Bleeding From My Dental Implant
You brush your teeth, maybe floss gently around that new dental implant, and then you see it: a streak of red on your toothbrush or in the sink.
Your stomach drops. After everything you went through to get that implant—the consultation, the procedure, the healing—the last thing you want is a problem.
Let me say this right away: a small amount of bleeding around a dental implant is often normal, especially in the first few days or weeks. But not all bleeding is the same. Some types require a simple adjustment in your cleaning routine. Others need a professional’s attention.
In this guide, we will walk through every possible reason for bleeding from your dental implant. You will learn what is common, what is concerning, and exactly what to do in each situation. No medical jargon. No scare tactics. Just clear, honest information you can use.
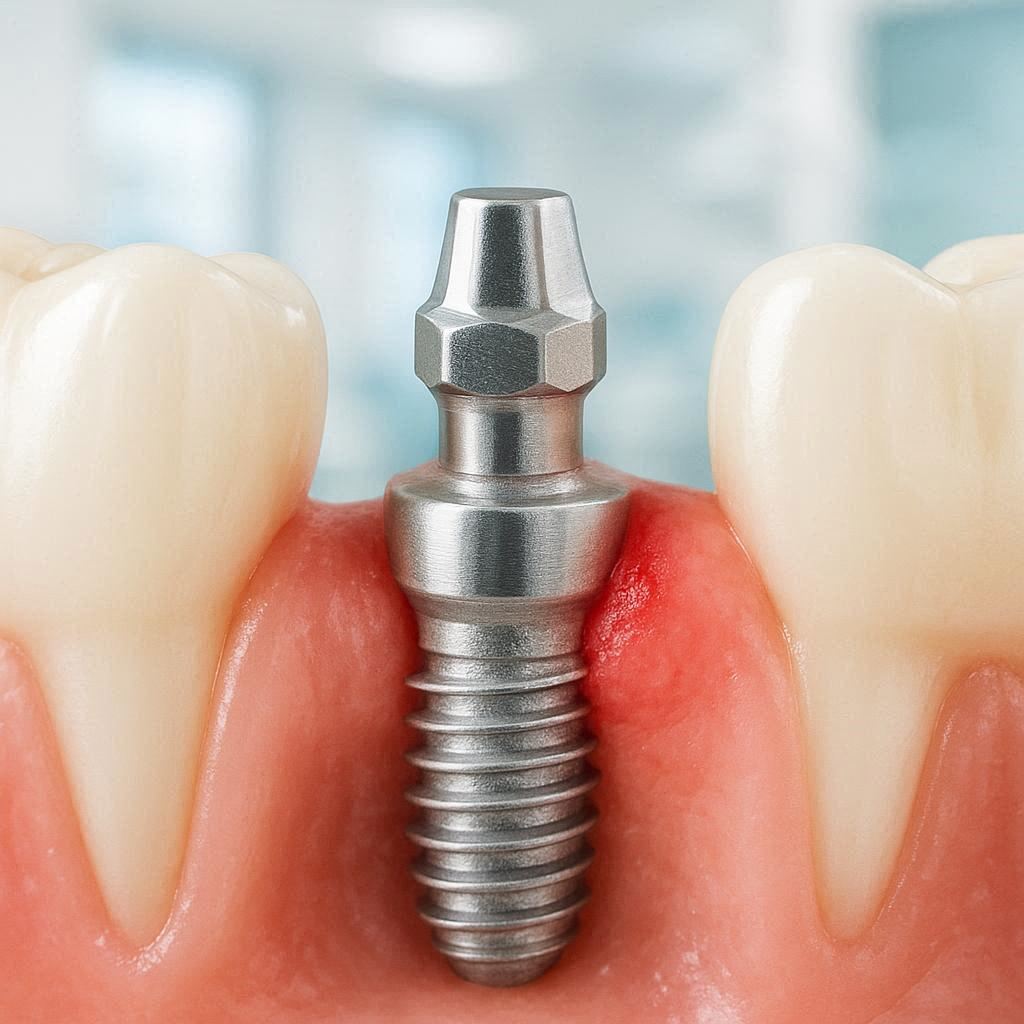
Understanding Normal vs. Concerning Bleeding
Before we dive into causes and solutions, let us establish a simple rule of thumb.
Normal bleeding often looks like:
- A slight pink tint on your toothbrush or dental floss
- Occasional minor spotting when you brush a little too hard
- Light bleeding that stops within a minute or two
- Bleeding only during active cleaning, not spontaneously
Concerning bleeding often looks like:
- Bright red blood that flows freely or drips
- Bleeding that continues for more than 5–10 minutes without stopping
- Blood that appears without any touching or brushing
- Bleeding accompanied by pain, swelling, or a bad taste
If your bleeding matches the first group, you can usually breathe easy. If it matches the second group, call your dentist or oral surgeon sooner rather than later.
Why Do Dental Implants Bleed? The Short Answer
A dental implant is a titanium post surgically placed into your jawbone. Over time, your bone grows around it—a process called osseointegration. But the implant also passes through your gum tissue. That gum tissue behaves much like natural gum tissue around a real tooth.
Just like natural gums, the gums around an implant can become irritated, inflamed, or injured. And when gum tissue gets irritated, it bleeds.
The difference with an implant? You cannot get a cavity in an implant. But you can absolutely get gum disease around it. That inflammation is called peri-implant mucositis (early stage) or peri-implantitis (advanced stage). Bleeding is often the very first warning sign.
Important note: Do not ignore bleeding just because you think “implants don’t get problems.” They do. But most problems are completely manageable when caught early.
Common Causes of Bleeding From a Dental Implant
Let us break down the most frequent reasons people see blood around their implants. I have organized these from least to most serious.
1. Normal Post-Surgical Bleeding
In the first 24 to 72 hours after implant placement, some oozing and light bleeding is expected. You just had a surgical procedure. Your body needs time to form clots and begin healing.
What you might see:
- Pink-tinged saliva
- Light spotting on gauze
- Slight bleeding when you rinse gently with salt water
What to do:
- Bite gently on a clean, moist gauze pad for 20–30 minutes
- Avoid spitting, using a straw, or rinsing vigorously
- Sleep with your head slightly elevated
- Follow your surgeon’s specific post-op instructions
When to worry: If bright red blood fills your mouth quickly or you cannot stop the flow with pressure, contact your surgeon immediately.
2. Brushing or Flossing Too Aggressively
This is probably the most common cause of minor bleeding weeks or months after surgery. You want to keep your implant clean—that is great. But using a hard-bristled toothbrush or snapping floss down against the gum can cause tiny tears.
Signs it is you, not the implant:
- Bleeding only happens right after you clean that area
- The gum looks healthy otherwise (pink, not swollen)
- There is no pain or tenderness
What to do:
- Switch to a soft or extra-soft toothbrush
- Use unwaxed floss or implant-specific floss (more on that later)
- Try a water flosser on a low setting
- Be gentler. Think “massage,” not “scrub.”
3. Poor Oral Hygiene Leading to Gum Inflammation
On the opposite end of the spectrum, not cleaning well enough allows plaque to build up along the gumline. That plaque contains bacteria. Your gums react with inflammation (gingivitis), and inflamed gums bleed easily.
Signs of inflammation-related bleeding:
- Bleeding even with very light brushing
- Red, puffy, or shiny gums around the implant
- Possible bad breath or a metallic taste
What to do:
- Improve your hygiene routine (see the cleaning section below)
- Consider a professional dental cleaning
- Do not stop cleaning the area—bleeding gums need more gentle cleaning, not less
A common myth is “My gums bleed, so I will avoid that area.” That is the opposite of what you should do. Gums bleed because they are inflamed. Gentle, thorough cleaning removes the plaque causing the inflammation. Within a week or two, the bleeding usually stops.
4. Improperly Fitted Crown or Abutment
The abutment is the connector piece between the implant (in the bone) and the crown (the visible fake tooth). If the crown or abutment does not fit perfectly, it can create a gap where food and bacteria accumulate. It can also put pressure on the gum in a way that causes chronic irritation.
Signs of a fit issue:
- Bleeding that is always in the exact same spot
- Food getting stuck around the implant constantly
- The gum looks pinched or white in one area
- You feel pressure when biting that the dentist did not warn you about
What to do: This requires a dental visit. Your dentist can check the fit with X-rays and sometimes by trying new components. In many cases, a simple adjustment or a new abutment solves the problem.
5. Peri-Implant Mucositis (Reversible Gum Inflammation)
Think of this as “gingivitis, but for an implant.” The gum tissue around the implant is inflamed, but the bone underneath is still healthy. The good news? This stage is reversible with proper care.
Signs include:
- Bleeding on gentle probing (your dentist checks this)
- Redness and swelling confined to the gum tissue
- No deepening of the pocket around the implant
- No bone loss visible on X-ray
What to do:
- Schedule a professional cleaning focused on the implant
- Improve your home care significantly
- Use an antimicrobial mouthwash as recommended by your dentist
- Return for a re-evaluation in 4–6 weeks
Most people with peri-implant mucositis can resolve it completely with three to four weeks of excellent home care and one professional cleaning.
6. Peri-Implantitis (Bone Loss Around the Implant)
This is the more serious condition. Peri-implantitis occurs when inflammation moves beyond the gums and starts destroying the bone supporting your implant. Bleeding is almost always present. So is pocketing (deep spaces around the implant).
Signs include:
- Bleeding that is easy to provoke
- Pus or discharge when you press on the gum
- Deep probing depths (over 5–6 mm)
- Visible bone loss on X-rays
- Possible mobility of the implant (in advanced cases)
What to do: This is not a DIY situation. You need professional treatment, which may include:
- Non-surgical deep cleaning (scaling and root planing, but adapted for implants)
- Laser therapy to decontaminate the surface
- Antimicrobial gels or locally delivered antibiotics
- In advanced cases, surgical flap procedures or even bone grafting
The earlier you catch peri-implantitis, the better the outcome. Do not delay.
7. Retained Cement (For Cement-Retained Implants)
Some implants use cement to attach the crown to the abutment, similar to a traditional dental crown. If excess cement spills beyond the margin and stays under the gum, it acts like a foreign object. Bacteria love it. The gum bleeds as it tries to push the cement out.
Signs of cement-related bleeding:
- Bleeding that started shortly after the crown was placed
- No improvement with better brushing or flossing
- A dentist sees white cement on an X-ray or during probing
What to do: Your dentist needs to remove the excess cement. This sometimes means removing the crown, cleaning everything thoroughly, and re-cementing it carefully. In stubborn cases, switching to a screw-retained crown eliminates the issue entirely.
8. Trauma or Injury
You bit down on something hard. You got elbowed playing sports. You dropped a fork against your implant crown. Trauma can cause immediate bleeding from the gum around an implant.
Signs of traumatic bleeding:
- Bleeding starts right after a specific event
- The gum may look torn or bruised
- The implant itself may feel slightly different when biting
What to do:
- Apply gentle pressure with a clean cloth or gauze
- Use ice on the outside of your cheek for the first 24 hours
- Eat soft foods for a few days
- See your dentist if bleeding does not stop or if the implant feels loose
Most trauma-related bleeding resolves on its own. However, if the implant shifted or feels mobile, you need an X-ray to check for a fracture in the implant or the bone.
9. Underlying Medical Conditions or Medications
Sometimes the bleeding has nothing to do with your implant at all. It is simply more noticeable there because the gum tissue is slightly thinner or more delicate.
Conditions that increase bleeding tendency:
- Diabetes (especially if poorly controlled)
- Bleeding disorders like hemophilia or von Willebrand disease
- Liver disease
- Leukemia or other blood cancers
Medications that increase bleeding:
- Blood thinners (warfarin, apixaban, rivarrests, clopidogrel)
- High doses of NSAIDs like ibuprofen or aspirin
- Some antidepressants (SSRIs like fluoxetine)
- Certain supplements (fish oil, vitamin E, ginkgo, garlic)
What to do: Do not stop any prescribed medication without talking to your doctor. But do tell your dentist about every medication and supplement you take. They can adjust your cleaning recommendations and may coordinate with your primary care physician.
10. Loose Implant Components
Your implant system has several parts: the implant body (in the bone), the abutment (connector), and the crown (tooth). The abutment screws into the implant. That screw can loosen over time, especially if the crown takes heavy biting forces.
Signs of a loose component:
- Bleeding that comes and goes
- A clicking or slight movement when you push on the crown
- Food packing around the implant more than usual
- A feeling that something is “not right”
What to do: This is a simple fix but needs a dentist. They will tighten the screw (or replace it) and check the crown’s fit. Do not try to tighten anything yourself—you risk damaging the internal threads of the implant.
11. Allergic Reaction (Rare)
True allergy to titanium (the metal most implants are made from) is extremely rare, affecting less than 1% of patients. However, some people react to other metals in the abutment or crown, such as nickel or chromium.
Signs of an allergic reaction:
- Bleeding accompanied by persistent burning or itching
- Redness that spreads beyond the implant area
- Swelling that does not respond to better hygiene
- Possible rash on nearby skin or lips
What to do: Ask your dentist about allergy testing. If confirmed, they can replace the implant components with more biocompatible materials, such as zirconia.
Comparative Table: Common Causes at a Glance
| Cause | Bleeding Pattern | Other Symptoms | Can I Fix It at Home? |
|---|---|---|---|
| Post-surgical (normal) | Oozing, pink saliva | Mild discomfort | Usually yes, with rest |
| Aggressive cleaning | Only during/after brushing | None | Yes, change technique |
| Poor hygiene/inflammation | Even with light brushing | Red, puffy gums | Usually yes, with better care |
| Poorly fitted crown | Same spot daily | Food trapping, pressure | No, needs dental adjustment |
| Peri-implant mucositis | On probing, brushing | Redness, no bone loss | Partially—needs some professional help |
| Peri-implantitis | Easy to provoke, possible pus | Deep pockets, bone loss | No, requires treatment |
| Retained cement | After crown cementation | None visible to you | No, dentist must remove cement |
| Trauma | Sudden, after injury | Bruising, possible mobility | Only if very mild |
| Medical/medication | General easy bleeding | Bleeding elsewhere | No, coordinate with doctors |
| Loose component | Intermittent | Clicking, movement | No, dentist must tighten |
| Allergic reaction | Persistent, burning | Itching, spreading redness | No, needs allergy testing |
Step-by-Step: What to Do Right Now If You See Bleeding
You just noticed blood. Do not panic. Here is a straightforward action plan.
Step 1: Assess the amount
Is it a few dots or a steady flow? If steady or dripping, call your dentist now. If minimal, proceed.
Step 2: Rinse gently
Mix a cup of warm water with half a teaspoon of salt. Swish gently for 30 seconds, then let the water fall out of your mouth. Do not spit forcefully.
Step 3: Identify the trigger
Did you just brush or floss? Did you bite something hard? Has this happened before?
Step 4: Modify your cleaning for 2–3 days
- Switch to a softer toothbrush
- Use a water flosser on the lowest setting
- Floss every other day instead of every day
- Brush that area last, with less pressure
Step 5: Monitor for 5–7 days
Keep a simple log. Does the bleeding get better, worse, or stay the same?
Step 6: Decide on professional help
If bleeding improves within a week, you likely fixed the cause. If it stays the same or worsens, call your dentist.
Do not stop cleaning the implant entirely. Avoiding the area allows plaque to build up, which makes inflammation and bleeding worse over time.
How to Properly Clean Around a Dental Implant
Most bleeding problems stem from either too much aggression or too little cleaning. Here is the middle path that works.
Daily Cleaning Tools You Actually Need
A soft or extra-soft toothbrush
Standard toothbrushes are often too hard for implant gums. Look for “soft” or “ultra-soft” on the package. Electric toothbrushes are fine but use a sensitive or gum-care head.
Implant-specific floss or superfloss
Regular floss is thin and can snap against the gum. Superfloss has a stiff end for threading, a spongy middle for cleaning around the abutment, and regular floss at the other end. Use the spongy section gently.
Water flosser (optional but excellent)
A water flosser on a low setting can flush out debris without mechanical trauma. Aim the tip at a 45-degree angle toward the gumline. Use warm water.
Interdental brushes (proxy brushes)
If your implant has a wider space between it and the next tooth, a small interdental brush can be very effective. Choose one that fits without forcing. You should feel gentle resistance, not pain.
Step-by-Step Cleaning Routine
- Rinse first with plain water or a non-alcoholic mouthwash to loosen debris.
- Water floss on low setting, directing the stream between the gum and the implant crown.
- Brush all your teeth normally, but use very light pressure around the implant. Two minutes total.
- Floss the implant last. Gently thread the spongy floss between the gum and the abutment. Hug the side of the implant crown, then the side of the adjacent tooth. Do not snap.
- Interdental brush if needed. Insert gently, move back and forth 2–3 times, and remove.
- Final rinse with salt water or a prescribed rinse if your dentist recommended one.
This routine takes about three extra minutes. It is worth every second.
When to Call Your Dentist Immediately
Some situations are not “wait and see.” Call your dentist or oral surgeon right away if you experience:
- Bleeding that does not stop after 10 minutes of gentle pressure
- Bleeding accompanied by severe pain (not just soreness)
- A visible piece of the implant or crown that feels loose or moves
- Swelling that spreads to your cheek, eye, or neck
- Fever over 101°F (38.3°C) along with implant bleeding
- Pus or foul discharge coming from the gum around the implant
- Numbness in your lip, chin, or tongue after the initial healing period
- A metallic taste that persists for more than a day or two
Your dentist will likely want to see you the same day or the next morning for these symptoms. Do not feel silly calling. They would rather see a false alarm than a delayed problem.
Professional Treatments for Implant Bleeding
If home care is not enough, your dentist has several tools to help. Here is what they might do, from least to most invasive.
Professional Dental Cleaning (Prophy)
For simple gum inflammation, a regular cleaning removes plaque and calculus from above and slightly below the gumline. The hygienist uses special plastic or carbon-fiber instruments because metal scalers can scratch the implant surface. Scratched surfaces hold bacteria more easily.
Non-Surgical Peri-Implant Debridement
For peri-implant mucositis or mild peri-implantitis, the dentist or periodontist will:
- Numb the area (if needed)
- Use ultrasonic scalers with plastic-coated tips
- Hand scale with titanium or plastic instruments
- Flush the pocket with an antimicrobial solution like chlorhexidine
- Possibly place an antibiotic gel (e.g., minocycline microspheres) into the pocket
This is often done in one 30–60 minute appointment. You may need a second visit 4–6 weeks later to check healing.
Implant Surface Decontamination
If the implant surface itself has bacterial buildup, surface decontamination methods include:
- Air polishing with glycine powder (gentle on titanium)
- Laser therapy (diode or Er:YAG lasers kill bacteria without touching the surface)
- Titanium brush that mechanically cleans the threads
Surgical Treatment for Advanced Peri-Implantitis
When bone loss is significant, surgery becomes necessary. Options include:
- Open flap debridement: The gum is lifted, the implant is cleaned directly, and the gum is sutured back.
- Bone grafting: Lost bone is replaced with graft material, sometimes covered with a membrane.
- Implantoplasty: The exposed rough part of the implant is smoothed down so bacteria have less surface area to cling to.
In very advanced cases, the implant may need to be removed entirely. The bone is then allowed to heal for several months before placing a new implant.
How to Prevent Bleeding Problems Long-Term
Prevention is simpler and cheaper than treatment. Follow these five principles.
1. Commit to Regular Maintenance Visits
Natural teeth need cleaning every 6–12 months. Implants often need more frequent checks—every 3–6 months, depending on your risk factors. At these visits:
- Your dentist checks pocket depths around the implant
- X-rays (usually once a year) look for bone loss
- The hygienist professionally cleans the implant
2. Stop Smoking or Using Tobacco
Smoking is one of the strongest risk factors for implant bleeding and failure. Smokers have higher rates of peri-implantitis, more bone loss, and worse healing overall. If you cannot quit completely, cutting back significantly still helps.
3. Manage Systemic Health Conditions
Get your diabetes under control (HbA1c under 7% is ideal). Treat gum disease elsewhere in your mouth—untreated gum disease on natural teeth can spread to implants. If you have arthritis or another condition that makes brushing difficult, ask about adaptive tools.
4. Wear a Nightguard If You Grind Your Teeth
Bruxism (teeth grinding) puts excessive force on implants. Unlike natural teeth, implants have no ligament to cushion the blow. That force can cause component loosening, bone loss, and bleeding from chronic trauma. A custom nightguard distributes the force safely.
5. Watch What You Eat
Very hard foods (ice, hard candy, bones) can chip crowns or traumatize gums. Sticky foods (caramels, taffy) can pull at restorations. You do not need a special diet, but use common sense. Cut whole apples rather than biting into them. Avoid using your implant as a tool to open packages or crack nuts.
Realistic Bleeding Scenarios (Examples)
Let me paint three common real-world situations so you can see how this plays out.
Scenario A: Maria, 3 weeks post-implant placement
Maria sees pink on her toothbrush every morning. The area is a little tender but not painful. She has been using a medium toothbrush and brushing hard because she is scared of infection. After switching to a soft brush and using a water flosser on low, the bleeding stops in 4 days. Cause: aggressive cleaning.
Scenario B: James, 2 years with implant
James notices bleeding when flossing around his lower left implant. He also has a persistent bad taste. He has not seen a dentist in 18 months. At his checkup, the hygienist finds 5mm pockets and mild bone loss on X-ray. Diagnosis: early peri-implantitis. Treatment: non-surgical debridement and a chlorhexidine rinse. He also starts using an interdental brush. Six weeks later, there is no bleeding and pockets are 3mm. James now sees his dentist every 4 months.
Scenario C: Linda, 5 years with implant
Linda’s implant suddenly bleeds after she bites into a crusty bread roll. The gum looks slightly torn. There is no mobility. Her dentist takes an X-ray, which shows no fracture. Linda uses salt water rinses and soft foods for a week. The gum heals completely. Cause: minor trauma. No further treatment needed.
Quotations from Implant Professionals (Synthesized from Common Clinical Wisdom)
“Bleeding is the smoke alarm of the mouth. Do not remove the battery. Find the fire.” – Implant periodontist, 20 years of experience
“The most common mistake I see? Patients who brush their implant like they are scrubbing a dirty pan. Gentle and frequent beats hard and occasional, every time.” – Dental hygienist specializing in implant maintenance
“When a patient tells me ‘my implant bleeds but it doesn’t hurt,’ I listen carefully. Painless bleeding is still bleeding. It still means inflammation.” – Oral surgeon
“I would rather see an implant patient every three months for a quick cleaning than every two years for a surgical rescue.” – Restorative dentist
Additional Resources and Recommended Link
For further reading on dental implant maintenance and recognizing early warning signs, the American Academy of Periodontology offers a free patient guide:
Recommended external resource:
American Academy of Periodontology – Dental Implants Patient Information
Note: Always verify that external links are active and consult your own dental professional for personalized advice.
Important Notes for Readers (Do Not Skip)
📌 This article is for informational purposes only. It does not replace professional medical or dental advice. Every mouth is different.
📌 Do not stop prescribed blood thinners because of minor gum bleeding without speaking to the doctor who prescribed them. The risk of a stroke or blood clot far outweighs gum bleeding.
📌 If you are pregnant, hormone changes can make gums bleed more easily. Tell your dentist. Routine dental care is safe during pregnancy, but X-rays and medications need special consideration.
📌 Implants are not “set it and forget it.” Plan on lifelong maintenance. The best implant in the world will fail without proper home care and professional checkups.
📌 Do not use over-the-counter numbing gels on bleeding implant gums. They can mask important symptoms and sometimes irritate tissues further.
📌 If your bleeding started right after a dental procedure (like a crown placement or cleaning), call that office first. They know exactly what they did and can give the most specific advice.
Conclusion – In Three Lines
Bleeding from a dental implant ranges from normal post-surgical oozing to serious peri-implantitis. Most cases resolve with gentler cleaning or a professional dental cleaning, but persistent bleeding always warrants a dental evaluation. Catch problems early, maintain regular checkups, and your implant can serve you well for decades.
Frequently Asked Questions (FAQ)
1. Is it normal for a dental implant to bleed after one year?
No, not as a routine event. By one year, the surgical site should be fully healed. If you see bleeding a year after placement, something is causing inflammation or trauma. See your dentist.
2. Can I use regular toothpaste on my dental implant?
Yes, but avoid “whitening” toothpastes or those with baking soda, charcoal, or harsh abrasives. They can scratch the implant crown surface. Standard fluoride toothpaste is fine.
3. Why does my implant bleed only when I floss?
That usually means the floss is snapping against the gum (aggressive technique) or there is plaque buildup right at the flossing site. Try implant-specific floss and be gentler. If bleeding continues for two weeks, see your dentist.
4. How long does it take for bleeding gums around an implant to heal after improving hygiene?
With correct home care, mild inflammation bleeding usually improves within 5–14 days. If you see no change after two weeks, professional help is likely needed.
5. Can a dental implant bleed years later for no reason?
There is always a reason, even if you do not see it. Possible hidden causes include a loose screw, retained cement, or the start of peri-implantitis. Do not assume “it will go away on its own.”
6. Should I use mouthwash if my implant is bleeding?
Yes, but choose wisely. An alcohol-free, chlorhexidine-based rinse (by prescription only for short-term use) or a saline (salt water) rinse is best. Avoid alcohol-based mouthwashes—they dry and irritate.
7. Can stress cause my dental implant to bleed?
Indirectly, yes. Stress can lead to teeth grinding (bruxism), which puts extra force on the implant and can cause trauma bleeding. Stress also affects immune function, making gum inflammation worse.
8. What does it mean if bleeding comes with a bad smell?
A foul odor or taste suggests bacterial infection. This could be peri-implantitis or an abscess. Call your dentist promptly. Do not wait.
9. Is it safe to use an electric toothbrush on an implant?
Yes, it is safe and often more effective than a manual brush. Use a soft head and a sensitive/easy-start mode if available. Avoid scrub brush heads.
10. Can my implant fall out from bleeding?
The bleeding itself will not cause the implant to fall out. But if the bleeding is from advanced peri-implantitis with significant bone loss, the implant can become loose and eventually fail. That is why early treatment matters.
Disclaimer:
This article is for general informational purposes only and does not constitute medical or dental advice. Always seek the advice of your dentist or other qualified health provider with any questions you may have regarding a dental or medical condition. Never disregard professional advice or delay in seeking it because of something you have read here. The author and publisher are not responsible for any adverse effects or consequences resulting from the use of any information in this article.