What Causes Bone Loss Around Dental Implants
You’ve invested time, money, and hope into your dental implant. For months, you’ve treated it like a precious part of your body. Then, during a routine check-up, your dentist mentions something unsettling: slight bone loss around the implant.
Your heart sinks. Is the implant failing? Did you do something wrong?
Let me stop you right there. A small amount of bone loss around a dental implant is actually normal during the first year. Yes, normal. But beyond that, bone loss is a signal. It’s your body telling you that something is off.
In this guide, we’ll walk through every possible cause of bone loss around dental implants. No dense medical jargon. No scare tactics. Just clear, honest answers to help you understand what’s happening and what you can do about it.
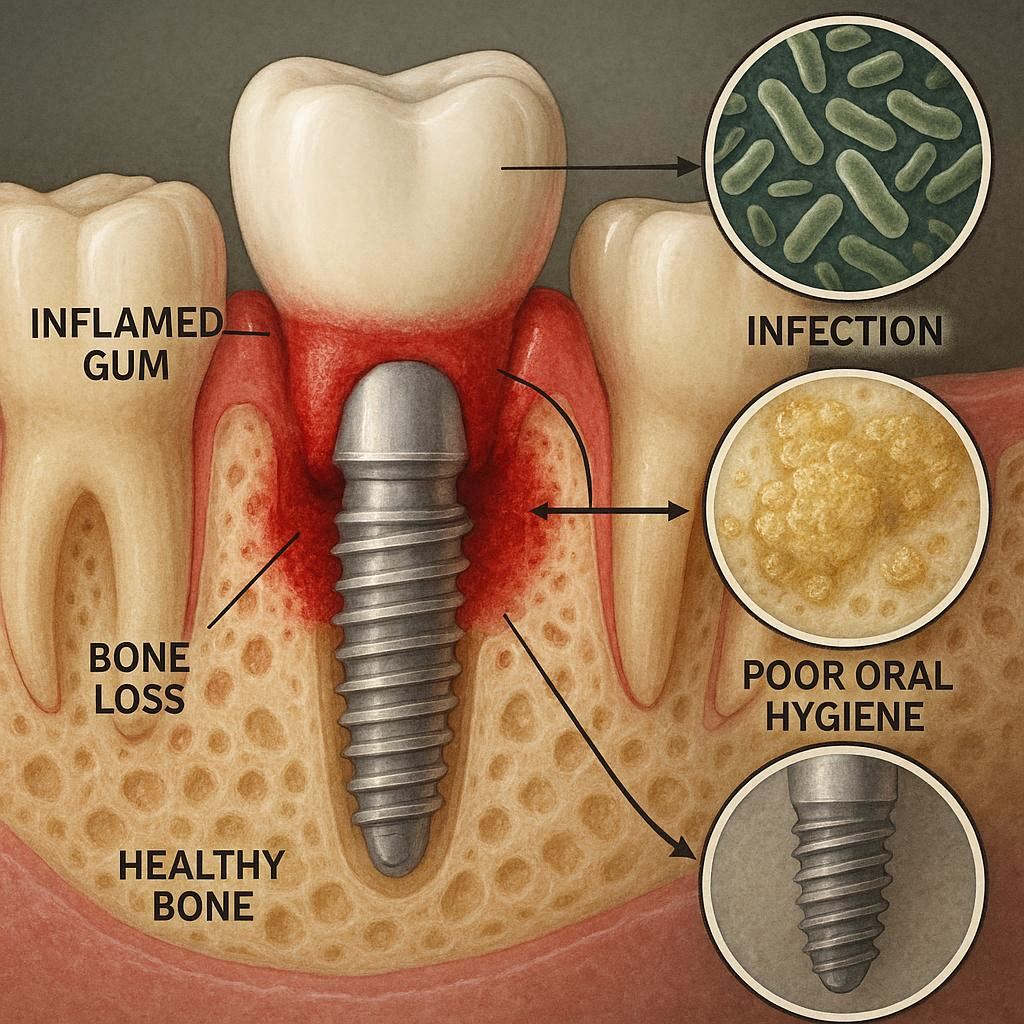
Understanding Bone Loss Around Implants: The Basics
Before we dive into causes, let’s get clear on what we’re actually talking about.
Bone loss around a dental implant means the jawbone that surrounds and supports the implant begins to shrink or dissolve. Unlike a natural tooth, an implant has no periodontal ligament. That ligament acts as a shock absorber and has a rich blood supply. Implants are fused directly to bone—a process called osseointegration.
When bone loss happens, that fusion is threatened.
What’s Normal vs. What’s Dangerous
| Type of Bone Loss | Typical Amount | When It Happens | Action Needed |
|---|---|---|---|
| Normal remodeling | 1.0 – 1.5 mm | First year after placement | None, just monitor |
| Minor bone loss | 0.2 mm per year | After first year | Routine check-ups |
| Moderate bone loss | 2 – 4 mm | Any time | Investigate cause |
| Severe bone loss | 5+ mm | Any time | Immediate intervention |
Important Note: Not all bone loss leads to implant failure. The key is identifying the cause early. Early bone loss is often reversible or stoppable. Late-stage bone loss is harder to manage.
The Top 10 Causes of Bone Loss Around Dental Implants
Let’s get straight to the heart of the matter. Below are the real, documented reasons why implants lose bone support.
1. Peri-Implantitis (The Number One Culprit)
If there’s one cause you need to remember, it’s peri-implantitis. This is an inflammatory disease that affects the gum and bone around an implant. Think of it as the implant version of severe gum disease.
How it happens: Bacteria build up on the implant surface, just like they do on natural teeth. But implants don’t have the same natural defenses. The inflammation spreads deeper, faster. Over months or years, the infection destroys the bone holding the implant.
Signs to watch for:
- Gums that bleed easily when you brush around the implant
- Red or purple discoloration of the gum tissue
- Pus coming from around the implant
- A deep pocket (over 5 mm) between the gum and implant
Peri-implantitis doesn’t happen overnight. It develops slowly, which is good news. It means you have time to catch it.
2. Smoking and Tobacco Use
Let’s be honest with each other. Smoking is one of the worst things you can do for an implant.
Nicotine constricts your blood vessels. That means less oxygen and fewer nutrients reach the bone around your implant. Your body’s ability to fight infection drops significantly.
What the research shows:
- Smokers have a 2 to 3 times higher rate of bone loss around implants
- Heavy smokers (more than 10 cigarettes per day) are at even higher risk
- Quitting before implant placement reduces risk dramatically
“I’ve placed thousands of implants over 20 years. The single biggest predictor of bone loss I see? Smoking. Not even close.” — Anonymous oral surgeon
3. Poor Oral Hygiene at Home
You brush your natural teeth. But do you clean around your implant with the same care?
Implants have different surfaces than natural teeth. Some are rough, some are smooth. Bacteria love to hide in tiny grooves and threads. If you’re only using a regular toothbrush, you might be missing a lot.
What effective implant hygiene looks like:
- Brushing twice daily with a soft brush
- Using a water flosser on a low setting
- Interdental brushes (the little cone-shaped brushes) for tight spaces
- Avoid harsh, abrasive toothpastes that can scratch the implant surface
Remember: You can’t get a cavity on an implant. But you can absolutely lose bone around it from poor cleaning.
4. Lack of Regular Professional Maintenance
Here’s something many implant patients don’t realize: implants need professional care just like natural teeth. But not just any cleaning.
Regular dental cleanings use metal scalers. Those metal tools can scratch the surface of some implants. Scratches become bacteria highways. Some hygienists aren’t trained on implant-specific instruments.
What you should ask your dental office:
- “Do you use plastic or titanium instruments for implant cleaning?”
- “Do you have an implant maintenance protocol?”
- “How often should I come in for my specific implant case?”
Most patients should have implant check-ups every 6 months. But if you’ve had bone loss before, every 3 to 4 months may be better.
5. Occlusal Overload (Too Much Pressure)
Natural teeth are suspended by ligaments. Those ligaments give slightly when you bite down. Implants don’t move. They’re fixed rigidly in the bone.
When you bite down with excessive force, that pressure transfers directly to the bone. Over time, the bone can micro-fracture and resorb (dissolve).
Who is at risk for occlusal overload?
- People who grind their teeth at night (bruxism)
- Those who clench during the day
- Patients with a very strong bite
- Implants placed in the back of the mouth where forces are highest
Signs of overload:
- The implant crown feels too high or hits first
- You notice chips or cracks in the crown material
- The implant feels slightly loose (this is late-stage)
- X-rays show a characteristic “saucer-shaped” bone loss pattern
6. Improper Implant Placement (Surgical Errors)
Let’s talk about something no dentist wants to admit: sometimes bone loss starts with the placement itself. Not all implant positions are created equal.
Common placement issues that cause bone loss:
| Problem | Why It Causes Bone Loss |
|---|---|
| Implant placed too close to adjacent teeth | Prevents natural bone remodeling |
| Implant angled incorrectly | Creates uneven bite forces |
| Implant placed too shallow | Lacks proper bone coverage |
| Damage to adjacent bone during surgery | Compromises initial healing |
This isn’t about blaming surgeons. Even excellent surgeons sometimes face unexpected anatomy. But if you had bone loss very early (within the first few months), placement factors are worth investigating.
7. Systemic Health Conditions
Your whole-body health directly affects your jawbone. Several medical conditions increase bone loss risk around implants.
High-risk conditions include:
- Diabetes (uncontrolled): High blood sugar impairs healing and fuels infection.
- Osteoporosis: The same bone-thinning disease affects your jaw. However, osteoporosis medication (bisphosphonates) is a separate concern.
- Autoimmune diseases: Rheumatoid arthritis, lupus, and Crohn’s disease all affect inflammation levels.
- HIV/AIDS: Advanced cases weaken immune response.
Important: Having these conditions doesn’t mean you can’t have implants. It means your implant team needs to know, and you may need closer monitoring.
8. Medications That Affect Bone Healing
Some medications directly alter how your bone responds to an implant.
Medications to discuss with your doctor:
- Bisphosphonates (Fosamax, Actonel, Boniva): Used for osteoporosis. These drugs dramatically slow bone remodeling. In rare cases, they can cause osteonecrosis of the jaw (bone death).
- Steroids (long-term use): Suppress immune function and reduce bone density.
- Some antidepressants: SSRIs have been linked to slightly lower bone density.
- Proton pump inhibitors (heartburn meds): Long-term use can reduce calcium absorption.
Never stop any medication without talking to your prescribing doctor. But do have the conversation before implant placement.
9. The Material and Design of the Implant Itself
Not all implants are created equal. The surface texture, thread design, and connection type all influence bone loss risk.
Features linked to lower bone loss:
- Roughened/sandblasted surfaces (better bone attachment)
- Platform switching (a design where the abutment is smaller than the implant)
- Tapered body designs (better stress distribution)
Features linked to higher bone loss:
- Smooth, machined surfaces (older designs)
- External hex connections (more prone to micro-movement)
- Wide-diameter implants in narrow bone (overpreparation)
This is why choosing an experienced implant dentist matters. They’ll select the right implant system for your specific bone quality and bite forces.
10. Allergic or Inflammatory Reactions (Rare but Real)
Less than 0.6% of people have true titanium allergies. But even without a true allergy, some people have heightened inflammatory responses to implant materials.
Symptoms of a reaction include:
- Persistent swelling long after healing
- Red, inflamed gums that don’t respond to cleaning
- Chronic bone loss despite perfect hygiene
- Skin rashes or eczema (in rare, systemic cases)
If you have a known metal allergy (to nickel, cobalt, or chromium), you’re at slightly higher risk. Zirconia (ceramic) implants are an alternative for these rare cases.
How Dentists Diagnose the Cause of Your Bone Loss
Your dentist won’t guess. They’ll follow a systematic process to identify what’s causing your bone loss.
Step 1: Review Your History
They’ll ask you about:
- When the implant was placed
- Any complications during healing
- Your cleaning habits (be honest!)
- Medical changes (new medications, new diagnoses)
- Any trauma or unusual bite patterns
Step 2: Clinical Examination
| What They Check | What It Reveals |
|---|---|
| Bleeding on probing | Active infection/inflammation |
| Pocket depths (probing) | How much attachment is lost |
| Mobility | Advanced bone loss (50%+) |
| Plaque and calculus | Your hygiene effectiveness |
| Gum color and texture | Chronic vs. acute inflammation |
Step 3: X-Ray Analysis (The Decisive Test)
Standard X-rays show bone levels. But for implants, dentists look for specific patterns:
- Saucer-shaped loss: Usually occlusal overload
- Vertical, angular loss: Often infection starting at the gum line
- Horizontal, even loss: Possibly systemic or medication-related
- Widening around the implant: Possibly a loose abutment connection
Step 4: Sometimes, Advanced Imaging
If the diagnosis isn’t clear, a CBCT (3D X-ray) provides detailed views of bone quality and quantity around the entire implant.
Can Bone Loss Around Implants Be Reversed?
This is the question everyone wants answered. Here’s the honest truth: it depends on the cause and the stage.
Reversible (Early Stage)
- Mild peri-implantitis: Yes, with deep cleaning and improved hygiene
- Occlusal issues: Yes, by adjusting the crown or using a night guard
- Poor hygiene alone: Yes, with professional cleaning and home changes
Manageable but Not Reversible (Moderate Stage)
- Moderate peri-implantitis: You can stop further loss, but lost bone rarely grows back fully
- Some placement issues: You can’t move the implant, but you can manage forces around it
Irreversible (Advanced Stage)
- Severe bone loss (over 50% of implant length): The implant will eventually fail and need removal
- Cracked implant body or fractured bone: Removal is usually the only option
Important: Don’t wait to see if bone loss “gets better on its own.” It won’t. Every week of delay reduces treatment options.
Treatment Options by Cause and Severity
Let’s match causes to solutions. Here’s what your dentist might recommend.
For Peri-Implantitis (Bacterial Cause)
Non-surgical treatment (early/moderate):
- Mechanical debridement with plastic or titanium instruments
- Laser therapy to disinfect deep pockets
- Antimicrobial rinses (chlorhexidine or hydrogen peroxide)
- Often requires 3-4 sessions over several months
Surgical treatment (advanced):
- Flap surgery to expose the implant surface
- Bone grafting to fill lost areas
- Surface decontamination
- Sometimes, implantoplasty (smoothing exposed rough threads)
For Occlusal Overload (Pressure Cause)
- Bite adjustment (reshaping the crown surface)
- Night guard fabrication (for grinding)
- Sometimes, removing a crown and making a new one with different contours
- In severe cases: removing and replacing the implant in a better position
For Poor Maintenance (Hygiene Cause)
- Professional implant cleaning
- Home tool training (water flosser, interdental brushes)
- More frequent recall visits (every 3-4 months)
- Chlorhexidine gel for stubborn areas
For Medical/Systemic Causes
- Coordination with your primary care doctor
- Adjusting medications if possible (never on your own)
- Optimizing diabetes or other condition management
- Antibiotic protocols for vulnerable patients
When Removal Is the Best Option
Sometimes, removing a failing implant is the kindest choice. This happens when:
- Bone loss exceeds 75% of the implant’s length
- The implant is already mobile
- You have untreatable infection spreading to adjacent bone
- The cost of saving it exceeds the value of the result
The good news? Failed implants can often be replaced after 3-6 months of healing.
A Practical Checklist to Protect Your Implants
You have more control than you think. Use this checklist daily and yearly.
Daily Home Care
- Brush twice daily with a soft or extra-soft brush
- Use a water flosser on medium setting around each implant
- Pass an interdental brush between the crown and gum
- Avoid hard, sticky, or crunchy foods on the implant side
- If you smoke, make a plan to reduce or quit
Professional Maintenance (Every 6 months minimum)
- Implant-specific cleaning (ask for plastic instruments)
- Pocket depth measurements around each implant
- X-rays every 12-24 months to compare bone levels
- Bite check (occlusal analysis)
- Review of your home cleaning technique
Red Flags That Need Immediate Attention
- Bleeding when you brush around the implant
- A bad taste or smell from the implant area
- Visible recession (gum pulling away)
- Any mobility or clicking sensation
- Sudden change in how the crown fits when you bite
Frequently Asked Questions (FAQ)
1. Is some bone loss around an implant normal?
Yes. Most implants lose about 1-1.5 mm of bone in their first year. This is normal bone remodeling. Beyond that, any ongoing bone loss needs investigation.
2. Can bone grow back around an existing implant?
Rarely on its own. With bone grafting procedures, some lost bone can be regenerated. But preventing further loss is the primary goal. Regrowing lost bone is difficult and not always successful.
3. How fast does bone loss happen around implants?
It varies. Aggressive peri-implantitis can destroy 1-2 mm of bone per month. Mild bone loss might take years to become significant. This is why regular X-rays are critical—they catch slow loss early.
4. Can a dental implant be saved after bone loss?
Yes, if the bone loss is less than 50% of the implant length. Treatments include deep cleaning, bone grafting, and bite adjustments. Once mobility develops, saving the implant is unlikely.
5. Does a night guard help prevent bone loss?
Absolutely. If you grind your teeth, a night guard distributes forces more evenly. It’s one of the most effective ways to prevent occlusal overload bone loss.
6. How often should I have my implants checked with X-rays?
Every 12-24 months for stable implants. If you’ve had bone loss before, every 6-12 months is better.
7. Are some people just more prone to implant bone loss?
Yes. Genetics, immune function, and bone density all play roles. Your dentist can’t predict everything, but a thorough medical history helps identify higher-risk patients.
8. What’s the success rate for treating peri-implantitis bone loss?
Non-surgical treatment stops progression in about 60-70% of early cases. Surgical treatment is more successful (80-90%) but is more invasive. Prevention is always better than treatment.
Conclusion
Bone loss around dental implants happens for many reasons, but most are preventable. The number one cause is peri-implantitis—bacterial infection around the implant. Other major causes include smoking, poor hygiene, missed maintenance visits, excessive bite forces, placement errors, and certain medical conditions. The good news is that early bone loss is often treatable, and late-stage bone loss is rare if you stay consistent with home care and professional check-ups. Your implant can last a lifetime, but only if you remain an active partner in its care.
Additional Resource
For a visual guide to proper implant hygiene techniques, including water flosser use and interdental brush selection, visit the American Academy of Implant Dentistry’s patient education library:
www.aaid.com/patient-resources/implant-hygiene
This resource includes free downloadable checklists and video demonstrations.
Disclaimer: This article is for informational purposes only and does not constitute medical or dental advice. Every patient is different. Always consult with your own licensed dentist or oral surgeon for diagnosis and treatment of bone loss around your dental implants.


