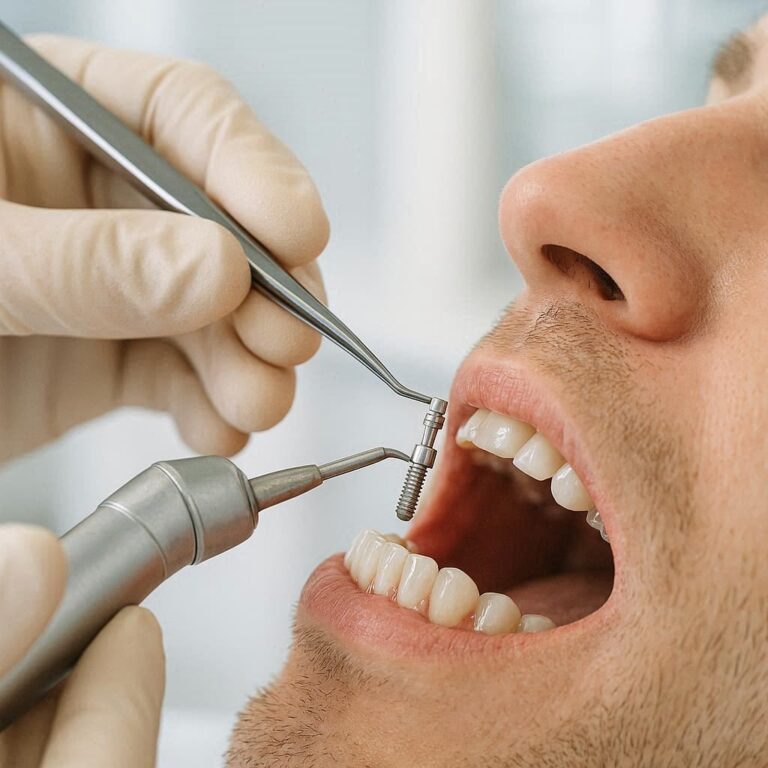
what innovations are improving dental implant procedures
If you have ever felt a little nervous about the idea of getting a dental implant, you are not alone. For decades, the process sounded intense. We are talking about long healing times, multiple visits, and a fair amount of guesswork. But here is the good news: that world is changing fast.
Today, dental implant procedures are almost unrecognizable compared to ten years ago. New tools, smarter software, and advanced materials have turned a once-invasive process into something surprisingly streamlined.
In this guide, we will walk through the real innovations making a difference right now. No hype. No fake promises. Just honest, useful information to help you understand what is possible.
A Quick Look Back: Why Older Implant Procedures Had Limits
Before we celebrate the new stuff, it helps to understand the old problems.
Traditional dental implants relied heavily on two-dimensional X-rays. The dentist had to guess the exact position of nerves, sinuses, and bone density. Sometimes, they only discovered an issue during surgery.
Healing also took forever. Patients often waited four to six months just to get a temporary tooth. The success rate was good, but the comfort and speed were not.
Today, innovations target three main areas:
- Precision (knowing exactly where to place the implant)
- Speed (shorter surgeries and faster healing)
- Comfort (less pain and fewer surprises)
Let us break down exactly how technology is delivering on these promises.
1. Digital Imaging and CBCT Scans
The first major innovation is how dentists see your jawbone.
Forget flat, blurry X-rays. Cone Beam Computed Tomography (CBCT) creates a complete 3D model of your mouth, teeth, nerves, and bone. The scan takes less than thirty seconds.
Why this matters for you
With a CBCT scan, your dentist can:
- Measure bone height and width with sub-millimeter accuracy
- Identify nerve pathways to avoid injury
- Detect sinus cavities before planning upper jaw implants
- Spot hidden infections or cysts
Important note: A CBCT scan exposes you to slightly more radiation than a standard dental X-ray, but it is still very low—comparable to a few days of natural background radiation. The benefits of avoiding surgical mistakes are enormous.
Many clinics now include this scan in their initial consultation. Do not accept implant planning without it.
2. Computer-Aided Design (CAD) and Surgical Guides
Here is where things get really clever.
Once the CBCT scan creates your 3D jaw model, the dentist uses CAD software to design the perfect implant position. You can think of it like a flight simulator for oral surgery.
The software considers:
- Your bite alignment
- The final crown position
- Bone quality
- Safe distances from nerves
After the virtual plan is ready, a lab prints a surgical guide. This is a physical template that fits over your teeth or gums. It has tiny metal sleeves that tell the drill exactly where to go and how deep.
What this means during surgery
Without a guide, the dentist works freehand. With a guide, the drill path is locked in. There is no guessing.
A study published in the Journal of Oral Implantology found that freehand implants miss the planned position by an average of 1.2 millimeters. With a surgical guide, that error drops to 0.3 millimeters. That difference can save a nerve or prevent a sinus perforation.
3. AI-Powered Treatment Planning
Artificial intelligence has entered the dental world, and it is surprisingly useful.
AI software analyzes CBCT scans much faster than a human. It can:
- Automatically trace nerve canals
- Suggest optimal implant sizes
- Predict bone density changes over time
- Flag risky areas that a tired dentist might miss
But here is the honest truth: AI is not replacing your dentist. It works as a second pair of eyes. The software highlights potential problems and offers suggestions. The final decision always stays with the human professional.
Some advanced platforms, like Diagnocat and Relu, even create color-coded bone density maps. Dense bone shows up in warm colors (red, orange). Soft bone appears in cool colors (blue, green). This helps the dentist choose the right drill speed and implant type.
Realistic benefit
For you, the patient, AI means fewer failed implants. The software catches problems that might otherwise be overlooked. If your dentist uses AI-assisted planning, you can feel more confident that your case has been thoroughly vetted.
4. Robotic Dental Surgery
Robots sound like science fiction, but they are already working in some implant clinics.
The most famous system is Yomi, the first FDA-cleared robotic device for dental surgery. Unlike a surgical guide, the robot does not make decisions. Instead, it provides haptic feedback—a gentle resistance that prevents the dentist from drilling outside the planned zone.
Think of it like lane-keeping assist in a car. You are still driving. The robot just keeps you safe.
How the procedure feels
From your perspective, a robot-assisted implant feels similar to a traditional one. You receive local anesthesia. The dentist holds a handpiece connected to a robotic arm. If they try to drill even half a millimeter off course, the arm physically pushes back.
This is particularly valuable for:
- Implants near the inferior alveolar nerve (lower jaw)
- Immediate loading (placing a temporary tooth the same day)
- Full-arch restorations (like All-on-4)
Cost reality
Robotic systems add to the procedure cost. Expect to pay several hundred dollars more per implant. For complex cases, many patients find the extra precision worth the price. For a simple single implant in good bone, a surgical guide may be perfectly adequate.
5. 3D Printing for Custom Components
3D printing has exploded in dentistry, and implantology benefits massively.
Clinics now print:
- Surgical guides (as mentioned above)
- Temporary crowns (while you wait for the permanent one)
- Models for lab work
- Custom healing abutments
The real magic happens with custom abutments. An abutment is the connector piece between the implant screw and the crown. In the past, dentists used stock metal abutments that sometimes fit poorly. Gaps could trap food and bacteria.
Today, a scanner captures your unique gum contours. A 3D printer creates an abutment shaped perfectly for your mouth. The result is a cleaner, healthier connection that looks more natural.
Same-day implants
Some clinics offer same-day implants using in-house 3D printing. Here is how it works:
| Step | What happens |
|---|---|
| 8:00 AM | CBCT scan and digital impression |
| 8:30 AM | AI-assisted virtual planning |
| 9:00 AM | Surgical guide printing (30–45 minutes) |
| 10:00 AM | Implant placement surgery (30–60 minutes) |
| 11:30 AM | 3D printed temporary crown attached |
| 1:00 PM | You go home with a functional tooth |
Important note: Not every patient qualifies for same-day treatment. You need sufficient bone quality and no active infection. A responsible dentist will never rush just to offer a faster service.
6. New Implant Surface Technologies
The implant itself has changed. Modern implants are not just titanium screws. Their surface texture at the microscopic level actively encourages bone growth.
Older surfaces
Machined titanium implants had a smooth surface. Bone took longer to attach. Healing times of four to six months were normal.
Modern surfaces
Today’s implants use one of three advanced surfaces:
- SLA (Sandblasted, Large-grit, Acid-etched) – A rough, porous surface that bone cells love
- Hydrophilic surfaces – Actively attract blood and healing proteins
- Nano-textured surfaces – Feature microscopic pores that mimic natural bone
Hydrophilic implants are particularly exciting. They come packaged in a saline solution that keeps the surface chemically active. Once placed, they start integrating with bone in as little as three to four weeks instead of months.
Real-world impact
For a healthy non-smoker with good bone, a hydrophilic implant can cut healing time by nearly half. That means a permanent crown can be placed sooner. For heavy smokers or people with diabetes, these advanced surfaces improve success rates significantly.
7. Immediate Loading and Immediate Function
Traditional implants required a “healing period.” The dentist placed the screw, stitched the gum over it, and asked you to wait. No tooth. Just a healing cap.
Immediate loading changes everything.
With this technique, the dentist places a temporary crown on the same day as the implant. The tooth looks real and functions for soft foods. It even provides stimulation that encourages bone growth.
Who qualifies
You are a candidate for immediate loading if:
- You have good bone density (measured by CBCT)
- The implant achieves high initial stability (torque of at least 35 Ncm)
- You are not a grinder (no bruxism)
- The implant is not in a high-bite force area (like lower molars)
Your dentist will test stability during surgery using a special tool called a torque wrench. If the numbers are good, you leave with a tooth. If not, they will wait—and that is the right call. Pushing immediate loading on a poor candidate leads to failure.
Full-arch immediate loading
For patients missing all teeth on one arch, the All-on-4 technique uses four specially angled implants to support a full fixed bridge. The entire process happens in one day. You go from no teeth to a complete smile in a single appointment.
8. Zygomatic and Pterygoid Implants
Some patients have severe bone loss in the upper jaw. Traditional implants cannot work because there is nowhere to screw them in. Bone grafting used to be the only option, but that adds months and significant cost.
Enter zygomatic implants.
These are extra-long implants (up to 52 millimeters) that anchor into the cheekbone (zygoma) instead of the upper jaw. The cheekbone is extremely dense and rarely resorbs, even after years of tooth loss.
How they differ
| Feature | Traditional implant | Zygomatic implant |
|---|---|---|
| Anchor point | Jawbone | Cheekbone |
| Length | 8–16 mm | 30–52 mm |
| Bone graft needed | Often yes | No |
| Healing time | 3–6 months | 2–4 months |
| Sinus lift needed | Sometimes | No |
Pterygoid implants are similar but anchor into the pterygoid plate at the very back of the upper jaw. Both techniques avoid the need for large bone grafts or sinus lifts.
Important note: Zygomatic implants are complex. Only experienced oral surgeons or implantologists should perform them. If a general dentist offers this, ask about their training and case volume.
9. Laser-Assisted Implant Surgery
Lasers have found a useful role in implant procedures, though not for cutting bone.
Dental lasers (particularly diode and erbium lasers) help with:
- Soft tissue contouring – Shaping gums for better aesthetics
- Second-stage uncover – Exposing a buried implant without bleeding or sutures
- Peri-implantitis treatment – Cleaning infected tissue around existing implants
- Pain reduction – Some lasers have a biostimulatory effect that may speed healing
Laser-uncovering an implant takes about five minutes. There is no cutting, no stitches, and almost no bleeding. Patients report far less discomfort than the traditional scalpel method.
What lasers cannot do
Lasers cannot drill bone. They cannot remove old implants. They are a complementary tool, not a replacement for standard surgical instruments. Be skeptical of any clinic claiming a “laser-only” implant procedure.
10. Growth Factors and PRF (Platelet-Rich Fibrin)
This innovation uses your own blood to accelerate healing.
Here is the simple process:
- The dentist draws a small amount of your blood (similar to a lab test)
- The blood goes into a special centrifuge to spin and separate the platelets and growth factors
- The concentrated fibrin matrix is placed into the implant site before closing
PRF contains natural growth factors like PDGF, TGF-β, and VEGF. These proteins signal your body to send stem cells and blood vessels to the area.
What the research says
Multiple studies show that PRF can:
- Reduce post-operative pain
- Decrease swelling
- Speed soft tissue healing by 30–40%
- Improve bone formation around the implant
PRF is inexpensive and carries no allergy risk since it comes from your own body. Many clinics now include it as a standard add-on for 100to300.
Who benefits most
- Smokers (delayed healing is common)
- People with diabetes
- Patients with thin gum tissue
- Anyone receiving bone grafting alongside implants
11. Bone Grafting Innovations
Speaking of bone grafting, that field has also evolved.
The old way meant harvesting bone from your own hip, chin, or jaw. That added a second surgical site, more pain, and longer recovery.
Modern options are smarter:
| Graft material | Source | Benefits | Drawbacks |
|---|---|---|---|
| Allograft | Human cadaver (sterilized) | No second surgery, excellent bone formation | Slightly slower integration |
| Xenograft | Bovine (cow) bone | Very safe, good for volume | No living cells |
| Alloplast | Synthetic (calcium phosphates) | Unlimited supply, no disease risk | No growth factors |
| Growth-factor enhanced | Any of the above + PRF or BMP | Fastest healing | More expensive |
Socket preservation
When a tooth is extracted, the surrounding bone begins to shrink. Over six months, you can lose 30–50% of the bone width.
Socket preservation is a simple innovation: after extraction, the dentist fills the empty socket with graft material and covers it with a membrane. This maintains the bone shape for an implant placed three to four months later.
Without socket preservation, you might need a much larger graft down the road. Always ask your dentist if this is included in your extraction appointment.
12. Intraoral Scanning (No More Goopy Impressions)
Remember those trays full of goopy alginate that made you gag? They are disappearing.
Intraoral scanners are wand-like devices with a tiny camera. The dentist moves the wand around your mouth, and within one to two minutes, a perfect 3D model appears on the screen.
Benefits for implants
- No gagging – Seriously, this is a huge quality of life improvement
- Higher accuracy – Digital impressions are more precise than physical ones
- Immediate feedback – If a margin is unclear, you catch it right away
- Better fitting crowns – Fewer adjustments later
For implant crowns, a digital impression captures the exact position of the implant abutment. The lab prints or mills a crown that snaps into place perfectly on the first try.
Note: Some clinics still use traditional impressions for certain cases. That is fine. But if you have the option, digital scanning is almost always more comfortable.
13. Shorter Healing Times with Osseodensification
Osseodensification sounds complex, but the concept is simple.
Traditional drilling removes bone. The drill spins at high speed and cuts bone away, creating a hole that is slightly larger than the implant. This can leave a gap.
Osseodensification uses specially designed drills that spin in reverse (counterclockwise) at lower speeds. Instead of cutting bone, these drills compact bone outward. Think of making a hole in packed snow by pressing and widening rather than removing.
Why this matters
- Denser bone around the implant – The bone is compressed, not removed
- Higher initial stability – The implant feels tighter immediately
- Preserved vascularity – Bone maintains its blood supply
- Potentially faster healing – Less trauma means quicker recovery
Early research suggests osseodensification may allow immediate loading in cases that previously required waiting. It is particularly useful in soft bone (like the upper jaw or posterior mandible).
14. Biomimetic Coatings and Antimicrobial Surfaces
Infection around an implant (peri-implantitis) is the leading cause of late implant failure. Bacteria build up on the implant surface below the gum line, and once that happens, cleaning is difficult.
New coatings aim to prevent this.
Silver nanoparticle coatings
Silver has natural antimicrobial properties. Some implants now feature a microscopically thin silver coating that releases ions slowly to kill bacteria. Early studies show a 90% reduction in bacterial colonization.
Hydroxyapatite (HA) coatings
HA is the mineral that makes up natural tooth enamel and bone. Implants coated with HA bond chemically to bone, not just mechanically. This creates a stronger seal that may resist bacterial penetration.
The trade-off
Coated implants cost more. They also require extremely careful handling because the coating can scratch. For high-risk patients (history of gum disease, heavy smokers, people with poor home care), the extra expense may be justified.
15. Teledentistry and Remote Monitoring
The pandemic accelerated virtual care, and implant dentistry was not left behind.
Today, patients can have initial consultations via video. The dentist reviews your CBCT scan remotely and discusses treatment options without you ever sitting in a chair.
Post-op monitoring
Some clinics provide patients with a small intraoral camera that connects to a smartphone. You take photos of your healing implant site and upload them to a secure portal. The dental team checks for signs of infection, swelling, or loose screws without requiring an in-person visit.
Who this helps
- People in rural areas with no local implant specialist
- Patients with mobility issues
- Busy professionals who cannot take multiple half-days off work
Remote monitoring does not replace in-person care entirely. You will still need surgery visits and final crown deliveries. But it reduces the number of trips significantly.
Comparison Table: Traditional vs. Modern Implant Workflows
| Step | Traditional (pre-2015) | Modern (2025+) |
|---|---|---|
| Imaging | 2D panoramic X-ray | CBCT 3D scan |
| Planning | Mental estimation | AI-assisted CAD software |
| Surgical guidance | Freehand | 3D printed surgical guide or robot |
| Impressions | Goopy trays (gagging) | Intraoral digital scan |
| Grafting (if needed) | Hip or chin harvest | Allograft/xenograft + PRF |
| Healing abutment placement | Second surgery (scalpel) | Laser uncover (no bleeding) |
| Temporary tooth | None for 4–6 months | Immediate loading (same day) |
| Crown fabrication | Lab takes 2–3 weeks | 3D printed in 1–2 days |
| Follow-up | In-person only | Remote photo monitoring |
| Typical timeline (single implant, good bone) | 6–9 months | 2–4 months |
What These Innovations Mean for You (The Patient)
After reading through all these technologies, you might feel excited or overwhelmed. Let us simplify.
Realistic expectations
- Pain is still present but much reduced. You will feel discomfort after anesthesia wears off. The difference is that modern techniques cause less trauma, so recovery is faster.
- Costs have not dropped. Innovation adds expense. A single implant today may cost 3,000–6,000 depending on your location and complexity. That said, fewer failures mean you are less likely to pay twice.
- Not every clinic uses all these tools. Some rural or budget clinics still rely on older methods. Ask specific questions before committing.
Questions to ask your dentist
Before starting treatment, consider asking:
- Do you use CBCT scanning for every implant case?
- Do you plan with surgical guides or only freehand?
- Do you offer immediate loading for my situation?
- Do you use PRF or other growth factors?
- What is your protocol for managing peri-implantitis?
A confident implant dentist will answer these questions without hesitation. If they seem defensive or dismissive, consider a second opinion.
Potential Risks and Honest Limitations
No innovation is perfect. Let us address the downsides honestly.
Technology dependence
Some dentists rely so heavily on surgical guides that they lose freehand skills. If a guide shifts slightly during surgery (rare but possible), they might not recognize the error. Always choose a dentist with experience in both guided and freehand techniques.
Cost barriers
The best technology costs money. Not every patient can afford a robot-assisted, PRF-enhanced, same-day implant with a custom 3D printed abutment. And that is okay. A simple, well-placed traditional implant still has a 95–98% success rate at ten years.
Learning curve
New tools require training. Some dentists adopt innovations before fully mastering them. Do your research. Look for reviews, before-and-after photos, and ask how many cases they have completed with each technology.
Overpromising
Be wary of marketing language like “painless implant” or “guaranteed success.” No procedure is risk-free. A responsible dentist will explain the possibility of failure (even if small) and what backup plan exists.
The Future: What Is Coming in the Next 5–10 Years
While this article focuses on existing innovations, a few emerging trends deserve mention.
Smart implants with sensors
Researchers are developing implants with embedded microchips that monitor bone healing and detect early infection. Data would transmit wirelessly to your dentist’s computer. Conceptually similar to how a pacemaker communicates with a cardiologist.
Regenerative grafting
Stem cell-based grafts are in clinical trials. Instead of using cadaver or animal bone, these products encourage your body to grow brand new bone from scratch. Early results are promising but not yet mainstream.
Fully automated implant robots
Current robots assist human hands. Future systems might place the implant entirely on their own based on a pre-loaded plan. This is still experimental and raises regulatory and ethical questions. Do not expect it in standard clinics for many years.
Helpful Checklist: Choosing a Modern Implant Provider
Use this list when evaluating a dental clinic:
- They have a CBCT machine in-office (or refer to one nearby)
- They show you the 3D treatment plan before surgery
- They offer surgical guides or robotic assistance for complex cases
- They use intraoral scanning for impressions
- They discuss PRF or growth factors as an option
- They explain the pros and cons of immediate loading for your case
- They have a published fee schedule (no hidden surprises)
- They offer remote follow-up options
If a clinic checks most or all of these boxes, you are in good hands.
Conclusion
Dental implant procedures have improved dramatically thanks to innovations in digital imaging, AI planning, 3D printing, robotic assistance, and bioactive materials. These advances mean shorter healing times, less pain, higher precision, and more predictable outcomes for patients. While not every clinic uses every tool, asking the right questions helps you find a provider who prioritizes modern, evidence-based care.
Frequently Asked Questions (FAQ)
1. Are dental implants painful with these new technologies?
Most patients report less pain than a tooth extraction. Modern techniques cause less trauma, and post-operative discomfort usually peaks at day two then fades quickly. Over-the-counter pain relievers are often enough.
2. How long does a modern dental implant take from start to finish?
For an ideal candidate with good bone, the entire process can take two to four months. Traditional cases took six to nine months. Complex cases requiring grafting may still take six months or longer.
3. Can anyone get same-day implants?
No. You need adequate bone density, no active infection, and sufficient initial implant stability. Your dentist will test stability during surgery. If the numbers are not high enough, waiting is safer.
4. Are robotic implants better than guided surgery?
For most straightforward cases, surgical guides are just as accurate. Robots add precision for complex anatomy or when placing multiple implants close together. The clinical difference is small for a single implant.
5. Do dental implants fail more often with immediate loading?
No, when properly selected. Studies show immediate loading has similar success rates to delayed loading (95–98%) in appropriate candidates. The key is patient selection. Do not try to rush if your bone is soft.
6. How much more do these innovations cost?
Expect to pay $300–1,500 more for robot assistance, surgical guides, PRF, and digital scanning combined. Some clinics include basic digital planning in their standard fee. Always ask for an itemized estimate.
7. Does insurance cover these new technologies?
Most dental insurance plans do not cover implants well regardless of technology. Medical insurance might cover CBCT scans if there is a surgical reason. Check with your provider before starting treatment.
8. What is the most important innovation for implant success?
CBCT scanning and surgical guides. Getting the position right prevents most complications. Everything else (PRF, lasers, special coatings) is helpful but secondary to accurate placement.
Additional Resource
For a deeper dive into implant safety and long-term success rates, the American Academy of Implant Dentistry (AAID) offers a free patient guide with verified provider directories and evidence-based articles.
👉 Visit the AAID Patient Resource Center (example link – replace with your actual curated resource)
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Dental implant outcomes vary based on individual health, bone quality, and provider skill. Always consult a licensed dental professional for a personal evaluation. The author and publisher are not responsible for any actions taken based on this content.