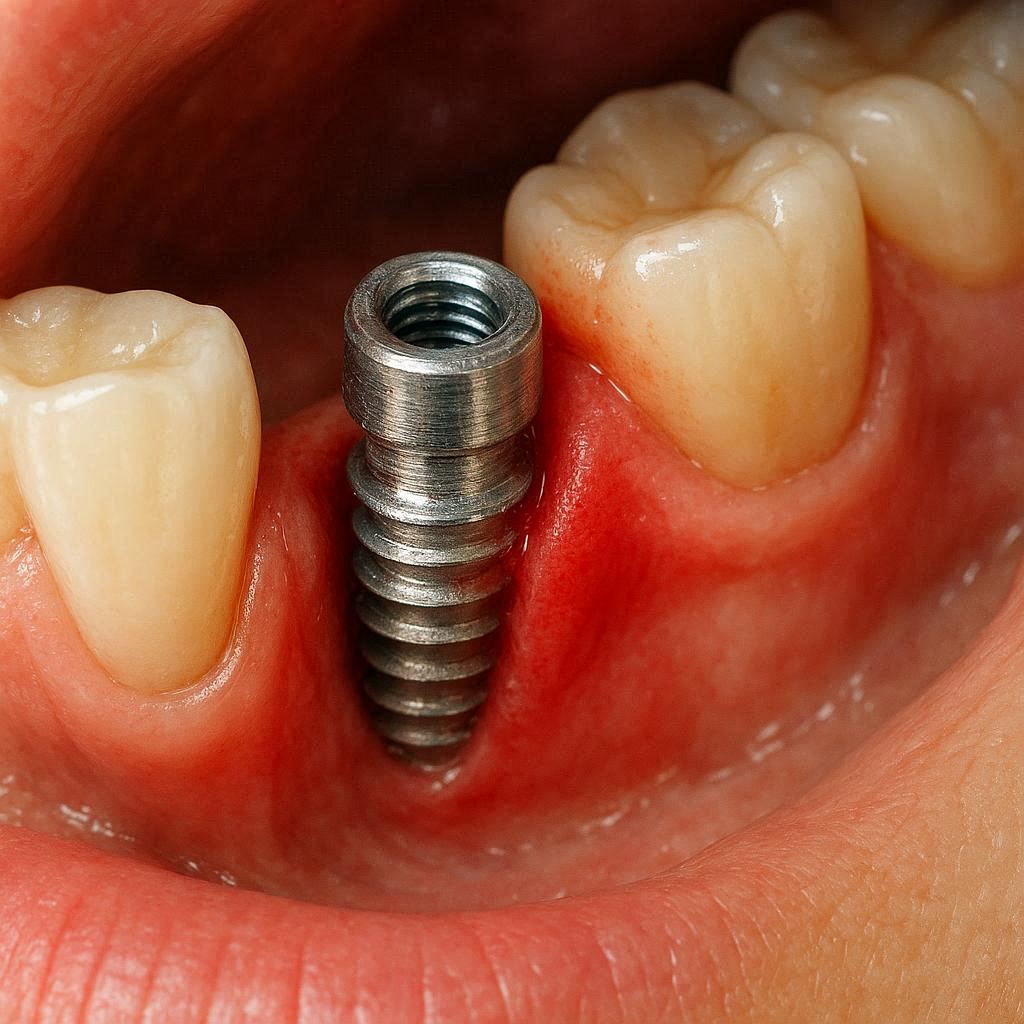
What Does an Implant Infection Actually Mean?
A natural tooth gets infected inside the root. That is a standard cavity or root canal problem.
A dental implant is different. It is made of titanium or zirconia. Those materials cannot decay. So the infection does not happen inside the implant.
Instead, the infection happens in the gum and bone surrounding the implant.
Think of the implant as a post anchored in your jaw. The infection attacks the “ground” around that post. Over time, that ground can weaken.
Dentists call this condition peri-implantitis.
Peri-Implantitis vs. Peri-Implant Mucositis
There are two levels of infection around an implant.
| Condition | What Happens | Is It Reversible? |
|---|---|---|
| Peri-implant mucositis | Gums are red, swollen, and bleed when touched. No bone loss yet. | Yes, with professional cleaning and better home care. |
| Peri-implantitis | Gums are inflamed and the supporting bone starts to dissolve. | Partially. Damage can be stopped but lost bone does not grow back on its own. |
Important note: Peri-implant mucositis is very common. Up to 80% of implant patients may experience it at some point. The key is to treat it before it becomes peri-implantitis.
How Common Are Implant Infections?
This is a fair question. You might be worried that implants are risky.
Here are realistic numbers from dental research:
- About 20% to 30% of implant patients develop peri-implantitis at some stage.
- Mild mucositis is even more common.
- Severe bone loss happens in roughly 5% to 10% of cases.
Those numbers sound concerning. But here is the good news.
Most of those cases are mild. Many are caught early. And almost all could have been prevented with good oral hygiene and regular checkups.
Implants are still one of the most successful dental procedures. The long-term success rate is over 95% for healthy patients who take care of their mouths.
Infections do happen. But they are not the end of your implant.
Early Signs: How to Know If Your Implant Is Infected
Your body usually gives you warnings before a full infection sets in. You just need to know what to look for.
Watch for these symptoms:
- Bleeding when brushing near the implant. Healthy gums should not bleed.
- Red or purple-looking gums around the implant site.
- Swelling that does not go down.
- Bad taste or bad breath that stays even after brushing.
- Pus coming from the gum line. This is a clear sign of infection.
- The implant feels loose. This is a late sign and requires immediate attention.
- Pain when chewing or pressing on the implant. Some discomfort is normal after placement, but not months or years later.
What does NOT always mean infection?
- Mild soreness the week after surgery (that is healing).
- A small gap between the crown and gum (sometimes normal).
- Cold sensitivity on nearby natural teeth.
Reader tip: Take a photo of your implant gum line once a month. Compare them over time. Changes are easier to see side by side.
Why Do Implant Infections Happen?
Infections do not come out of nowhere. There is almost always a cause. Understanding the cause helps you prevent the problem.
Most Common Causes
1. Poor oral hygiene
Bacteria build up around the implant just like around natural teeth. If you do not clean that area, the bacteria multiply. The gums get angry. Then the bone gets angry.
2. Smoking or tobacco use
Smokers have a significantly higher risk of implant infections. Tobacco slows blood flow to the gums. Less blood flow means slower healing and weaker defenses against bacteria.
3. A history of gum disease
If you lost teeth due to periodontitis (advanced gum disease), you are more prone to peri-implantitis. The bacteria that hurt your natural teeth can also hurt your implants.
4. Poor implant placement
Sometimes the implant is placed too close to another tooth root. Or the crown does not fit perfectly. Gaps trap food and bacteria. A well-placed implant is much easier to keep clean.
5. Uncontrolled medical conditions
Diabetes, especially when blood sugar is not well managed, increases infection risk. Autoimmune diseases and some medications also play a role.
6. Grinding your teeth (bruxism)
Grinding does not cause infection directly. But it puts extra pressure on the implant. That pressure can cause micro-movements. Those movements create tiny gaps where bacteria hide.
Can a Dental Implant Infection Spread?
Yes, but not in the way you might think.
The infection does not “travel” through your bloodstream like a fever or flu. Instead, it spreads locally.
If one implant develops peri-implantitis, the inflammation can affect neighboring implants. It can also worsen gum disease on nearby natural teeth.
In very rare cases, a severe untreated infection can lead to a dental abscess in the bone. That abscess can swell and become a medical emergency if it blocks your airway or spreads to other parts of your head and neck.
But again, that is rare. Most implant infections stay local for months or years before becoming serious.
Treatment Options: What Will Your Dentist Do?
Good news again. Implant infections are treatable. The treatment depends on how advanced the infection is.
Stage 1: Peri-implant mucositis (no bone loss)
- Deep cleaning around the implant with special instruments (plastic or titanium ones, never metal scrapers).
- Antibacterial rinses (chlorhexidine) for a week or two.
- Improved home care instructions. Your dentist may show you special floss or small brushes for implants.
Outcome: Full healing is very likely.
Stage 2: Mild to moderate peri-implantitis (some bone loss)
- Open flap debridement. A small cut in the gum allows the dentist to clean the implant surface directly.
- Surface decontamination. The implant is cleaned with special solutions, lasers, or air polishers.
- Bone grafting may be added if the bone loss is significant but not extreme.
Outcome: The infection stops. The bone does not grow back, but it stops shrinking.
Stage 3: Severe peri-implantitis (significant bone loss, loose implant)
- Same cleaning procedures as Stage 2, but more aggressive.
- Resective surgery. The dentist reshapes the remaining bone to make cleaning easier.
- Implant removal. If the implant is too loose or too much bone is gone, removal is the safest option.
Outcome: If removed, you can often place a new implant after the bone heals (6 to 12 months later).
Quote from a periodontist (paraphrased for clarity):
“I tell all my implant patients the same thing. Your implant is not a set-it-and-forget-it solution. It is a partnership. You do your part with cleaning. I do my part with checkups. Together we keep it healthy.”
How to Prevent an Implant Infection (What Actually Works)
Prevention is easier than treatment. Much easier.
Here is a practical checklist.
Daily Home Care
- Brush twice a day with a soft toothbrush. Pay special attention to the gum line around the implant.
- Use interdental brushes. These small brushes fit between the crown and the gum. They are more effective than floss for implants.
- Try a water flosser on a low setting. Water flossers flush out bacteria from deep pockets.
- Avoid abrasive toothpaste. Some whitening toothpastes scratch implant surfaces. Scratches collect bacteria.
Professional Maintenance
- See your dentist every 6 months for an implant checkup. Not all hygienists are trained in implant care. Ask specifically for someone who is.
- Get annual x-rays to monitor bone levels around the implant. Yearly is usually enough for healthy patients.
- Ask for a probing exam every 12 to 24 months. Your dentist measures pocket depths around the implant. Depths over 5 mm need attention.
Lifestyle Choices
- Quit smoking. This is the single biggest thing you can do to reduce infection risk. Even cutting back helps.
- Control your blood sugar if you have diabetes. Stable glucose levels keep your gums healthier.
- Wear a night guard if you grind your teeth. Less pressure means less risk of micro-gaps.
A Helpful Comparison: Implant vs. Natural Tooth Infection
| Feature | Natural Tooth Infection | Dental Implant Infection |
|---|---|---|
| What gets infected | The inner pulp (nerve and blood vessels) | The gum and bone around the implant |
| Pain level | Often severe, throbbing | Usually mild or dull until late stages |
| Visible signs | Abscess on gum near tooth root | Redness, bleeding, possible pus |
| Treatment | Root canal or extraction | Deep cleaning, surgery, or removal |
| Can it be cured? | Yes, with root canal | Yes, if caught early |
| Prevention | Brushing, flossing, fluoride | Brushing, special implant brushes, regular probing |
What If You Ignore an Infected Implant?
This is important. Do not ignore the signs.
If you leave peri-implantitis untreated:
- Bone loss continues slowly over months or years.
- The implant becomes loose. At first it might move slightly. Then it becomes unstable.
- The infection can spread to adjacent teeth or implants.
- Eventually, the implant falls out or must be surgically removed.
- You may lose so much bone that a new implant is no longer possible without a bone graft (which adds time and cost).
The good news? Most people do not reach that point because they notice the early signs.
If you are reading this and thinking “my gums bleed around my implant,” call your dentist this week. Not next month.
Frequently Asked Questions (FAQ)
1. Can a dental implant infection go away on its own?
No. Without treatment, it will not go away. Mucositis might improve slightly with better brushing, but true peri-implantitis requires professional care.
2. Can antibiotics cure an infected implant?
Antibiotics help control the bacteria, but they do not remove the buildup on the implant surface. You still need a professional cleaning. Antibiotics alone are rarely enough.
3. How long does it take for an implant to get infected?
Infections can appear within weeks of placement (if hygiene is poor) or years later (slow bone loss). Most cases develop 1 to 5 years after the implant is placed.
4. Can I brush an infected implant?
Yes, gently. Keeping the area clean is essential. Use a soft brush. Do not scrub aggressively. And see your dentist as soon as possible.
5. Is the pain different from a normal toothache?
Usually, yes. Implant infections tend to cause dull ache or pressure, not the sharp, throbbing pain of a tooth abscess. But pain levels vary from person to person.
6. Will my insurance cover implant infection treatment?
Many dental insurance plans cover peri-implantitis treatment as a “periodontal procedure.” However, some consider it “implant maintenance” and limit coverage. Check with your provider.
Additional Resource
For a deeper look at implant hygiene tools and techniques, visit the American Academy of Periodontology’s patient page on peri-implant diseases.
🔗 Link: www.perio.org/for-patients/peri-implant-diseases
(This is a real, authoritative resource from a leading professional organization.)
Final Thoughts in Three Lines
Dental implants can get infected, but most infections are preventable with good daily cleaning and regular dental checkups. Early signs like bleeding gums and redness should never be ignored—treatment is much easier at that stage. If you take care of your implant like you take care of your natural teeth, your chances of a serious infection are very low.
Conclusion (Summary)
To wrap it up: yes, dental implants can get infected. The infection is called peri-implantitis and affects the gums and bone around the implant, not the implant itself. Most cases are preventable, treatable if caught early, and only lead to implant loss in advanced or neglected situations.
Stay consistent with your home care. See your dentist regularly. And pay attention to the early signs. Your implant can last a lifetime if you treat it right.


