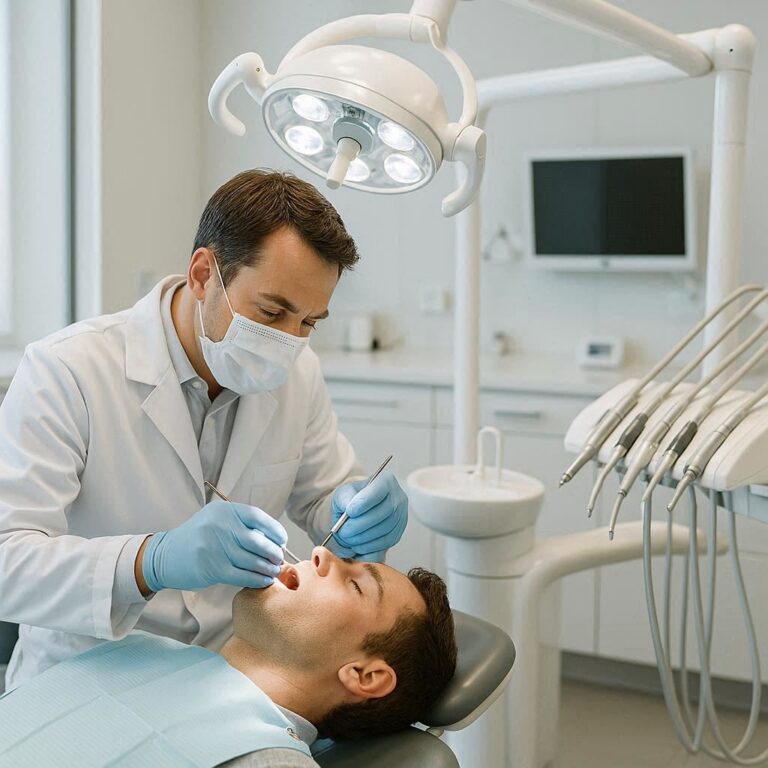
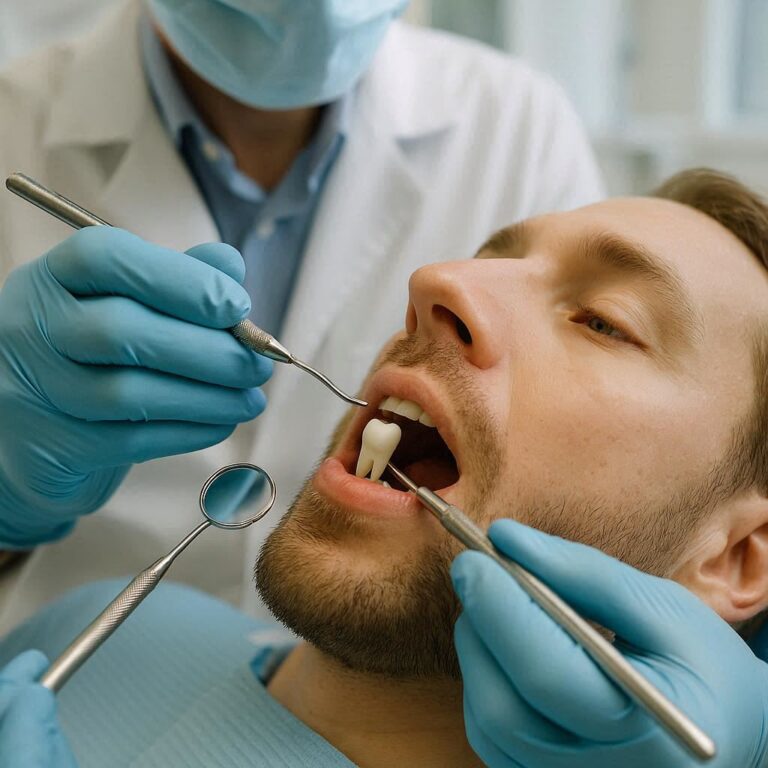
Dental Surgeon: Your Complete Guide to Diagnosis, Procedures, and Recovery
When someone mentions the words “dental surgeon,” many people immediately think of pain, drills, and long recovery times. But the truth is much less scary. A dental surgeon is a highly trained professional who helps you keep your mouth healthy, fix problems before they get worse, and even improve the way you look when you smile.
In this guide, we will walk you through everything you need to know. You will learn what a dental surgeon actually does, when you need to see one, what happens during common procedures, and how to recover quickly. No complicated medical terms. No fear tactics. Just clear, honest, and useful information.

What Is a Dental Surgeon? (And How Is Different from a Regular Dentist?)
Most people use the terms “dentist” and “dental surgeon” as if they mean the same thing. In reality, all dental surgeons are dentists, but not all dentists are dental surgeons. The difference comes down to training, credentials, and the type of procedures they perform.
A general dentist handles cleanings, fillings, crowns, and basic extractions. They are your first line of defense. But when a case becomes more complex—think impacted wisdom teeth, jaw realignment, or dental implants—a dental surgeon steps in.
The Extra Training Matters
After finishing dental school, a dental surgeon completes three to seven additional years of hospital-based surgical training. This residency focuses on:
- Anesthesia and sedation techniques
- Facial trauma surgery
- Bone grafting
- Wisdom tooth removal
- Corrective jaw surgery
- Pathology (removing tumors or cysts)
That extra training changes everything. A dental surgeon can treat problems that go beyond the teeth themselves. They work on the jawbone, facial muscles, nerves, and even the sinuses.
Important Note: In the United States, Canada, and many other countries, the official title is “Oral and Maxillofacial Surgeon.” The term “dental surgeon” is often used interchangeably by the public, but the surgical specialist is the one with advanced residency training. Always check credentials before any surgical procedure.
When Should You See a Dental Surgeon?
You do not wake up one day and decide to visit a dental surgeon for no reason. Usually, your general dentist gives you a referral. But sometimes, you notice symptoms that point directly to the need for surgical care.
Here are the most common reasons people see a dental surgeon.
Impacted Wisdom Teeth
Wisdom teeth are the last molars at the back of your mouth. They usually appear between ages 17 and 25. For many people, there is simply no room for them. When a wisdom tooth grows in at an angle or stays trapped under the gum, it becomes “impacted.” This can cause:
- Severe pain
- Swelling around the jaw
- Infection
- Damage to nearby teeth
A dental surgeon removes impacted wisdom teeth regularly. It is one of the most common surgical procedures in the world.
Dental Implants
If you lose a tooth, a bridge or denture is one option. But many people prefer implants because they look and feel like natural teeth. Placing an implant requires surgery. The surgeon drills a small hole into your jawbone and inserts a titanium post. Over time, that post fuses with the bone. Then, a dentist attaches a crown on top.
Only a trained dental surgeon or periodontist with surgical training should place implants.
Jaw Problems (TMJ Disorders)
The temporomandibular joint (TMJ) connects your jaw to your skull. When this joint does not work correctly, you may experience:
- Clicking or popping sounds
- Locked jaw
- Pain when chewing
- Headaches or earaches
Many cases of TMJ disorder improve with medication, physical therapy, or mouthguards. But severe cases may require surgery. A dental surgeon can perform arthrocentesis, arthroscopy, or even open-joint surgery to fix the problem.
Corrective Jaw Surgery (Orthognathic Surgery)
Some people are born with jaws that do not line up correctly. This can make it hard to chew, speak, or even breathe properly. Braces alone cannot fix a misaligned jawbone. In these cases, a dental surgeon cuts and repositions the jaw. The surgery sounds intense, but it is safe and common. Many patients notice dramatic improvements in both function and appearance.
Facial Trauma and Infections
Accidents happen. A fall, a car crash, or a sports injury can break your facial bones or knock out teeth. A dental surgeon repairs these injuries. They can wire jaws back together, reconstruct fractured cheekbones, and save teeth that have been pushed out of place.
Also, some dental infections spread to the neck or face. If antibiotics cannot control the infection, a surgeon may need to drain the area surgically.
Biopsies and Tumor Removal
Not all lumps in the mouth are dangerous. But some are. If your dentist finds a suspicious growth, they will refer you to a dental surgeon for a biopsy. The surgeon removes a small piece of tissue and sends it to a lab. If the growth is cancerous or precancerous, the surgeon can remove it completely.
The Most Common Procedures Explained (Step by Step)
Understanding what happens during surgery reduces fear. Let us walk through the most common procedures a dental surgeon performs. We will explain each step in plain English.
Wisdom Teeth Removal
Step 1: Consultation and X-rays
Your surgeon takes X-rays to see the position of each wisdom tooth. Impacted teeth may sit horizontally or press against nerves.
Step 2: Anesthesia
You will receive local anesthesia to numb the area. Many patients also choose sedation or general anesthesia so they sleep through the whole thing.
Step 3: The Incision
The surgeon cuts the gum tissue to expose the tooth and bone.
Step 4: Bone Removal (If Needed)
If the tooth is fully impacted, the surgeon removes a small amount of bone to access it.
Step 5: Tooth Sectioning
Large wisdom teeth are sometimes cut into smaller pieces for easier removal.
Step 6: Extraction and Cleaning
The surgeon removes the tooth pieces and cleans the socket.
Step 7: Stitches
Most surgeons use dissolvable stitches. You do not need to return to have them removed.
Step 8: Recovery
You go home the same day. Recovery takes about one week.
Dental Implant Surgery
Step 1: Initial Evaluation
The surgeon checks your bone density. If your jawbone is too thin or soft, you may need a bone graft first.
Step 2: Bone Graft (If Required)
The surgeon adds bone material to weak areas. Then, you wait several months for new bone to grow.
Step 3: Implant Placement
The surgeon makes a small cut in your gum, drills a hole in the bone, and inserts the titanium post. Then, they close the gum over the implant.
Step 4: Osseointegration
This fancy word just means “bone fusing to metal.” You wait three to six months for the implant to bond with your jawbone.
Step 5: Abutment Placement
The surgeon reopens the gum and attaches a small connector (abutment) to the implant.
Step 6: Crown Placement
Your general dentist makes a custom crown and attaches it to the abutment. Done.
Corrective Jaw Surgery
This procedure takes place in a hospital. It requires general anesthesia.
Step 1: Planning
Your surgeon works with an orthodontist. You often wear braces for 12 to 18 months before surgery.
Step 2: The Surgery
The surgeon makes small cuts in your jawbone. They move the bone into the correct position and hold it with small plates and screws.
Step 3: Recovery Room
You stay in the hospital for one to two nights.
Step 4: Healing
Swelling and numbness are normal. Most people return to work or school after two to four weeks.
Comparison Table: General Dentist vs. Dental Surgeon
| Feature | General Dentist | Dental Surgeon (Oral & Maxillofacial Surgeon) |
|---|---|---|
| Years of School After College | 4 years | 4 years dental school + 4 to 7 years residency |
| Performs Routine Cleanings | Yes | No |
| Fills Cavities | Yes | No |
| Removes Simple Wisdom Teeth | Sometimes | Always for impacted teeth |
| Places Dental Implants | Basic cases only | Complex cases and all bone grafting |
| Performs Jaw Surgery | No | Yes |
| Treats Facial Trauma | No | Yes |
| Administers Deep Sedation/General Anesthesia | Rarely | Yes, routinely |
| Removes Tumors or Cysts | No | Yes |
How to Choose the Right Dental Surgeon
Choosing a dental surgeon is a big decision. You are trusting someone to operate inside your mouth, close to your nerves, sinuses, and airway. Do not rush this process.
Check Credentials First
Look for board certification from the appropriate organization in your country. In the US, that is the American Board of Oral and Maxillofacial Surgery (ABOMS). Board certification means the surgeon has passed rigorous exams and meets high standards.
Read Patient Reviews (But Be Smart)
Online reviews help you understand a surgeon’s bedside manner and office efficiency. But remember: no surgeon pleases everyone. One or two negative reviews among hundreds of positives should not scare you away. Look for patterns. If multiple patients mention extreme pain, rude staff, or botched procedures, move on.
Ask About Experience with Your Specific Procedure
A dental surgeon who removes 200 wisdom teeth per year is very different from one who removes 20. Ask directly: “How many of these procedures do you perform each month?” Honest surgeons will answer without offense.
Consider Hospital Privileges
Even if a surgeon has an office, they should also have privileges at a local hospital. This ensures they can admit you if complications arise. It is a sign of good standing in the medical community.
Questions to Ask at Your Consultation
Write these down and bring them with you:
- What are the risks of this specific procedure for me?
- Do I need sedation or general anesthesia?
- How long will recovery take?
- What pain medications will I need?
- What is the total cost? (Ask for a written estimate.)
- What happens if something goes wrong after hours?
What to Expect Before Surgery
Preparation reduces anxiety and prevents complications. Follow these steps carefully.
Medical History Review
Your surgeon needs to know everything. That includes:
- All medications (prescription, over-the-counter, and supplements)
- Allergies (especially to latex, antibiotics, or anesthesia)
- Medical conditions (diabetes, high blood pressure, heart problems)
- Previous reactions to sedation or anesthesia
Do not hide anything. Even herbal supplements like ginkgo or garlic can increase bleeding during surgery.
Fasting Instructions
If you receive sedation or general anesthesia, you cannot eat or drink for a set number of hours before surgery. Usually, that means no food after midnight and no water for two to four hours before the procedure.
Why? If your stomach has food in it, you could vomit while sedated. That vomit could enter your lungs, causing a life-threatening condition called aspiration pneumonia. These rules exist to keep you safe.
Arrange a Ride
You cannot drive yourself home after sedation or general anesthesia. The drugs stay in your system for hours. You may feel fine, but your reaction time is dangerously slow. Arrange for a trusted friend or family member to drive you to and from the appointment.
Set Up Your Recovery Space at Home
Before your surgery, prepare your home. You will thank yourself later.
- Stock soft foods (yogurt, pudding, applesauce, soup, mashed potatoes)
- Fill ice packs and put them in the freezer
- Place pillows on your bed or couch to keep your head elevated
- Fill any pain prescriptions ahead of time
- Plan time off work or school (at least one to three days for simple extractions, longer for major surgery)
Recovery: A Day-by-Day Guide
Recovery looks different for everyone. Age, overall health, and the type of surgery all play a role. But here is a general timeline for common procedures like wisdom tooth removal or implant placement.
Day of Surgery
You go home with gauze pads in your mouth. Change them when they become soaked with blood. Most bleeding stops within four hours.
Keep your head elevated. Apply ice packs to your face for 20 minutes on, then 20 minutes off. This reduces swelling.
Eat only cold, soft foods. Drink plenty of water but do not use a straw. Sucking on a straw can dislodge the blood clot that forms in the socket, leading to a painful condition called dry socket.
Do not rinse your mouth, spit forcefully, or smoke. Smoking dramatically increases the risk of infection and dry socket.
Day 2 and 3
Swelling peaks around day two or three. Your face may look puffy. This is normal.
Switch from ice to warm compresses. Warmth increases blood flow and helps with healing.
You may start gently rinsing your mouth with warm salt water (one teaspoon of salt in a cup of warm water). Do not swish hard. Just tilt your head side to side.
Stick to soft foods. Avoid anything crunchy, spicy, or hot.
Days 4 to 7
Swelling goes down. Pain decreases. You can slowly add semi-soft foods like scrambled eggs, pasta, or soft bread.
Most people return to work or school by day four or five. But everyone heals differently. Listen to your body.
Keep cleaning the area gently. Your surgeon may give you a curved syringe to flush out food particles from the extraction site.
Week 2 and Beyond
By the second week, most patients feel close to normal. You can resume normal eating, exercise, and activities. However, avoid contact sports for at least four weeks if you had bone work or implants.
If you had jaw surgery, expect a longer recovery. You may be on a liquid or soft diet for six weeks. Full healing takes three to six months.
Warning Signs: When to Call Your Surgeon
Most surgeries go smoothly. But complications can happen. Call your dental surgeon immediately if you experience:
- Bleeding that soaks through more than one gauze pad per hour after the first 24 hours
- Severe pain that does not improve with prescribed medication
- Swelling that gets worse after day three instead of better
- Fever over 101°F (38.3°C)
- Pus or foul drainage from the surgical site
- Difficulty breathing or swallowing
- Numbness that lasts beyond 24 hours (some numbness is normal, but prolonged numbness may indicate nerve injury)
- Blood or unusual color when you cough or blow your nose (after upper wisdom tooth removal)
Do not wait for these symptoms to go away on their own. Infection can spread quickly in the head and neck. A phone call could save you from a hospital stay.
Costs and Insurance: What You Need to Know
Dental surgery costs vary widely based on your location, the surgeon’s experience, and the complexity of your case. Let us look at realistic numbers.
Average Costs in the United States (Without Insurance)
| Procedure | Typical Cost Range |
|---|---|
| Simple wisdom tooth extraction (one tooth, fully erupted) | $150 – $400 |
| Impacted wisdom tooth extraction (one tooth) | $300 – $1,000 |
| Four impacted wisdom teeth (with IV sedation) | $1,500 – $4,000 |
| Single dental implant (post only) | $1,500 – $3,000 |
| Implant with crown (complete) | $3,000 – $6,000 |
| Bone graft | $500 – $1,500 |
| Corrective jaw surgery (one jaw) | $15,000 – $25,000 |
| Corrective jaw surgery (both jaws) | $30,000 – $40,000 |
Does Insurance Cover Dental Surgery?
It depends on the reason for the surgery.
- Medical insurance covers procedures deemed medically necessary. Examples include jaw surgery for breathing problems, tumor removal, and trauma repair.
- Dental insurance covers procedures for tooth-related problems. Examples include wisdom teeth removal and dental implants.
Always call both your medical and dental insurance companies before scheduling surgery. Ask specifically: “Is this procedure covered? What is my out-of-pocket cost? Do you require a pre-authorization?”
Important Note: Many dental surgeons have financial coordinators on staff. These employees help you understand your benefits and set up payment plans. Ask for their help. It is part of their job.
Sedation and Anesthesia: Your Options Explained
Fear of pain or being “put to sleep” stops many people from getting needed surgery. Understanding your options can put your mind at ease.
Local Anesthesia
You stay fully awake. The surgeon injects numbing medicine into the area. You will feel pressure and movement but no sharp pain.
Best for: Single, simple extractions or minor procedures.
Nitrous Oxide (Laughing Gas)
You breathe gas through a mask. It makes you feel relaxed and slightly giggly. The effect wears off immediately when the mask is removed. You can drive yourself home afterward.
Best for: Mild anxiety during simple procedures.
Oral Sedation
You take a pill (usually a benzodiazepine like Valium or Halcion) about an hour before surgery. You remain conscious but very drowsy. Many patients fall asleep and remember little to nothing.
Best for: Moderate anxiety. You need a ride home.
IV Sedation (Twilight Sleep)
The surgeon gives sedative drugs through a small tube in your vein. You enter a state of deep relaxation. You breathe on your own but are not fully conscious. Most patients have no memory of the procedure.
Best for: Impacted wisdom teeth, multiple implants, or very anxious patients. You need a ride home.
General Anesthesia
You are completely unconscious. A breathing tube may be placed. An anesthesiologist or nurse anesthetist monitors your vital signs throughout.
Best for: Major jaw surgery, facial trauma, or long, complex procedures. Requires hospital or surgical center. You need a ride home.
How to Reduce Anxiety Before Dental Surgery
Even adults with high pain tolerances can feel terrified of dental surgery. That fear is normal. Here are proven strategies to calm your nerves.
Talk to Your Surgeon Honestly
Say the words out loud: “I am scared.” A good surgeon will not judge you. They hear this every day. Together, you can create a plan that may include:
- Prescribing an anti-anxiety pill for the night before
- Arranging for you to listen to music during the procedure
- Using more sedation than usual
- Scheduling a “pre-visit” just to look around and meet the staff
Bring a Support Person
Having a trusted friend or family member in the waiting room lowers stress. You know someone is there for you when you wake up.
Use Distraction Techniques
Bring headphones and play calming music or a podcast during local anesthesia procedures. Some patients watch movies on tablets. Focus on something pleasant rather than the sounds of the room.
Practice Deep Breathing
Slow, deep breaths activate your parasympathetic nervous system. That is the “rest and digest” mode. Try this: inhale for four seconds, hold for four seconds, exhale for six seconds. Repeat five times before walking into the office.
Remember: The Anticipation Is Worse Than Reality
Thousands of studies confirm that humans fear uncertainty more than pain itself. The waiting before surgery feels awful. The actual procedure? Most patients describe it as “not nearly as bad as I expected.”
Long-Term Care After Dental Surgery
Surgery is just one step. What you do afterward determines your long-term success. Follow these guidelines.
For Extractions
After a tooth is removed, the nearby bone shrinks over time. This can cause neighboring teeth to shift. Talk to your surgeon about replacement options if the extracted tooth is visible when you smile.
For Implants
Implants require the same care as natural teeth. Brush twice daily, floss once daily, and visit your general dentist every six months. Neglected implants can develop peri-implantitis, an infection that destroys bone and causes implant failure.
For Jaw Surgery
After corrective jaw surgery, you will likely wear braces or clear aligners for several more months. Wear your retainers as instructed. Your bite can relapse if you skip your retainer.
General Oral Health Tips
- Stop smoking. Smokers have dramatically higher rates of implant failure, dry socket, and surgical infections.
- Control your blood sugar. Diabetics heal more slowly. Well-controlled diabetes is safe; poorly controlled diabetes increases risks.
- Take calcium and vitamin D. Strong bones support dental work.
Frequently Asked Questions (FAQ)
Is a dental surgeon the same as an oral surgeon?
Yes. In most countries, “dental surgeon” is a general term that can refer to any dentist. However, for surgical procedures beyond simple extractions, you want an Oral and Maxillofacial Surgeon. That is the specialist with additional years of hospital-based training.
Does dental surgery hurt?
During the procedure, no. You will receive anesthesia or sedation. Afterward, you will have some pain and swelling. But prescription or over-the-counter pain medication manages this effectively. Most patients describe the discomfort as “annoying” rather than “excruciating.”
How long does it take to recover from wisdom teeth removal?
Most people return to school or desk jobs within three to five days. Full healing of the bone takes several weeks, but you will feel normal after one to two weeks.
Can I eat normally after dental implants?
You will eat soft foods for about one week after implant placement. Once the crown is attached (months later), you can eat normally, including steak, apples, and nuts. Implants are incredibly strong.
Is jaw surgery worth it?
For people with severe bite problems, chronic pain, or difficulty chewing: yes, absolutely. Many patients report that jaw surgery changed their lives. But understand the recovery is long. You will need several weeks off work and a liquid diet. Weigh the benefits against the temporary challenges.
What is the success rate of dental implants?
Over 95% for lower jaw implants and over 90% for upper jaw implants. Success depends on your bone quality, oral hygiene, and whether you smoke.
How do I find a good dental surgeon near me?
Start with your general dentist’s referral. Then, check the American Board of Oral and Maxillofacial Surgery (ABOMS) website for board-certified surgeons in your area. Read reviews, but take them with a grain of salt. Finally, schedule two consultations and compare your comfort levels.
Will my insurance cover wisdom tooth removal?
Most dental insurance plans cover a portion of wisdom tooth removal, especially if the teeth are impacted. Call your insurance company before your consultation to understand your benefits.
Can a dental surgeon perform a root canal?
No. Root canals are performed by general dentists or endodontists (root canal specialists). A dental surgeon focuses on extractions, implants, bone grafts, jaw surgery, and facial trauma.
What should I do if I have a dental emergency after hours?
Most dental surgeons have an on-call number for emergencies. Call their office number and listen for instructions. If you cannot reach anyone and you have difficulty breathing, severe uncontrolled bleeding, or eye swelling that closes your eye, go to the nearest emergency room.
Additional Resources
For more information, visit the American Association of Oral and Maxillofacial Surgeons (AAOMS) patient education section:
Link: https://myoms.org
This website offers procedure guides, animations, and patient stories you can trust.
Conclusion
A dental surgeon does much more than pull teeth. These specialists treat infections, repair facial injuries, replace missing teeth with implants, and correct jaw problems that affect breathing and eating. While the idea of oral surgery makes many people nervous, modern anesthesia and sedation make procedures comfortable and safe. By choosing a qualified surgeon, preparing properly, and following recovery instructions, you can get the care you need without unnecessary fear or pain. Your smile—and your overall health—will thank you.
Disclaimer: This article provides general information and does not constitute medical advice. Every patient and procedure is unique. Always consult with a licensed dental surgeon or physician before making decisions about your health.