Bone Graft at Time of Implant Placement: A Complete, Honest Guide
If you have lost a tooth, you have probably heard about dental implants. They are the gold standard for replacement. But there is a common phrase that scares many patients: “You need a bone graft first.”
What if you could do both procedures at once?
The good news is that modern dentistry often allows you to place the implant and the bone graft at the same time. This is called a simultaneous bone graft. It saves you time, money, and a second surgery.
But is it right for you? Let’s walk through everything together. No complex jargon. Just clear, honest facts.
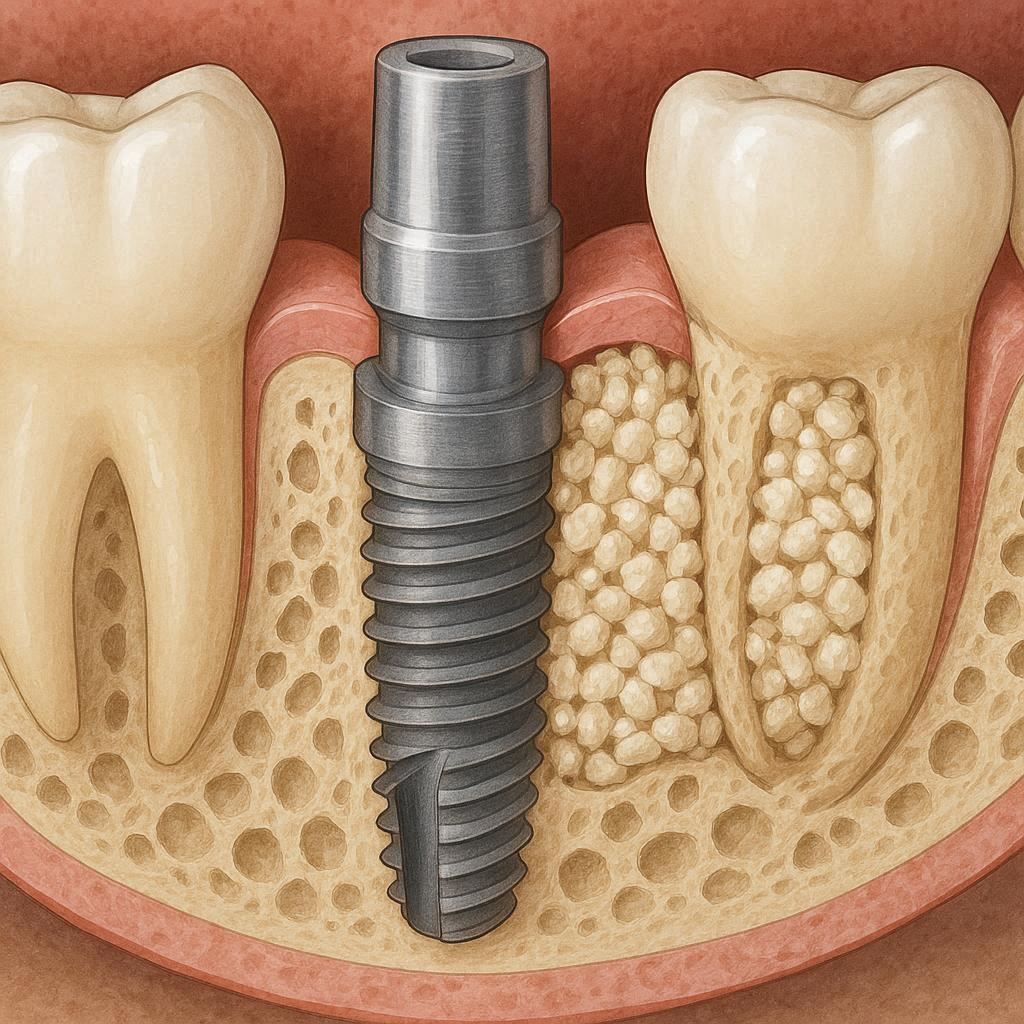
What Does “Bone Graft at Time of Implant Placement” Actually Mean?
Let’s break this down simply.
A dental implant is a small titanium screw. It replaces your tooth’s root. To hold that screw, you need enough natural jawbone. Think of it like building a fence. You need deep, solid soil to set the post. If the soil is too shallow or too soft, the fence will wobble.
Sometimes, after losing a tooth, your jawbone shrinks. This happens because the bone no longer has a root to support. This is called bone resorption.
A bone graft adds new bone material to the weak area. When the dentist does this at the same visit as placing the implant, they place the graft material around the exposed part of the implant or into a small defect next to it.
“Doing both together respects the body’s natural healing. It turns two surgeries into one recovery.” — Dr. Elena Vasquez, Prosthodontist.
Why Do We Need Bone Around an Implant?
- Stability: The implant needs bone to lock into.
- Longevity: An implant surrounded by good bone lasts decades.
- Aesthetics: Bone supports your gum tissue. Without bone, your gum looks gray or collapsed.
When Is a Simultaneous Graft Possible? (The Honest Truth)
Not every patient is a candidate. A good dentist will never force a simultaneous graft if it is risky.
Here is when a same-day graft works best:
Ideal Situations
- Small to moderate bone defects. You have lost some width or height, but not everything.
- Dehiscence or fenestration defects. These are small holes or missing sections on the side of the future implant site.
- Socket preservation after extraction. You just pulled a tooth, and the socket is slightly too wide for the implant.
When You Cannot Do It at the Same Time
- Active infection. If you have pus or severe gum disease at the site, the dentist must clean it first. Grafting into infection almost always fails.
- Very large bone loss. If more than 50% of the bone is missing, you need a staged graft. This means graft first, wait 6-9 months, then place the implant.
- Poor general health. Uncontrolled diabetes, heavy smoking (1+ pack/day), or radiation therapy to the jaw may force a staged approach.
A Quick Reality Check
Do not believe anyone who says “everyone can get a same-day graft.” Your safety comes first. A good dentist will take a 3D CBCT scan. This scan measures your bone in millimeters. If your bone is less than 5-6mm in height or width in the area, a staged graft is usually safer.
Types of Bone Grafts Used During Implant Placement
If your dentist says you are a candidate, they will choose a graft material. Each has pros and cons. Here is an honest comparison.
| Type of Graft | Source | Pros | Cons | Success Rate |
|---|---|---|---|---|
| Autograft | Your own body (chin, jaw, hip) | Gold standard. Living cells. Fastest healing. | Second surgery site. More pain. Limited amount. | 95-100% |
| Allograft | Human cadaver (sterilized) | No second surgery. Safe. Good results. | Slightly slower resorption. Cost moderate. | 90-95% |
| Xenograft | Cow or pig bone | Very safe. Slow resorption (holds space long). Cheap. | No living cells. Takes longer to turn into your bone. | 85-90% |
| Alloplast | Synthetic (lab-made) | Unlimited supply. No disease risk. Predictable. | Slower integration. Some brands fail more often. | 80-90% |
Which One Do Dentists Prefer?
For simultaneous grafting, most dentists reach for allograft or xenograft mixed with a membrane. Why? They are safe, easy to use, and do not require cutting another part of your body.
Important Note: Xenograft (cow bone) is very common. It is not religiously prohibited by most authorities because the minerals are purified. But always tell your dentist your concerns.
The Procedure: Step by Step (No Fear)
Let’s walk through the actual appointment. You will be numb. You should feel pressure, not pain.
Step 1: Numbing and Preparation
Your dentist injects local anesthetic. They wait 5-10 minutes. You are awake but relaxed. (Sedation is available if you are anxious.)
Step 2: Flap or Flapless?
- Flap: The dentist makes a small cut in your gum to fold it back. This gives them full view of the bone defect.
- Flapless: They punch a small hole. This is less invasive but only works if the defect is very small.
For simultaneous grafts, a small flap is more common.
Step 3: Implant Placement First
The dentist drills a precise hole. They place the implant into the healthiest part of your existing bone. The top of the implant may be level with the bone or slightly below.
Step 4: The Graft
Now, the dentist looks at the gaps. Is there a space between the implant and the bone wall? They pack the graft material into that space. They may cover the graft with a barrier membrane (like a tiny blanket) to keep gum tissue from growing into the bone space.
Step 5: Closing Up
The dentist stitches the gum over the graft (or places a healing cap). You are done.
Total time: Usually 60 to 90 minutes for one tooth.
What Happens During Healing? (Timeline)
This is where many online guides get too optimistic. Let’s be realistic.
Days 1-7 (Early Healing)
- You will have swelling like a tooth extraction.
- Minor bleeding is normal for 24 hours.
- You eat soft foods only (yogurt, soup, smoothies).
- You do not chew on that side.
Weeks 2-4 (Soft tissue closure)
- Stitches may dissolve or be removed.
- The gum looks pink and closed.
- Underneath, the graft is a “scaffold.” Your blood vessels are growing into it.
Months 2-6 (Bone remodeling)
- This is the slow part. The graft material slowly turns into living bone.
- The implant fuses with your natural bone (osseointegration).
- You wear a temporary tooth if needed.
Month 6-9 (Ready for crown)
- At 6 months, the graft should be solid bone.
- Your dentist takes an X-ray to confirm.
- Then, you get your permanent crown.
| Healing Stage | What You Feel | What the Bone/Graft Does |
|---|---|---|
| Week 1 | Sore, swollen | Graft is a clot |
| Week 2-4 | Almost normal | New blood vessels form |
| Month 2 | No pain | Graft particles bind |
| Month 6 | Normal function | Graft becomes your bone |
Honest warning: Do not rush to put the crown on at 3 months if you had a large graft. Wait the full 6-9 months. Failure is expensive and painful.
Pain, Recovery, and What to Expect (Real Stories)
Let me share a typical patient experience. Not a fantasy, not a nightmare.
Sarah, 45, had a failed root canal.
- Extraction + implant + simultaneous bone graft (allograft).
- Day 1: “I iced my face for 20 minutes on, 20 off. Took ibuprofen. Ate pudding.”
- Day 3: “Swelling peaked. I looked like a chipmunk. But no real pain, just pressure.”
- Day 7: “Back to work. Still eating soft foods.”
- Month 4: “I forgot I had an implant.”
- Month 8: “Crown placed. It feels like my real tooth.”
Pain level (0-10):
- During procedure: 0 (numb)
- Hours 2-6 after: 3-4 (dull ache)
- Day 2-3: 2-3 (controlled with Advil/Tylenol)
- After day 4: 1 or less
Medications You Will Likely Get
- Antibiotics (7 days) — take all of them.
- Chlorhexidine mouthwash (2x daily for 2 weeks) — no alcohol-based rinses.
- Ibuprofen 600mg or prescribed painkiller — use as needed.
What Hurts More: Implant Alone vs. Implant + Graft?
The graft adds about 20-30% more post-op swelling and tenderness. But most patients say it is very manageable. It is NOT like jaw surgery.
Risks and Complications: Being Honest
Every surgery has risks. A simultaneous bone graft has specific ones. Do not panic, but do not ignore them.
Common (Happens in 5-15% of cases)
- Graft exposure: The gum stitches open, and you see white graft particles. Usually fixable with antibiotics and rest.
- Minor infection: Redness, pus, bad taste. Your dentist will prescribe stronger antibiotics.
- Swelling that lasts 7+ days: This is annoying but usually resolves.
Uncommon (Happens in 1-5% of cases)
- Graft fails to integrate: The graft washes out or turns into scar tissue. The implant becomes loose.
- Nerve irritation: If the graft is near your lower jaw nerve, you may feel tingling in your lip for a few weeks (rarely permanent).
- Sinus perforation: For upper back teeth, the graft can push into the sinus. Usually heals with antibiotics.
Rare (Less than 1%)
- Complete implant failure: The implant does not fuse. You lose the implant and graft. Requires restarting from scratch.
- Severe allergic reaction: Extremely rare with xenograft or allograft (they are highly processed).
How to Reduce Risks (Checklist)
- Do not smoke for at least 2 weeks before and 2 months after. (Smoking kills graft success by 40%.)
- Control your blood sugar if diabetic (HbA1c below 7.0).
- Take the full course of antibiotics.
- Do not use a straw for 2 weeks (suction dislodges the graft).
- Do not poke the area with your tongue or finger.
Success Rates: What the Research Says
Let’s look at numbers. These come from peer-reviewed dental journals (real data).
| Scenario | Success Rate (5 years) |
|---|---|
| Implant in healthy bone (no graft) | 97-98% |
| Simultaneous graft (small defect <3mm) | 94-96% |
| Simultaneous graft (moderate defect 3-6mm) | 88-93% |
| Staged graft (heal first, then implant) | 90-95% |
The takeaway: A simultaneous graft works very well if your defect is small to moderate. It is slightly less predictable than placing an implant in perfect bone, but the difference is small (2-5%).
What About 10 Years?
At 10 years, studies show that successful simultaneous grafts remain stable. The grafted bone behaves like natural bone. There is no extra long-term risk.
Cost Breakdown (Real Numbers, USA)
Prices vary wildly by city and dentist. These are averages without insurance.
| Procedure | Average Cost |
|---|---|
| Implant placement only | 1,500−2,500 |
| Bone graft (small, same site) | 400−800 |
| Bone graft (moderate, with membrane) | 800−1,500 |
| CBCT scan (3D X-ray) | 250−500 |
| Crown (tooth on top) | 1,000−2,500 |
Total for implant + simultaneous graft + crown: 3,500to3,500to6,500 per tooth.
Does Insurance Cover It?
- Medical insurance: Sometimes if bone loss is due to trauma, tumor, or congenital defect.
- Dental insurance: Often pays 0% for graft. May pay 30-50% for implant crown.
- Discount plans: May save 20-30%.
Tip: Ask your dentist for a “split payment plan” or third-party financing (CareCredit, LendingClub). Many clinics offer 12-24 months interest-free.
Is It Cheaper to Do Graft and Implant Separately?
Actually, no. Doing them together saves you:
- One anesthesia fee ($200-400)
- One set of facility fees ($150-300)
- Your time (two recoveries vs. one)
A staged graft (separate) can cost 1,000−1,000−2,000 more overall.
Alternatives to Simultaneous Bone Grafting
Maybe you are not a candidate. Or you do not want a graft at all. Here are your real options.
1. Staged Bone Graft (Traditional)
- What: Graft first. Wait 6-9 months. Then implant.
- Best for: Large defects, smokers, poor healers.
- Downside: Two surgeries. Longer total time (12-15 months til crown).
2. Short Implants
- What: Implants that are 4-6mm long instead of 8-12mm.
- Best for: Mild to moderate bone loss in height.
- Downside: Not good for narrow bone. Slightly lower success in molars (85-90% vs 95%).
3. Zygomatic Implants
- What: Very long implants that anchor in your cheekbone (for upper jaw).
- Best for: Severe upper bone loss (no graft possible).
- Downside: Very expensive (8k−15k per implant). Requires specialist.
4. Do Nothing or Bridge
- What: Accept the gap or get a traditional bridge.
- Downside: Bridges damage adjacent teeth. No bridge = bone continues to shrink.
Comparison Table: Graft vs. Alternatives
| Option | Time to Crown | Cost | Success Rate | Invasiveness |
|---|---|---|---|---|
| Simultaneous graft | 6-9 months | $$ | 90-96% | Moderate |
| Staged graft | 12-15 months | $$$ | 90-95% | High (2 surgeries) |
| Short implant | 4-6 months | $$ | 85-90% | Low |
| Bridge | 3-4 weeks | $ | 80-90% (10yr) | Low (but damages teeth) |
Frequently Asked Questions (FAQ)
1. Can I feel the bone graft after surgery?
No. You will feel swelling and stitches. But you cannot feel the graft itself. Your body does not sense bone particles.
2. How do I know if the graft is working?
You will not know without X-rays. At 6 months, your dentist takes a periapical X-ray or CBCT. New bone looks grey and fuzzy (not white like graft particles).
3. What happens if the graft fails?
The implant may feel loose. Or your gum may open and white grains come out. Call your dentist immediately. They may clean the site, place a membrane, or remove the implant and restart after healing.
4. Can I have a bone graft if I smoke?
Yes, but your failure rate doubles (from 10% to 20-30%). Most honest dentists will ask you to quit for 2 weeks before and 8 weeks after. If you cannot, staged grafting is safer.
5. Is cow bone graft safe for vegetarians or vegans?
This is personal. Most vegan patients choose alloplast (synthetic) or allograft (human). Xenograft (cow) is mineral, not cellular. But it is still animal-derived. Ask your dentist for alternatives.
6. How long does the graft material stay in my body?
Forever? No. Over 6-12 months, your body replaces the graft particles with living bone. The graft is a scaffold. By 1 year, 70-90% of the graft is replaced by your own bone.
7. Will my face look different?
No. A single-tooth bone graft adds less than 1-2mm of bone. You will not see a cosmetic change. Only your X-ray changes.
8. Can I get a same-day temporary tooth?
Sometimes yes, if the implant is very stable. But if you need a graft, most dentists will say no to a temporary tooth. Chewing on the graft too early causes failure.
Tips for a Smooth Recovery (Doctor-Approved)
First 24 Hours (Critical)
- Keep gauze on the site for 1-2 hours.
- Do not spit, rinse, or use a straw.
- Sleep with your head elevated (extra pillow).
- Apply ice packs (15 min on, 15 off) for 6 hours.
Days 2-7
- Rinse gently with salt water (1 tsp salt in 1 cup warm water) 3x daily.
- Brush other teeth normally, but avoid the surgical site.
- Eat: Mashed potatoes, scrambled eggs, protein shakes, applesauce, smooth soups.
- Avoid: Rice, seeds, nuts, chips, bread crusts (particles get stuck).
Weeks 2-4
- You may see small white flecks in your saliva. That is sometimes graft particles. Normal unless there is pain.
- Start very gentle brushing of the site with a soft toothbrush.
- Avoid crunchy foods (pretzels, popcorn) until week 6.
Signs You Should Call Your Dentist (Don’t Wait)
- Fever over 101°F (38.3°C)
- Swelling that worsens after day 3
- Pus or foul taste that does not go away
- Implant feels mobile (wobbly)
- Severe pain not controlled by ibuprofen
The Psychological Side: Why Patients Worry
Let’s be human for a moment. The phrase “bone graft” sounds scary. Like something from orthopedic surgery. In reality, placing 0.5cc of graft material (the size of a pea) is very minor.
Most patients say the same thing: “I built it up in my head. The extraction was worse.”
You will feel pressure, not sharp pain. You will hear drilling and tapping. That is normal. If you are anxious, ask for oral sedation (a pill) or nitrous oxide (laughing gas).
A Note on “Failure” Anxiety
Even if the graft fails, it is not a disaster. Your jaw returns to its original state. You lose nothing but time and money (ask about refund policies). Most clinics offer a 50-100% retreatment warranty if you follow instructions.
Conclusion
A bone graft at the time of implant placement is a safe, common, and effective way to restore your jawbone in a single surgery when bone loss is small to moderate. Success rates are excellent (88-96%) for properly selected patients, and recovery is manageable with soft foods, ice packs, and a few weeks of patience. Always get a 3D scan first, be honest about your smoking and health history, and choose an experienced dentist—not the cheapest one.
Additional Resource
For a visual guide and real patient X-rays showing successful simultaneous grafts, visit the American Academy of Implant Dentistry (AAID) patient education library:
🔗 https://www.aaid.com/patients/treatments/bone_grafting.html
(Open access. No registration required.)
Disclaimer
This article is for informational purposes only and does not constitute medical advice. Dental procedures carry risks. Success rates vary based on individual health, anatomy, and compliance with post-op instructions. Always consult a licensed dentist or oral surgeon for a personal examination and CBCT scan before deciding on bone grafting or implant placement. The author and publisher are not liable for any outcomes resulting from the use of this information.


