what can i do if my dental implant falls out
You rinse your mouth, feel something hard against your tongue, and your heart sinks. It is your dental implant. Or part of it. This moment can feel alarming, but here is the truth you need to hear: you are not alone, and this is not a disaster.
Dental implants fail or become dislodged for many reasons. Some are simple to fix. Others require more planning. What matters most is what you do in the first few minutes after you notice the problem.
This guide walks you through every realistic scenario, from a loose crown to a full implant body coming out. You will learn the exact steps to protect your health, save money, and get your smile back.
No medical jargon. No panic. Just honest, useful information from a professional perspective.
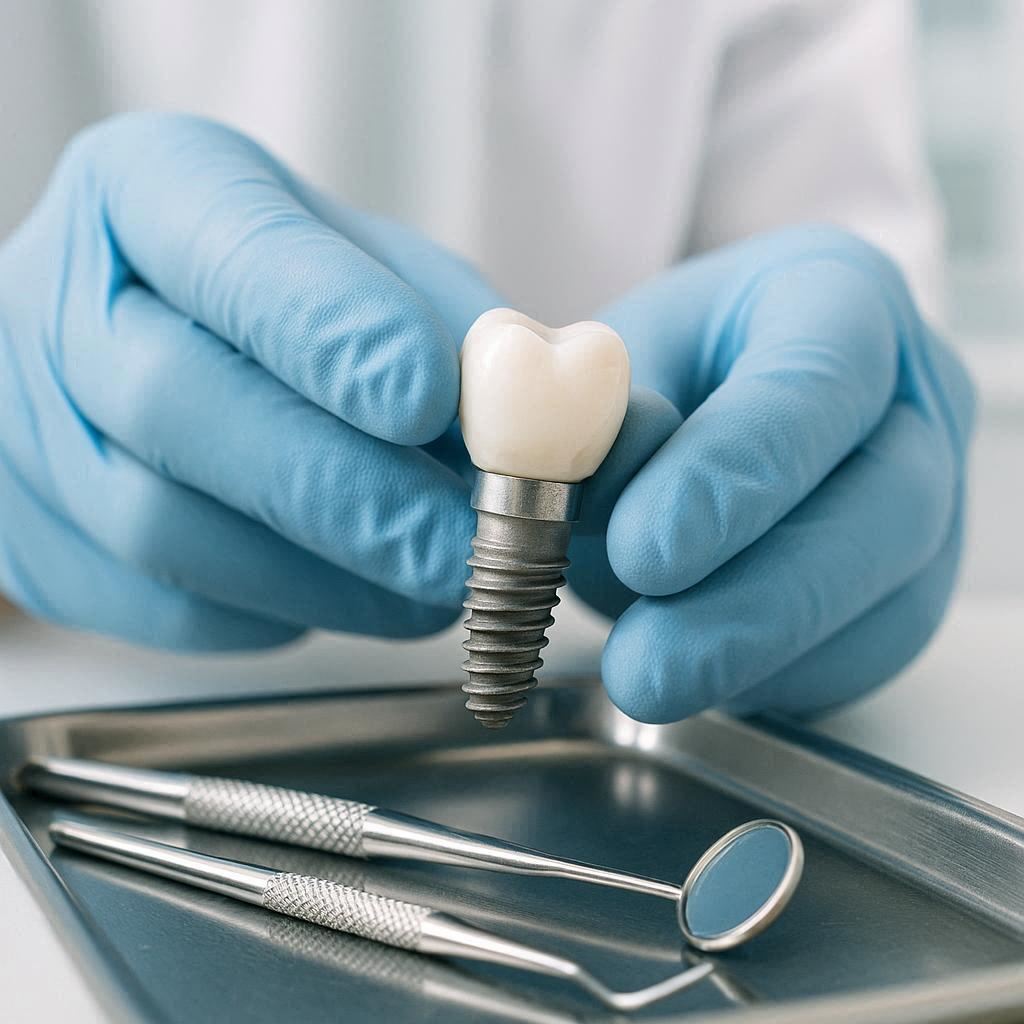
Understanding What Just Happened: Implant or Crown?
Before you do anything, take a slow breath. Then look at what came out. This sounds simple, but many people mistake one part for another.
A dental implant system has three main pieces:
- The implant fixture: The screw-like post placed into your jawbone. This acts as your new tooth root.
- The abutment: A connector piece that attaches to the implant and sticks above the gum line.
- The crown: The visible, tooth-shaped part that you see when you smile.
When something “falls out,” you might have lost only the crown. Or the crown and abutment together. In rarer cases, the entire implant fixture comes out.
Important note: A true implant failure—where the screw-like post falls out of your jaw—is much less common than a loose crown. Most panicked calls to dental offices turn out to be cement or screw-retained crowns that simply detached.
Quick Identification Guide
| What you see | What likely happened | Urgency level |
|---|---|---|
| Hollow tooth-shaped cap | Crown came off abutment | Moderate |
| Small metal piece with screw threads | Abutment + crown detached | Moderate to high |
| Long metal screw with threads | Entire implant fixture fell out | High |
| Tiny metal fragment | Part of abutment or screw broke | High |
Look at the piece under good light. If you see a hollow cap with no metal inside, relax slightly. If you see a long threaded post that looks like a screw for wood or metal, call your dentist immediately.
Step One: Stay Calm and Retrieve the Piece
Panic leads to mistakes. You might accidentally swallow the implant or throw it away. Here is what to do in order.
- Spit gently into a tissue or small bowl. Do not swallow. If you already swallowed the piece, do not induce vomiting. Most implant components pass safely, but you should still call your dentist.
- Rinse the fallen piece with cool water. Use tap water only. No soap, alcohol, or harsh cleaners. Gently remove any visible debris.
- Place it in a clean, dry container. A pill bottle, small glass jar, or zip-top bag works perfectly. Add a slightly damp piece of cotton ball to keep the crown from drying out if it has a temporary cement layer.
- Label the container with the date and time. This seems excessive, but it helps your dentist understand the situation.
Do not scrub the piece. Do not soak it in mouthwash, bleach, or hydrogen peroxide. These chemicals can damage the surface and make re-cementation or reattachment impossible.
What if you cannot find the piece?
Sometimes the implant or crown falls out while eating, sleeping, or brushing. If you cannot locate it, do not dig around your mouth with tools. Instead:
- Check the sink drain trap.
- Look on the floor near where you were standing.
- Search your bedding if it happened overnight.
If you still cannot find it, tell your dentist. They can take an X-ray to confirm whether the piece is lodged somewhere in your mouth or if it simply went down the drain.
Step Two: Inspect Your Mouth Gently
After retrieving the piece, you need to check the area where the implant used to be. Wash your hands thoroughly. Then use a clean finger or the handle of a clean spoon to gently feel the gum tissue.
What to look for:
- A visible hole in the gum where the implant sat
- Bleeding (light oozing is normal, gushing is not)
- Swelling or redness
- Exposed bone (rare, but possible)
- A small metal post still sticking out of the gum
If you see a metal post still in your gum, your implant fixture remains in the bone. Only the abutment and crown fell off. This is good news. Your dentist can usually screw everything back together in one short appointment.
If you see only a gum-colored or pink dimple with no metal, either the abutment or the entire implant came out. This requires a more careful evaluation.
Do not push anything back into the hole yourself. You could introduce bacteria deep into the bone or push the wrong piece into the wrong space.
Controlling bleeding and discomfort
Minor bleeding is common. Roll a clean piece of gauze or a damp tea bag into a small ball. Place it directly over the extraction site (where the implant fell from). Bite down gently but firmly for 15 to 20 minutes.
For pain, over-the-counter options work well:
| Medication | Typical dose | Note |
|---|---|---|
| Ibuprofen (Advil, Motrin) | 400-600 mg | Reduces inflammation best |
| Acetaminophen (Tylenol) | 500-1000 mg | No anti-inflammatory effect |
| Naproxen (Aleve) | 220-440 mg | Longer lasting |
Avoid aspirin if you have active bleeding, as it thins the blood. Never place aspirin directly on your gum. This causes chemical burns.
Step Three: Protect the Site Until You See a Dentist
You cannot always see your dentist the same day. Weekends, holidays, and after-hours emergencies happen. Here is how to manage until your appointment.
Eating and drinking
- Stick to soft, lukewarm or cold foods: yogurt, applesauce, smoothies, mashed potatoes, scrambled eggs, soup (cooled down)
- Avoid anything hot, crunchy, hard, sticky, or spicy
- Chew only on the opposite side of your mouth
- Drink through a straw only if your dentist approved it previously (some implant sites heal better without straw suction)
Oral hygiene
Keeping the area clean prevents infection. But you must be gentle.
- Rinse with warm salt water (1 teaspoon of salt in 8 oz of warm water) after every meal
- Do not spit forcefully. Let the water fall out of your mouth.
- Brush your other teeth normally, but avoid the exposed implant site
- Do not use water flossers, toothpicks, or any pointed object near the hole
Temporary cover (only if necessary)
Some people feel anxious about an open hole in their gum. If you absolutely must cover it (for a job interview, a special event, etc.), use only dental wax or sugar-free gum pressed gently over the area. Remove it before eating or sleeping.
Never use:
- Super glue
- Household cement
- Denture adhesive (unless your dentist specifically told you to)
- Cotton balls (fibers get stuck in the healing tissue)
These DIY “fixes” almost always cause more harm than good.
Step Four: Call Your Dentist the Right Way
When you call your dental office, the front desk needs clear information to prioritize your appointment. Say something like this:
“I have a dental implant that fell out. The piece is [describe it: crown only / abutment and crown / the whole screw]. There is [little / moderate / heavy] bleeding. I am not in severe pain, but I want to be seen as soon as possible.”
If the office is closed, listen to the voicemail instructions. Many dentists have an after-hours emergency number. If they do not, call a local emergency dental clinic.
Do you need an emergency room?
Most fallen implants are not true medical emergencies. However, go to an ER if you experience:
- Bleeding that will not stop after 30 minutes of firm pressure
- Difficulty breathing or swallowing
- Swelling that spreads to your eye or neck
- Fever over 101°F (38.3°C)
- Severe pain that does not respond to over-the-counter medication
The ER cannot reattach your implant. But they can control severe bleeding, prescribe antibiotics, and rule out dangerous infections.
Why Do Dental Implants Fall Out?
Understanding the cause prevents the same problem from happening again. Implants fail for different reasons depending on when the failure occurs.
Early failure (within the first 3-6 months after placement)
This usually means the implant never fused properly with your jawbone. The medical term is “failed osseointegration.”
Common causes:
- Smoking or nicotine use (vaping counts too)
- Poor bone quality or quantity
- Infection at the time of surgery
- Overheating the bone during drilling
- Loading the implant with a crown too soon
- Uncontrolled diabetes or autoimmune conditions
Late failure (months or years after successful integration)
When an implant functions well for a year or more and then falls out, the cause is usually different.
Peri-implantitis is the number one culprit. This is like gum disease but around an implant. Bacteria accumulate under the gum line, destroy bone, and loosen the implant.
Other late failure causes:
- Bruxism (teeth grinding or clenching)
- Poor oral hygiene over many months
- Ill-fitting crown that traps food and plaque
- Trauma (punch, fall, car accident)
- Allergic reaction to titanium (extremely rare, but possible)
Mechanical failures
Sometimes the implant fixture stays solidly in the bone, but a small screw breaks. Or the abutment fractures. These are not implant failures in the strict sense. They are hardware failures. And they are usually much easier to fix.
| Failure type | Likelihood | Fix complexity |
|---|---|---|
| Loose crown cement | Common | Low |
| Broken abutment screw | Moderate | Moderate |
| Fractured crown | Common | Low to moderate |
| Failed implant fixture | Uncommon | High |
| Broken implant driver tool | Rare | Moderate |
Can You Save and Reuse the Same Implant?
This is the question everyone wants answered. And the answer depends entirely on what fell out.
Scenario A: Only the crown fell off
Yes. Your dentist can usually clean the crown and re-cement it or replace the screw. This takes 15 to 30 minutes. The cost is minimal (often just an office visit fee).
Scenario B: The abutment and crown fell off together
Often yes. The abutment may need a new screw, but the crown can be reattached. Your dentist will check if the abutment is damaged. If not, they screw everything back in place.
Scenario C: The entire implant fixture came out of your jaw
No. Once a titanium implant loses its integration with bone, you cannot simply push it back in. The bone around the failed implant is either infected, weakened, or never grew properly. Reusing the same implant would almost guarantee another failure.
Your dentist will recommend one of three paths:
- Let the bone heal for 3 to 6 months, then place a new implant
- Bone grafting followed by a new implant after healing
- A different restoration like a dental bridge or partial denture
Scenario D: A piece of the implant broke off inside your jaw
This is the most complex situation. Your dentist will need a CBCT (3D X-ray) to locate the fragment. Removing it may require a minor surgical procedure. You cannot reuse the broken implant.
Hard truth: Many patients ask to keep their failed implant as a souvenir. Dentists almost always say no. Used implants cannot be sterilized and re-sterilized to surgical standards. They go into medical waste disposal.
What Your Dentist Will Do at Your Appointment
Knowing what to expect reduces anxiety. The steps vary, but here is a typical sequence.
Step 1: Examination and X-ray
Your dentist will look at the site, then take a periapical X-ray (small, focused image) or a panoramic X-ray. This shows:
- Whether any implant fragments remain in the bone
- The amount of bone loss around the site
- The condition of adjacent teeth
Step 2: Cleaning the area
The socket (hole) where the implant sat must be cleaned of infected tissue and debris. Your dentist uses sterile saline and special curettes. You will receive local anesthetic for this.
Step 3: Decision time
Based on what they see, your dentist will present options:
For loose crown only: Clean, dry, and re-cement or re-screw. Done.
For failed abutment screw: Remove broken screw fragment (if any), replace screw, torque to proper value. Done.
For failed implant fixture: Discuss bone grafting and replacement timeline. No immediate fix.
Step 4: Immediate protection
If you cannot get a new implant right away, your dentist may place a:
- Healing abutment (a small metal cap that shapes the gum)
- Temporary partial denture (a removable fake tooth)
- Resin-bonded bridge (a fake tooth attached to neighboring teeth)
These protect the space and keep adjacent teeth from shifting.
Treatment Options After an Implant Falls Out
One failed implant does not mean you cannot have another successful one. In fact, most people are excellent candidates for a second attempt. Here are your realistic options.
Option 1: New implant after bone healing
This is the gold standard. You wait 3 to 6 months for the bone to fill in the socket. Then a surgeon places a new implant. The success rate for second implants in the same site is over 90% when the original cause of failure is addressed.
Pros: Permanent, feels like a natural tooth, preserves bone
Cons: More expensive than a bridge, requires surgery again, longer timeline
Option 2: Bone graft followed by implant
If you lost significant bone after the first implant failed, you will need a graft. The surgeon places donor bone (human, cow, or synthetic) into the socket. You wait 4 to 9 months for new bone to grow. Then you get the implant.
Pros: Restores lost bone, makes future implant possible
Cons: Adds time (often 6-12 months total) and cost ($500-$3,000 for graft alone)
Option 3: Dental bridge
A bridge uses the two teeth next to the gap as anchors. Your dentist shaves down those teeth and connects three crowns together.
Pros: No surgery, faster (3-4 weeks total), often covered by insurance
Cons: Requires damaging healthy teeth, does not preserve bone, needs replacement every 10-15 years
Option 4: Partial denture
A removable false tooth (or teeth) that clips onto adjacent teeth.
Pros: Least expensive option, non-invasive
Cons: Less stable, can be uncomfortable, may accelerate bone loss, requires removal for cleaning
Comparison table for long-term solutions
| Feature | New implant | Bone graft + implant | Dental bridge | Partial denture |
|---|---|---|---|---|
| Preserves bone | Yes | Yes | No | No |
| Affects adjacent teeth | No | No | Yes | Minimal |
| Average lifespan | 20+ years | 20+ years | 10-15 years | 5-8 years |
| Typical cost | $3,000-$5,000 | $4,000-$8,000 | $2,000-$4,000 | $500-$2,000 |
| Surgery required | Yes | Yes (twice) | No | No |
| Feels like natural tooth | Yes | Yes | Moderate | No |
How to Prevent an Implant From Falling Out Again
Prevention is not complicated. But it does require daily discipline. Most people who lose an implant later succeed with a second one because they change their habits.
Daily home care (non-negotiable)
- Brush twice daily with a soft-bristled brush. Pay special attention to the gum line around your implant.
- Floss every single day. Use implant-specific floss or super floss with a stiff end to thread under the crown.
- Use a water flosser on low setting to flush out bacteria from under the gum line. Do this before bed.
- Avoid abrasive toothpaste. No whitening pastes, baking soda, or charcoal products. These scratch the crown surface and allow bacteria to stick.
Professional maintenance
Your dentist or hygienist needs to see your implant just like they check your natural teeth.
- Recall visits every 6 months (every 3-4 months if you have a history of gum disease)
- Peri-implant probing once a year to measure gum pockets around the implant
- X-rays every 12-24 months to check bone levels
Lifestyle changes
| Risk factor | How it affects implants | What to change |
|---|---|---|
| Smoking | Reduces blood flow, increases infection risk 3x | Quit or switch to nicotine replacement therapy |
| Grinding/clenching | Overloads the implant, loosens screws | Nightguard worn during sleep |
| Poorly controlled diabetes | Slows healing, increases infection | Work with your doctor on blood sugar control |
| Frequent sugary snacks | Feeds bacteria that cause peri-implantitis | Reduce frequency, rinse with water after eating |
A note on nightguards: If you grind your teeth, a custom nightguard from your dentist is not optional. Over-the-counter boil-and-bite guards often make grinding worse. Invest in the professional version. It costs $300-$600 but protects an implant that cost you thousands.
When to Seek a Second Opinion
Dentists have different skill levels and treatment philosophies. You should absolutely get a second opinion if:
- Your dentist wants to extract the failed implant and immediately place a new one in the same appointment (this almost never works)
- You are told you have no options except a bridge or denture
- The recommended treatment plan seems rushed or vague
- You feel pressured to decide on the spot
A good second opinion comes from either:
- A prosthodontist (implant restoration specialist)
- An oral surgeon (implant surgery specialist)
- A periodontist (gum and bone specialist)
Ask for copies of your X-rays before the second visit. Most dental offices will email them to you or put them on a USB drive at no charge.
Costs and Insurance: What to Expect Realistically
Money is a real concern. Let me be direct about numbers. Prices vary widely by region (urban vs rural, US vs other countries), but these are realistic U.S. averages without insurance.
Cost to fix a fallen implant by scenario
| Situation | Typical cost | Insurance coverage |
|---|---|---|
| Re-cement loose crown | $75 – $200 | Often covered (diagnostic code) |
| Replace broken abutment screw | $150 – $400 | Usually covered partially |
| New crown (if old one broke) | $800 – $2,500 | Varies by plan |
| Remove failed implant fixture | $300 – $800 | Often covered as surgery |
| Bone graft after failure | $500 – $3,000 | Rarely covered |
| New implant placement | $1,500 – $3,000 (just the implant) | Usually not covered |
| New implant + crown | $3,000 – $5,000 total | Rarely covered |
Does dental insurance help?
Most dental insurance plans specifically exclude implants. Or they cover only a small portion (10-20%). However, they often cover:
- The extraction or removal of a failed implant (under “oral surgery”)
- Diagnostic X-rays and exams
- A temporary partial denture (under “prosthodontics”)
- Treatment for peri-implantitis (under “periodontics”)
Read your policy carefully. Some plans have a “missing tooth clause” that excludes coverage for any tooth that was missing before the policy started. This includes implant failures.
Financing options
If you need a new implant but cannot pay all at once:
- CareCredit (medical credit card with 6-12 month no-interest plans)
- In-office payment plans (ask your dentist directly)
- Dental school clinics (50-70% lower fees, supervised by experienced faculty)
- Clinical trials (search clinicaltrials.gov for implant studies in your area)
Common Myths About Fallen Implants
Let me clear up some dangerous misinformation that circulates online.
Myth 1: “You can push the implant back in yourself.”
Truth: Absolutely not. You will push bacteria deep into the bone and likely push it in crooked. This turns a salvageable situation into a surgical nightmare.
Myth 2: “If an implant falls out, you can never get another one.”
Truth: False. Most people are candidates for a second implant after proper healing. Success rates for second attempts are excellent—often over 90% when the original problem is corrected.
Myth 3: “Implants last forever.”
Truth: They can last 20, 30, even 40 years. But “can” is not “will.” Implants require the same care as natural teeth. Neglect leads to failure.
Myth 4: “Titanium allergies are common.”
Truth: True titanium allergy affects less than 0.6% of the population. Most people who suspect an allergy actually have peri-implantitis (infection) or a reaction to the crown material (like nickel in cheap metal crowns).
Myth 5: “You should never fly after an implant falls out.”
Truth: Flying is perfectly safe. Cabin pressure changes will not affect the failed site. However, if you need emergency dental care, do not fly to another country expecting cheap treatment. That often backfires.
Frequently Asked Questions (FAQ)
1. Is a dental implant falling out an emergency?
Not usually a medical emergency, but it is a dental urgency. You should see a dentist within 24-48 hours. If you have uncontrollable bleeding, severe pain, or signs of infection (fever, spreading swelling), go to an ER.
2. Can I eat with a missing implant?
Yes, but stick to soft foods on the opposite side. Avoid anything crunchy, sticky, or hard until your dentist evaluates you. Do not let food pack into the open socket.
3. Will my insurance cover a replacement implant?
Most plans do not. However, some cover the crown portion or the surgical removal of the failed implant. Call your insurance company directly and ask for the “implant replacement” clause.
4. How long do I have to wait before getting a new implant?
If the fixture fell out: usually 3-6 months for bone to heal. If only the crown fell off: no wait time—it can be reattached immediately. If you had peri-implantitis: 4-9 months after bone grafting.
5. Can a fallen implant damage my other teeth?
It can. If you leave the gap open for many months, adjacent teeth may drift into the space. This causes bite problems and makes future implant placement more difficult. Do not wait longer than 3-6 months to replace it.
6. Why does my implant smell bad after falling out?
Bacteria accumulate under failed crowns and around loose implants. The smell is from anaerobic bacteria producing sulfur compounds. This is a sign of infection. Rinse with salt water and see your dentist.
7. Can I superglue my crown back on myself?
Never. Superglue is toxic to gum tissue, and you will glue the crown on crooked. Your dentist has medical-grade cement that is safe and reversible.
8. What if I swallowed my implant?
Most swallowed dental objects pass through the digestive system in 24-72 hours without problems. Eat high-fiber foods (bread, bananas, oatmeal) to help it move. If you develop chest pain, vomiting, or severe abdominal pain, go to an ER.
9. Does vaping cause implant failure?
Yes. Nicotine constricts blood vessels regardless of whether you inhale smoke or vapor. Vaping also heats the mouth, and some flavor chemicals irritate gum tissue. For implant success, zero nicotine is best.
10. Can I get an MRI after my implant falls out?
Yes, if the entire implant is out. If a metal fragment remains, tell the MRI technician. Titanium is generally MRI-safe, but fragments can heat up or move. Always disclose your full dental history before any MRI.
Realistic Timeline: From Fallout to New Smile
To help you plan, here is a realistic timeline for each common path.
Path 1: Only crown fell off (simplest)
- Day 1: Crown falls out. You call dentist.
- Day 2-3: Appointment. Dentist cleans and reattaches crown.
- Done. Total time: 48 hours.
Path 2: Failed abutment screw
- Day 1: Crown and abutment fall out.
- Day 3: Appointment. Dentist removes broken screw (if any), places new screw, reattaches crown.
- Done. Total time: a few days.
Path 3: Entire implant fixture failed (no bone graft needed)
- Day 1: Implant falls out. Call dentist.
- Day 3-7: Removal appointment (if any fragments remain). Cleaning of socket.
- Month 1-4: Healing period. You wear a temporary partial denture or leave the gap.
- Month 4: CBCT scan to confirm bone healing.
- Month 4-5: New implant placement surgery.
- Month 8-10: Osseointegration healing (implant fuses to bone).
- Month 10: Abutment placement.
- Month 11: Crown delivery.
- Total time: 10-12 months.
Path 4: Failed implant with bone graft needed
- Day 1: Implant falls out.
- Week 1: Removal and bone graft placement (same appointment often).
- Month 4-9: Graft heals and matures.
- Month 9: New implant placement.
- Month 12-15: Osseointegration.
- Month 15-16: Abutment and crown.
- Total time: 12-18 months.
Perspective: Yes, a year sounds like a long time. But compare that to living 30 years with a poorly fitting denture or a bridge that damages healthy teeth. The waiting period is an investment in decades of comfort.
Additional Resource
For a detailed, dentist-reviewed library of implant aftercare instructions, troubleshooting guides, and a search tool to find implant specialists in your area, visit:
🔗 American Academy of Implant Dentistry (AAID) Patient Resources
[https://www.aaid.com/patients/index.html]
This resource includes:
- A “Find an Implant Dentist” search by zip code
- Downloadable implant home care guides
- Videos explaining implant failure and repair
- Cost estimator tools
Final Disclaimer
This article provides general educational information and does not constitute medical or dental advice. Every person’s oral health situation is unique. Do not use this article as a substitute for a professional examination, diagnosis, or treatment plan. Always consult a licensed dentist or oral surgeon for any dental emergency or concern. The author and publisher disclaim any liability for any adverse effects arising from the use or application of the information contained here.
Conclusion
If your dental implant falls out, stay calm, retrieve the piece, and call your dentist within 24 hours. Most cases are simple crown recementing or screw replacement, not catastrophic failures. With proper care and professional guidance, you can almost always restore your smile successfully, whether through a simple repair or a well-planned second implant.


