I Can Feel My Dental Implant Through My Gum
You run your tongue along your gum line, and suddenly, you feel it. A hard, foreign shape. It is not a tooth. It is not smooth like your natural enamel. It feels like metal or a rough edge sitting right under the surface of your gum tissue.
If you are reading this, you are likely experiencing that exact sensation. First, take a deep breath. You are not alone, and this issue is more common than most people think.
Feeling your dental implant through your gum can range from a completely normal part of the healing process to a sign that something needs a dentist’s attention. The key is knowing the difference.
In this guide, we will walk you through every possible reason you might feel your implant, what the sensation actually means for the health of your mouth, and the exact steps you should take next.
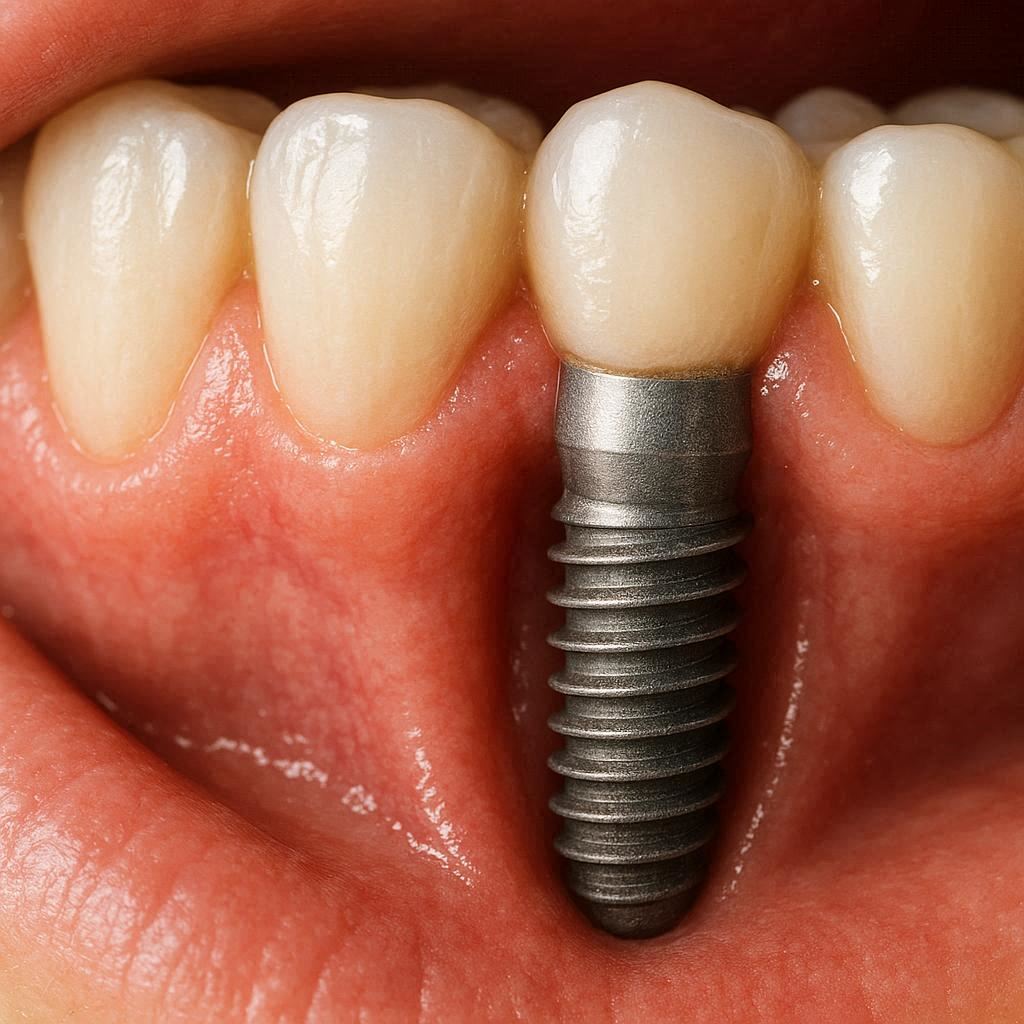
Understanding the Layers: What Is Under Your Gum?
Before we dive into why you feel your implant, let us quickly look at what a dental implant actually is. Think of it as an artificial tooth root. It is typically made of titanium or zirconia. The dentist places this screw-like post into your jawbone.
Over time, your bone grows around the implant. This process is called osseointegration. Once that bond is strong, the dentist attaches an abutment (a connector piece) and finally a crown (the visible “tooth”).
Between the implant and the outside world is your gum tissue. In a perfect scenario, you should feel nothing but smooth gum. You should not detect edges, screws, or metal. So when you do feel something, it means one of the layers between you and the implant has changed.
Why Can I Feel My Dental Implant Through My Gum? (The Short Answer)
Since you want the truth quickly, here it is: you can feel your dental implant through your gum because either (1) the gum tissue has thinned or receded, (2) the implant components are sitting too high, or (3) there is swelling that is pushing the implant against sensitive tissue.
In most cases, feeling the implant is not an emergency. However, in some specific situations, it is a red flag. Let us break down every possible cause in detail so you know exactly where you stand.
Complete List of Reasons You Feel Your Implant (Honest and Realistic)
We will not give you vague answers. Below is a realistic, clinically accurate list of why you might be sensing that hard shape under your gum.
1. Normal Healing: The First Few Weeks
If you just had your implant placed within the last two to four weeks, what you are feeling might be completely normal.
Why This Happens
When a dentist places an implant, they must cut through the gum to access the bone. They then stitch the gum closed over or around the implant. In the early days, the gum tissue is swollen, tight, and inflamed. Your tongue is hyperaware of any change in your mouth.
During this period, you may feel the shape of the underlying implant simply because the tissue has not yet relaxed into its final form.
What It Feels Like
- A vague hardness under the gum
- A sensation of something “foreign” but not sharp
- No exposed metal visible in the mirror
What You Should Do
Nothing. Give your mouth time. Most patients stop feeling the implant outline after four to six weeks as swelling subsides and the gum matures.
Important Note: Do not poke or press on the area with your finger or tongue repeatedly. This can delay healing and create irritation.
2. Thin Gum Biotype (Your Natural Anatomy)
Some people are simply born with thinner gum tissue. This is called a “thin scalloped biotype” in dental terms. If you have naturally delicate gums, you are more likely to feel your implant.
Why This Happens
Your gum thickness is genetic. If your tissue is less than 2mm thick, it acts like a thin blanket over the implant. Unlike a natural tooth root, which is covered by a ligament that provides some cushion, an implant is rigid. A thin gum cannot hide that rigidity well.
What It Feels Like
- A distinct, clear outline of the implant’s top
- No pain
- No bleeding
- The sensation is constant but not getting worse
What You Should Do
This is generally not a problem as long as the gum remains healthy. However, you should tell your dentist. They may recommend a gum graft in the future to thicken the tissue and protect the implant long-term.
3. The Abutment or Healing Cap Is Too High
This is one of the most common mechanical reasons people feel their implant. Between the implant screw (in the bone) and the crown (the fake tooth), there is a small connector called an abutment.
Sometimes, that abutment sits a little too high above the gum line.
Why This Happens
During the second phase of your implant procedure, the dentist uncovers the implant and screws on a healing abutment (a small metal or plastic cap) to shape the gum. If that cap is tall, you will feel it as a hard bump.
What It Feels Like
- A firm, round protrusion under the gum
- You can press it and feel no give
- It may feel like a small marble under the surface
- No pain unless you press hard
What You Should Do
This is an easy fix. Your dentist can replace the healing abutment with a shorter one. If the final crown is already placed and you feel the abutment underneath, the crown may need to be adjusted or remade.
4. Gum Recession (Exposing the Implant Surface)
This is where you need to pay closer attention. Gum recession means your gum tissue is shrinking or pulling away. When that happens, more of the implant becomes exposed.
Why This Happens
Recession can occur due to:
- Aggressive brushing
- Smoking or tobacco use
- Gum disease (peri-implantitis)
- Poor implant placement angle
- Lack of attached gum tissue around the implant
What It Feels Like
- You feel a rough or threaded texture (the implant body itself)
- The sensation increases over weeks or months
- You may also see a darker color under the gum (gray or metal)
What You Should Do
Schedule a dental appointment. Early recession can often be managed with a gum graft or better home care. Advanced recession with bone loss may require more complex treatment.
5. Peri-Implantitis (Infection Around the Implant)
This is the most serious reason you might feel your implant. Peri-implantitis is an inflammatory disease that affects the soft and hard tissues around a dental implant. It is similar to severe gum disease but around an implant instead of a natural tooth.
Why This Happens
Bacteria accumulate under the gum and around the implant threads. The body attacks the bacteria, but in doing so, it also destroys bone and gum tissue. As the bone dissolves, the implant becomes exposed.
What It Feels Like
- You feel the implant, but it is accompanied by:
- Bleeding when you brush or floss
- Bad taste or bad breath
- Red, swollen, or shiny gums
- Pain when chewing
- The implant may feel slightly loose (this is a late sign)
What You Should Do
Do not wait. See your dentist or a periodontist immediately. Peri-implantitis can lead to implant failure if not treated. Early treatment involves deep cleaning and antibiotics. Late treatment may require surgery or implant removal.
6. Implant Thread Exposure Without Disease
Sometimes you can feel the threads of an implant simply because of how the implant was positioned. This is different from disease-related exposure.
Why This Happens
If the implant was placed too close to the surface of the bone, or if the bone is naturally thin on one side, the threads may sit very close to the gum. Over time, even minor gum shrinkage can reveal them.
What It Feels Like
- A ribbed or corrugated texture under the gum
- No bleeding
- No pain
- The implant feels solid
What You Should Do
If there is no infection, many dentists will simply monitor this. A soft tissue graft can cover the threads if they bother you or if they are at risk of future problems.
7. Loose Healing Abutment or Cover Screw
This is a minor mechanical issue that produces a scary sensation.
Why This Happens
The small screw that holds the healing abutment in place can loosen over time. When it does, the abutment can shift or tilt slightly, pushing against the gum from the inside.
What It Feels Like
- You feel a hard edge that moves slightly when you touch it with your tongue
- A clicking sensation
- The feeling comes and goes
What You Should Do
Call your dentist. They need to retighten the screw. Do not try to do this yourself. Using the wrong tool can damage the implant’s internal hex.
8. Scar Tissue or Fibrous Healing
After any surgery, the body forms scar tissue. Around dental implants, scar tissue can feel denser and harder than normal gum tissue.
Why This Happens
Some patients form thick collagen bands during healing. This fibrous tissue feels like a hard ridge. You are not actually feeling the metal implant. You are feeling the body’s response to the surgery.
What It Feels Like
- A hard, smooth ridge
- No specific shape (not round like an abutment)
- No tenderness
- The sensation is stable over time
What You Should Do
This is harmless. Over several months, this tissue often softens. Massaging the area gently with a clean finger (after your dentist approves) can help remodel the scar tissue.
Normal vs. Concerning: A Quick Comparison Table
To help you decide if you need to call your dentist today or wait for your next checkup, use this table.
| Sensation / Symptom | Likely Cause | Urgency Level |
|---|---|---|
| Feels hard but smooth, no pain, recent surgery | Normal healing or thin gums | Low (monitor at home) |
| Feels like a round marble, no redness | Healing abutment too tall | Low to moderate (call dentist) |
| Feels rough or threaded, no bleeding | Thread exposure without disease | Moderate (schedule visit) |
| Feels rough + bleeding + bad taste | Peri-implantitis | High (see dentist this week) |
| Feels movable or clicking | Loose screw | Moderate (see dentist soon) |
| Feels hard + visible gray metal + pain on chewing | Advanced recession or bone loss | High (urgent dental visit) |
| Feels different but looks healthy, no change over months | Scar tissue or normal anatomy | Very low (no action needed) |
The One Sensation That Requires an Emergency Visit
We want to be very clear. Most of the time, feeling your implant is not an emergency. But there is one exception.
If you feel your implant AND the crown or abutment is visibly moving when you push it gently with your finger, you need to see a dentist within 24 to 48 hours.
Movement indicates that the implant has lost its integration with the bone. This is called a failed osseointegration. The only solution is usually removing the implant, letting the bone heal, and trying again later.
Do not wait weeks if your implant feels loose. Early evaluation can sometimes save it if the issue is just a loose abutment screw rather than a failed implant body.
What Should You Do Right Now? (Step-by-Step Action Plan)
Instead of worrying, follow this simple four-step plan.
Step 1: Perform a Self-Assessment (The Mirror Test)
Go to a well-lit bathroom. Open your mouth. Look closely at the gum around your implant.
- Can you see any metal? If yes, that is recession.
- Is the gum red or purple? If yes, that suggests inflammation.
- Is there a pimple-like bump on the gum? If yes, that could be a fistula (drainage tract for infection).
If you see any of these, call your dentist. If everything looks pink and healthy, move to step two.
Step 2: The Clean-Finger Test
Wash your hands thoroughly. Gently feel the area with a clean finger.
- Does it hurt when you press lightly? Pain suggests inflammation.
- Does the shape move? Movement suggests a loose component or failed implant.
- Is the texture simply hard and smooth? That is often normal.
Step 3: Check Your Habits
Ask yourself these honest questions:
- Have you been brushing that area too hard?
- Do you smoke?
- Do you clench or grind your teeth at night? (Grinding can push implants against bone and cause microfractures in the gum tissue.)
Step 4: Call Your Dentist (With the Right Information)
When you call, say: “I had an implant placed [X months/years ago]. I can feel the implant through my gum. There is [no pain / some pain / bleeding]. The implant feels [solid / slightly movable].”
This helps the office prioritize your case.
How Dentists Diagnose the Problem (So You Know What to Expect)
If you decide to see your dentist, here is exactly what they will do.
Visual and Tactile Exam
The dentist will look at the color, contour, and texture of your gum. They will gently probe around the implant with a periodontal probe. Measurements deeper than 5mm often indicate bone loss.
Radiographs (X-rays)
A periapical X-ray or a CBCT (3D scan) shows the bone level around your implant. The dentist can see exactly how much bone remains and whether the threads are exposed below the gum.
Mobility Testing
Using two metal instrument handles, the dentist will tap your implant crown. A solid, high-pitched sound means it is integrated. A dull, low sound or visible movement means it is loose.
Bleeding on Probing (BOP)
If the gum bleeds easily when touched, that is a sign of active inflammation or peri-implantitis.
Based on these findings, your dentist will give you one of three verdicts: “normal anatomy,” “monitor only,” or “treatment needed.”
Treatment Options: From Simple Fixes to Advanced Procedures
Let us be realistic. Most people who feel their implant do not need surgery. But some do. Here are the actual treatments based on the cause.
For Thin Gums or Minor Recession
- Observation: No treatment if healthy.
- Gum graft (connective tissue graft): A small piece of tissue taken from your palate and sewn over the exposed area. This thickens the gum.
For a Healing Abutment That Is Too High
- Abutment exchange: Your dentist numbs the area, removes the tall abutment, and screws in a shorter one. Takes ten minutes.
For a Loose Abutment Screw
- Retorquing: Your dentist uses a torque wrench designed for implants to tighten the screw to the correct value (usually 15 to 35 Ncm).
For Peri-Implantitis (Mild to Moderate)
- Non-surgical debridement: Special plastic or titanium instruments clean the implant surface without scratching it. Local anesthesia is used.
- Laser therapy: A dental laser disinfects the pocket and stimulates healing.
For Peri-Implantitis (Moderate to Severe)
- Open flap debridement: The gum is surgically reflected (lifted back) to expose the implant threads. They are cleaned thoroughly. Bone grafting material may be placed.
- Implantoplasty: The exposed rough threads are smoothed down to make them harder for bacteria to colonize.
For Failed Implant (Loose or Severe Bone Loss)
- Explanation: Surgical removal of the implant. The site is cleaned and grafted with bone. A new implant can usually be placed after four to six months of healing.
Home Care for an Implant That You Can Feel (But Is Healthy)
If your dentist has told you that your situation is normal or just a cosmetic issue, you still need to care for that area differently than a natural tooth.
Do Not Use Metal Instruments
Never use a metal dental scaler on an exposed implant surface. It will scratch the titanium. Bacteria love scratches. Use only plastic or rubber instruments.
Switch to a Soft or Extra-Soft Toothbrush
Hard bristles can push gum tissue further down over time. Soft bristles clean effectively without causing recession.
Try a Water Flosser
A water flosser on a low to medium setting is excellent for flushing out bacteria around an implant that you can feel. Aim the stream at a 45-degree angle toward the gum line.
Use a Low-Abrasion Toothpaste
Avoid toothpaste with baking soda, charcoal, or harsh whitening agents. These can abrade both the implant crown and the surrounding gum tissue. Use a non-abrasive gel or a toothpaste specifically labeled for implants or sensitive teeth.
Consider a Night Guard
If you grind your teeth, ask your dentist for a night guard. Grinding generates extreme forces. Those forces can compress the gum tissue against the hard implant, making the sensation of feeling the implant worse over time. A night guard acts as a shock absorber.
Long-Term Prognosis: Will It Get Worse?
Here is the honest truth that many articles avoid. Once you start feeling your implant, in some cases, the sensation may never fully go away. But that does not mean you will lose the implant.
- If the cause is thin gum biotype: You will likely always feel the outline. But with good care, your implant can last 20+ years.
- If the cause is a healing abutment: The feeling will disappear once the final crown is placed and the gum matures.
- If the cause is mild recession without bone loss: With a gum graft, you will stop feeling it. Without a graft, you will continue to feel it, but it may remain stable.
- If the cause is peri-implantitis: The prognosis depends entirely on how quickly you seek treatment. Treated early, success rates are over 85%. Treated late, the implant may fail within two to three years.
The most important predictor of long-term success is not whether you feel the implant. It is whether you have bleeding, pain, or mobility. No bleeding + no pain + solid implant = good prognosis even if you feel it.
Common Myths About Feeling a Dental Implant (Do Not Believe These)
Let us clear up some dangerous misinformation.
Myth 1: “If you feel it, it is failing.”
Truth: Feeling your implant is often just an anatomical quirk. Millions of people walk around every day with perfectly healthy implants they can feel. The implant does not know you can feel it. The bone does not care.
Myth 2: “You should never feel any part of an implant.”
Truth: In a perfect world, yes. But dental medicine is not perfect. Many clinically successful implants are palpable through thin gums. Your dentist will look for signs of disease, not just sensation.
Myth 3: “Brushing harder will fix the gum problem.”
Truth: Brushing harder causes recession. It will expose more of the implant, not less. Gentle, consistent brushing is the answer.
Myth 4: “Flossing is dangerous around an implant you can feel.”
Truth: Flossing is essential. Use implant-specific floss or super floss with a stiff end to thread under the crown. Do not avoid cleaning because you are afraid.
When to Get a Second Opinion (And How to Choose the Right Specialist)
If your current dentist says “it is fine” but you are still worried, or if you feel dismissed, you have every right to seek a second opinion. This is your body and your money.
Go to a Specialist, Not a General Dentist
For implant concerns, see:
- A periodontist: Gum and bone specialist. Best for recession, thin gums, and peri-implantitis.
- A prosthodontist: Implant restoration specialist. Best for abutment fit, crown issues, and bite problems.
What to Bring to Your Second Opinion
- Your most recent X-rays (ask your current dentist for copies or have them emailed)
- The name and brand of your implant (if known)
- A written timeline: when placed, when crowned, when symptoms started
A good specialist will spend at least 15 minutes examining you and explaining their findings. If they rush, leave.
Prevention: How to Avoid Feeling Your Implant in the First Place
If you are reading this before getting an implant, or if you are planning a second implant, these steps can dramatically reduce your chances of ever saying “I can feel my dental implant through my gum.”
Choose an Experienced Surgeon
The number one factor is the surgeon’s skill. An implant placed at the correct depth (3mm below the planned crown margin) and with adequate bone on the facial side is much less likely to become palpable over time.
Ask About Your Gum Biotype Before Surgery
A good dentist will measure your gum thickness before placing the implant. If you have a thin biotype, they may recommend a simultaneous gum graft at the time of implant placement.
Request a Custom Abutment
Stock abutments (mass-produced) often have bulky profiles that stretch the gum thin. Custom-milled abutments are designed to fit your specific gum contour. They cost more but reduce the chance of feeling the implant.
Commit to Maintenance Appointments
Every six months, your dentist should check your implant with probing and X-rays. Most problems that cause you to feel the implant (like peri-implantitis) are detectable years before you ever feel them.
Personal Stories (Anonymized, Realistic Cases)
These are composite cases based on common clinical scenarios. They are not real patients but represent real patterns.
Case 1: Sarah, age 42.
Sarah had a lower molar implant placed two years ago. Six months ago, she noticed she could feel a hard ridge under her gum. No pain, no bleeding. Her dentist measured 3mm pocket depths (healthy) and took an X-ray showing no bone loss. Diagnosis: thin gum biotype. Treatment: none. Sarah still feels the ridge, but she has accepted it as normal. Her implant is healthy.
Case 2: Mark, age 58.
Mark felt his upper front tooth implant every time he spoke. It bothered him constantly. His dentist found that the healing abutment was 3mm too tall. The dentist swapped it for a shorter one. Within one week, Mark could no longer feel the implant. His problem was solved completely.
Case 3: Linda, age 67.
Linda ignored the sensation of feeling her implant for over a year. She also noticed bleeding when she brushed. By the time she saw a periodontist, she had lost 60% of the bone around the implant. She needed a bone graft and a new implant. Linda wishes she had acted sooner.
Frequently Asked Questions (FAQ)
Q1: Is it normal to feel the edge of my implant with my tongue?
Yes, this is very common, especially for implants in the front of the mouth where the tongue naturally explores. As long as the gum looks pink and does not bleed, this is usually just an anatomical reality.
Q2: Can a dental implant slowly push through the gum over time?
No. Implants do not “erupt” like natural teeth. However, the gum can recede around a stable implant, which creates the illusion that the implant is coming through. The implant itself remains in the same position.
Q3: Will food get stuck under the gum if I can feel the implant?
Possibly. If the implant margin (where the crown meets the implant) is below the gum, food can pack into that space. A water flosser is excellent for flushing these areas. Ask your dentist if your crown margin is accessible for cleaning.
Q4: I feel my implant, but my dentist says it looks perfect on X-ray. Should I trust them?
Yes, in most cases. X-rays show bone health, which is the real measure of implant success. If your bone levels are stable, feeling the implant is a soft tissue issue, not a structural emergency. However, if your anxiety persists, a second opinion is always your right.
Q5: Can allergies to titanium cause me to feel my implant?
True titanium allergy is extremely rare (less than 0.6% of the population). It typically presents with chronic swelling, rash-like gums, and burning pain, not just a palpable sensation. If you have those symptoms, ask your dentist about allergy testing.
Q6: How much does it cost to fix a gum recession that exposes an implant?
A gum graft for a single implant typically costs between $600 and $1,500 without insurance. Dental insurance may cover a portion if the recession is due to disease rather than cosmetic preference. Many periodontists offer payment plans.
Q7: Can I use over-the-counter numbing gels if the area feels sensitive?
No. Numbing gels will not address the cause. They also mask pain, which is an important warning sign. If you have pain from your implant, see a dentist. Do not self-medicate with topical anesthetics.
Q8: I had my implant placed 10 years ago and just started feeling it. Why now?
Late-onset sensation is usually due to gradual gum recession from aging, changes in your bite, or the slow progression of peri-implantitis. A dental evaluation is definitely warranted in this case.
Additional Resource Link
For a deeper understanding of how to maintain dental implants long-term and prevent complications like peri-implantitis, visit the American Academy of Periodontology’s patient education page on dental implants.
👉 perio.org/consumer/dental-implants
This resource includes video animations of implant placement, detailed guides on home care, and a searchable directory of board-certified periodontists in your area.
Conclusion
Feeling your dental implant through your gum is often a harmless result of thin natural tissue or a slightly tall healing abutment that can be easily adjusted. However, if the sensation is accompanied by bleeding, redness, pain, or movement, it may signal peri-implantitis or bone loss requiring prompt professional care. Always have any new or worsening sensation evaluated by a dentist, but remember that a palpable implant without other symptoms is frequently a normal, manageable finding.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a licensed dental professional for diagnosis and treatment of dental implant issues.


