Dental Implants and Gum Disease: What You Must Know Before Treatment
If you are missing teeth and have been told you have gum disease, you might feel stuck. You want a permanent solution like dental implants, but your gums feel sore, bleed when you brush, or maybe you have already lost bone.
Here is the honest truth: gum disease and dental implants have a complicated relationship.
You can absolutely get dental implants if you have a history of gum disease. However, if you have active, untreated gum disease right now, no ethical dentist will place an implant into your mouth. Why? Because implants need healthy bone and firm, infection-free gums to survive.
This guide walks you through everything you need to know. We will cover risks, treatments, long-term success rates, and how to protect your investment for decades.
Let us start with the most important question of all.
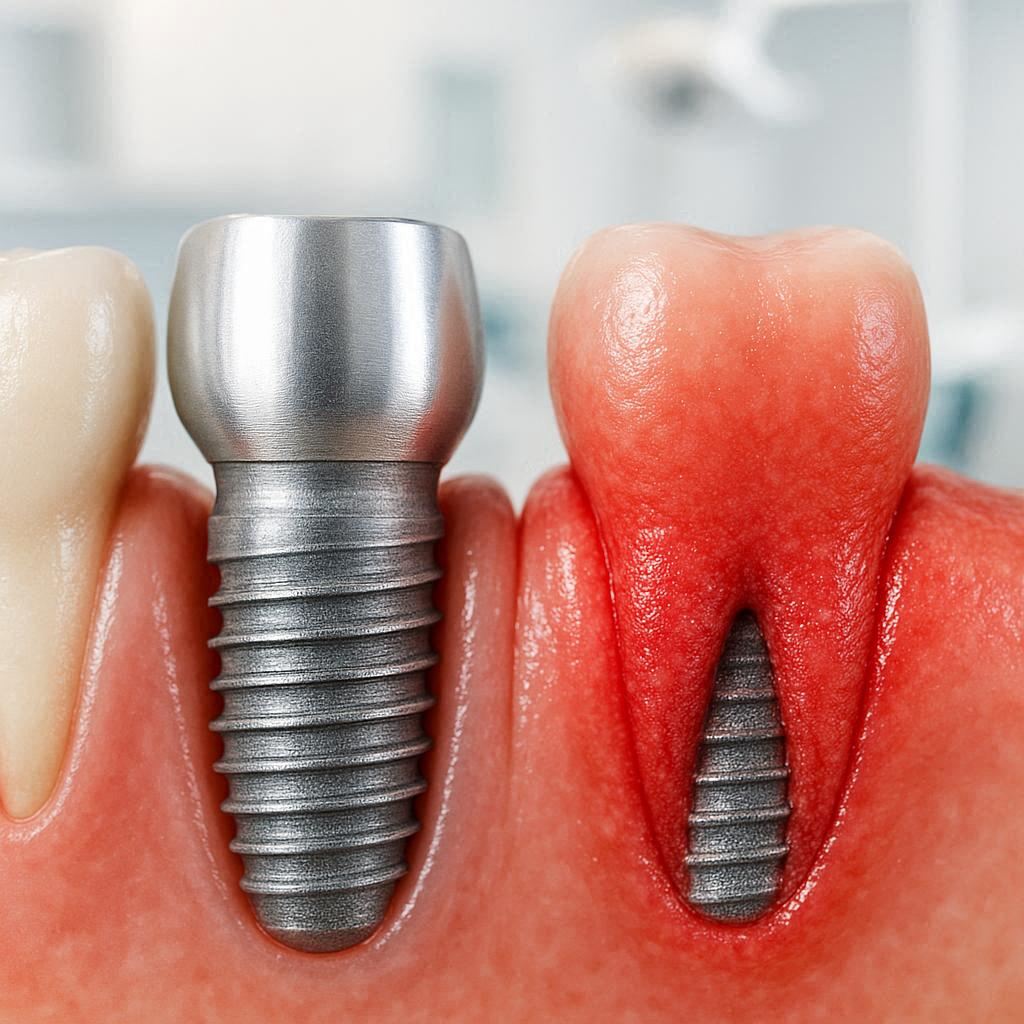
What Is Gum Disease and Why Does It Threaten Dental Implants?
Gum disease, also called periodontal disease, is an infection of the tissues that hold your teeth in place. It starts with bacteria from plaque and tartar building up along your gum line.
In the early stage, known as gingivitis, your gums may look red, feel swollen, and bleed easily. At this point, the damage is still reversible with professional cleaning and better home care.
But if you ignore gingivitis, it progresses to periodontitis. That is the more advanced form. The infection spreads below the gum line, and your body’s immune response actually starts breaking down the bone and connective tissue that hold teeth in place.
Now, here is why this matters for dental implants.
An implant is a titanium post surgically placed into your jawbone. Your bone needs to fuse with that post through a process called osseointegration. That fusion only happens in healthy, infection-free bone.
If you have active gum disease:
- The bone around your implant will not heal properly.
- Bacteria can travel from your remaining natural teeth to the implant site.
- You risk a condition called peri-implantitis, which is like gum disease for implants.
Important note: Peri-implantitis is the number one cause of late implant failure. It causes bone loss around the implant, and in many cases, the implant becomes loose and must be removed.
So, no, you cannot just “get implants” while you have bleeding, infected gums. But do not lose hope. Most people with gum disease can still become good candidates for implants. They just need to treat the gum disease first.
Can You Get Dental Implants If You Have a History of Gum Disease?
Yes. Many people with successfully treated gum disease go on to have dental implants that last for 20 years or more.
The key word here is treated.
Think of it this way: gum disease is a chronic condition, like high blood pressure. You cannot cure it completely, but you can manage it. Once you bring the infection under control and establish a solid maintenance routine, your mouth can become a safe environment for implants.
Studies show that people with a history of periodontitis have a slightly higher risk of implant complications compared to people who never had gum disease. But the difference is not huge if you follow a strict maintenance schedule.
One long-term study found that after 10 years, implant survival rates in people with treated gum disease were around 90% to 95%. That is still excellent.
So the answer is not “no.” The answer is “yes, with careful planning and lifelong care.”
What Dentists Look For Before Approving Implants
Before any implant surgery, your dentist or periodontist will evaluate several factors:
| Factor | What is healthy? | What is a problem? |
|---|---|---|
| Gum inflammation | No bleeding, pink tissue | Bleeding on probing, redness, swelling |
| Pocket depths | 1–3 mm | 4 mm or deeper with bleeding |
| Bone level | Solid bone height and width | Bone loss visible on X-rays |
| Plaque control | Minimal plaque | Heavy plaque and calculus |
| Overall health | Non-smoker, no uncontrolled diabetes | Smoking, uncontrolled systemic disease |
If you fail any of these checks, you are not ready for implants yet. But you can become ready with proper treatment.
Step-by-Step: The Path from Gum Disease to Dental Implants
This section outlines the realistic journey you will follow. Every person is different, but most people go through these five stages.
Step 1: Diagnosis and Full Mouth Assessment
Your dentist will take X-rays (panoramic or CBCT) to measure your bone volume. They will use a small probe to measure pocket depths around your remaining teeth. They will also check for bleeding, pus, and tooth mobility.
You may be referred to a periodontist, a specialist in gum disease and implant placement.
Step 2: Active Gum Disease Treatment (Non-Surgical)
For most people, the first treatment is scaling and root planing (SRP). This is a deep cleaning below the gum line. The dentist or hygienist removes plaque and tartar from root surfaces, then smooths the roots so gum tissue can reattach.
SRP is usually done with local anesthesia. You may need two to four appointments, one for each quadrant of your mouth.
After SRP, you will likely use a prescription mouth rinse (chlorhexidine) for a short period. Some dentists also recommend local antibiotics like Arestin placed directly into deep pockets.
Step 3: Re-Evaluation (4 to 6 Weeks Later)
Your dentist will re-measure your pocket depths. Healthy response looks like:
- Less bleeding
- Pocket depths reduced by 1–2 mm
- Firmer, pinker gum tissue
If your pockets remain deep (5 mm or more with bleeding), you may need further treatment. That could include periodontal surgery.
Step 4: Surgical Periodontal Treatment (If Needed)
For moderate to advanced gum disease, non-surgical cleaning may not be enough. Surgical options include:
- Flap surgery: The gum is lifted back, tartar is removed from deep pockets, and the gum is sutured back in place.
- Bone grafting: If you have lost bone, your dentist may place graft material to regenerate lost support.
- Guided tissue regeneration: A special membrane encourages your body to grow new bone and ligament tissue.
Only after your gums are stable and infection-free will you move to implant planning.
Step 5: Implant Placement (After Healing)
You will need a healing period after gum treatment. This can range from 4 to 12 months. Your bone and gums need time to mature and become healthy.
Once your periodontist confirms that your gum disease is inactive (no bleeding on probing, pocket depths under 4 mm, stable bone levels), you can proceed with implant surgery.
Realistic timeline: From the day you start gum disease treatment to the day you receive your final implant crown, plan for 9 to 18 months. Rushing the process is the fastest way to fail.
Peri-Implantitis: The Silent Threat After Implants
Even after you receive implants successfully, your history of gum disease puts you at higher risk for a condition called peri-implantitis.
Peri-implantitis is inflammation and infection around an implant. It destroys the bone supporting the implant. Unlike natural teeth, implants have no periodontal ligament. That means when infection starts, it spreads faster because there is no natural barrier.
Signs of Peri-Implantitis
- Red or purplish gums around the implant
- Bleeding when you brush or floss near the implant
- Pus coming from the gum around the implant
- Deep pocket depths (over 5 mm) around the implant
- The implant feels mobile (this is a late sign)
- You notice bad taste or bad breath that does not go away
What Causes Peri-Implantitis?
| Cause | Explanation |
|---|---|
| Poor oral hygiene | Plaque builds up around the implant crown |
| Smoking | Reduces blood flow and healing |
| Untreated gum disease elsewhere | Bacteria spread from natural teeth to implants |
| Improper implant placement | Crown too rough or ill-fitting, trapping bacteria |
| Lack of professional maintenance | No regular cleanings after implant restoration |
| Genetic factors | Some people over-react to bacterial presence |
Can Peri-Implantitis Be Treated?
Yes, but early detection is everything.
- Early stage (mucositis): Inflammation limited to gum tissue. Reversible with professional cleaning and improved home care.
- Moderate peri-implantitis: Bone loss visible on X-rays. Treatment includes non-surgical debridement, local antibiotics, and laser therapy.
- Advanced peri-implantitis: Significant bone loss. Requires surgical flap surgery, bone grafting around the implant, or even implant removal if too much bone is gone.
If you lose an implant to peri-implantitis, you may still be able to place another implant later, but only after the infection is fully controlled and new bone is grafted. This is expensive and time-consuming. Prevention is far better.
How to Protect Your Dental Implants When You Have Gum Disease History
You have the power to keep your implants for life. It just takes consistent effort. Here is what works.
Your Daily Home Care Routine
Think of your implants as high-maintenance investments. Natural teeth have some built-in defenses. Implants have none. Bacteria can stick to implant surfaces more easily.
Follow this checklist every single day:
- Brush twice a day with a soft-bristled toothbrush. An electric toothbrush is even better.
- Use a water flosser on a low setting. Aim the water stream at the gum line around each implant.
- Use interdental brushes (proxy brushes) for spaces between implants and natural teeth.
- Floss daily with implant-specific floss or super floss that has a stiff end to thread under the crown.
- Use a non-abrasive toothpaste. Avoid whitening toothpastes with harsh grit that can scratch implant surfaces.
- Rinse with an antimicrobial mouthwash (alcohol-free) if your dentist recommends it.
Professional Maintenance Schedule
Do not skip your dental cleanings. Ever.
For someone with a history of gum disease who has implants, the standard recommendation is:
- Every 3 months: Periodontal maintenance cleaning. This includes measuring pocket depths around all teeth and implants, scaling, and polishing.
- Every 12 months: Full-mouth X-rays to check bone levels around implants.
Some patients with excellent home care and stable gums can stretch to every 4 months. But very few people with past gum disease can safely wait 6 months between cleanings.
Lifestyle Changes That Protect Implants
Quit smoking. This is non-negotiable. Smokers with a history of gum disease have implant failure rates up to three times higher than non-smokers. Nicotine reduces blood flow to your gums, masks early signs of infection, and impairs healing.
Control diabetes. If you have diabetes, keep your HbA1c below 7%. Uncontrolled diabetes dramatically increases infection risk around implants.
Reduce stress. High stress raises cortisol levels, which can worsen gum inflammation. Stress also leads to teeth grinding (bruxism), which can overload implants.
Eat a gum-friendly diet. Limit sugary snacks and sodas. Eat crunchy vegetables like carrots and celery, which naturally clean tooth surfaces. Include calcium and vitamin D for bone health.
Implant Options for People with Bone Loss from Gum Disease
One of the most frustrating effects of advanced gum disease is bone loss. When you lose bone, you may not have enough height or width in your jaw to place a standard implant.
But modern dentistry has solutions.
Bone Grafting
A bone graft rebuilds lost bone. The graft material can come from:
- Your own bone (from your chin, jaw, or hip)
- Donor bone (human cadaver bone, processed and sterilized)
- Animal bone (usually bovine)
- Synthetic bone materials
The graft is placed into the deficient area, then covered with a membrane. You wait 4 to 9 months for new bone to grow. After that, you can place implants normally.
Sinus Lift (For Upper Back Teeth)
If you have lost upper molars and gum disease destroyed the bone above them, your sinus cavity may have expanded downward. A sinus lift adds bone between your jaw and the sinus floor. This is a common, predictable procedure.
Short Implants
Traditional implants are about 10 to 16 mm long. Short implants are 6 mm or less. They work well in areas with limited bone height, and they often avoid the need for grafting. Short implants have high success rates when placed correctly.
Zygomatic Implants
For extreme bone loss in the upper jaw where even grafting is impossible, zygomatic implants anchor into the cheekbone (zygoma) instead of the jawbone. These are rare, expensive, and only performed by highly trained specialists. Most people never need them.
Mini Implants
Mini implants are narrower (less than 3 mm in diameter). They require less bone volume but are also less strong. They are best for stabilizing lower dentures, not for replacing single teeth in heavy biting areas.
| Implant Type | Bone Requirement | Best For | Success Rate |
|---|---|---|---|
| Standard implant | 10 mm height, 6 mm width | Single tooth, multiple teeth | 95%+ |
| Short implant | 6 mm height | Limited height (lower jaw) | 90–95% |
| Bone graft + standard | Any (graft creates bone) | Moderate to severe bone loss | 85–90% |
| Zygomatic | Minimal jawbone | Extreme upper jaw loss | 90–95% (specialist only) |
| Mini implant | Low volume | Denture stabilization | 80–85% |
The Cost Reality: Gum Disease Treatment + Implants
Let us talk money honestly. Treating gum disease and placing implants is not cheap. But ignoring gum disease and losing natural teeth or implants is more expensive in the long run.
Here is a realistic breakdown of costs in the United States (without insurance):
| Procedure | Average Cost Range |
|---|---|
| Full mouth exam and X-rays | $150 – $350 |
| Scaling and root planing (full mouth) | $500 – $1,500 |
| Periodontal maintenance cleaning (per visit) | $100 – $250 |
| Periodontal flap surgery (per quadrant) | $800 – $1,500 |
| Bone graft (small area) | $500 – $1,200 |
| Sinus lift (one side) | $1,500 – $3,000 |
| Single dental implant (post only) | $1,500 – $2,500 |
| Abutment and crown for implant | $1,000 – $2,000 |
| Full implant-supported denture (one arch) | $15,000 – $30,000 |
If you need treatment for moderate gum disease plus two implants, your total could easily range from $6,000 to $12,000. For full-mouth reconstruction, $30,000 to $60,000 is common.
Does insurance help?
Medical insurance rarely covers dental implants. Dental insurance often covers a portion of gum disease treatment (scaling, surgery) but typically caps out at $1,000 to $2,000 per year. For implants, most dental plans cover nothing or only a small percentage.
Financing options:
Many dental offices offer payment plans through CareCredit, LendingClub, or in-house financing. Some patients travel to Mexico, Costa Rica, or Colombia for lower-cost implants, but this comes with risks like follow-up care and quality control.
Frequently Asked Questions (FAQ)
1. Can I get dental implants if my gums are receding?
Yes, but you must treat the cause of recession first. Gum recession is often a sign of past or active gum disease, or aggressive brushing. Once your gums are healthy, your dentist can place implants. In some cases, you may need a gum graft to create enough healthy tissue around the implant.
2. How long do dental implants last if you have had gum disease?
With excellent home care and 3- to 4-month professional cleanings, implants can last 20 years or more. Studies show 10-year survival rates above 90% in treated gum disease patients. Without good maintenance, failure can happen in 2 to 5 years.
3. What are the first signs of implant failure due to gum disease?
Bleeding when you brush around the implant is the earliest sign. Next comes redness, bad taste, and pocket deepening. If you catch it at the bleeding stage (peri-implant mucositis), it is reversible. Waiting until bone loss appears on X-rays means you need surgery.
4. Can I get all-on-4 implants if I have gum disease?
Yes, but only after your gum disease is fully treated and stable. All-on-4 uses four implants to support a full arch of teeth. Because these implants are angled and placed in better bone, they can work even with some bone loss. However, active gum disease is an absolute contraindication.
5. Is it better to get implants or dentures if I have gum disease?
If your gum disease is well-controlled, implants are almost always better for long-term bone preservation, chewing function, and comfort. If you cannot control your gum disease (for example, if you refuse to quit smoking or attend cleanings), dentures are safer because failed dentures do not destroy bone like failed implants do.
6. Can gum disease spread from natural teeth to implants?
Yes. Bacteria from untreated gum disease around your natural teeth travel through your saliva. They colonize the surfaces of your implants. This is one of the most common reasons people with one or two implants develop peri-implantitis. Treat all gum disease everywhere in your mouth, not just near the implant site.
7. Do I need antibiotics before implant surgery if I have gum disease history?
Your dentist or periodontist will decide based on your specific case. Many specialists prescribe prophylactic antibiotics one hour before implant surgery for patients with a history of periodontitis. This reduces bacterial load during the critical healing phase.
8. Can I reverse gum disease after implants are placed?
You can stop its progression and reduce inflammation, but you cannot fully reverse bone loss. If you develop peri-implantitis after implants are placed, early treatment (non-surgical cleaning, laser, antibiotics) can control it. Advanced cases require surgery. Prevention through maintenance is your best strategy.
9. What is the best toothbrush for implants and gum disease?
An electric toothbrush with a pressure sensor (like Oral-B or Sonicare) is excellent. Use a brush head labeled “sensitive” or “orthodontic” with extra-soft bristles. Avoid hard bristles, which can scratch implant abutments and cause microscopic grooves where bacteria hide.
10. How do I find a dentist who specializes in implants and gum disease?
Look for a periodontist. They have three extra years of training in gum disease and implant placement. You can search the American Academy of Periodontology website (perio.org) for a specialist near you. A prosthodontist also has advanced training in implant restorations.
Additional Resource
For a step-by-step visual guide to daily cleaning around implants, including videos on water flosser techniques and interdental brush use, visit the American Academy of Periodontology’s patient education page:
🔗 https://www.perio.org/for-patients/periodontal-treatments-and-procedures/dental-implants/
This official resource is free, evidence-based, and updated regularly. It includes downloadable instructions for home care and a “Find a Periodontist” tool.
Conclusion
Dental implants and gum disease can coexist, but only if you take gum disease seriously before, during, and after implant placement. Treat active infection first, then rebuild lost bone if needed, and finally commit to a lifetime of meticulous home care and professional cleanings every three to four months. With this honest approach, even patients with advanced periodontitis can enjoy the function and confidence of dental implants for decades.


