Pain After Implant Placement: What to Expect, How to Manage It, and When to Worry
So, you just got a dental implant. First of all, congratulations. You have taken a big step toward restoring your smile and your chewing ability.
Now, you are probably feeling some discomfort. You might be asking yourself: Is this pain normal? How long will it last? Did something go wrong?
Let us be honest. Dental implant surgery is a surgical procedure. You had a tiny titanium post placed directly into your jawbone. Your body will react to that. Some pain after implant placement is completely normal. In fact, it is expected.
However, not all pain is the same. There is a big difference between standard healing discomfort and signs of a complication.
This guide will walk you through everything you need to know. We will cover the first 24 hours, the first week, and the months after. You will learn practical tips to reduce pain, red flags to watch for, and realistic timelines for feeling better.
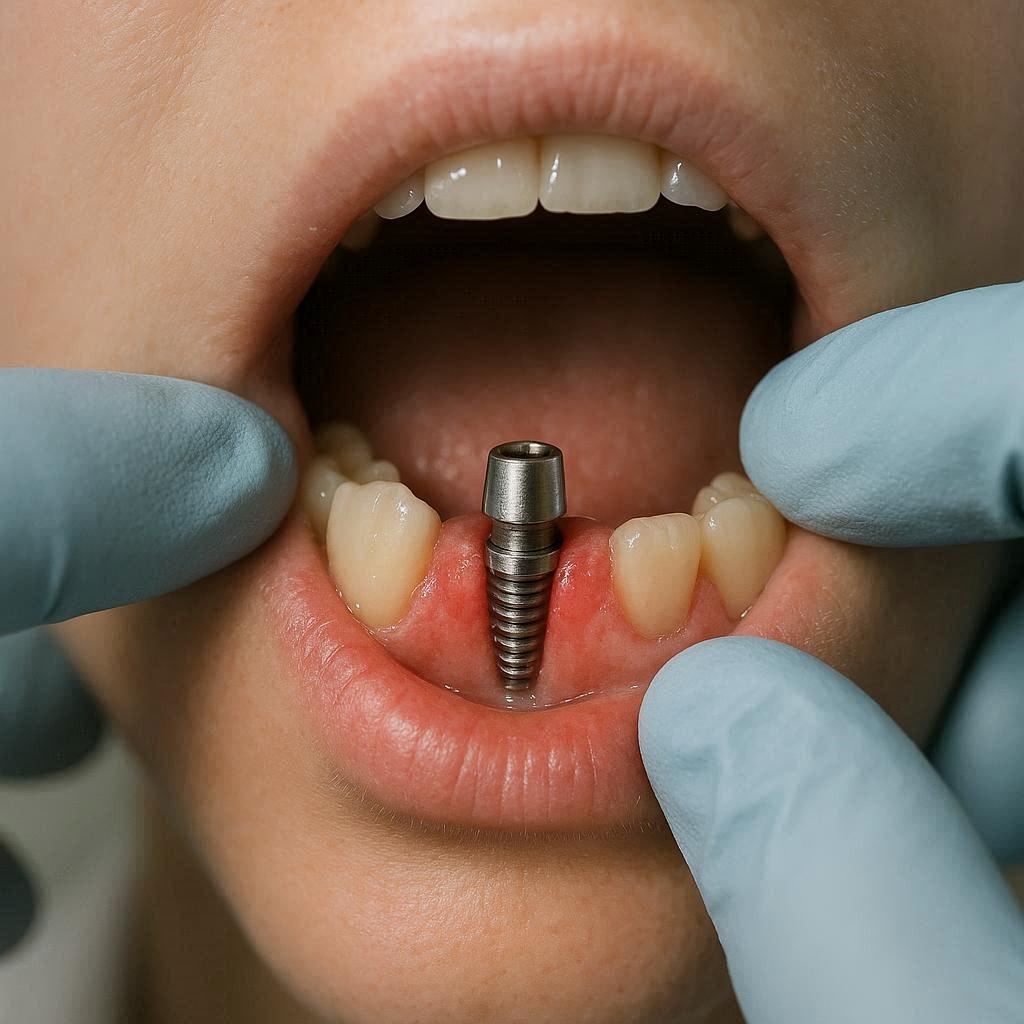
Understanding the Procedure: Why Does It Hurt?
Before we talk about pain management, it helps to understand what actually happened during your surgery.
A dental implant is not a natural tooth. It is a screw-like post made of titanium. Your dentist or oral surgeon placed this post deep into your jawbone. They did this to replace the root of your missing tooth.
During the procedure, your dentist had to:
- Cut through your gum tissue.
- Drill a precise hole into your bone.
- Insert the implant.
- Possibly place a healing cap or suture the gum tissue over the implant.
Your body sees this as an injury. So, it sends inflammatory cells to the area. This inflammation causes swelling, redness, and pain. This is not a bad thing. In fact, inflammation is the first step of healing.
Important note: The amount of pain you feel depends on several factors. These include the number of implants placed, whether you needed bone grafting, your personal pain tolerance, and the skill of your surgeon.
Normal Pain vs. Abnormal Pain After Implant Placement
This is the most important section of this article. Knowing the difference between normal and abnormal pain can save you from serious problems.
What Normal Pain Feels Like
Normal pain after implant placement is predictable. It follows a pattern.
| Timeframe | Typical Sensation | Intensity (0-10 scale) |
|---|---|---|
| First 6-8 hours | Dull ache, throbbing as anesthesia wears off | 3 to 6 |
| Day 1 to 3 | Localized soreness, tenderness to touch | 2 to 5 |
| Day 4 to 7 | Mild discomfort, occasional twinges | 1 to 3 |
| Week 2 onward | Intermittent sensitivity, no constant pain | 0 to 1 |
Key characteristics of normal pain:
- It gets better day by day.
- It responds to over-the-counter medication.
- It is located only around the implant site.
- It does not wake you up at night after the first 48 hours.
- You can control it with ice packs and rest.
What Abnormal Pain Feels Like
Abnormal pain is different. It is your body sending an urgent signal.
| Sign | What It Means |
|---|---|
| Pain that gets worse after day 3 | Possible infection or inflammation overload |
| Sharp, shooting pain | Possible nerve involvement |
| Pain spreading to ear, eye, or neck | Signs of spreading infection |
| Unbearable pain that medication does not touch | Possible dry socket (rare for implants) or fracture |
| Pain with fever over 101°F (38.3°C) | Systemic infection |
Important note: If you feel any of the abnormal pain signs, call your dentist immediately. Do not wait to “see if it gets better.”
The First 24 Hours: What to Expect Hour by Hour
Let us walk through the first day after your surgery. Knowing what comes next will reduce your anxiety.
Hours 1-3: The Numb Phase
You just left the dental office. Your lips, cheek, and tongue still feel numb. You have gauze pads biting down on the implant site.
What you feel: Nothing yet. The local anesthesia is still working.
What you should do:
- Keep the gauze in place for 45-60 minutes.
- Do not eat anything until the numbness wears off completely.
- Do not spit, rinse, or use a straw.
- Go home and rest with your head elevated.
Hours 4-8: The Waking Pain
The anesthesia is wearing off. You will start to feel a dull, throbbing ache. This is the most intense phase of pain after implant placement for most people.
What you feel: A deep, pressure-like pain. It might feel like a bad toothache. Swelling begins to appear.
What you should do:
- Take your first dose of pain medication before the numbness completely disappears. Do not wait for the pain to become severe.
- Apply an ice pack to your face for 20 minutes on, 20 minutes off.
- Eat soft, cold foods like yogurt, smoothies (with a spoon, not a straw), or ice cream. Cold helps reduce swelling.
- Rest. Do not bend over or lift anything heavy.
Hours 9-24: The Settling Phase
The initial sharp pain should start to fade. It becomes a manageable soreness.
What you feel: A constant ache that feels like a bad bruise. Swelling peaks around hour 18.
What you should do:
- Continue ice packs.
- Take your medication as prescribed or recommended.
- Sleep with your head on two pillows to reduce swelling.
- Stick to liquids and soft foods.
Days 2 to 7: The Healing Curve
This is the week where most patients see dramatic improvement. Each day should feel slightly better than the last.
Day 2: The Swelling Peak
Your face might look puffy now. Swelling often reaches its maximum on the second day. It might even travel down to your jawline or neck. This is normal.
Pain level: Moderate. More of a constant ache than sharp pain.
Tips for day 2:
- Switch from ice to warm compresses after 48 hours. Warmth increases blood flow and speeds healing.
- Gently rinse your mouth with warm salt water (1 teaspoon salt in 1 cup water) three times a day. Do not swish hard. Just tilt your head.
- Do not use mouthwash that contains alcohol.
Days 3-4: The Turnaround Point
By day three, you should notice the pain starting to decline. If it is getting worse, see the red flags section.
Pain level: Mild to moderate. You might still need pain medication, but less frequently.
What to expect:
- The swelling starts to go down.
- Bruising might appear on your face or neck. It will look yellow or purple. This is harmless and will fade.
- You can start eating soft foods like mashed potatoes, scrambled eggs, and oatmeal.
Days 5-7: Returning to Normal
Most people feel significantly better by the end of the first week. You might still have some tenderness when you touch the area, but constant pain should be gone.
Pain level: Mild. More of an awareness than actual pain.
What you can do:
- Return to work or school (if you have a desk job).
- Resume light physical activity like walking.
- Start using a soft-bristled toothbrush around the area very gently.
Important note: Do not smoke. Smoking dramatically increases pain, delays healing, and is the number one cause of implant failure. If you smoke, your pain will be worse and last longer.
Weeks 2 to 6: The Silent Healing Phase
You might think all pain should be gone by now. For most people, it is. But some patients experience what we call “silent healing” with occasional reminders.
What You Might Feel
- Intermittent sensitivity: Cold water or air might cause a brief, sharp sensation. This is normal because the gum tissue is still maturing.
- Pressure discomfort: Chewing on that side might feel strange or slightly uncomfortable. Your brain is learning that a metal post is now part of your jaw.
- Itching: Some people feel an itchy sensation deep in the bone. That is bone cells attaching to the implant surface. It is a good sign.
What You Should Not Feel
- Constant, throbbing pain.
- Pain that wakes you up.
- Pain that spreads to your ear or temple.
- A bad taste or pus coming from the site.
If you feel any of those things at week three or four, you might have peri-implantitis (an infection around the implant) or a failing osseointegration (the bone is not fusing to the implant).
Complete Pain Timeline Table (0 to 6 Months)
Here is a detailed table to guide your expectations.
| Period | Normal Sensation | Pain Level | Activities | Warning Signs |
|---|---|---|---|---|
| Day of surgery | Numbness, then dull ache | 0 then 3-6 | Rest, ice, soft food | Bleeding that won’t stop |
| Days 1-3 | Throbbing, swelling, tenderness | 3-5 | Soft diet, no exercise | Fever, spreading pain |
| Days 4-7 | Soreness, occasional sharp twinges | 1-3 | Light walking, return to desk work | Pain getting worse |
| Week 2 | Mild tenderness to touch | 0-2 | Normal activities, avoid heavy lifting | Constant throbbing |
| Weeks 3-4 | Almost none. Pressure sensitivity | 0-1 | Chew soft foods on opposite side | Bad taste, pus |
| Weeks 5-8 | None at rest. Mild with hard food | 0 | Resume normal chewing gradually | Pain with tapping on implant |
| Weeks 9-12 | None | 0 | Full chewing, but be careful | Looseness or movement |
| Months 3-6 | None | 0 | Normal function | Any pain is abnormal now |
Pain Management Strategies That Actually Work
Let us talk about practical ways to reduce your discomfort. You do not have to suffer.
Medication Options
Your dentist will likely recommend one of these approaches.
| Medication Type | Examples | Best For | Notes |
|---|---|---|---|
| Over-the-counter NSAIDs | Ibuprofen (Advil, Motrin) | Inflammation and mild to moderate pain | Take with food. Most effective for dental pain. |
| Over-the-counter analgesic | Acetaminophen (Tylenol) | Pain without inflammation | Can be taken with ibuprofen for severe pain. |
| Prescription NSAIDs | Naproxen (higher dose) | Moderate to severe pain | Short-term use only. |
| Prescription opioids | Hydrocodone, Codeine | Severe pain (rarely needed) | High risk of side effects. Use only as directed. |
A note from experienced patients: Many people find that alternating 400mg of ibuprofen with 500mg of acetaminophen every 4-6 hours works better than prescription opioids. Always confirm this with your dentist first.
Non-Medication Strategies
These methods are free, safe, and very effective.
- Ice, then heat: First 48 hours = ice. After 48 hours = warm compress.
- Head elevation: Sleep propped up for the first three nights. Gravity reduces swelling and throbbing.
- Salt water rinses: Start 24 hours after surgery. Do this 4-5 times a day. It keeps the area clean and soothes the gums.
- Distraction: Watch movies. Listen to podcasts. Read a book. The less you focus on the pain, the less you will feel it.
- Avoid vasodilators: Alcohol, caffeine, and nicotine all expand blood vessels. This increases bleeding, swelling, and pain. Avoid them for at least 72 hours.
“The best painkiller is prevention. Follow your post-op instructions like your life depends on it. Because the success of your implant does.” — Dr. Elena Vasquez, oral surgeon.
Factors That Increase Pain After Implant Placement
Not everyone experiences the same level of pain. These factors can make your recovery more uncomfortable.
1. Number of Implants
One implant causes less pain than multiple implants. A full arch of implants (like All-on-4) causes significantly more post-operative discomfort. This makes sense. More trauma equals more inflammation.
2. Bone Grafting
If your jawbone was too thin or soft, your dentist might have added bone graft material. This is a second procedure at the same site. Bone grafting almost always increases post-operative pain. Expect your pain level to be about 2 points higher on a 10-point scale compared to a simple implant.
3. Sinus Lift
For upper back teeth (molars and premolars), the sinus cavity is close to the jawbone. Some patients need a sinus lift, where the surgeon lifts the sinus membrane and places bone graft underneath. This procedure causes more deep, pressure-like pain in the cheek and under the eye.
4. Your Age and Health
Younger patients tend to heal faster and report less pain. Older patients may have a longer recovery.
Chronic conditions that increase pain risk:
- Diabetes (uncontrolled)
- Autoimmune diseases
- Osteoporosis
- Chronic pain syndromes (fibromyalgia)
5. Smoking and Vaping
We cannot say this enough. Smoking is a disaster for dental implants. It restricts blood flow to the gums and bone. This means:
- More pain after surgery.
- Pain lasts longer.
- Higher risk of infection.
- Higher risk of implant failure.
If you smoke, your pain will be worse. That is not an opinion. That is a fact from dozens of clinical studies.
When Is Pain a Sign of Implant Failure?
Let us address the fear that many patients have. What if my implant is failing?
First, know this: Implant failure is rare. The success rate for dental implants is over 95% in healthy patients. Most pain is just normal healing.
However, failure does happen. And pain is often the first sign.
Early Failure (First 3-4 months)
Early failure happens before the bone fuses to the implant. Causes include infection, overheating of the bone during surgery, or the patient grinding their teeth.
Pain symptoms of early failure:
- Pain that starts mild but progressively gets worse after week one.
- The implant feels loose or moves when you touch it with your tongue.
- You feel a dull ache that is deep, not on the surface.
- The gum around the implant looks red and bleeds easily, but no amount of cleaning helps.
Late Failure (After 4 months or after crown placement)
Late failure is almost always caused by peri-implantitis. This is a bacterial infection that destroys the bone around the implant.
Pain symptoms of late failure:
- Pain when chewing on the implant crown.
- Bleeding when you brush near the implant.
- A bad taste or smell coming from the area.
- The gum recedes, exposing the threads of the implant.
- Eventually, the implant becomes loose.
Important note: If your implant fails, do not panic. It can often be removed, the bone can heal, and a new implant can be placed. You have options.
10 Common Questions Patients Ask About Pain After Implant Placement
Let me answer the questions I hear most often.
1. Is the pain worse than a tooth extraction?
No. Most patients say implant pain is less intense than a difficult tooth extraction. The difference is that implant pain lasts longer at a low level, while extraction pain is sharp but short.
2. Can I drive myself home after surgery?
No. If you received any form of sedation (including laughing gas or oral sedatives), you cannot drive for 24 hours. Even with just local anesthesia, the pain might distract you. Have someone drive you.
3. How long do I need to take off work?
Most people take 1 to 3 days off for a single implant. For multiple implants or bone grafting, plan for 3 to 5 days. If you have a physical job, you may need a full week.
4. When can I sleep on my implant side?
Wait at least one week. Sleeping directly on the implant site puts pressure on the healing gum and bone. This can increase pain and delay healing.
5. Why does my implant hurt when I yawn?
Yawning stretches the muscles of your jaw and face. If those muscles are still inflamed from surgery, stretching hurts. This is normal and will fade by week two.
6. Can I use a heating pad on my face?
Yes, but only after 48 hours. Before that, use ice. Heat increases blood flow, which is great for healing but bad for fresh swelling.
7. Does salt water really help with pain?
Yes. Salt water creates a hypertonic environment. This means it draws fluid out of swollen tissues. It reduces inflammation and cleans the wound. It is not a painkiller, but less swelling means less pain.
8. My implant site hurts when I drink cold water. Is that normal?
For the first 4-6 weeks, yes. The gum tissue over the implant is thin and sensitive. It has not fully matured. As the gum heals and thickens, cold sensitivity will disappear.
9. When can I chew food on my implant?
You should not chew on the implant at all until your dentist gives you permission. For a single implant, this is usually 3 to 6 months. Chewing too early causes micromovement. Micromovement causes pain and implant failure.
10. My pain went away and then came back on day 10. Why?
A returning pain on day 7-14 is often a sign of a localized infection. It could also be a bone spicule (a tiny piece of dead bone working its way out). Call your dentist. Do not ignore it.
Practical Day-by-Day Recovery Checklist
Use this checklist to track your recovery.
Day 1 (Surgery Day)
- Bite on gauze for 1 hour.
- Take first pain pill before numbness wears off.
- Apply ice packs 20 on / 20 off.
- Eat only cold, soft foods.
- Do not spit, rinse, or use straws.
- Sleep with head elevated.
Day 2
- Continue ice packs (last day for ice).
- Start warm salt water rinses (3x daily).
- Take medication as needed.
- Eat warm soft foods (soup, mashed potatoes).
- Rest. Do not exercise.
Day 3
- Switch to warm compresses.
- Gently brush other teeth. Avoid the implant site.
- Pain should be decreasing. If not, call dentist.
- You can shower normally.
Day 4-7
- Swelling should be noticeably down.
- Start gentle cleaning around the implant with a soft brush.
- Return to work if you feel ready.
- Resume light walking.
Week 2
- Most pain should be gone.
- You can try soft chewable foods like pasta or scrambled eggs on the opposite side.
- See your dentist for suture removal if needed.
Week 3-4
- No pain at rest.
- You might forget you have an implant.
- Keep the area very clean. Plaque causes pain.
Special Situations: Pain After Complex Implant Cases
Not all implant surgeries are the same. Here is what to expect if you had a more complex procedure.
Immediate Implant Placement (Extraction + Implant Same Day)
When a tooth is extracted and an implant is placed immediately, pain is often more intense. Why? Because the bone socket is still healing from the extraction trauma. You are healing two wounds at once.
What to expect: Moderate to severe pain for 3-5 days. Swelling is more pronounced. You may see bruising on your face.
Advice: Be patient. This is major surgery. Take the full first week off work. Use both ice and anti-inflammatories.
Multiple Implants (3 or more)
More implants mean more drilling, more bone trauma, and more inflammation.
What to expect: You will need prescription pain medication for at least 3 days. You will have significant facial swelling. Your diet will be liquid for the first 4-5 days.
Advice: Plan for a helper. You will not want to cook or clean. Stock up on protein shakes, pudding, and broth.
Full Arch Implants (All-on-4 or All-on-6)
This is the most extensive implant procedure. Four to six implants are placed in one surgery, often with immediate temporary teeth.
What to expect: Significant pain for the first week. Swelling that makes you look unrecognizable for 2-3 days. Bruising that travels down to your neck and chest. Pain that requires opioids for 4-7 days.
Advice: This is a major operation. Treat it like one. Take two full weeks off work. Do not lift anything over 10 pounds for 10 days. Sleep sitting up for the first 5 nights.
Realistic quote from a full arch patient: “The first three days were brutal. I won’t lie. But by day seven, I turned a corner. And now, six months later, I have no pain at all and I can eat an apple. Worth it.”
The Connection Between Stress and Implant Pain
Here is something many articles do not discuss. Your mental state affects your physical pain.
When you are anxious or stressed, your body releases cortisol. Cortisol increases inflammation. Increased inflammation means more pain. It is a vicious cycle.
Practical tips to break the cycle:
- Breathe deeply. Inhale for 4 seconds, hold for 4, exhale for 6. Do this for 2 minutes whenever you feel pain spiking.
- Do not Google your symptoms. Seriously. Searching “implant pain day 5” will show you worst-case scenarios. That raises your anxiety and makes the pain feel worse.
- Trust the timeline. Remind yourself: “This pain is normal. It will improve tomorrow.”
- Talk to someone. Isolation amplifies pain. Call a friend. Ask them to distract you.
Post-Implant Pain vs. Referred Pain
Sometimes the pain you feel is not coming from the implant itself.
Referred Pain Explained
Your nerves are connected. Pain from your jaw can travel to your ear, temple, neck, or even your shoulder.
Examples:
- Pain in your ear = Often your jaw joint (TMJ) reacting to the surgery.
- Pain in your lower neck = Swelling draining down from your jaw.
- Headache on one side = Muscle tension from holding your mouth open during surgery.
The rule: Referred pain is usually dull, achy, and diffuse. It does not have a sharp, pinpoint location. It improves with rest and warm compresses.
When to worry: If the referred pain is sharp, shooting, or electric-like, you might have nerve damage. Tell your dentist immediately.
Food and Drink Guide for Pain Management
What you eat directly affects your pain level. Hard or hot foods increase pain. Soft, cold foods decrease pain.
First 3 Days (Liquid + Cold)
| Allowed | Not Allowed |
|---|---|
| Protein shakes (drink from a cup, not a straw) | Hot coffee or tea |
| Smoothie bowls (eat with a spoon) | Carbonated drinks (soda, sparkling water) |
| Yogurt | Alcohol |
| Applesauce | Any food you have to chew |
| Ice cream | Nuts, chips, crackers |
| Cold soup (gazpacho) | Spicy foods |
Days 4-7 (Soft Foods)
| Allowed | Not Allowed |
|---|---|
| Mashed potatoes | Steak or tough meat |
| Scrambled eggs | Crusty bread |
| Oatmeal | Popcorn |
| Cottage cheese | Raw vegetables |
| Cooked pasta (cut into small pieces) | Chewy candy |
| Pancakes (soft) | Pizza crust |
Week 2 and Beyond
Gradually reintroduce normal foods. Chew on the opposite side of your implant. If a food causes pain, stop eating it and try again in another week.
Complications That Cause Severe Pain
Let us be direct about the complications that cause severe, abnormal pain. This section is not meant to scare you. It is meant to help you recognize problems early.
1. Infection (Peri-Implantitis)
Pain profile: Constant, gnawing pain that gets worse over days. Often accompanied by a bad taste, bleeding, and pus.
What to do: See your dentist for antibiotics and a professional cleaning around the implant.
2. Nerve Injury
The inferior alveolar nerve runs through your lower jaw. If an implant is placed too close to it, you may feel:
- Sharp, electric shock pain when touching the area.
- Numbness or tingling in your lip, chin, or gums.
- Burning sensation.
What to do: Report any nerve symptoms immediately. Some nerve injuries heal on their own. Others require medication or even implant removal.
3. Implant Fracture (Very Rare)
The titanium post itself can crack. This causes a sudden, sharp pain when you bite down.
What to do: The implant must be removed and replaced.
4. Failed Osseointegration
The bone never attached to the implant. The implant moves slightly when you press on it. This movement irritates the bone and causes a deep, dull ache.
What to do: The implant is a failure. Remove it. Let the bone heal for 3-6 months. Then try again.
Professional Tips for a Low-Pain Recovery
These tips come from oral surgeons, periodontists, and patients who have been through the process.
Tip 1: Take your first pain pill before the numbness wears off. Do not wait for the pain to become severe. It is harder to stop severe pain than to prevent it.
Tip 2: Do not use a straw for two weeks. The suction pulls on the blood clot. A dislodged blood clot causes dry socket. Dry socket is extremely painful.
Tip 3: Do not rinse vigorously. Gently move your head from side to side. Let the salt water fall out of your mouth. Do not spit.
Tip 4: Buy a wedge pillow for sleeping. Sleeping flat increases blood flow to your head, which increases throbbing. A wedge pillow keeps you elevated comfortably.
Tip 5: Set alarms for your medication. Do not wait until the pain breaks through. Take ibuprofen around the clock for the first 48 hours, even if you feel fine.
Tip 6: Keep your mouth moist. Dry mouth increases bacterial growth and irritation. Sip water constantly. Use a humidifier in your bedroom.
The Emotional Side of Implant Pain
We focused a lot on physical pain. But dental pain also has an emotional component.
Many patients feel:
- Frustration: “Why is this taking so long?”
- Anxiety: “What if this never stops hurting?”
- Regret: “I should have just left the gap.”
These feelings are normal. Acknowledge them. Then let them go.
Remind yourself of the facts:
- Dental implants have a 95%+ success rate.
- Severe pain after implant placement is uncommon.
- Most pain resolves completely by week two.
- In one year, you will have a tooth that feels, looks, and functions like a natural tooth.
“I cried on day three. I thought I had made a huge mistake. On day thirty, I couldn’t even feel the implant. On day ninety, I ate a steak. That cry was worth it.” — Maria, actual implant patient.
Frequently Asked Questions (FAQ)
Q1: How long does pain after implant placement last on average?
A: Mild to moderate pain lasts 3-5 days. Minor soreness can last up to two weeks. Any pain beyond four weeks should be evaluated by your dentist.
Q2: Can I use over-the-counter pain relievers only?
A: Yes, for most single implants. Ibuprofen alone is often enough. For multiple implants or bone grafts, you may need a prescription for a few days.
Q3: Why is my implant throbbing at night?
A: When you lie flat, blood pressure in your head increases. This increases pulsing and throbbing. Sleep with your head elevated on two or three pillows.
Q4: Is it normal to have pain when smiling or laughing?
A: Yes, for the first week. Smiling and laughing stretch your upper lip and cheek muscles. If those muscles are near the implant site, they will pull on healing tissue.
Q5: When can I brush my implant?
A: Gently brush the area starting on day 3. Use an extra-soft toothbrush. Do not use an electric toothbrush near the implant for at least two weeks.
Q6: Can I use mouthwash?
A: Avoid alcohol-based mouthwash for two weeks. Use salt water or a chlorhexidine rinse only if your dentist prescribed it.
Q7: My pain is mild but my face is very swollen. Is that okay?
A: Yes. Swelling and pain do not always match. You can have severe swelling with mild pain, or mild swelling with severe pain. As long as pain is improving, swelling alone is not a red flag.
Q8: What is the worst day for pain?
A: For most people, day 2 is the worst. The anesthesia is completely gone. Inflammation is peaking. But you are still early in healing. By day 4, you should feel clearly better.
Q9: Can stress make my implant hurt more?
A: Absolutely. Stress increases inflammation and lowers your pain threshold. Practice deep breathing, distraction, and positive self-talk.
Q10: When should I go to the emergency room?
A: Go to the ER if you have difficulty breathing, difficulty swallowing, severe bleeding that won’t stop, or a fever over 102°F (38.9°C) that does not respond to medication.
Additional Resource
For a visual guide to post-implant recovery and step-by-step video instructions on cleaning your healing implant, visit the American Academy of Implant Dentistry’s patient education page:
https://www.aaid.com/patients/
Note: This external resource offers general educational information. Always follow the specific instructions provided by your own dentist or surgeon.
Conclusion (Three Lines Summary)
Pain after implant placement is normal for the first 3 to 7 days, but it should gradually decrease, not increase.
Manage discomfort with ice, elevation, soft foods, and over-the-counter anti-inflammatories while watching for red flags like spreading pain, fever, or a bad taste.
With proper care, your pain will resolve, and your implant will provide years of comfortable, natural function.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Every patient and every surgical procedure is unique. You should always follow the specific post-operative instructions provided by your own dentist or oral surgeon. If you have concerns about your pain or healing, contact your dental professional immediately. Do not delay seeking care based on information you read online.